Seeing the first few red spots appear on your child’s skin can be frightening for any parent. Is it a heat rash, an insect bite, or chickenpox?
Most parents recognise chickenpox, but watching your little one struggle with intense itching, fever, and discomfort is never easy. While this highly contagious viral infection is often mild, it can sometimes lead to serious complications such as bacterial skin infections or pneumonia.
Knowing how the virus spreads, recognising the warning signs, and learning when to seek medical help can protect your child and give you peace of mind during this challenging time.
What is chickenpox?
Chickenpox is a highly contagious infection caused by the varicella-zoster virus (VZV). It usually shows up as an itchy, blister-like rash that often starts on the chest, back, or face before spreading to the rest of the body.
Chickenpox is most common in children under 10, but it can affect any child who has not had the infection or the varicella vaccination. The virus does belong to the herpes virus family, but this simply refers to how the virus behaves in cells. It's completely different from genital herpes.
Most children recover well with proper care. After recovery, the virus remains inactive in the body, usually causing no issues. In some cases, it can reactivate later in life as herpes zoster, also known as shingles, which is more common in adults. This happens because the immune system naturally weakens with age, allowing the virus to become active again.
How does it spread?
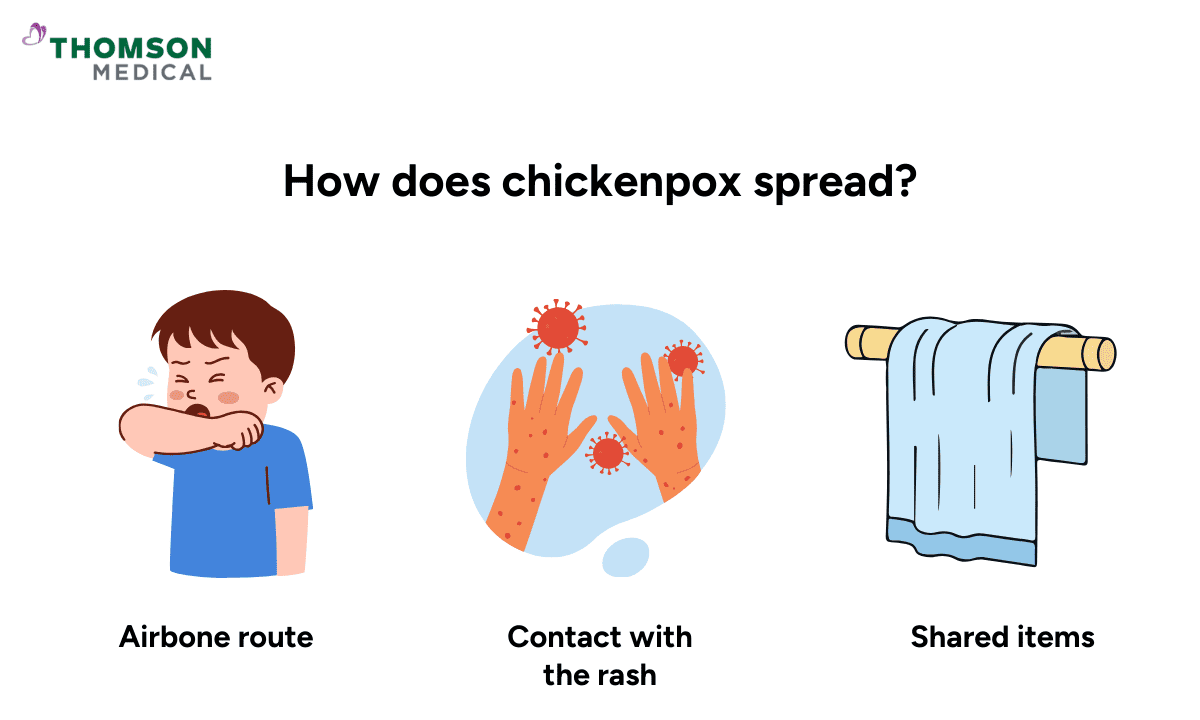
Chickenpox spreads very easily from person to person through close contact, which can be worrying, especially when your child is at childcare or school.
Your child may catch it through the air or by direct contact with the virus, including:
Through the airborne route:
The virus can spread through tiny droplets released when an infected person coughs or sneezes.
Through contact with the rash:
Touching fluid from chickenpox blisters (vesicular fluid) can pass the virus on.
Through shared items:
The virus can live for a short time on items like clothing, bedding, or towels.
This is a less common route of spread.
Chickenpox spreads quickly at home. When one family member gets infected, others who have not had chickenpox or the vaccine have a high chance of catching it. While this can be stressful to manage, most children recover well with proper care.
What are the signs and symptoms?
