A burn can occur suddenly and may cause significant pain and distress, especially when the skin develops blisters or appears swollen. If you suspect a second-degree burn, it is natural to feel unsure about how serious it is and what steps to take next.
Second-degree burns affect deeper layers of the skin than minor burns and may require closer care depending on their size and location. While many heal well, some benefit from medical assessment to support recovery and prevent complications.
Understanding how second-degree burns happen, what symptoms to expect, and when to seek medical advice can help you respond calmly and ensure appropriate care.
What is a second-degree burn?
A second-degree burn, also called a partial-thickness burn, affects both the outer layer of your skin (the epidermis) and the layer beneath it (the dermis).
Unlike first-degree burns that only redden the skin's surface, second-degree burns penetrate deeper and cause blistering. This type of burn is painful because the nerve endings in the dermis layer are affected but not completely destroyed.
With attentive care, most second-degree burns will heal within two to three weeks, though deeper ones may need a bit more time.
Symptoms of second-degree burn
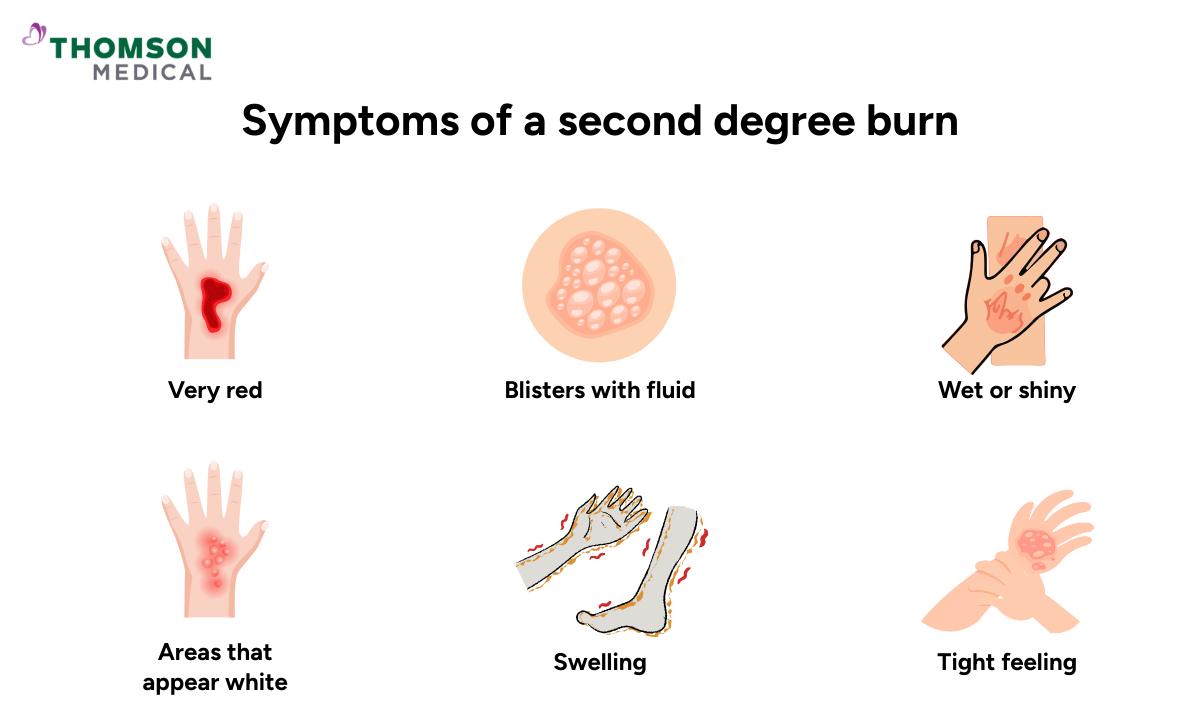
Knowing what to look for can help you assess the severity of a burn injury and decide on the right course of action. Second-degree burns have distinct characteristics that set them apart from other types of burns.
Here are some symptoms of second-degree burns:
Visible signs on your skins
When you have a second-degree burn, you'll notice several telltale signs that help identify what you're dealing with:
Very red or splotchy skin, with colour often more intense than a simple sunburn
Blisters filled with clear fluid, typically forming within a few hours
Wet or shiny appearance to the skin
Areas that appear white or discoloured
Noticeable swelling around the injury
Tight feeling in the skin around the burn
As healing begins, you may notice the top layer of skin starting to peel away. These visible changes are your body's way of responding to the injury.
