Experiencing anus pain can be uncomfortable. One bowel movement can feel like a deep ache that refuses to go away. Many people in this situation feel embarrassed or don't know when to seek help.
Fortunately, in most cases this pain does not come from a serious issue but rather from common and manageable conditions. Identifying the root cause can help you find the right treatment soon and get back to your normal routine.
What is anus pain?
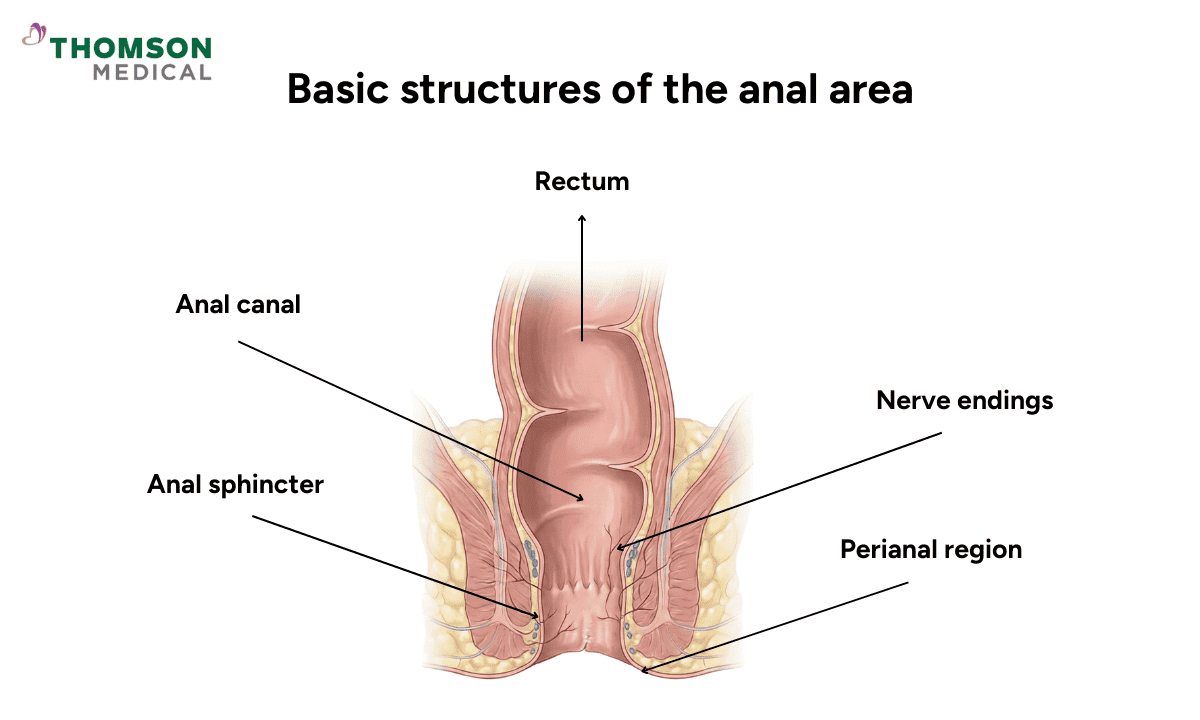
When you experience anus pain (anal pain), you may feel discomfort in or around your anal canal, which is the short passage at the end of your digestive tract where stool exits your body.
This area contains many nerve endings and is surrounded by a ring of muscles called the anal sphincter, which helps control bowel movements. Because this region is so sensitive, even a small irritation can cause noticeable pain.
This discomfort might happen only when you use the toilet, or it could last throughout the day. Even a small bowel movement can sometimes feel like a sharp sting.
Understanding these sensations and pinpointing exactly what they feel like helps narrow down the cause. By doing so, you and your care team can start addressing the root problem early.
What causes anus pain?
