It’s hard not to feel your heart race a little when your child has a fever and a few red spots and suddenly refuses to eat because their mouth hurts. You may know this feeling all too well, especially after receiving a notice from their school that there's a case of hand, foot, and mouth disease (HFMD) in the class.
HFMD shows up a lot in babies and young children, especially those under 5. The good news is that it's usually mild and clears up on its own. Most children get better at home with the right care and a bit of patience. Let’s walk through what to expect and how you can help your child feel better, step by step.
What is hand, foot, and mouth disease?
Hand, foot, and mouth disease (HFMD) is a viral infection that mainly affects babies and young children. That's why you often see outbreaks at childcare settings such as nurseries, preschools, and daycare centres.
HFMD is caused by a group of viruses called enteroviruses. It’s not caused by poor hygiene or anything you did wrong. Even the most careful families deal with it because young children often share toys, touch surfaces, and put their hands in their mouths.
How to recognize HFMD symptoms
Many parents first notice that their child seems more tired, clingy, or irritable than usual. This often happens before any symptoms show up. After that, other signs begin to develop.
Common symptoms usually include:
Fever
Sore throat
Painful mouth ulcers or blisters
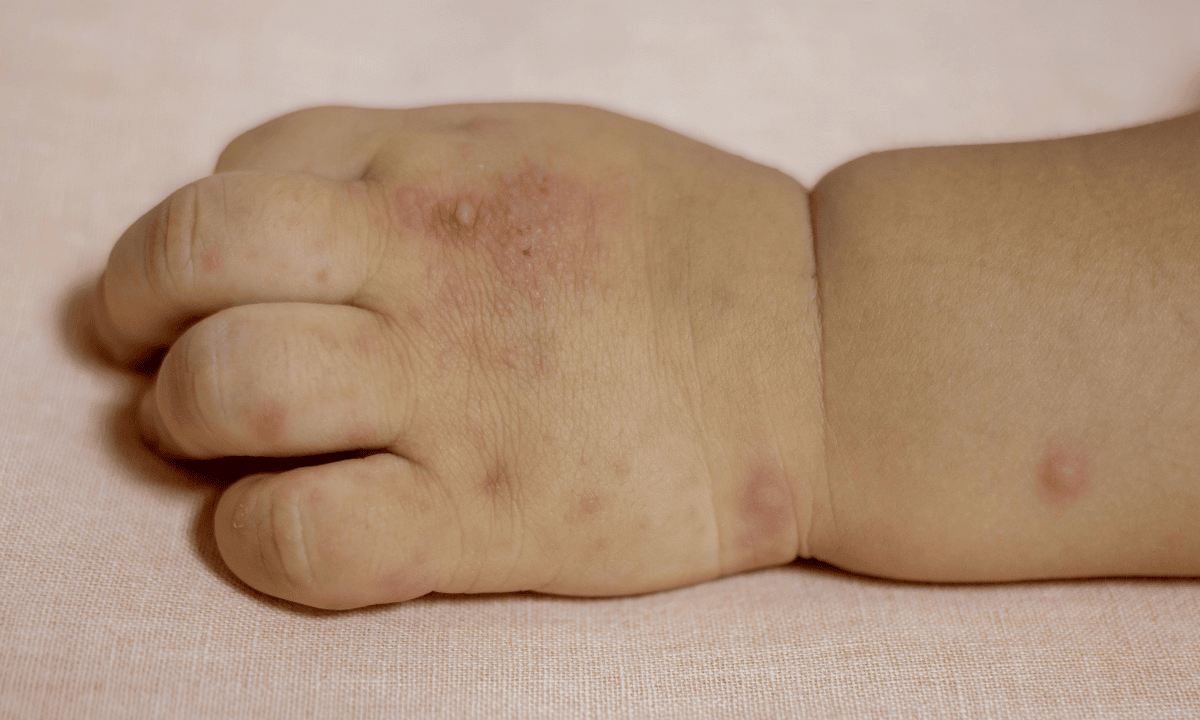
A rash or small red spots on hands, feet, buttocks, or legs
Reduced appetite because swallowing hurts
These mouth sores can be one of the most difficult symptoms to deal with. Your child may refuse food or drinks because it stings. This can feel worrying, but it’s a typical part of HFMD and usually settles as the illness runs its course.
