If you have been waking up with deep joint pain that does not ease normally, it is understandable to feel concerned.
If this sounds familiar, you may be suffering from an issue known as rheumatic pain. Knowing the symptoms, possible causes, and available treatment options is a helpful first step towards seeking the right support and care.
What is rheumatic pain?
Rheumatic pain is a broad term doctors use to describe ongoing pain that affects your joints, muscles, bones and tendons.
It is more than a simple sports injury or a temporary strain. This type of pain is usually linked to long-term inflammation inside your body. In many cases, it is connected to various rheumatic diseases and autoimmune conditions, where your immune response mistakenly attacks healthy tissues, especially around the joints.
How rheumatic pain affects your joints and muscles
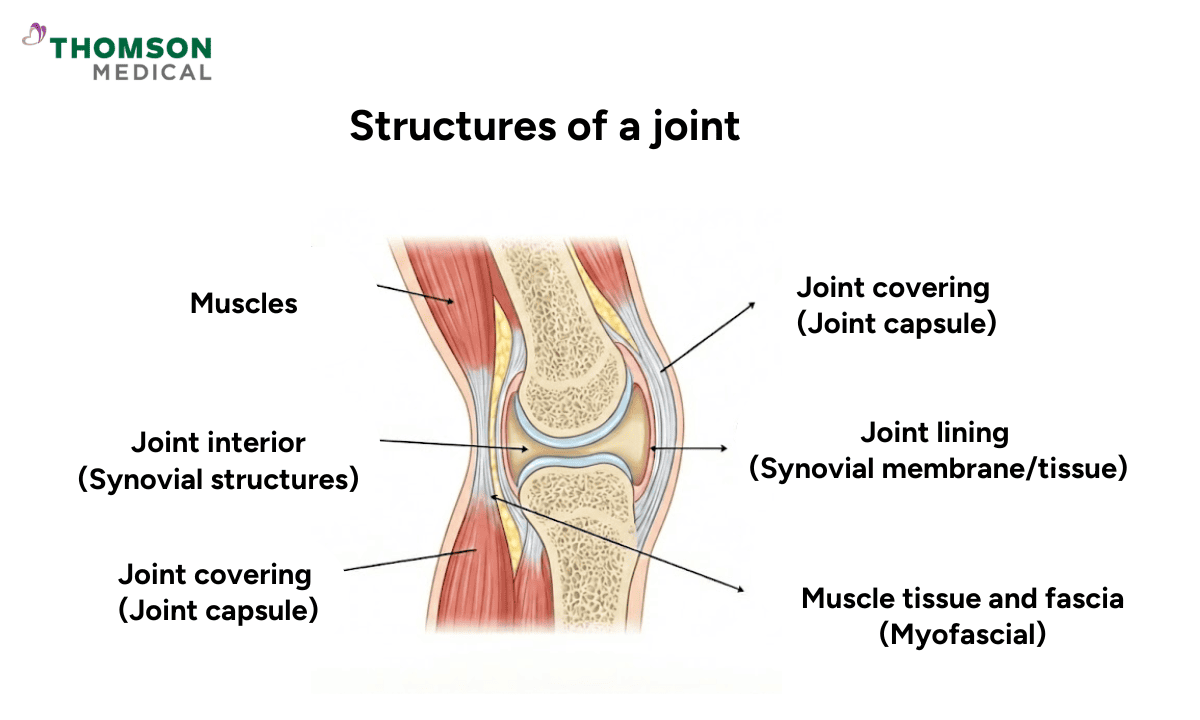
When inflammation flares up, here is why your body may feel stiff and sore:
Musculoskeletal pain:
You might feel a heavy ache in your muscles and bones.
It makes simple movements like walking uncomfortable.
Joint swelling and stiffness:
Your joints are lined with synovial tissue and supported by the joint capsule.
When these tissues become inflamed, excess fluid can accumulate inside your joint.
This leads to swelling, tightness, and stiffness.
Myofascial pain:
The irritation can spread to the thin tissues wrapping your muscles.
This is why a joint flare-up may make your entire body feel heavy and exhausted.
Living with ongoing pain can be exhausting. When inflammation continues for a long time, your nervous system can become more sensitive, which makes pain feel stronger and harder to ignore.
This is why early treatment matters. Addressing the problem sooner can help calm the inflammation and protect your joints.
What causes rheumatic pain?