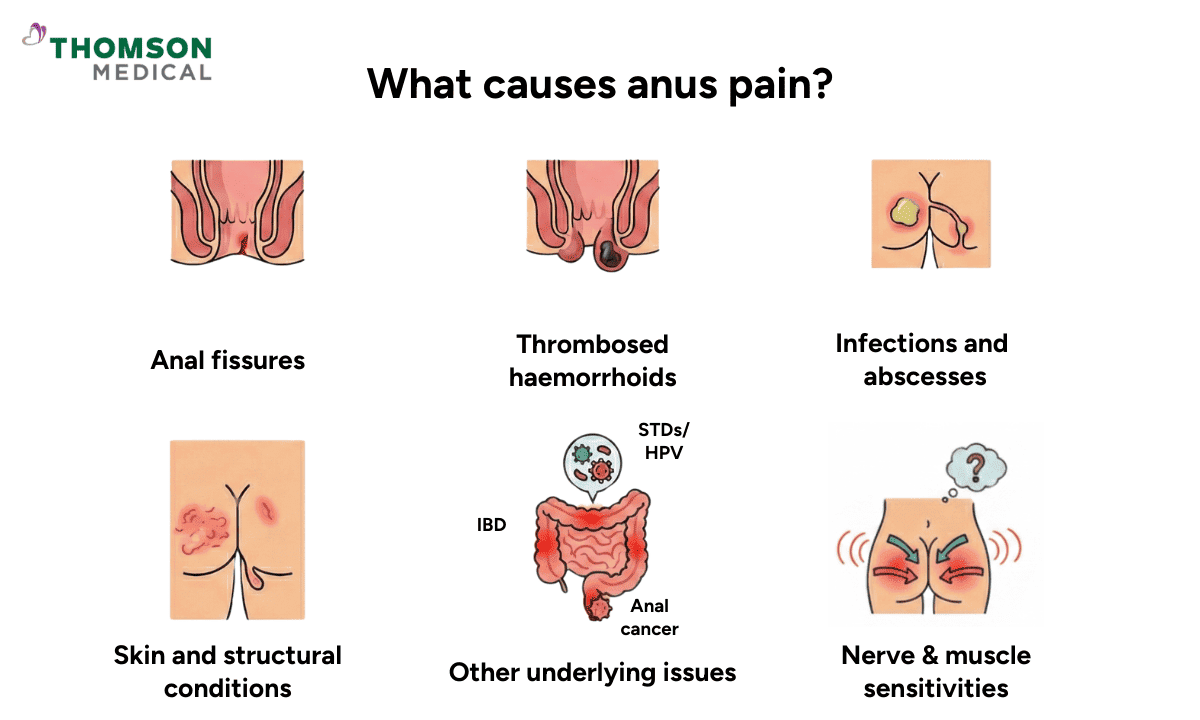
Because your anal canal has many sensitive tissues, muscles, and nerves, anal pain can come from several different causes. Finding out exactly what is going on is the first step towards feeling better.
Anal fissures
Anal fissures are small tears or splits in the skin lining your anus. This usually happens when this area is overstretched, especially after you pass a large or hard stool.
The tear can also cause the anal sphincter muscle to spasm, which increases pain and makes the discomfort last longer.
You might notice these signs if you have a tear:
A sharp, tearing pain during a bowel movement
Discomfort that lasts for minutes to hours after going to the toilet
Small drops of bright red blood in your stool (rectal bleeding)
Although anal fissures can be very uncomfortable, they are common and often settle with appropriate care. If the pain continues or becomes troublesome, your doctor can help determine effective ways to relieve your symptoms.
Thrombosed haemorrhoids
Haemorrhoids are swollen blood vessels in the lower rectum or around your anus, is a condition that is commonly occurring amongst many, and they are often painless.
The condition may become different if a blood clot forms inside an external haemorrhoid, developing thrombosed haemorrhoids.