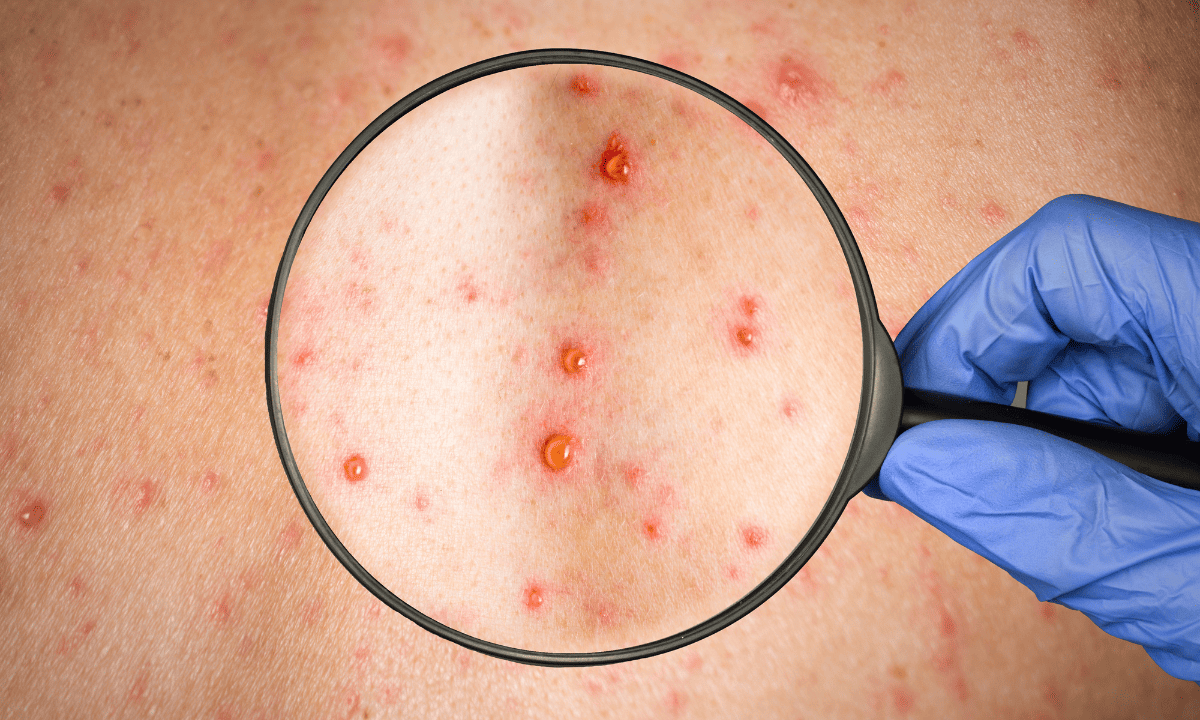
Chickenpox can look different from child to child, which can make it confusing for you to notice at first. It often begins with early symptoms, sometimes called prodromal symptoms, before the rash appears. Recognising these early signs can help you understand what's happening as the illness develops.
Before the rash appears, your child may experience:
Fever
Headache
Loss of appetite
Fatigue or feeling generally unwell
The rash then usually shows up one to two days after the fever starts and develops in stages:
Raised spots:
Small pink or red bumps appear on the skin.
Blisters:
The bumps turn into small fluid-filled blisters.
Scabs:
The blisters break, leak fluid, and then form scabs as they heal.
It is normal for your child to have spots in different stages at the same time. The rash can also appear inside the mouth, which may be painful and make eating or drinking uncomfortable.
Chickenpox can feel uncomfortable and itchy for your child, and it can be worrying to see the rash spread. Keeping your child comfortable and monitoring their symptoms can help them get through this stage more easily.
If your child develops symptoms of chickenpox or you have concerns about exposure, you may schedule an appointment with a doctor at Thomson Paediatric Centre for further assessment.
Our paediatric specialists
Loading...
What complications should you watch out for?
Most children recover from chickenpox without serious problems. However, in some cases, complications can happen, especially in susceptible individuals with weakened immune systems.
Possible complications include:
Bacterial skin infections:
If your child scratches the blisters, bacteria can enter the skin and cause an infection.
This may lead to infections such as Staphylococcus aureus or Group A Streptococcus, which can sometimes become serious.
Varicella pneumonia:
In some cases, chickenpox can infect your child’s lungs.
You may notice symptoms such as a persistent cough, chest pain, or difficulty breathing.
Neurological complications:
Sometimes, chickenpox can affect the nervous system, which may lead to problems with movement or balance.
Reye syndrome:
A rare but serious condition that affects the liver and brain.
This is why aspirin (a pain-relieving and fever-reducing medicine) should never be given to children with chickenpox or any viral illness.
