Being told you need laparoscopic surgery can bring up a lot of questions. It's natural to want to understand exactly what you're signing up for.
Asking the right questions before your operation can make a real difference. It helps you understand what to expect, how to prepare, and what recovery will look like, so you can walk into the operating room feeling informed rather than overwhelmed.
What is laparoscopic surgery?
Laparoscopic surgery, also known as keyhole surgery, is a minimally invasive procedure that allows your doctor to see inside your abdomen or pelvis through a few tiny incisions rather than one large cut.
Laparoscopic surgery is usually used for:
Gastrointestinal surgeries:
Such as removal of the appendix or gall bladder, hernia repair, gastric bypass surgery, and colonic surgeries.
Gynaecological surgeries:
Such as fibroid or cyst removal, endometriosis treatment, ectopic pregnancy removal, tubal ligation and reversal, and vaginal reconstruction surgery.
Urological surgeries:
Such as urethral reconstruction, kidney, or prostate surgeries.
Other procedures:
Such as biopsies, small tumour removal, and testicle correction (orchidopexy).
Once you have a clear picture of what laparoscopic surgery involves, you'll be in a much better position to ask the right questions and get the answers that matter most to you.
Why laparoscopic surgery is recommended
Compared to traditional open surgery, laparoscopic surgery often involves less tissue disruption. Because it uses smaller incisions, you may find recovery feels more manageable than you expected.
Here is what that can mean for you:
Smaller scars
Less bleeding during the procedure
Lower risk of wound infection due to smaller incision sites
Less pain during recovery and a reduced need for pain relief
Faster return to normal activities
It is also worth knowing that laparoscopy can serve two purposes in one procedure. Your doctor may use it to confirm a diagnosis and, if needed, treat the problem at the same time. This is why it may be recommended even if you have already had imaging done.
That said, everyone responds differently. Your doctor will assess your condition and discuss whether these benefits apply to your specific situation.
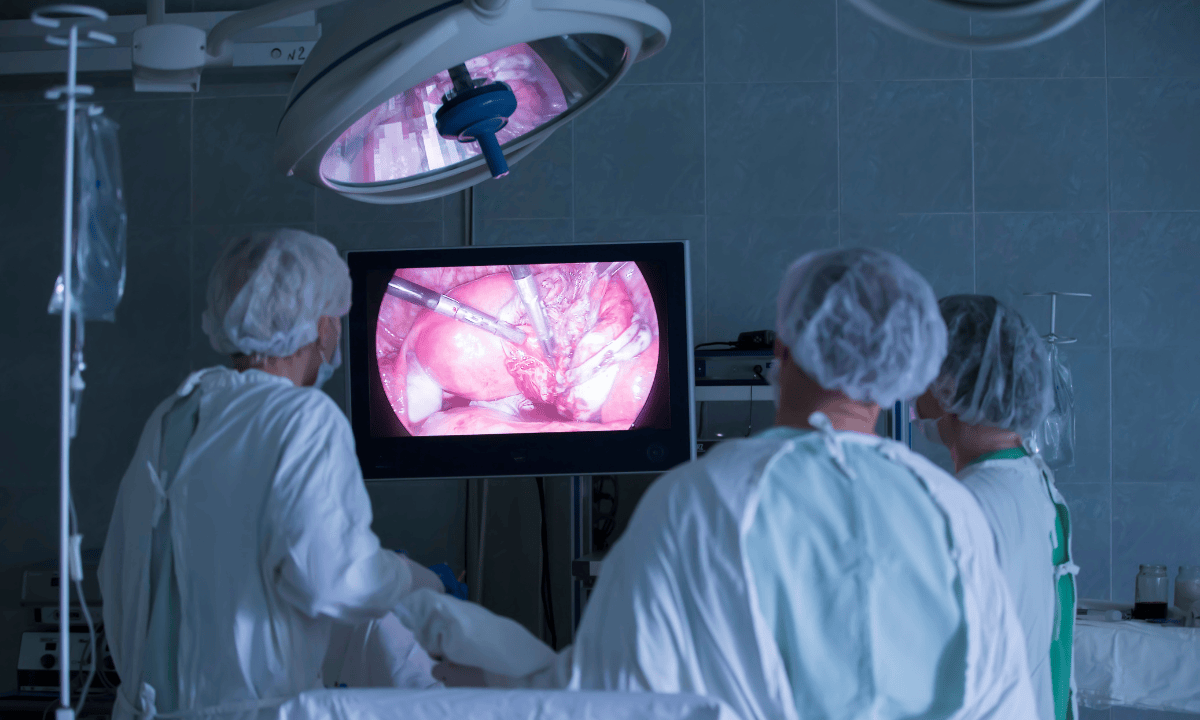
How the surgery will be performed
First, you will lie comfortably on the operating table with your head slightly tilted lower than your feet. Your anaesthetist will then use general anaesthesia to put you into a deep and painless sleep.