When this happens, it can lead to:
A hard, tender lump near the opening of your anal area
Sudden and severe pain
Discomfort that makes sitting or walking very difficult
While they can be incredibly painful, these clots usually go away on their own. Your doctor can recommend soothing ointments and what to do at home to shrink the clots and make everyday movements much more bearable.
If you develop a painful lump or severe discomfort that affects your daily activities, it is advisable to seek medical evaluation for appropriate relief. You may arrange a consultation with Thomson Medical Centre for a proper assessment and personalised treatment advice.
Infections and abscesses
An anal abscess is a painful collection of pus-filled bumps on the skin around your anus (perianal region). This often happens when the small glands located just inside your anal area get clogged and infected.
If left untreated, infections can lead to:
An anal fistula, which is a small tunnel connecting the infected gland to your perianal skin
Intense itching and soreness from a fungal infection
Severe discomfort from a pinworm infection, caused by a tiny parasite called Enterobius vermicularis
Because infections in this area can worsen if ignored, it is important to seek medical care. With the right treatment, whether medication or a minor procedure, the infection can clear up and you can prevent further complications.
Skin and structural conditions
The skin around your anus is highly vulnerable to irritation. This can easily lead to various anal skin conditions, such as eczema or psoriasis, which can cause itching and discomfort.
Sometimes, the pain is linked to structural issues, including:
Anal tags are small, harmless extra folds of skin that can become irritated from rubbing against tight clothing.
Pilonidal disease starts when hair near your tailbone gets trapped under the skin and causes irritation or infection.
Pilonidal cysts are swollen pockets under your skin that can become infected, red, and very painful.
Simple steps can make a big difference. Wearing loose cotton underwear and keeping the area clean and dry helps reduce friction and irritation.
If you have a cyst caused by trapped hair, a minor procedure may be recommended to clear it and reduce the chance of it coming back.
Other underlying issues
Several other medical conditions can cause ongoing discomfort in your lower digestive tract. For example, inflammatory bowel disease (IBD) causes long-term inflammation inside your intestines and can lead to frequent, painful bowel movements.
Other potential causes are:
Sexually transmitted diseases (STDs) that cause sores and swelling
The human papillomavirus (HPV), a common virus that can lead to anal warts
Anal cancer, which is rare but can cause a persistent lump, severe pain, or bleeding
If your pain keeps recurring, it is important to look at the root cause. Whether the issue is inflammation in your gut or a viral infection, treating the underlying condition should take priority for you to focus on the things that matter most.
Having an open conversation with a doctor about your digestive and sexual health can help you understand your situation better and prevent the problem from recurring.
