Being told you need a double mastectomy, or deciding to have one, can be a daunting experience. It is a big decision, and it is completely normal to feel uncertain or scared by the information coming your way.
What many people find is that once they understand what the surgery actually involves and what life looks like afterwards, things can start to feel a little less overwhelming. Learning more about the different surgical approaches available, how to prepare, and what recovery genuinely looks like can help shift your uncertainty into a clearer sense of what to expect.
What is a double mastectomy?
A mastectomy is a surgery to remove breast tissue. When only one breast is removed, it is called a single mastectomy. When both breasts are removed, this is called a double mastectomy, or bilateral mastectomy.
A double mastectomy may be recommended to treat breast cancer or as a preventive measure for those who carry a significantly higher risk of developing it. For some people, this surgery reduces the constant worry about cancer developing or returning, which can feel like regaining control over an uncertain future.
Who should consider a double mastectomy?
Your doctor may recommend or discuss a double mastectomy with you to either treat existing breast cancer or significantly reduce your risk of developing it.
For treatment, a double mastectomy may be considered if:
The cancer has spread across a large area of the breast
There are multiple tumours present in the same breast
You want to reduce the chance of cancer returning in the other breast
Your type of breast cancer may respond better to surgery than other treatments
For prevention, your doctor may discuss this option if you:
Carry the BRCA1 or BRCA2 gene mutation (a gene change that can significantly raise your risk of breast cancer)
Have a strong family history of breast or ovarian cancer
Have been diagnosed with LCIS (a condition where abnormal cells are found in the milk-producing glands of the breast, which increases cancer risk)
Have previously had radiation therapy to the chest area
If any of these apply to you, it is worth discussing with your doctor whether a double mastectomy is right for you. This is a very personal decision, often involving a choice between ongoing intensive screening and surgery that significantly lowers risk but permanently changes your body. Many people find it helpful to speak with a genetic counsellor before making their decision.
If you have been advised to consider a double mastectomy because of your cancer diagnosis or strong family history, it is important to seek personalised medical advice before making a decision. Request an appointment with the Thomson Breast Centre to review your risk factors and discuss whether a double mastectomy is medically appropriate for you.
Types of mastectomy
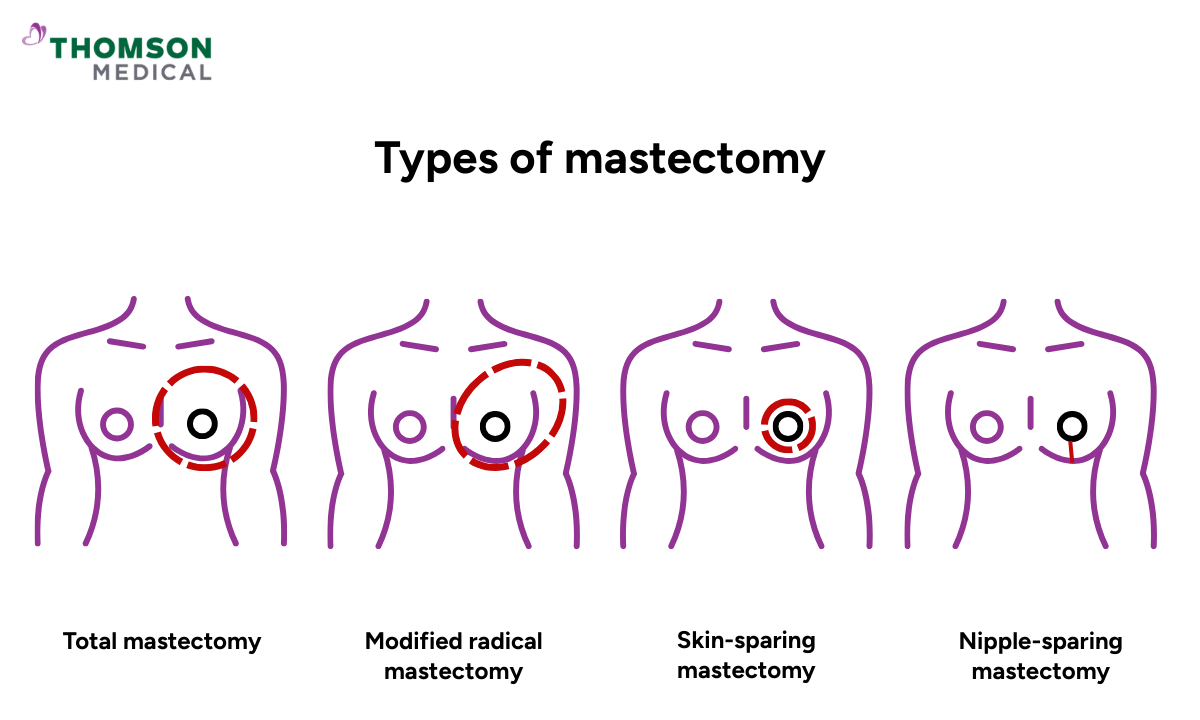
When it comes to a double mastectomy, the same surgical approaches used for a single mastectomy are applied to both breasts. The right one for you will depend on your diagnosis, your anatomy, and whether you are considering breast reconstruction afterwards.