Is HFMD serious?
For most children, HFMD is uncomfortable but not dangerous. It behaves a bit like a bad cold that comes with a rash. Your child may feel miserable for a few days, but their body clears the virus on its own.
In many cases, the illness:
Improves with rest and fluids
Doesn’t need special or antiviral medication
Heals without long-term problems
Leaves no scars
Most children recover smoothly at home, but as a parent, you may be wondering when it's time to check in with a doctor.
When to see a doctor
Contact your paediatrician if you notice:
Your child refuses to drink or has very little urine (possible dehydration)
Persistent high fever (more than 3 days)
Extreme sleepiness or unusual drowsiness
Repeated vomiting
Severe headache or neck stiffness
Symptoms that don't improve after about 10 days
During the visit, your paediatrician can usually recognise HFMD by examining the rash and asking about your child's age and symptoms. In most cases, a simple check-up is all that's needed for reassurance.
Sometimes, your doctor may take a small throat or stool sample for testing, though this isn't always necessary. The point is to confirm what's happening and make sure your child gets the right care.
Our paediatricians can assess your child and provide clear, practical advice, so you won't have to second-guess. If you would like a further evaluation, don't hesitate to request a consultation with Thomson Paediatric Centre.
Our paediatricians in Singapore
Loading...
Home care for HFMD
Watching rashes spread across your child's skin while they refuse to eat because their mouth hurts is really tough. And there's no medicine that will clear it up overnight.
But you can help your child feel better at home while they recover.
Pain and fever management
Fever and mouth sores make children feel uncomfortable. When the pain eases, your child may find it easier to drink, eat, and rest.
You can use age-appropriate fever or pain relief medications, such as paracetamol or ibuprofen, as advised by your doctor. These medications don't cure the virus, but they can lower fever and reduce soreness.
Try offering medicine about 30 minutes before meals. When the pain is under control, your child may be more willing to drink or eat a little.
Keeping your child hydrated with mouth sores
With mouth sores and fever, your child may not feel like drinking, but their body loses fluids faster than usual. Consuming fluids regularly helps prevent dehydration, keeps their energy up, and supports their body as it heals.
You can try:
Small, frequent sips of water
Cold milk or chilled formula
Oral rehydration solutions
Ice chips or ice pops
Smoothies or cold yogurt drinks
Remember that cool or cold fluids often feel better on sore mouths than warm drinks.
Food that won’t hurt sore mouths

Eating with mouth ulcers is uncomfortable, so softer, cool or room-temperature foods with mild flavours work better.
Good options include:
Porridge or oatmeal
Soup or broth
Mashed potatoes
Scrambled eggs
Yogurt or pudding
Tofu
Bananas
Smoothies
Try to avoid:
Spicy food
Salty food
Fried food
Acidic food like citrus or tomato
Don't worry too much if your child eats less for a few days. An appetite usually returns once the mouth heals. Offer small amounts more often rather than full meals.
Soothing skin rashes
HFMD rashes often look worse than they feel. Many children aren’t very bothered by them but keeping the skin cool and clean helps prevent irritation.
You can try:
Dressing your child in loose, lightweight, cotton clothing
After bathing, gently patting the skin dry instead of rubbing
Avoiding thick or oily creams that trap heat and moisture.
Keeping nails short and clean to prevent scratching and possible infection
Although the rash may appear concerning, it commonly improves on its own as your child recovers. With gentle skin care and a bit of patience, these spots typically clear without the need for specific treatments.
Creating a calm, comfortable environment
When children feel sick, they often want to be close to you. Your presence matters just as much as any treatment.
You can help your child feel better by:
Keeping the room cool and well-ventilated
Offering extra cuddles and reassurance
Reducing active play while they’re unwell
Gentle routines, quiet play, and additional rest can help your child feel more at ease while their body recovers. It is reasonable for normal activities to slow down for a few days during illness.
How long does HFMD last?