How it feels
Pain is one of the most prominent features of a second-degree burn. You'll likely experience a sharp, throbbing pain that can be quite intense, especially in the first few hours after the injury. The area will be extremely sensitive to touch, air, and temperature changes.
Some people describe the sensation as feeling raw or exposed. This heightened sensitivity happens because the nerve endings in the dermis layer are irritated but still functioning.
When symptoms appear
Most second-degree burn symptoms develop immediately or within the first few hours after injury. Blisters may take a bit longer to form, sometimes appearing several hours after the initial burn. The pain is usually most intense in the first 24 to 48 hours and gradually improves with proper care.
Common causes of second-degree burns
Many second-degree burns occur in moments we least expect them, often during routine daily activities. Identifying these common scenarios will help you feel more prepared and protected going forward.
Heat-related burns
Scalding from hot liquids is one of the most frequent causes of second-degree burns, particularly in home settings. This might happen when hot tea, coffee, or cooking water spills onto your skin. Even brief contact with boiling water can cause significant damage
Direct contact with hot surfaces, such as cooking equipment, heated styling tools, or hot metal, can also result in second-degree burns. Steam burns are particularly common in kitchens and can be deceptively severe, as steam carries a great deal of heat.
Flames from candles, fireplaces, or cooking accidents can quickly cause second-degree burns. Even a moment's contact with an open flame can damage both layers of your skin.
Chemical burns
Certain household chemicals can cause second-degree burns when they come into contact with your skin. Strong cleaning products, drain cleaners, and industrial chemicals can damage skin tissue on contact. These burns may not be immediately apparent but can develop over several minutes.
If you work with or handle chemicals, it's important to take extra care and wear appropriate protection. Chemical burns may require specific treatment beyond standard burn care.
Electrical burns
Electrical injuries can cause burns that appear minor on the surface but may be more serious beneath the skin. These burns often occur from faulty electrical equipment or accidents with power sources. Even seemingly small electrical burns should be assessed by a medical professional, as internal damage may be present.
Sun-related burns
Severe sunburn can progress to a second-degree burn, especially after prolonged exposure without adequate protection. This is more common in people with fair skin, at high altitudes, or near reflective surfaces like water or snow. The burn may not reach its full severity for several hours after sun exposure.
Immediate first aid for second-degree burns

Taking the right steps immediately after a burn injury can significantly affect healing and reduce complications. Here's what you should do in the first moments after the injury occurs.
Cool the burn
As soon as possible after the injury, run cool (not cold) water over the burn for at least 10 to 20 minutes. This helps stop the burning process and reduces pain and swelling. If running water isn't available, you can use a cool, clean compress.
Don't use ice, ice water, or very cold water, as extreme cold can damage the tissue further and slow healing. Simply cool, comfortable water is what your skin needs right now.
Protect the area
Once you've cooled the burn, cover it loosely with a clean, non-stick bandage or clean cloth. This protects the sensitive area from infection and helps reduce pain. Don't apply adhesive bandages directly to blisters or broken skin.
Remove any jewellery, watches, or tight clothing near the burnt area before swelling begins. This prevents additional complications if the area swells.
Manage pain
Over-the-counter pain relief medication can help manage discomfort. Follow the dosing instructions on the packaging. Keeping the area elevated above heart level when possible can also help reduce throbbing and swelling.
What you should avoid
There are several common misconceptions about burn treatment that can actually cause more harm.
Knowing what to avoid is just as important as knowing what to do:
Don't apply ice directly to the burn, as this can cause additional tissue damage
Avoid using butter, oil, egg whites, or toothpaste on the burn, as these home remedies have no medical benefit and can increase infection risk
Don't pop blisters, even if they look ready to burst, because intact blisters provide natural protection for the healing skin underneath
Breaking blisters increases the risk of infection and slows healing. Trust that your body knows what it's doing with those protective fluid pockets.