Here’s what your doctor will do next:
Create space:
Your doctor will make a small incision near your belly button or just below your rib cage.
Through this incision, they’ll gently fill your belly with gas via the gas tube.
This creates space inside so your doctor can see and work more clearly.
Insert tools:
Your doctor will then remove the gas tube and insert a laparoscope through the same incision.
They may make other incisions on your belly to insert other surgical instruments to look at other organs.
Guide the procedure:
The laparoscope feeds live images to a monitor, so your doctor can have a real-time view and guide their movement.
Once the procedure is done, they will release the gas from your body and close the incision.
The whole surgery may take up to 3 hours, depending on the complexity of the surgery.
What are the alternatives to laparoscopic surgery?
Laparoscopic surgery isn’t the only option available. Based on your condition, your doctor may consider one of the following alternatives:
Hysteroscopic surgery:
Your doctor uses a hysteroscope, which is a viewing instrument, to look into and treat conditions related to your cervix and uterus.
Robotic surgery:
This is similar to laparoscopy, but your doctor will control the instruments remotely using a computer, guided by a 3D monitor.
This allows more precise movements and smaller cuts, which can mean faster healing.
Open surgery:
It is often needed for complex issues such as large tumours, organ transplants, or emergencies such as trauma or appendicitis that require direct and wider access.
Open surgery offers better visibility and control than minimally invasive methods like laparoscopic. But recovery tends to be longer.
Your doctor will guide you toward the option that is suitable for your specific condition and overall health.
Possible complications
Like any surgical procedure, laparoscopic surgery carries some risks.
Possible complications can include:
Bleeding
Infection
Injury to nearby structures or blood vessels
Complications from anaesthesia
Abdominal swelling
Blood clots that can travel through your legs (deep vein thrombosis) or lungs (pulmonary embolism)
These complications are uncommon, but it’s important to be aware of them so you know what to watch out for during recovery.
Anaesthesia options
For most laparoscopy procedures, you’ll be under general anaesthesia. This means you’ll be in deep sleep and won’t feel anything throughout the surgery. Before the procedure begins, your doctor will insert a breathing tube to keep your airway safe and protected.
In some cases, regional anaesthesia, such as epidural or spinal anaesthesia, may be used. This numbs the lower part of your body rather than putting you fully to sleep.
Regional anaesthesia offers benefits like better pain control and a faster recovery. But it carries a risk of hypotension (low blood pressure), so it isn’t commonly used for laparoscopic surgery.
If you have questions about your upcoming laparoscopy or want to better understand your options, schedule an appointment with Thomson Medical. Our specialists will walk you through every step of the process and make sure you feel confident and informed before your surgery day.
Gynaecologists at Thomson Medical
Loading...
What should I ask before laparoscopic surgery?
Surgery can feel like a lot to take in, but preparing ahead of time can ease your uncertainty. The more informed and ready you are, the smoother your experience is likely to be, from the moment you arrive at the hospital to the day you head home.
Are there any foods I should avoid before the surgery?
What you eat and drink in the days before your surgery is more important than you may think. Your doctor will give you specific instructions based on your surgery and the type of anaesthesia.
Here’s what you can expect:
Alcohol:
You should avoid alcohol at least 24 hours before surgery, as alcohol may slow down your recovery, interfere with your anaesthesia, and increase the risk of bleeding and dehydration.
Smoking:
You should ideally stop smoking 4 to 6 weeks before surgery to reduce complications such as bleeding, infection, poor healing, and breathing problems.
Solid foods:
You will need to stop eating solid foods 8 hours before surgery. This includes solid, rich, fatty, or heavy foods, snacks, or even chewing gum.