The risk of Reye syndrome is the main reason paracetamol is recommended instead.
These complications are rare, but recognising the warning signs can help you act quickly if needed. Paying attention to how your child is feeling and seeking medical advice when something seems off can make a big difference.
How does chickenpox affect pregnancy and newborns?

Chickenpox can be more serious when it occurs during pregnancy, as it may affect both the mother and baby.
Congenital varicella syndrome:
Happens if the chickenpox infection occurs in the first 20 weeks of pregnancy.
The baby may be born with birth defects, limb problems, or skin scarring.
Neonatal varicella:
Happens if a mother develops a rash 5 days before delivery to 2 days after delivery.
The newborn could be at risk because their immune system is still very weak.
In these situations, your baby’s doctor may give a protective treatment called varicella-zoster immune globulin (VZIG). This does not prevent infection, but it helps reduce how severe the infection may become for you and your baby.
How is chickenpox diagnosed?
If the diagnosis is unclear, or if your child is at higher risk of complications, your doctor may recommend additional tests.
These can include:
Blood test to check for the varicella virus or protective antibodies (Immunoglobulin G)
Blister fluid test to confirm the presence of the varicella virus
Chickenpox is often straightforward to recognise, but you should bring your child to a doctor if you are unsure. A proper check can help you know how to care for your child and what signs to watch for while they recover.
How to manage chickenpox?

Treatment for chickenpox mainly focuses on keeping your child comfortable while their immune system fights the virus.
You can help manage your child’s symptoms at home by:
Offering plenty of fluids to keep your child well-hydrated, such as water, milk, or breast milk or formula for babies
Using calamine lotion, oatmeal baths, or antihistamines prescribed by your doctor to help relieve itching
Giving paracetamol to reduce fever and discomfort
Avoiding aspirin and ibuprofen, as they may increase the risk of serious complications
Keeping your child’s fingernails short to reduce scratching and prevent skin infections
Most children recover well with home care. However, some children may need additional medical treatment, especially if they are at higher risk of complications.
In these cases, your doctor may prescribe acyclovir, an antiviral medicine that helps slow down the virus. This medicine works best when started within 24 hours after the rash first appears.
If you are unsure whether your child needs medical treatment, it is always safe to speak with a healthcare professional for guidance.
How to protect your child from chickenpox?
Protecting your child from chickenpox is possible through immunisation. The chickenpox vaccine, also called the varicella vaccine, helps your child’s body build protection against the virus before they contact the virus.
In Singapore, vaccination against chickenpox is included in the National Immunisation Programme. It is usually given as part of the combined MMRV vaccine, which protects against all four diseases in one injection:
Measles
Mumps
Rubella
Varicella (chickenpox)
Your child will need two doses to build lasting protection. Some vaccinated children may still catch chickenpox. However, symptoms are usually much milder, with fewer blisters and little or no fever.
High vaccination rates also create community protection for vulnerable groups who cannot receive the vaccine, such as newborns or children with weakened immune systems.
If you are unsure whether your child has received the chickenpox vaccine or needs the next dose, a consultation may be helpful. You may consider scheduling an appointment with a doctor at Thomson Paediatric Centre.
FAQ
Can my child still get chickenpox after vaccination?
Yes, but this is uncommon. If your child develops breakthrough varicella, it is usually very mild, with fewer than 50 spots and little or no fever. Vaccination reduces the risk of severe illness.
Are “chickenpox parties” safe for children?
No. Intentionally exposing your child to chickenpox is strongly discouraged. Chickenpox can sometimes lead to serious complications such as lung infections, severe skin infections, or Reye syndrome. Vaccination is a much safer way to protect your child.
When can my child return to school or childcare?
Your child is contagious from 1 to 2 days before the rash appears until all blisters have dried and formed scabs, which usually takes about 5 to 7 days. Your child should stay home until they are no longer contagious to protect other children and carers.
What is the link between chickenpox and shingles?
Both conditions are caused by the VZV virus. After your child recovers from chickenpox, the virus stays inactive in the body. It can reactivate years later as shingles, which causes a painful rash.
Is it safe for pregnant women to be around a child with chickenpox?
If she’s pregnant and has had chickenpox or the vaccine before, she is usually protected. If you’re unsure or have never had chickenpox, try to avoid contact and speak to your doctor promptly for advice and possible preventive treatment.
When should I bring my child to see a doctor?
You should seek medical advice if your child has:
A high fever
Trouble breathing
Severe headache
Unusual drowsiness
Signs of skin infection such as redness, swelling, or pus
It is also important to see a doctor if your child is very young or has a weakened immune system.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice for your little one's conditions, request an appointment with Thomson Paediatric Centre today.