If your symptoms persist, recur, or are accompanied by bleeding or unusual lumps, it is important to seek medical advice for a proper evaluation. You may schedule a consultation with Thomson Medical Centre to discuss your concerns and receive personalised care.
What are the symptoms to watch for?
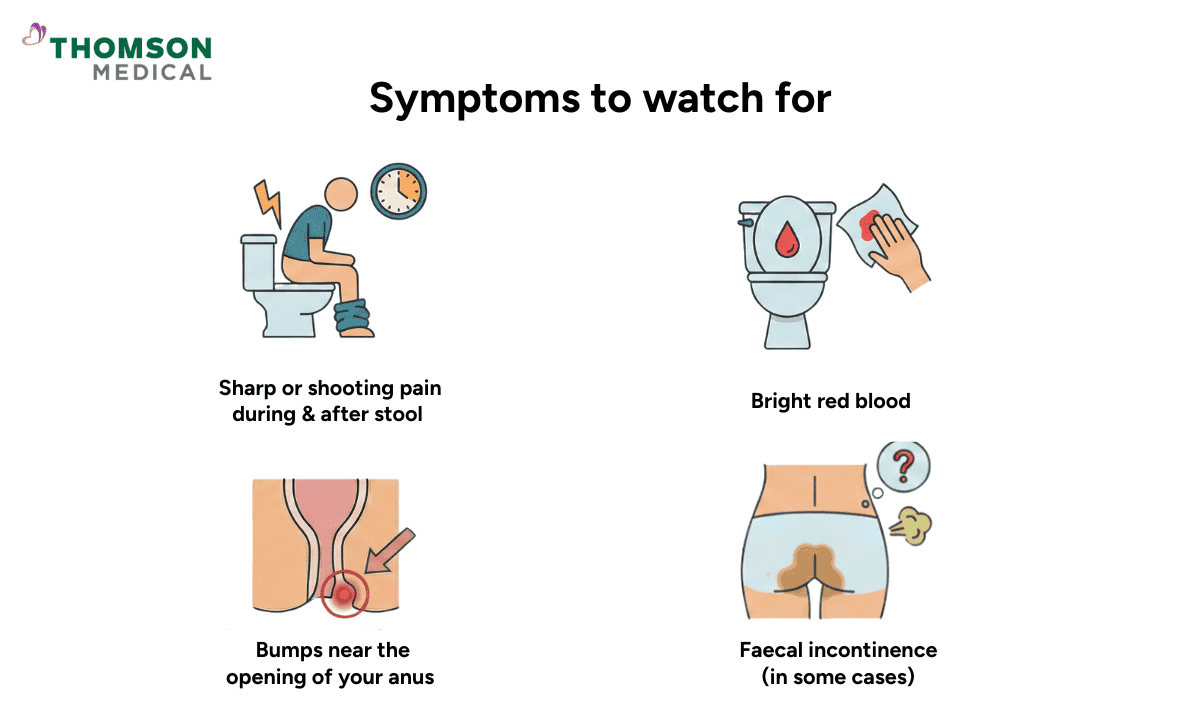
Anal pain does not feel the same for everyone. Taking note of your specific symptoms can give your doctor helpful clues about what might be causing the issue.
You might notice signs such as:
Sharp or shooting pain when passing stool, which can linger for hours afterwards
Bright red blood in the toilet bowl or on your toilet paper
A tender, hard bump near the opening of your anus
In some cases, infection or injury can affect the muscles and nerves in this area, making bowel control more difficult. You may notice unexpected leakage or difficulty holding in gas or stool, a condition known as faecal incontinence.
Noticing exactly when it hurts, like during a bathroom trip or while sitting at your desk, narrows down the possibilities. When you share these details openly with your doctor, it becomes much easier to find the right treatment and start healing sooner.
When should you seek urgent care?

Most cases of pain in this area improve with rest or simple treatment. However, certain symptoms require immediate medical attention.
Seek medical attention straight away if you:
Have a high fever or chills alongside a painful lump
Notice a large amount of rectal bleeding that does not stop
Experience pain that is severe, sudden, or spreading quickly
Cannot pass urine or control your bowels
These signs may indicate a serious infection, significant bleeding, or another urgent condition that needs immediate medical treatment.
If your symptoms are not urgent but continue to worsen or keep returning, arrange a medical review. Most causes of anal pain are treatable, and early assessment can prevent complications and help you recover more comfortably.
Our colorectal surgeons
Loading...
How is anus pain diagnosed?
If you suspect an issue in your anus, it is important to check with your care team. It starts with a conversation about your medical history and your symptoms.
To understand what is causing your discomfort, your doctor might suggest:
A physical exam to gently look at the area and check for tears, lumps, swelling, or signs of infection
A digital rectal examination, where your doctor carefully inserts a lubricated, gloved finger into the rectum to feel for any unusual areas
A small camera test, such as an anoscopy or sigmoidoscopy, which allows your doctor to see the inside more clearly if needed
These tests are usually quick and done with care. Knowing the exact cause of your symptoms helps your doctor recommend the most suitable treatment and bring you relief as soon as possible.
What are some treatment options?
Many people are able to feel better with simple, conservative care. The main goal is to soothe the irritated area and help your body heal.
Common ways to help you feel better include:
Home care and hygiene:
Take warm sitz baths (sitting in a shallow basin of warm water) to help relax the anal sphincter muscles and improve blood flow to the area.
