Experiencing unexpected changes in your body can be worrying. If you have been dealing with discomfort in your pelvis or changes to your cycle, you might be wondering what is going on.
Two common conditions that affect the female reproductive system are fibroids and ovarian cysts. While they share some symptoms, they are quite different. Understanding the differences can help you take charge of your health and find the relief you deserve.
What are fibroids?
Fibroids, also called uterine leiomyomas, are non-cancerous growths that develop in or on your uterus. They are tumours composed of muscle and fibrous tissue. They vary in size, from tiny seed-like nodules to large masses that can distort the shape of your reproductive organs.
Types of fibroids
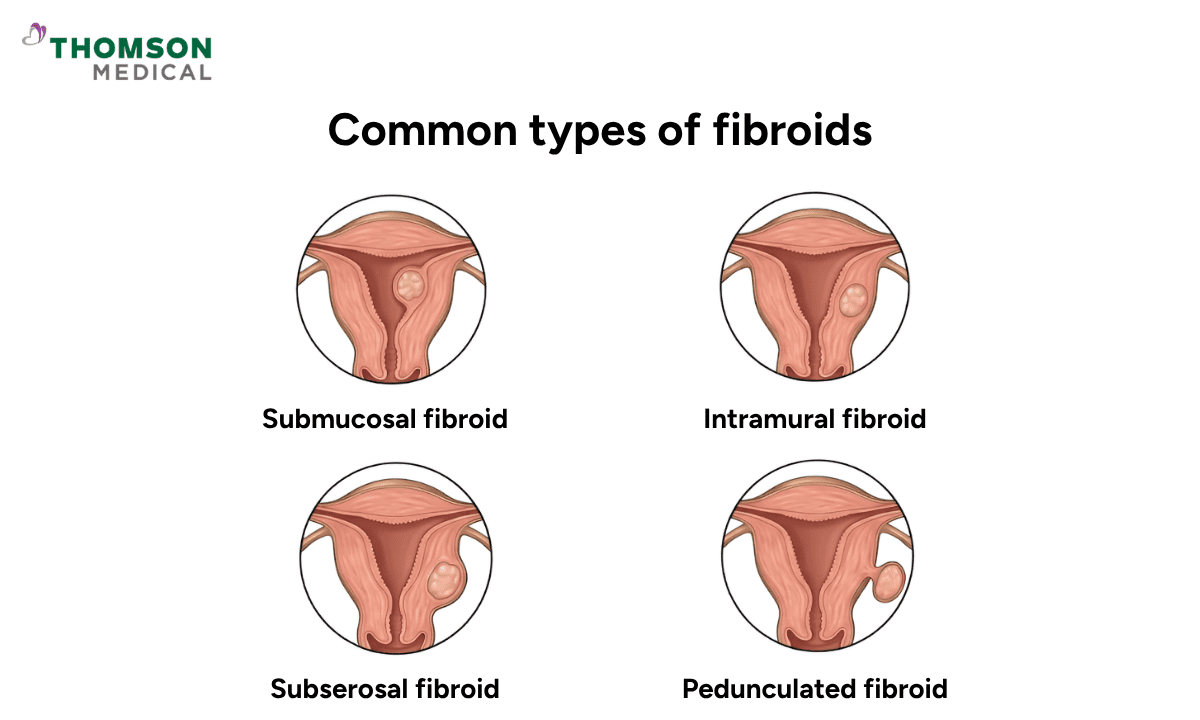
Fibroids are classified based on their location within the uterus.
Common types of fibroids include:
Submucosal fibroids:
Grow just beneath the lining of the uterus and can protrude into the uterine cavity
Often cause heavy bleeding or fertility issues
Intramural fibroids:
Develop within the uterine walls and can enlarge your uterus
Sometimes cause pain or pressure
Subserosal fibroids:
Grow on the outer surface of your uterus and may press on surrounding organs
May lead to urinary or bowel-related symptoms such as constipation or pelvic pain
Pedunculated fibroids:
Attached to your uterus by a stalk and can be submucosal or subserosal
May cause sudden pain if the stalk twists
Knowing the specific type of fibroid you have helps your doctor tailor the right approach for your care.
What causes fibroids?
The exact cause of uterine fibroids is not fully understood, but several hormonal factors contribute to their development.
Hormones, particularly oestrogen and progesterone, stimulate fibroid growth through specific hormone receptors. This is why they are more common during your reproductive years and may naturally shrink after menopause.
Genetics also play a role, as women with a family history are more likely to develop them. Other factors include obesity, early menarche, and certain growth factors that promote cell proliferation in the uterine muscle cells.
If you’re concerned about fibroids or want a personalised assessment, you may schedule a consultation with Thomson Medical to discuss your reproductive health and next steps.
What are cysts?
Cysts are simply fluid-filled sacs that can develop in various parts of your body. When they develop in your ovaries, they are known as ovarian cysts.