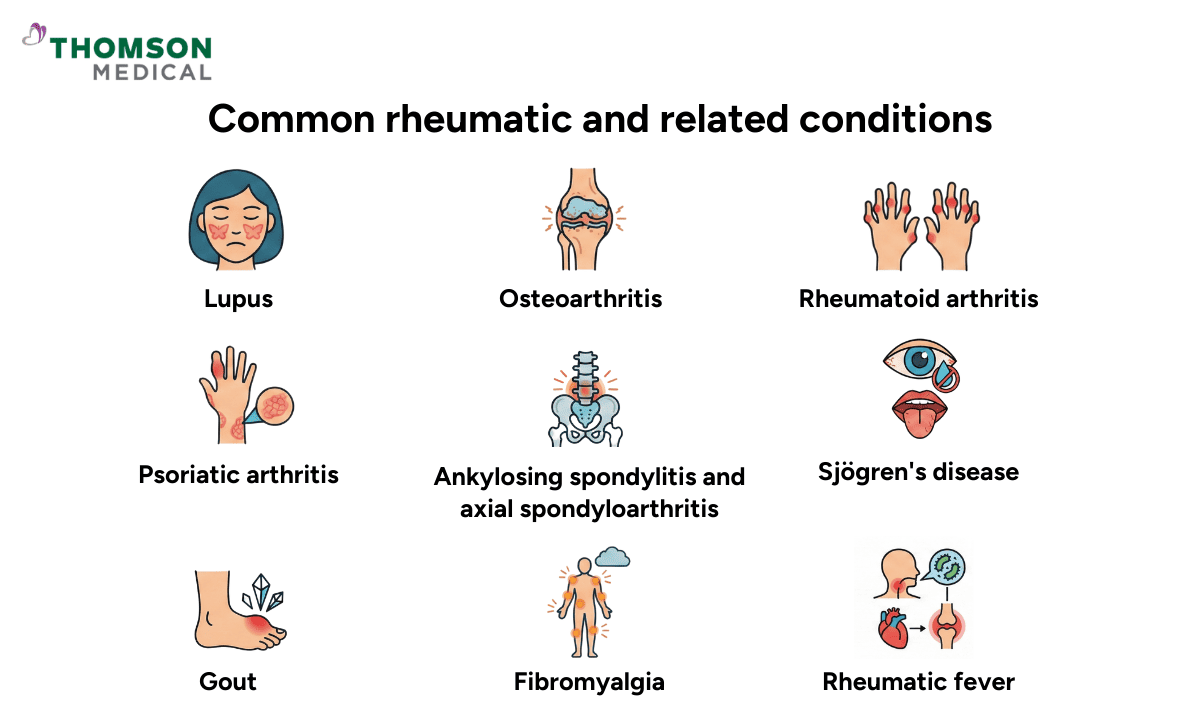
There are many different conditions that can cause rheumatic pain. While some involve autoimmune activity, others have different underlying causes. Although they may share similar symptoms, each condition affects the body differently and requires its own approach to treatment.
Rheumatoid arthritis
Rheumatoid arthritis is one of the most common inflammatory joint conditions. It usually begins in the smaller joints of your hands and feet.
You may notice:
Swollen, warm joints
Stiffness in the morning that lasts more than 30 minutes
Pain on both sides of the body, such as both hands or both feet
Ongoing fatigue
Rheumatoid arthritis doesn't just cause occasional flare-ups. If left untreated, the ongoing inflammation can lead to permanent joint damage. Catching it early can make a difference in protecting your hands, feet and everyday movement.
If you notice these symptoms lasting longer than usual, it is important to seek medical advice early. You may schedule a consultation with our specialists at Thomson Medical Centre for a proper assessment and timely management.
Osteoarthritis
Osteoarthritis is the most common joint condition overall. However, unlike autoimmune rheumatic diseases, it is not caused by the immune system. Instead, osteoarthritis develops gradually as the cartilage that protects the ends of your bones wears down from everyday use.
You may notice:
Joint pain that worsens with activity
Stiffness that improves within a short time after moving
Bony enlargement of joints, especially in the fingers or knees
Although osteoarthritis can occur alongside autoimmune conditions, the two have different causes and require different treatment. This is why it’s important to get an accurate diagnosis. Your doctor can help identify which condition is affecting you and what could help your situation.