When your child is sick, time feels slower. It is common for parents to wonder when things will start to improve.
Most children follow a similar timeline:
Fever: 2-3 days
Mouth sores and rash: 5-7 days
Full recovery: about 7-10 days
Once the fever breaks and your child starts eating and playing again, these are reassuring signs that they are getting better.
When can a child go back to school after HFMD?
If you're a working parent, you're probably juggling childcare leave, rearranging meetings, and wondering how long you need to stay home. You also don't want to send your child back too early and risk them feeling unwell or spreading the virus to their classmates.
In Singapore, most preschools and childcare centres follow Ministry of Health (MOH) and Early Childhood Development Agency (ECDA) guidelines. Children with HFMD should stay home until they're feeling better and symptom-free.
Some preschools and childcare centres may ask for:
A doctor's memo or medical certificate
At least 24 hours without fever
Dry or healed blisters
No new rashes appearing
By this point, your child is much less likely to spread the virus and usually feels well enough to join class again. Even after your child goes back, you might notice some mild skin peeling or fading marks. This is normal healing and doesn't mean they're still contagious.
Policies can vary between preschools and childcare centres, so it’s always helpful to check directly with your child's school for their specific requirements.
How to stop HFMD from spreading at home

Caring for one sick child can be tiring. Managing two or three children with fever, mouth ulcers, and rashes at the same time can get overwhelming fast.
The reassuring part is that you do not need extreme cleaning measures or strict household rules to stop this. Simple daily habits go a long way in reducing the risk of spreading HFMD.
Hygiene measures that work
HFMD mainly spreads through saliva, nasal discharge, stool, and fluid from blisters. That’s why hand hygiene practices play an important role.
Helpful practices include:
Washing hands thoroughly with soap and water, especially after diaper changes, toilet trips, and before meals
Cleaning toys, high-touch surfaces, and tabletops daily
Avoiding sharing cups, utensils, towels, or toothbrushes
Covering coughs and sneezes, then wash hands
These small routines may seem simple, but they can make a difference in slowing down the spread.
Protecting siblings and family members
Where practical, it may help to give your sick child their own utensils, towel, and sleeping space for a few days. You don't need strict isolation, but a little temporary separation can help reduce the chance of spread.
If siblings are old enough, remind them to wash their hands often and avoid touching their faces after playing together.
Importantly, be kind to yourself. Even with careful hygiene, HFMD can still spread within families because the virus is very contagious. Getting sick doesn't mean you weren't careful enough – it just means you're dealing with a common childhood illness.
Most children recover smoothly from HFMD with time and gentle care. But if you ever feel unsure, worried, or simply need peace of mind, our paediatricians are here to support you and your family every step of the way. Request a consultation with Thomson Paediatric Centre.
FAQ
How long is HFMD contagious?
HFMD is most contagious during the first week of illness, but the virus can still spread even before symptoms appear during the incubation period (usually 3–7 days). Some children may continue shedding the virus in stool for several weeks, which is why good hygiene remains important even after they feel better.
What is the cause of HFMD?
HFMD is caused by a group of viruses called enteroviruses, most commonly coxsackievirus and sometimes enterovirus 71. These viruses spread easily among young children through close contact.
Can adults catch hand, foot, and mouth?
Yes. Although it’s more common in children, adults can still catch HFMD because it is a viral disease. Symptoms in adults are often milder, but they can still spread the infection to others.
How do you treat HFMD?
There’s no specific cure for HFMD, as your child’s body clears the virus on its own. Treatment focuses on:
Managing fever and pain
Keeping your child well hydrated
Offering soft foods
Allowing plenty of rest
How to avoid getting HFMD from your child?
HFMD spreads through respiratory droplets, saliva, and stool. Practising good personal hygiene, such as frequent handwashing, cleaning toys and surfaces, and avoiding sharing utensils or towels, can significantly reduce the risk of infection.
Can HFMD lead to any complications?
Most cases are mild and recover fully. Complications such as viral meningitis or temporary nail loss can occur, but these are uncommon.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice for your little one's unique situations, request a consultation with Thomson Paediatric Centre.