When to seek urgent care
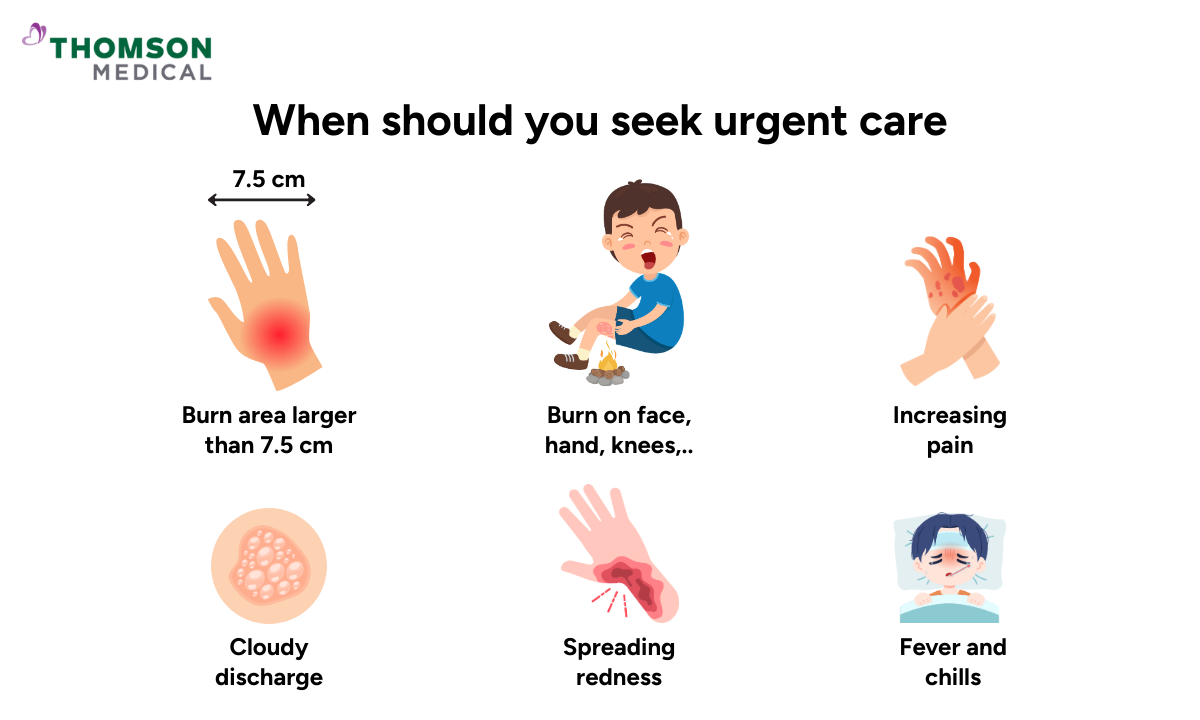
While many second-degree burns can be managed at home, certain situations require professional medical attention. Knowing when to seek help ensures you get appropriate treatment when you need it.
Size and location matter
Seek medical care if the burn meets any of these criteria:
The burn is larger than 7.5 cm (roughly the size of your palm)
Burns on your face, hands, feet, genitals, or over major joints like your knees or elbows
Burns that go all the way around a limb or body part
These locations and sizes warrant medical assessment because they can cause circulation problems as they swell and heal or may require specialised care to prevent complications.
Signs of infection
If you're caring for a burn at home, watch carefully for signs that infection may be developing.
Contact a healthcare provider if you notice any of these warning signs:
Increasing pain after the first few days
Spreading redness around the burn
Pus or cloudy discharge
Red streaks extending from the burn
Fever and chills
An infected burn requires medical treatment to prevent more serious complications. Your instincts matter here – if something doesn't feel right, it's worth getting checked.
Special circumstances
Certain people should always seek medical evaluation for second-degree burns, regardless of size:
Children
Elderly individuals
Pregnant women
People with weakened immune systems or chronic health conditions
Additionally, burns caused by chemicals or electricity should always be assessed by a medical professional, even if they appear minor.
If you're at all unsure about the severity of a burn or how to care for it, it's always better to seek professional advice. Your health and wellbeing are worth that extra care.
How second-degree burns heal
The healing process follows a predictable pattern, though the timeline varies depending on the burn's depth and location.
Here’s how second-degree burns heal:
The healing timeline
In the first few days after injury, you'll notice the most intense pain and swelling. Blisters may continue to form or grow during this period. By the end of the first week, you should begin to see some improvement. The pain will gradually lessen, though the area remains sensitive.
Most superficial second-degree burns heal within two to three weeks. Deeper ones that affect more of the dermis layer may take three to six weeks or longer. During this time, new skin grows from the edges of the burn and from hair follicles within the burnt area.
What to expect
As healing progresses, blisters will gradually flatten and drain on their own. New pink skin will appear underneath. The area may itch as it heals, which is a normal part of the process. Try not to scratch, as this can damage the delicate new skin.
You may notice the healing skin looks different from your surrounding skin. This is completely normal and the colour usually evens out over time, though it may take several months.
Caring for healing burns
Keep the burn clean and protected as it heals. Gently wash it daily with mild soap and water, pat it dry with a clean towel, and apply a thin layer of antibiotic ointment if recommended by your healthcare provider. Cover it with a clean bandage that you change daily or whenever it becomes wet or dirty.
