Pain on the side of your hip can be confusing. It is not quite back pain, and it does not feel like typical groin pain either. If you've come across the term 'gluteus medius' while searching for answers, you might be wondering whether this muscle is the reason behind your symptoms.
The gluteus medius is a key muscle on your outer hip that plays an important role in how you walk and move. When it's strained or weak, it tends to produce persistent pain right on the side of your hip.
Let’s walk through how to recognise the signs and what you can do about it.
What is the gluteus medius?
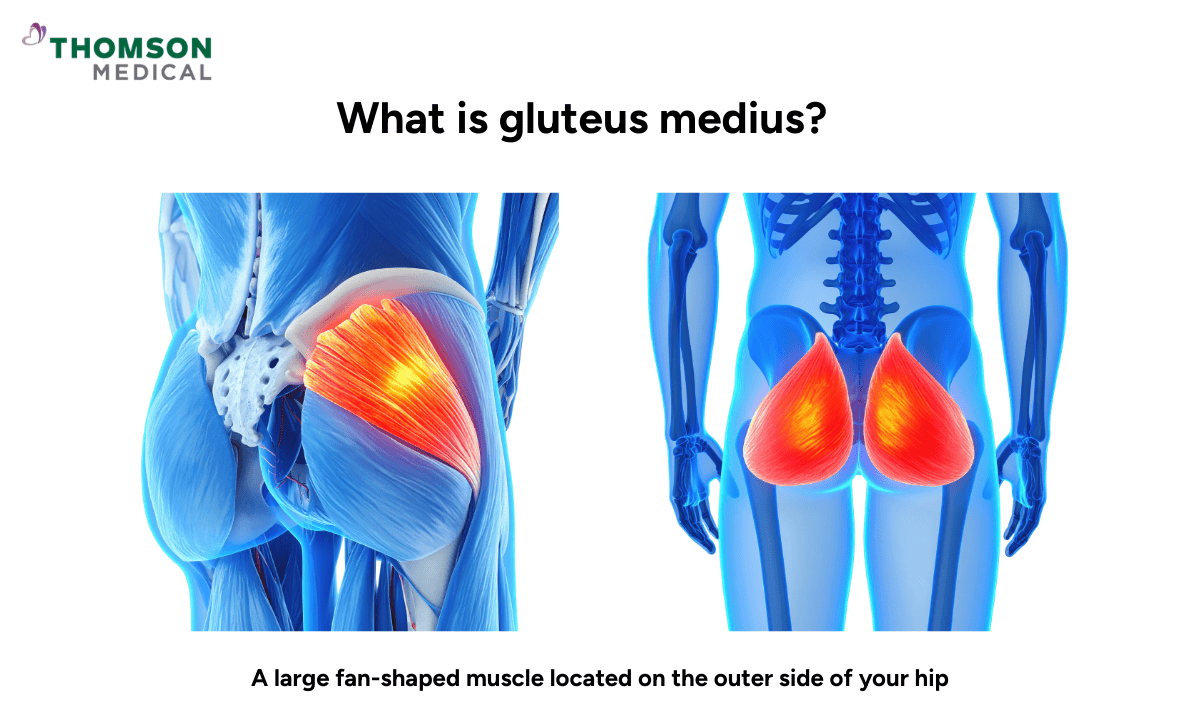
The gluteus medius sits on the outer side of your hip, beneath your larger gluteal muscles. To picture where it is, place your hand on the side of your pelvis and stand on one leg. The area that tightens up is where your gluteus medius is doing its job.
This muscle is responsible for:
Keeping your pelvis steady when you walk or run
Supporting your hip when you balance on one leg
Helping your lower back and knee stay properly aligned
Every time you take a step, climb stairs, or stand on one leg, your gluteus medius is involved.
What does gluteus medius pain feel like?
If you've been searching for answers and come across the term 'gluteus medius', you might be wondering whether what you're feeling actually fits. Learning how this type of pain tends to present can help you work that out.
Gluteus medius pain usually shows up as:
Aching on the outer side of your hip
Tenderness when you press the bony part of the hip
Pain when lying on that side
Discomfort when walking for longer periods
Pain when climbing stairs
A dull, deep ache in the buttock
If that sounds familiar, there's a reasonable chance your gluteus medius is involved. The good news is that this type of problem is usually very manageable once it is correctly identified.
Not sure if this sounds like your pain? A proper assessment can help confirm whether your gluteus medius is the source and guide you toward the right recovery plan. Request an appointment with Thomson Medical today so you don’t have to keep guessing.
Why does your gluteus medius hurt?
Gluteus medius pain tends to develop when the muscle has been overloaded, has become underactive, or has been asked to do more than it's ready for. The reasons vary, and certain habits and activities make this more likely.
Causes | Why it leads to pain | More likely in |
Muscle weakness or imbalance | A weak gluteus medius struggles to stabilise your pelvis, leading to overwork and irritation over time. | Office workers, older adults, people returning to exercise after a break |
Overuse and repetitive strain | Repeated running or climbing stairs can cause muscle fatigue. | Runners, hikers, people increasing training intensity |
Sudden change in activity | A rapid increase in walking, running, or new workouts can overload a muscle before it’s had time to adapt. | People starting new fitness routines |
Prolonged sitting & poor posture | Sitting for long periods keeps the muscle underactive, so it doesn’t respond well when suddenly required to work. | Desk-based workers, drivers |
Acute injury | Falling on your side or hitting the side during sports or any other type of accident can injure your gluteus medius. | Athletes |
Post-pregnancy pelvic changes | Changes in pelvic stability after pregnancy can increase strains on your hip muscles. | Postpartum women |
The gluteus medius plays a part in almost every step you take, which means it works continuously throughout the day. That's why it doesn't take a significant injury to trigger pain.