Gout

Gout is different from autoimmune conditions. It happens when uric acid builds up in your blood and forms tiny, sharp crystals inside a joint.
You may notice:
Sudden, severe joint pain
Redness and swelling
A hot, very tender joint, often in the big toe
A gout attack can feel sudden and overwhelming, sometimes waking you up at night. The upside is that once uric acid levels are brought under control, these painful flares can often be prevented.
If you experience sudden, severe joint pain or repeated gout attacks, seeking medical advice early can help prevent future flares and joint damage. You may schedule a consultation with Thomson Medical Centre for a proper assessment and personalised treatment plan.
Ankylosing spondylitis and axial spondyloarthritis
These conditions mainly affect your spine and the joints that connect your lower back to your pelvis.
You may notice:
Deep, aching pain in your lower back or buttocks
Stiffness that feels worse in the morning or after long periods of rest
Pain that gradually improves once you start moving
Symptoms that begin before the age of 40 and develop slowly over time
If this inflammation is not treated, your back can become stiffer and less flexible over time. Simple movements like turning, bending, or even standing up straight may start to feel harder. Spotting the signs early allows you to get medical advice and begin treatment before the stiffness worsens.
Psoriatic arthritis
Psoriatic arthritis develops in some people who have psoriasis, a skin condition that causes red, scaly patches. This condition can affect different joints throughout your body, including the small joints in your fingers and toes, and sometimes even your spine.
You may notice:
Tender, swollen joints
Fingers or toes that become noticeably puffy or “sausage-shaped”
Joint pain that flares up at the same time as skin symptoms
Because both your skin and joints are involved, flare-ups can feel especially frustrating. Paying attention to how these symptoms connect can help you and your doctor find the right balance in treatment.
Lupus (Systemic lupus erythematosus)
Lupus, also known as systemic lupus erythematosus or SLE, is an autoimmune condition where your immune system can affect multiple parts of your body, not just your joints. It is more common in women and can look very different from person to person.
You may notice:
Joint pain and swelling
A facial rash, often across your cheeks and nose
Extreme fatigue
Sensitivity to sunlight
Mouth ulcers
Hair thinning
Unlike conditions that mainly affect one area, lupus can involve your skin, kidneys, heart, lungs and blood cells. Because symptoms can come and go, it is sometimes mistaken for other illnesses in the early stages, therefore requiring careful examination from your doctor.
Sjögren's disease
Sjögren's disease is an autoimmune condition where your immune system mistakenly attacks the glands that produce moisture.
You may notice:
Dry eyes
Dry mouth
Joint pain
Ongoing fatigue
Although dryness is often the most noticeable symptom, this condition can cause joint pain and make you feel generally tired.
Sjögren’s can also develop on its own, but it can also occur alongside other autoimmune conditions, such as rheumatoid arthritis or lupus. Letting your doctor know about all your symptoms, including dryness, fatigue, and joint pain, helps ensure nothing is missed.
Fibromyalgia
Fibromyalgia is not an autoimmune or inflammatory condition, but it is often seen alongside rheumatic diseases.
It is considered a central sensitisation syndrome, meaning your nervous system becomes more sensitive to pain signals.
You may notice:
Widespread body pain affecting both sides of the body
Persistent fatigue
Poor sleep
Brain fog or difficulty concentrating
There is no visible joint damage or inflammation on scans, but the pain is very real. Some people with rheumatoid arthritis, lupus, or other autoimmune conditions may also experience fibromyalgia-like symptoms, which can make their pain feel more intense.
Recognising this overlap helps make sure that treatment addresses both inflammation and pain sensitivity, if needed.
Rheumatic fever
Rheumatic fever is different from long-term rheumatic conditions. It can develop suddenly after an untreated streptococcal throat infection.
Even though it can also cause joint pain and swelling, the cause is different. It is a reaction to a bacterial infection, not a chronic autoimmune condition.
The inflammation can also affect other parts of your body, including the skin, brain, blood vessels, and your heart valves.
You may notice:
Joint pain and swelling
A high temperature
A skin rash
Unusual movements or weakness
Signs of heart involvement, such as chest discomfort or a heart murmur (an unusual sound heard during a heartbeat cycle)
Your support team will confirm the infection with a throat swab and treat it with antibiotics to prevent further complications.
How is rheumatic pain diagnosed?
