Finding out you need a mastectomy can feel overwhelming, and it is natural to have many questions about what lies ahead. You may be wondering what the surgery actually involves, how your body will be affected, or how long it will take to get back to your normal routine.
Every person's experience with a mastectomy is different, and the path leading to this surgery will not be the same for everyone. What remains consistent is that understanding the procedure, the preparation, and what recovery looks like will help you feel more confident at every stage.
What is a mastectomy?
A mastectomy is an operation that removes breast tissue from one or both of your breasts. It is performed by a breast surgeon in a hospital setting and is carried out under general anaesthetic.
Depending on your diagnosis, the amount of tissue removed can vary. In some cases, only your breast tissue is removed, while in others, your nipple, surrounding skin, or nearby lymph nodes may also be included. Knowing what the surgery involves can help you feel more prepared for the conversations ahead with your surgical team.
Who may need a mastectomy?
A mastectomy may be recommended if your tumour is large, affects multiple areas of your breast, or if there is a higher chance of the cancer coming back if some breast tissue is left behind.
Your doctor may discuss this surgery with you if you:
Have been diagnosed with breast cancer
Carry certain gene mutations such as BRCA1 or BRCA2, which increase your lifetime risk of breast cancer
Previously received radiation therapy to your chest area
Have a non-cancerous but high-risk breast condition
Have a strong family history of breast cancer
A mastectomy is not always for advanced cancer, as removing your breast tissue at an early stage can sometimes offer better long-term protection. If you carry a gene mutation such as BRCA1 or BRCA2, it does not mean you will definitely develop breast cancer, but your risk is higher than average, which is why some people choose a preventive (prophylactic) mastectomy.
Your doctor will explain the reasoning behind their recommendation so you can feel confident in the decision.
Our breast cancer specialists in Singapore
Loading...
What are the different types of mastectomy?
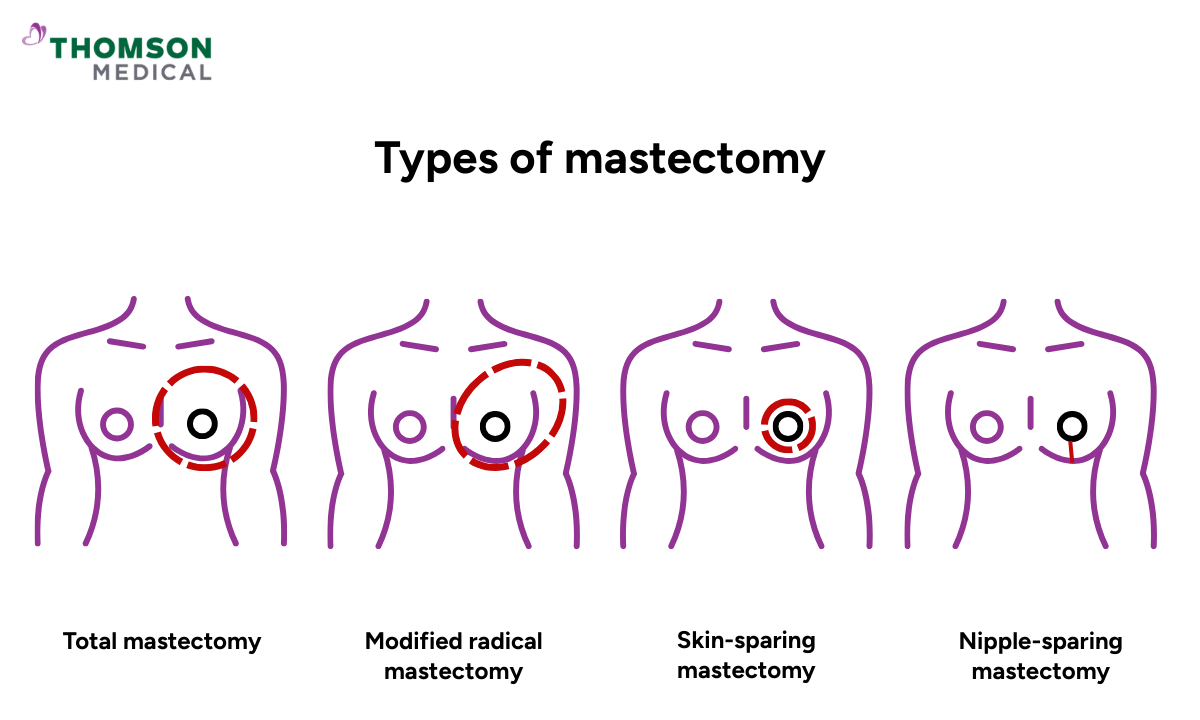
The type of mastectomy recommended for you will depend on the size and position of your cancer, whether it has reached nearby lymph nodes, and whether you are planning breast reconstruction.