How is gluteus medius pain diagnosed?
Diagnosis is usually straightforward and doesn't require complex scans.
Your doctor or physiotherapist will start by asking about your symptoms in detail, including when the pain started, what makes it better or worse, and how it affects your daily movement. Your answers help point toward whether the problem is muscular, joint-related, or coming from a nerve.
The physical examination tends to be the most useful part. Your clinician will generally:
Press on the outer hip
Observe how you walk
Test your hip strength
Check the flexibility of your hip
In most cases, imaging isn't needed. But if the pain is severe, getting worse, or not responding to rehabilitation, an ultrasound imaging or MRI (magnetic resonance imaging) scan can help confirm what's going on and rule out other conditions.
Our orthopaedic specialists
Loading...
Treatment options for gluteus medius pain
The good news is that most gluteus medius pain settles within four to six weeks. With some rest, lifestyle changes, and the right exercises, your symptoms usually improve. Surgical repair is rarely required, and you can usually remain active during recovery.
Physical therapy
Building strength in the gluteus medius is key to getting better. When the muscle has become weak or overloaded, simply stretching it or waiting for it to calm down usually isn't enough. It needs to relearn how to stabilise your pelvis properly through everyday movement.
An exercise programme may include:
Progressive hip abduction exercises
Single-leg stability work
Split squats
Core strengthening
Many people start with a few sessions with a physical therapist, who can tailor the exercise programmes and ensure correct technique. After that, most of the work continues at home, with occasional check-ins to adjust things as your strength and symptoms improve.
Activity modification
A common worry is being told to give up your sport or stop exercising completely. In most cases, this is not necessary.
Instead of complete rest, your doctor may recommend temporary physical activity adjustments, such as:
Reducing running distance or intensity
Avoiding hills or uneven surfaces
Limiting prolonged standing
Breaking up long periods of sitting
Small changes like these give irritated tissue room to settle while keeping you active enough to maintain your strength.
Pain management and support
In the early stages, short-term use of anti-inflammatory medication may help manage discomfort if recommended by your doctor. Applying ice after activity helps calm flare-ups, and gentle mobility work can stop stiffness from creeping in.
The aim isn't just to get through the day with less pain but also to create the right conditions for the tissue to heal.
Corticosteroid injections
If pain isn't responding after several weeks of consistent rehabilitation, a corticosteroid injection around the irritated tendon is sometimes recommended. It can bring down inflammation and make it easier to progress with strengthening exercises.
Gluteus medius pain can be frustrating because it gets in the way of ordinary things – walking, running, and even sleeping. But it's rarely a sign of anything serious. In most cases, it comes down to muscle strain, weakness, or imbalance, which usually responds well to appropriate treatment.
When to see a doctor
Most cases of gluteus medius pain aren't dangerous, and the discomfort tends to ease gradually as the muscle rebuilds strength and finds its balance again.
However, there are situations where it’s better to seek medical advice:
Pain is severe and sudden
You can't put weight through the leg
You have fever or unexplained swelling
Pain persists after several weeks of looking after it yourself
Getting assessed early can give you clarity and prevent manageable issues from becoming longer-term musculoskeletal problems such as chronic tendon irritation (gluteal tendinopathy), chronic low back pain, altered walking patterns, or reduced hip strength and stability over time.
If your hip or outer pelvic pain isn’t improving or is limiting your daily life, our specialists can help you identify the cause and tailor a personalised treatment plan. Request a consultation with Thomson Medical.
FAQ
How do you fix gluteus medius pain?
Gluteus medius pain is usually treated with:
Muscle-strengthening exercises
Activity modification
Short-term anti-inflammatory medication
Cortisone injection when needed
The goal is to restore your pelvic stability rather than simply resting completely.
Is walking good for gluteus medius pain?
Gentle walking is usually fine if it doesn’t significantly increase your pain. Long distances or uneven surfaces may need to be reduced temporarily.
What is the best sleeping position for gluteus medius pain?
Sleeping on your back or on the unaffected side with a pillow between your knees can reduce pressure on the irritated hip.
Can massage help gluteus medius pain?
Massage may temporarily relieve muscle tightness, but it doesn’t replace strengthening. It works best alongside a structured exercise programme.
What exercises should you avoid with gluteus medius pain?
Avoid high-impact running, deep single-leg squats, heavy side lunges, or exercises that sharply increase pain until your hip strength improves.
Can sitting cause gluteus medius pain?
Yes, prolonged sitting can contribute to gluteus medius pain. Sitting for long periods keeps the muscle underactive and slightly stretched, which can weaken it over time.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Medical Concierge
- 8.30am - 5.30pm
- WhatsApp: 9147 2051
Need help finding the right specialist or booking for a group?
Our Medical Concierge is here to help you. Simply fill in our form, and we'll check and connect you with the right specialist promptly.
Notice:
The range of services may vary between Thomson clinic locations. Please contact your preferred branch directly to enquire about the current availability.
Get In Touch