Keep the area clean and dry.
Avoid harsh soaps to reduce irritation.
Medication:
Your doctor may prescribe muscle relaxants or pain relief creams to numb the area.
Physical therapies:
If your pain is linked to muscle tension or spasms, pelvic floor physical therapy can help retrain and relax the muscles that support your bowel.
Biofeedback therapy is a technique that helps you learn how to better control and coordinate these muscles.
Medical procedures:
If you have an anal fistula or an anal abscess, your doctor may suggest a minor surgical procedure to drain the infection.
Your doctor will walk you through each treatment option step by step. They will discuss what might work best for you, helping you understand your choices clearly.
If your symptoms do not improve with home care or continue to return, it is advisable to seek medical advice for a proper evaluation. You may schedule a consultation with Thomson Medical Centre to discuss suitable treatment options and personalised care.
What can you do to prevent anus pain?
While not all cases of anal pain can be prevented, simple daily habits may help reduce your risk and keep this sensitive area comfortable.
Helpful prevention measures include:
Drinking plenty of water throughout the day to keep your stool soft and easy to pass
Eating a balanced diet rich in fibre to promote regular digestion and avoid straining
Staying active and exercising regularly to encourage healthy bowel function
Avoiding sitting on the toilet for long periods, as this can increase pressure on the blood vessels in your anus
Practising good hygiene, such as gentle wiping and keeping the area clean and dry
Wearing more loose-fitting clothes to reduce irritation
Looking after these small habits can go a long way in protecting the sensitive tissues in the area. Even if discomfort does happen, many causes respond well to early care.
FAQ
Can stress cause pain in this area?
Yes. Stress can tighten the muscles around your anal area. When these muscles stay tense for too long, they can cramp or spasm, leading to aching or pressure in the area. Simple relaxation techniques, such as slow breathing, stretching, or taking a warm bath, can help relax the muscles and ease the discomfort.
Is bleeding always a sign of a serious problem?
No. In many cases, minor bleeding is caused by simple issues such as small tears called anal fissures or swollen blood vessels known as haemorrhoids. However, any new, heavy, or persistent rectal bleeding should always be checked by a doctor to rule out more serious conditions.
Will I need surgery?
Probably not. Most common causes, such as small tears or swollen veins, improve with a high-fibre diet, warm sitz baths, and medication. Surgery is usually considered only if the condition is severe, such as a deep anal abscess or a complex anal fistula.
How do I know if it is a fissure or a haemorrhoid?
Anal fissures typically cause a sharp, tearing pain during a bowel movement, and the discomfort may linger afterwards due to anal sphincter spasm. Thrombosed haemorrhoids, on the other hand, often feel like a constant, tender lump near the opening of the anus. A doctor can usually confirm the difference with a quick and gentle examination.
Is it normal to have pain after using toilet paper?
Wiping too hard or using rough toilet paper can irritate the sensitive perianal skin. If you feel stinging after wiping, switching to soft, unscented tissue or rinsing gently with water can help soothe the area and prevent further irritation.
Can sitting for too long cause discomfort?
Yes. Sitting for extended periods increases pressure on the blood vessels and pelvic floor muscles. Sitting on the toilet for too long can be particularly straining and may trigger or worsen conditions such as haemorrhoids or muscle tension.
How long should I wait before seeing a doctor?
If your discomfort does not improve after a few days of simple home care, it is best to arrange a medical review. Seek immediate medical attention if you experience severe pain, high fever, or continuous bleeding.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Medical Concierge
- 8.30am - 5.30pm
- WhatsApp: 9147 2051
Need help finding the right specialist or booking for a group?
Our Medical Concierge is here to help you. Simply fill in our form, and we'll check and connect you with the right specialist promptly.
Notice:
The range of services may vary between Thomson clinic locations. Please contact your preferred branch directly to enquire about the current availability.
Get In Touch