Total mastectomy
This removes all of your breast tissue, breast skin, nipples, and areolas (the darker area of skin around the nipple).
Modified radical mastectomy
This is similar to a total mastectomy but also removes most or all of your underarm lymph nodes. It is often recommended when there is a higher chance that cancer has reached your lymph nodes.
Skin-sparing mastectomy
This removes all of your breast tissue, nipple, and areola but keeps most of your breast skin intact. Preserving the skin creates a natural pocket that can be used during reconstruction, which often leads to a more natural-looking result for you.
Nipple-sparing mastectomy
This removes all of your breast tissue while keeping your breast skin, nipple, and areola. It tends to offer the most natural appearance after reconstruction, though it is only suitable in certain situations depending on the position and size of your cancer.
In some cases, more than one type of mastectomy may be suitable for you, which means you may have a choice. It is worth asking your surgeon whether breast reconstruction can be done at the same time as your mastectomy, as this can influence which surgical approach is used.
If you are considering a mastectomy, it’s important to understand which type best suits your diagnosis and reconstruction goals. Request an appointment with the Thomson Breast Centre to discuss the suitable mastectomy option for you and explore breast reconstruction choices tailored to your needs and preferences.
How do you prepare for a mastectomy?
Being prepared ahead of surgery can make the experience feel a little less overwhelming. A few days or weeks before your operation, you will usually have a pre-surgery appointment to check your general health.
Your doctor may arrange one or more of the following tests:
It helps to write down any questions beforehand so you do not forget anything important.
There are also a few things you will need to do before your surgery date:
Do not eat or drink for up to 6 hours before the operation, as this allows the anaesthetic to work safely.
Stop smoking a few weeks beforehand if you can, as it slows down wound healing and increases your risk of complications.
Wear compression socks. These reduce the risk of a blood clot forming in your legs while you are walking less.
Letting your surgical team know about any medications you are currently taking is also important, as some may need to be paused before the operation (for example, blood thinners and certain supplements may interfere with the surgical procedure or recovery).
What happens during the operation?
You will be under general anaesthetic throughout, which means you will be asleep and will not feel or remember anything during the procedure. How long you will be in surgery depends on what is being done.
Here’s what to expect:
Removing one breast usually takes around one and a half hours
Removing both breasts can take around 3 hours
Having breast reconstruction at the same time means you can expect to be in surgery for around 4 to 6 hours
During surgery, your surgeon will make an incision from the armpit toward the centre of your chest. The amount of tissue removed will depend on the type of mastectomy you are having. Your surgeon will carefully plan this in advance based on what is appropriate for your treatment.
What happens after the operation?
After surgery, you will be moved to a recovery room where your care team will monitor you closely. You will be given medicine to manage pain and swelling. If needed, you may also receive fluids through a drip in your arm. Once you are stable and comfortable, you will be moved to a ward to rest.
Your length of stay will vary:
For a straightforward mastectomy, you may be able to go home the same day or within 1 to 2 days
If you had reconstruction at the same time, you will likely need to stay for a few days longer
Your team will also consider whether any surgical drains are still in place and how well your pain is being managed before you are discharged
Before you go home for recovery, your nurse will explain how to care for your wound and which symptoms to watch out for. Recovery after a mastectomy is a gradual process, and it is important to be patient with yourself.
Many people feel well enough to return to everyday activities within around 3 weeks, though full wound healing can take up to 6 weeks. It’s normal to feel tired and sore during this time as your body recovers.
What complications can a mastectomy cause?