Types of ovarian cysts
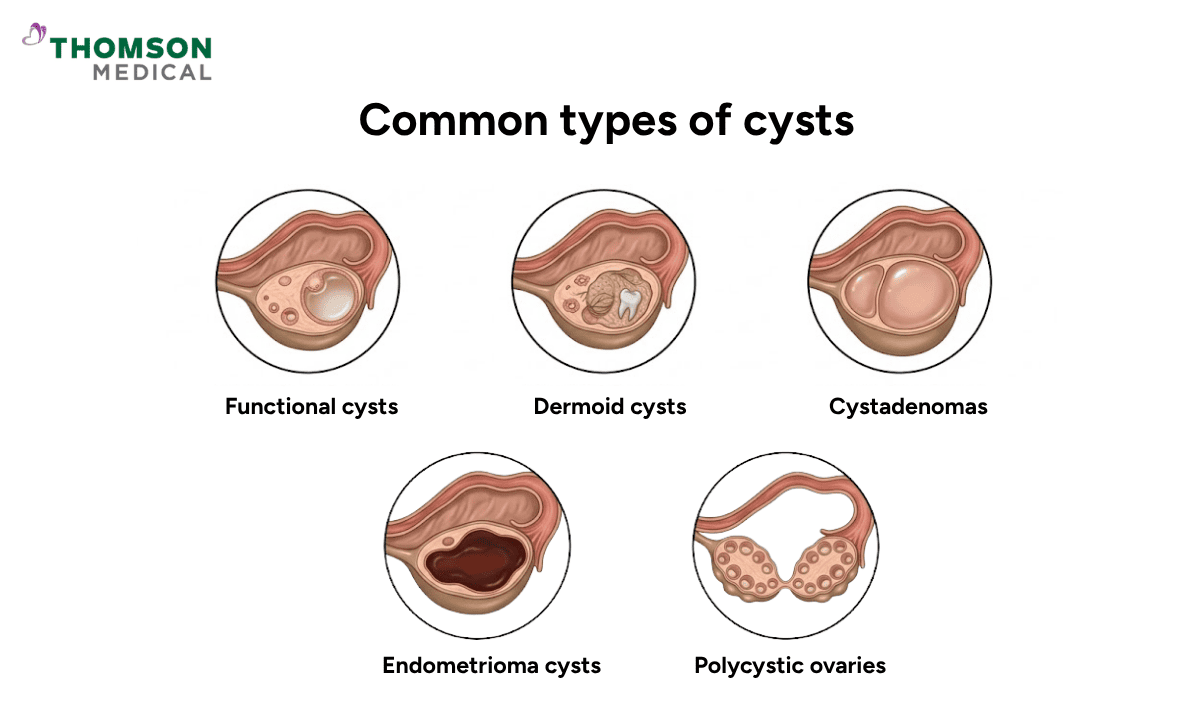
Ovarian cysts can be classified into several different types.
Common types of cysts include:
Functional cysts:
Form from ovarian follicles and include follicular cysts and corpus luteum cysts
Related to the normal menstrual cycle and usually resolve on their own
Dermoid cysts:
Contain various tissues like hair or fat
Commonly linked to congenital in nature
Cystadenomas:
Benign (non-cancerous) growths that develop from ovarian tissue
Can grow quite large
Endometrioma cysts:
May form in women with endometriosis
Usually contain thick, dark fluid
Polycystic ovaries:
Often seen in polycystic ovarian syndrome (also known as polycystic ovary syndrome or PCOS)
May contain multiple small cysts along the ovarian surface
Most of these cysts are usually harmless, but your doctor will help monitor them to ensure your peace of mind.
What causes ovarian cysts?
Ovarian cysts often develop as part of your menstrual cycle, especially as your hormone levels fluctuate throughout the month.
Common causes include ovulation-related changes, such as when a follicle fails to release an egg or the corpus luteum fills with fluid. These are the most common cause of ovarian cysts
Certain factors can also increase your chances of developing ovarian cysts, including:
Being in your reproductive years
Having had cysts before
Experiencing irregular periods
The reassuring part is that ovarian cysts are very common, and in many cases, they’re simply a normal part of how your body works.
Fibroid vs cyst: What is the difference?
Fibroids and cysts are both common growths in the reproductive system, but they’re quite different in what they are and how they affect your body.
Key differences between the two are the following:
Feature | Fibroids | Ovarian Cysts |
Composition | Solid, non-cancerous tumours made of muscle and fibrous tissue | Fluid-filled sacs |
Location | Form in or on your uterus | Typically develop in your ovaries |
Common effects & symptoms | Can cause heavy periods, abnormal uterine bleeding, pelvic pressure, or fertility issues depending on their size and location | Generally benign and may resolve on their own, though some can cause pelvic pain, bloating, or complications like rupture |
Knowing the difference can make things feel a little less overwhelming. More importantly, it helps you have clearer, more confident conversations with your doctor so you can choose what’s right for your body and your long-term health.