Keep the healing area out of direct sunlight for at least a year after healing, as new skin is more susceptible to sun damage. Use high-factor sun protection on the area when it must be exposed to sunlight.
Preventing second-degree burns
While accidents happen, many burns can be prevented with simple awareness and precautions.
Taking these steps can help protect you and your family from burn injuries:
Kitchen safety
The kitchen is where many household burns occur. These straightforward precautions can make a real difference:
Turn pot handles towards the back of the stove where they can't be knocked or grabbed by children
Use oven mitts when handling hot dishes and pans
Test the temperature of heated foods before serving them to children
Be especially careful when draining pasta or other foods cooked in boiling water
Always lift lids away from you to avoid steam burns
Small adjustments to your kitchen habits can create a much safer environment for everyone in your home.
Hot water precautions
Water temperature is one of the easiest burn risks to control:
Set your water heater to 50 degrees Celsius or below to prevent scalding burns
Always test bathwater temperature before getting in or placing a child in the bath
In homes with young children, consider installing anti-scald devices on taps and showerheads
These simple measures provide an extra layer of protection, especially for vulnerable family members.
Sun protection
Protect your skin from severe sunburn with these essential habits:
Apply broad-spectrum sunscreen with SPF 30 or higher
Reapply every two hours and after swimming or sweating
Seek shade during peak sun hours (typically 10am to 4pm)
Wear protective clothing, hats, and sunglasses when outdoors
Your skin will thank you for this consistent care, not just in preventing burns but in maintaining overall skin health.
Electrical safety
Electrical burns can be particularly serious, so prevention is crucial:
Keep electrical appliances away from water sources
Replace frayed cords and malfunctioning electrical devices
Teach children not to play with electrical outlets or appliances
Switch off the power source first if you must work with electricity
Use appropriate protective equipment when handling electrical items
Taking these precautions seriously can prevent injuries that may be more severe than they initially appear.
Right now, you might feel overwhelmed by everything that's happened. What can help is gently turning your attention to the things within your reach, like following your care routine, keeping the area protected, and taking your medication as needed. These small acts of self-care are meaningful steps forward.
Our urgent care specialists
Loading...
FAQ
How long does it take for a second-degree burn to stop hurting?
Most of the intense pain from a second-degree burn improves significantly within the first few days to a week. The area will remain sensitive for longer, but that sharp, throbbing pain should gradually ease as healing progresses. If pain worsens after the first few days, contact a healthcare provider, as this may indicate infection.
Should I pop the blisters from my burn?
No, you should not pop burn blisters. These fluid-filled bubbles protect the healing skin underneath from infection and contamination. The blister will eventually flatten and drain on its own as healing progresses. If a large blister breaks accidentally, gently clean the area, apply antibiotic ointment, and cover it with a clean bandage.
Can I use aloe vera on a second-degree burn?
Pure aloe vera gel may provide some soothing relief for superficial second-degree burns once the skin has cooled, though research on its healing benefits is mixed. However, avoid products with added ingredients, fragrances, or alcohol.
Always prioritise cooling the burn with water first, and check with a healthcare provider before applying anything to deep burns or blistered skin.
Will my second-degree burn leave a permanent scar?
Whether a second-degree burn leaves a scar depends on several factors, including how deep the burn is and how well it heals.
Superficial second-degree burns often heal with minimal to no visible scarring. Deeper burns that take longer to heal are more likely to leave scars. Proper wound care, avoiding infection, and protecting the healing skin from sun exposure can all help minimise scarring.
When can I return to normal activities after a second-degree burn?
This depends on the size and location of your burn. Small burns may not significantly limit your activities once the initial pain improves. Larger burns, especially those on hands, feet, or joints, may require you to modify activities until healing is complete. Follow your healthcare provider's guidance, and avoid activities that could injure the healing skin again or expose it to infection.
Can I shower with a second-degree burn?
Yes, you can shower with a second-degree burn, but you'll need to take some extra care to protect the area.
In the early stages of healing, it's best to keep the burn dry during showers. You can do this by covering it with a waterproof dressing or plastic wrap secured with medical tape, being careful not to make it too tight.
If water does touch the burn, make sure it's lukewarm and avoid directing the spray onto it. After showering, gently pat the area dry and replace any wet dressings with fresh ones.
The information is intended for general guidance only and should not be considered medical advice. For personalised recommendations and advice based on your unique situation, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Medical 24-Hour Urgent Care Centre (Novena)
- Call: 6350 8812
Notice:
The range of services, vaccinations, and tests may vary. Please contact us directly to enquire about the current availability.
Request an Appointment