Dairy products:
You should avoid milk, yoghurt, or smoothies at least 6 hours before surgery. Dairy products take a longer time to digest and can increase the risk of complications under anaesthesia.
Clear fluids:
You can drink water, clear broths, apple juice, black coffee, and tea up to 2 hours prior to surgery.
Your last meal:
For the last meal prior to surgery, opt for light and easy-to-digest foods.
If you’re unsure what to eat and what to avoid, don’t hesitate to ask your doctor.
What kind of medication should I avoid?
Some medicines can increase the risk of bleeding or interfere with anaesthesia, so it’s important to know which ones to pause and when.
Before laparoscopic surgery, your doctor may advise you to avoid:
Blood thinners:
Such as aspirin, clopidogrel, and warfarin (usually at least one week before surgery).
NSAIDs:
Such as ibuprofen and naproxen (usually 7-10 days prior to surgery).
Herbal supplements:
Including vitamin E, ginkgo, garlic, and ginseng.
Specific diabetic medications:
Such as insulin, dapagliflozin, and empagliflozin.
Antacids:
Such as antacids (usually on the day of surgery).
You should always confirm with your doctor first about the medications that you are taking now so they can provide personalised advice on when and how to stop and when it's safe to resume after surgery.
Are there any tests or assessments I need to do?
Before your surgery, your doctor will perform a comprehensive preoperative assessment to make sure you’re ready to undergo the procedure. This usually includes:
Medical history:
Your doctor will ask about your health background, previous surgeries, and any existing conditions.
Physical examination:
Your doctor may do a general check of your overall health.
You may be recommended a full blood count (CBC) to check for infection and anaemia, a kidney function test (U&E), a liver function test (LFT), and clotting studies.
Imaging studies:
Depending on your surgery, imaging tests may be recommended to get detailed images of your pelvic and abdominal organs. Your doctor may also order a lung X-ray to assess your lung health.
Cardiac studies:
An electrocardiogram (ECG) may be used to assess your heart function, especially if you have a history of heart disease.
These tests help your surgeon recognise potential risks early and tailor your care accordingly, so you can go into surgery with the right support in place.
What should I pack before coming to the hospital?
It’s easy to forget things when you’re focused on the surgery. This checklist helps ensure you have everything you need for a comfortable stay:
Important documents:
Insurance
Medication lists
Medical records
Clothing:
Loose, comfortable clothes
Socks and slippers
Underwear
Eye masks
Personal items:
Toiletries
Water bottles
Devices:
Phone and charger
Earbuds or headphones
Before your surgery day arrives, make sure you've gone through each of these steps with your doctor. If anything is unclear, whether it's about your diet, medications, or test results, they are there to help you work through it.
What should I ask about the day of surgery?
Once your preparation is done, the next thing on your mind is likely the day itself. Let's take a closer look at what to expect and what to ask your doctor so you can feel ready when the day arrives.
How long will it take?
Laparoscopic surgery duration varies widely. Simple diagnostic laparoscopies can be done in 30 minutes. More complex procedures can take up to 3 hours.
The exact duration depends on the complexity of your condition, your overall health, and your doctor's approach. Your doctor will give you a more specific estimate at your pre-surgery consultation.
Will I be in pain?
Some discomfort after the laparoscopic procedure is completely normal. Here’s what you may experience in the hours after your procedure:
Pain:
You may experience pain around the small cuts for a few days. Your doctor may prescribe pain medication to keep you comfortable.
Sore throat:
If a breathing tube was used during surgery, you may have a sore throat. This usually resolves on its own within a day or two.
Bloating, cramps, or shoulder pain:
Since gas is used to inflate the abdomen, some of it could remain inside and cause these symptoms.
These symptoms are generally benign and typically subside within a day or two as your body absorbs the remaining gas.
If anything feels more severe or persistent than expected, it’s best to check with your doctor so they can assess and advise you accordingly.
What can I expect after the operation?
The first few hours after surgery are all about rest and recovery. Your doctor will monitor you closely and guide you through each step.
Here’s what you can expect:
Fatigue:
You may feel fatigued from anaesthesia, which is normal. Rest as much as you need.
Getting up and moving:
You can start walking once you no longer feel dizzy.
Eating and drinking:
You can start with clear fluids and light foods once you are able to tolerate them. Staying hydrated and eating well can support your body’s healing process.