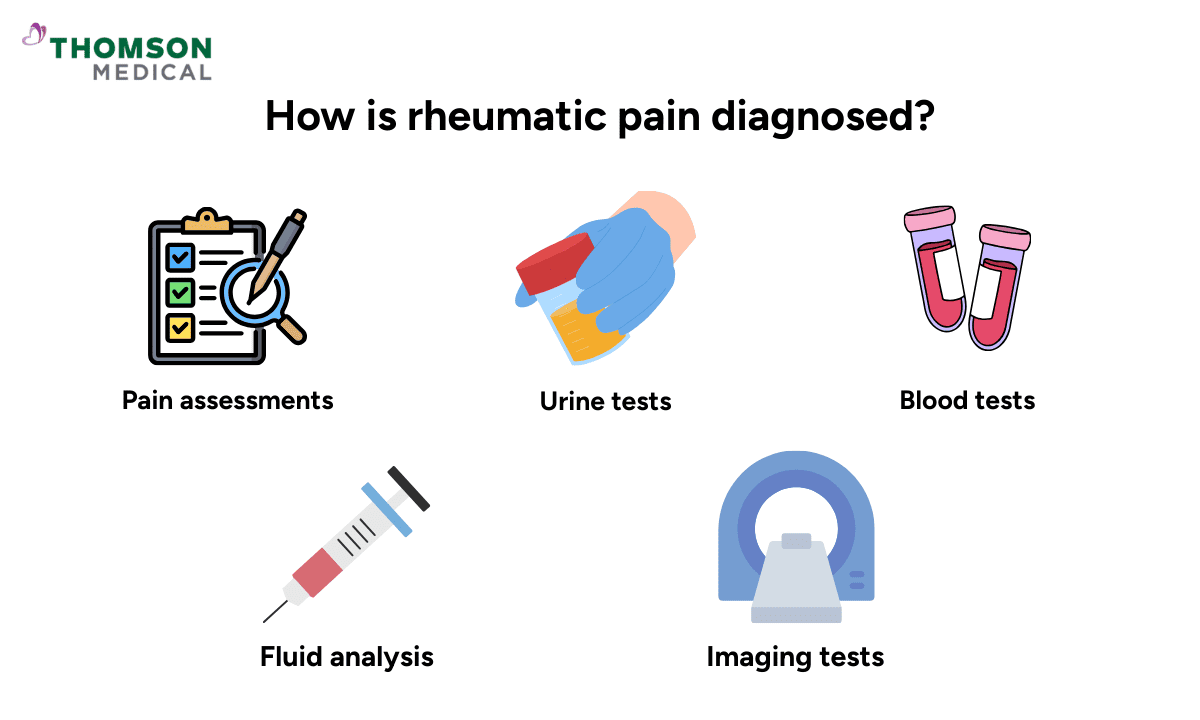
Figuring out exactly what is causing your pain can take time. Many rheumatic conditions share similar early symptoms, so your doctor will need to look at the full picture before making a diagnosis.
Your doctor will begin with a detailed discussion about your symptoms and a physical examination of your joints. If needed, further tests may be recommended.
Tests and assessments your doctor may use include:
Pain assessments:
You may be asked to rate your pain on a scale (visual analogue scales) or complete a short questionnaire (self-report scores).
This helps your doctor understand how severe the pain is and how much it is affecting you.
Urine tests:
These help assess kidney function, which can be affected in some rheumatic diseases such as lupus or gout.
Blood tests:
Some blood tests can look for signs of inflammation or certain markers linked to autoimmune conditions.
Two common tests are ESR (erythrocyte sedimentation rate) and CRP (C-reactive protein), which measure how much inflammation is present in the body.
Fluid analysis:
If a joint is very swollen, your doctor may use a fine needle to remove a small amount of fluid.
This can help check for uric acid crystals, infection, or inflammation.
Imaging tests:
All of these steps help your doctor piece together what is behind your symptoms. Once your doctor has all the test results in hand, they can develop a treatment plan suited to your needs.
If you are experiencing ongoing joint pain, swelling, or stiffness and are unsure of the cause, an early evaluation can help clarify your diagnosis. You may arrange a consultation with Thomson Medical Centre for a comprehensive assessment and personalised care plan.
How is rheumatic pain managed?
Living with ongoing pain can affect many parts of daily life. With the right support, however, symptoms can be managed and quality of life can improve.
Treatment often includes a combination of:
Medication:
Your doctor may prescribe medicines to help reduce inflammation and control the condition itself.