If you’re unsure whether your symptoms could be related to fibroids or ovarian cysts, schedule a consultation with Thomson Medical for a personalised assessment and guidance.
How to tell if you have a fibroid or cyst
It can be difficult to tell the difference between uterine fibroids and ovarian cysts based on symptoms alone, as both can affect the pelvic area. However, there are some diangositic methods that may help guide your doctor.
Diagnostic methods
Diagnosis usually starts with a gentle pelvic exam, where your doctor carefully checks for any unusual masses around the uterus or ovaries.
They may also recommend:
Blood tests to check hormone levels, detect hormonal imbalances, and sometimes measure CA-125, a protein that can be raised in both benign conditions and ovarian cancer.
Imaging tests
While this process can feel a little overwhelming, each step helps give you clearer answers so you can move forward with the right care and peace of mind.
Ultrasound and imaging
A pelvic ultrasound is the most common way to check for fibroids and ovarian cysts. It uses sound waves to create images and can help tell the difference between a solid mass and a fluid-filled sac.
Ultrasound is also useful over time, as it helps your doctor keep track of any changes in size or see how well treatment is working.
In some cases, a magnetic resonance imaging (MRI) scan may be recommended for a more detailed view, especially if the fibroids are large, the cysts are more complex, or if surgery is being considered.
When to see a doctor
You should seek professional medical advice if you experience:
Persistent abdominal or ongoing pelvic pain
Abnormal or heavy bleeding
Bloating that doesn’t go away
A feeling of pressure on the bladder
Sudden, sharp pain in the pelvis
Regular pelvic check-ups are also important, especially if you have a family history of gynaecological conditions or are planning a pregnancy.
Getting checked early helps ensure any growths are properly monitored, lowering the risk of complications such as ovarian torsion (when the ovary twists), pelvic infection, or, in rare cases, cancer.
Our specialists
Loading...
What are the treatment options for fibroids vs cysts?
Treatment depends on your symptoms, the size of the growth, and what feels right for your body and lifestyle.
Treatment approach | Fibroids | Ovarian cysts |
Careful monitoring | Small fibroids that don’t cause symptoms are usually monitored over time | Many functional cysts go away on their own and only need watchful waiting |
Medications | Medications may help regulate your cycle or reduce heavy bleeding and pain | Hormonal contraceptives may help prevent new functional cysts from forming |
Non-surgical procedures | Uterine artery embolisation, which helps block blood supply to fibroids, helping them shrink over time | Not commonly used, as cysts are usually managed with medication or surgery |
Surgical options | Minimally invasive surgery, such as laparoscopy, may be recommended for larger or persistent fibroids | Larger or symptomatic cysts can be safely removed through laparoscopy |
Treatment is not one-size-fits-all. It’s about finding an approach that matches your symptoms, your goals, and what feels manageable for you, with guidance from your doctor.
Can fibroids or cysts affect fertility?

Yes, both fibroids and ovarian cysts can affect fertility, but it really depends on their type, size, and where they are.
In most cases, fibroids do not significantly affect fertility. However, certain types, especially those that grow into your uterine cavity (the inner space of your uterus), can make it harder for a fertilised egg (embryo) to attach or may increase the risk of miscarriage. Some fibroids can also affect blood flow to your uterine lining.
Your doctor can assess whether your fibroids are likely to have an impact and discuss the options available to you.
Ovarian cysts, like endometriomas or larger cysts, may sometimes affect ovulation or impact nearby structures like your fallopian tubes. However, many functional cysts are harmless and often go away on their own without affecting fertility.
A simple check-up can give you clearer answers and help you take the next steps with more confidence and reassurance.
If you’re thinking about fertility and want to understand potential risks from fibroids or cysts, you may arrange a check-up with Thomson Medical to discuss your options.
FAQ
Can a cyst turn into a fibroid?
No. Cysts and fibroids are different types of growths and don’t turn into each other.
Are fibroids and cysts cancerous?
Most are not. Fibroids are almost always non-cancerous, and most ovarian cysts are benign too. A small number of cysts may need closer monitoring, just to be safe.
Can you have fibroids and cysts at the same time?
Yes, it’s possible. Since they form in different parts of the reproductive system, they can exist together and sometimes cause overlapping symptoms.
Do fibroids and cysts go away on their own?
Many ovarian cysts do, especially functional ones, which often resolve within a few cycles. Small fibroids may stay the same or shrink over time, particularly after menopause.
What size fibroid or cyst needs surgery?
Surgery is usually considered for fibroids or cysts that are large, symptomatic, or at risk of complications.
Fibroids larger than 5 to 6 cm or causing heavy bleeding or abdominal enlargement may require removal.
Ovarian cysts larger than 5 to 10 cm or persistent cysts may also require surgery.
The decision is always based on your symptoms, age, and overall health.
Can fibroids or cysts cause weight gain?
Not directly. They may cause bloating or a feeling of fullness, which can make your abdomen look larger, but true weight gain is usually linked to other factors such as diet or lifestyle.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