Wound care:
You should keep your incision wound clean and dry to reduce the risk of infection.
Before you go home, your doctor will walk you through everything you need to know. If anything feels off once you're home, reach out to them for more guidance.
Is an overnight stay required?
Many people can return home on the same day of the surgery or the next day. That said, everyone's recovery is different, and your doctor will advise based on how you're feeling after the procedure.
What should I ask about recovery after laparoscopy?
Recovery looks different for everyone, and it's normal to have questions about what you can and can't do once you're home.
Many people recover well from laparoscopic surgery, and with the right guidance, you can support your body's healing every step of the way.
Are there any activity restrictions?
After surgery, your body needs time and space to heal. Here’s what you should keep in mind:
Move gently:
Short, gentle walks are encouraged a few days after surgery. They help with circulation and can speed up your recovery.
Avoid bending or stretching:
You should avoid movements that strain your abdomen for at least 4 to 6 weeks after the surgery.
Stair climbing:
Take it slowly and steadily until you feel stronger.
It’s important to listen to your body throughout this process. If something causes pain or discomfort, slow it down and check in with your doctor before pushing further.
When can I return to work, exercise, and driving?
Your recovery time will depend on the type of procedure you had and how your recovery progresses. The good news is that most people can return to their desk jobs in 1 to 3 weeks.
For exercise:
Swimming:
Gentle swimming is usually allowed 1 to 2 weeks after the surgery, but it depends on your surgery type.
High-impact exercises:
Jumping, lifting heavy weights, and running are not recommended for at least 4 to 6 weeks after the surgery.
Lifting:
You should avoid carrying anything heavier than 4.5 kg for at least 4 to 6 weeks after the surgery.
Driving should also be avoided for at least 24 hours after the surgery. Your doctor will give you a more personalised timeline based on your specific procedure and recovery.
Are there any diet recommendations and restrictions?
Your digestive system needs time to settle, so sticking to gentle, easy-to-digest foods in the first few weeks can help you feel more comfortable and heal more smoothly.
During this time, try to avoid:
Fatty or fried foods
Spicy foods
Cauliflower or broccoli
Cabbage or beans
Carbonated drinks
Instead, soups, steamed vegetables, lean protein, and plenty of water are nourishing options you can opt for. Small, frequent meals are also easier on your system than large ones.
As your recovery progresses, you can gradually return to your usual diet. If you're unsure what's right for your specific situation, your doctor can help guide you.
If you're unsure about what to expect during recovery or need personalised guidance after your laparoscopy, schedule an appointment with Thomson Medical. Our specialists are here to support your healing journey and address any concerns as they arise.
FAQ
Can endometriosis be treated laparoscopically?
Yes, laparoscopy may be used for both diagnosing and treating endometriosis. Surgeons can remove or destroy endometrial tissue through the same small incisions, offering significant pain relief and, in many cases, improved fertility.
How long is the recovery?
The recovery for laparoscopic surgery depends on the type of surgery, its complexity, and your overall health.
Generally, most people feel better within 1-2 weeks. Full recovery can take up to 3 weeks for simpler procedures or 6 to 8 weeks for complex ones.
What type of anaesthesia is used?
General anaesthesia is usually used for laparoscopic surgery. In some cases, regional anaesthesia, such as spinal or epidural anaesthesia, may also be involved for better pain control after surgery.
What tests are necessary before laparoscopy?
Your doctor will perform a thorough preoperative assessment, which includes blood tests, an electrocardiogram (ECG), imaging studies such as X-rays, and urinalysis.
What are the benefits of laparoscopy?
Laparoscopy offers benefits such as smaller scars, faster healing, shorter hospital stays, and a lower risk of bleeding and infection compared to open surgery.
Your doctor will advise on the most appropriate approach for your condition.
How fast does endometriosis grow back after a laparoscopy?
Endometriosis can grow back soon after surgery if the disease isn’t completely removed or if your ovaries aren’t suppressed. Your doctor will discuss long-term management options with you.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and advice based on your unique situation, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) - Jurong:
6262 8588 (Call), 6262 8588 (WA) - Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
Notice
The range of services may vary between TWC/TS locations. Please contact your preferred branch directly to enquire about the current availability.
Request an Appointment