A mastectomy is a major operation, and like any surgery, it carries some risks. Many people recover without serious issues, but complications can sometimes occur in the days or weeks after you go home. Knowing what to watch for means you can contact your care team quickly if something does not feel right.
Possible complications include:
Bleeding from the wound
A build-up of fluid around the wound (known as seroma)
Infection
Painful scarring
A blood clot that forms in the leg
Numbness or reduced feeling in your arm
Reduced movement in your shoulder (frozen shoulder)
Swelling caused by fluid build-up (lymphoedema)
When complications are identified early, they can often be treated more effectively. Contact your care team if you notice increasing pain, redness, swelling, fever, or anything else that concerns you after surgery.
A mastectomy is a significant surgery, but for many people it is also the step that brings them closer to recovery. Understanding what the procedure involves, knowing what to expect at each stage, and being aware of the support available to you can make the journey feel more manageable.
How much does a mastectomy cost in Singapore?
Thinking about the cost of surgery is a natural part of planning ahead, and knowing what to expect can take some of the stress out of the process.
At public hospitals in Singapore, a subsidised mastectomy typically costs around SGD 1,744 to 3,860. At private hospitals, the inpatient bill for a mastectomy is around SGD 32,497.
On top of the hospital bill, fees may include:
Surgeon fee: SGD 6,649 to SGD 13,080
Anaesthetist fee: SGD 1,962 to SGD 2,616
Daily doctor attendance: SGD 230 to SGD 450 per day
These figures are based on a standard mastectomy with lymph node removal. Costs may be higher depending on the complexity of your surgery, whether breast reconstruction is done at the same time, and the length of your hospital stay.
If you have health insurance, your policy may help cover a portion of the costs. It is worth checking with your insurer before the procedure so you have a clear picture of what you will need to pay out of pocket.
Bill amounts are intended as a general guide by the Ministry of Health Singapore. Actual costs may vary depending on your condition, treatment plan, and choice of hospital. Please check with your hospital for a more accurate estimate.
Costs can feel overwhelming on top of everything else you are navigating. Request an appointment with the Thomson Breast Centre to get a clearer picture of what your surgery may involve and receive a more accurate cost estimate based on your individual situation.
FAQ
Can I keep my nipple during a mastectomy?
In some cases, yes. A nipple-sparing mastectomy preserves the nipple and surrounding skin, but it is only suitable depending on the size and position of the cancer. Your surgeon will advise whether this is an option for you.
What is the difference between a mastectomy and breast-conserving surgery?
Breast-conserving surgery removes only the tumour and a small area of surrounding breast tissue, while a mastectomy removes the entire breast. Your surgeon will recommend the appropriate option based on your diagnosis.
Will I need radiation therapy after a mastectomy?
Not always. Whether you need radiation treatment afterwards depends on factors such as the cancer stage, lymph node involvement, and your overall treatment plan. Your oncologist will discuss this with you.
Can breast reconstruction be done at the same time as my mastectomy?
Yes, in many cases, reconstruction surgery can be performed immediately after the mastectomy. Options include implants or autologous tissue reconstruction, which uses your own skin, fat, or muscle. A plastic surgeon will walk you through your reconstruction options.
What is a prophylactic mastectomy?
A prophylactic mastectomy, sometimes called a risk-reducing bilateral mastectomy, is a preventive surgery for people at high risk of developing breast cancer, such as those with a BRCA gene mutation or a strong family history. It is not a treatment for existing cancer but a way to significantly reduce the risk of it developing.
Will I need hormone therapy after a mastectomy?
This depends on the type of breast cancer you have. If your cancer is hormone receptor-positive, meaning it grows in response to oestrogen or progesterone, your doctor may recommend hormone therapy as part of your treatment plan after surgery. Your oncologist will discuss whether this applies to your situation.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, request an appointment with Thomson Breast Centre today.
Reference:
Ministry of Health Singapore. (2023). SA824B - Breast, tumor (malignant various lesions), simple mastectomy with axillary clearance, with/without sentinel node biopsy. https://www.moh.gov.sg/managing-expenses/bills-and-fee-benchmarks/cost-financing/tosp-sa824b-bill-information