They can also help protect your joints over time.
Physiotherapy:
A trained specialist guides you through exercises such as stretching or low-impact aerobics.
These may help improve movement, strengthen muscles around your joints and reduce stiffness.
Occupational therapy:
This focuses on practical changes that make everyday tasks easier.
These include adjusting how you sit, lift or work so your joints are under less strain.
Managing rheumatic pain is usually a long-term process that involves working closely with your healthcare team. Following your treatment plan, staying active within your limits, and addressing symptoms early can make a meaningful difference.
When should you see a doctor?

As you grow older, it's completely understandable to feel overwhelmed by your ongoing joint swelling or deep muscle aches. However, such issues should not be dismissed as simply another unavoidable part of ageing.
You should consider seeing a healthcare professional if you notice:
Joint pain that lasts more than a few weeks without a clear cause, such as an injury or strain
Morning stiffness that takes longer than 30 minutes to ease
Joints that feel warm, look red, or appear visibly swollen
Pain accompanied by fatigue, unexplained weight loss, or fever
Discomfort that disrupts your sleep or daily activities
Getting inflammation checked and managed early can be helpful, as it may reduce the risk of joint damage and make symptoms easier to control over time.
Our orthopaedic surgeons
Loading...
Can you prevent rheumatic pain and flare-ups?
While you cannot always stop an autoimmune condition from developing, there are many proactive steps you can take to protect your joints, reduce inflammation, and prevent painful flare-ups.
Do gentle exercises such as swimming or walking to keep your joints flexible
Limit foods high in uric acid, like red meat and alcohol, to prevent gout attacks
Eat a balanced diet with plenty of vegetables and oily fish
Seek medical care for severe sore throats, especially in children, to prevent rheumatic fever
Avoid heavy lifting and repetitive strain where possible to protect your joints from unnecessary daily wear and tear
Try simple relaxation techniques such as deep breathing, stretching or light yoga to ease muscle tension
By making small, sustainable changes to your daily routine, you can play an active role in protecting your joints and reducing the likelihood of painful flare-ups. If your discomfort changes or becomes harder to control, speak with a healthcare professional who can help you find the right approach for long-term management.
FAQ
How do I know if my joint pain is a rheumatic disease?
Simple muscle strains usually improve within a few days with rest. Rheumatic conditions, however, tend to cause pain that lasts for weeks, comes with swelling or stiffness in the morning, or keeps returning.
If your joint pain feels persistent, affects both sides of your body, or is accompanied by fatigue, it’s a good idea to see a doctor for a proper evaluation.
What is the difference between arthritis and rheumatic pain?
'Arthritis' refers specifically to inflammation or wear and tear affecting the joints. Rheumatic pain is a broader term that can involve joints, muscles, and connective tissues. In other words, arthritis is one type of rheumatic condition, but not all rheumatic pain is arthritis.
Is walking good for rheumatic pain?
In most cases, yes. Once severe inflammation has settled, gentle activities such as walking can help keep your joints flexible and strengthen the muscles that support them. The key is to pace yourself and avoid pushing through significant pain.
Can rheumatic diseases be cured?
Most chronic rheumatic conditions cannot be completely cured. However, with early diagnosis and the right treatment plan, many people can control their symptoms and live full, active lives.
Can changing my diet help manage rheumatic pain?
Diet can play a supportive role. For example, reducing purine-rich foods is important if you have gout, as it helps lower uric acid levels. For other inflammatory conditions, a balanced diet rich in vegetables, whole foods, and omega-3 fats may help support overall health and reduce inflammation.
How long will I need to take my prescribed medication?
Many rheumatic conditions are long-term, so treatment is often ongoing. The goal is to keep the disease well-controlled and prevent joint damage, not just relieve pain temporarily.
Your doctor will monitor you regularly with blood and, when necessary, urine tests to make sure the medication remains safe and effective. Over time, doses may be adjusted so you stay on the lowest amount needed to keep your condition stable.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Medical Concierge
- 8.30am - 5.30pm
- WhatsApp: 9147 2051
Need help finding the right specialist or booking for a group?
Our Medical Concierge is here to help you. Simply fill in our form, and we'll check and connect you with the right specialist promptly.
Notice:
The range of services may vary between Thomson clinic locations. Please contact your preferred branch directly to enquire about the current availability.
Get In Touch