Total (simple) mastectomy
Both breasts are removed, including the nipple and areola (the darker skin surrounding the nipple), while the chest muscle underneath is left in place. This is one of the more common approaches.
Modified radical mastectomy
This involves removing the breast tissue along with some of the lymph nodes in your armpit, which is part of your immune system that filters harmful substances. It may be recommended if cancer has spread, or is suspected to have spread, beyond the breast tissue itself.
Skin-sparing mastectomy
The breast tissue, nipple, and areola are removed, but most of the outer skin of the breast is kept intact. This approach is often used when reconstruction is planned, as preserving the skin can give a more natural result.
Nipple-sparing mastectomy
The breast tissue is removed while the nipple and areola are kept. This tends to suit people whose tumour is not too close to the nipple area.
The key difference between these approaches is what gets preserved and what gets removed. Skin-sparing and nipple-sparing approaches preserve more of your breast’s original appearance, which can help reconstruction look more natural and feel less drastic emotionally. However, they're only suitable when cancer hasn't spread to the skin or nipple area.
Your surgeon can explain which options are medically appropriate for your situation and how each might affect your breast reconstruction possibilities.
Our breast cancer specialists in Singapore
Loading...
How to prepare for surgery
Preparing well ahead of your operation can make a real difference to both your experience on the day and your recovery afterwards. Your care team will guide you through the specific steps, but here is a general overview of what to expect.
Before your surgery, you will likely need to:
Complete any required scans, blood tests, or assessments
Let your doctor know about all medications, supplements, and vitamins you take, as some may need to be paused beforehand
Stop smoking if you smoke, as this can affect how well your body heals
Avoid alcohol in the days leading up to your operation
At home, it helps to prepare for the first few weeks after surgery. Stock up on loose, button-front shirts that won't need to be pulled over your head. These small preparations can make a big difference when you're sore.
What happens during double mastectomy surgery?
Surgery can feel frightening when you don't know exactly what will happen. Understanding the process can help ease some of that anxiety.
A double mastectomy is performed under general anaesthesia, and you’ll fall asleep. The procedure takes around two to four hours, though this can vary depending on the type of surgery involved.
Here is what generally takes place:
Your surgeon removes the breast tissue from both breasts, following the agreed surgical plan
If your lymph nodes need to be assessed or removed, this is done during the same operation
Small drainage tubes are placed near the incision sites to collect any fluid that builds up
The wounds are carefully closed with stitches
It is normal to feel groggy, sore, or even emotional when you wake. Most people are moved to a ward within a few hours. Your surgical team will continue monitoring your recovery and support managing your pain levels.
Recovery after a double mastectomy
Recovery looks different for everyone, and it is important to be patient and kind with yourself during this time. Most people stay in hospital for one to three days after surgery.
In the first few weeks at home, you might notice:
Tiredness and soreness, especially around the chest and arms
The need for prescribed pain relief to stay comfortable
Drainage tubes remaining in place until fluid levels reduce, usually within one to two weeks
Most people can return to light daily activities within four to six weeks. During this time, you should avoid lifting children, carrying shopping, or doing heavy housework.
Full recovery may take several months, depending on the extent of your surgery. If you have had or are planning reconstruction, your surgeon will give you a more personalised timeline. Planning for these limitations ahead of time can help make recovery less stressful.
What are the risks and complications of a double mastectomy?
Like any major surgery, a double mastectomy carries some risks. Your doctor will go through these with you in detail before you give your consent, so you can make a fully informed decision.
Common side effects you may experience include:
Pain and discomfort around the chest area
Swelling and bruising
Numbness or changes in sensation across the chest
Fatigue during the recovery period
Some discomfort from drainage tubes while they are in place
Complications that can sometimes occur include:
Infection at the wound site
Bleeding during or after surgery
Seroma (a pocket of fluid that can collect under the skin near the wound, which usually resolves on its own or can be drained)
Lymphoedema (swelling in the arm caused by fluid build-up)
Scarring
Most people recover without serious complications. Your care team monitors you closely in hospital and gives you clear guidance on warning signs to watch for at home. Catching and addressing any issues early usually means they can be managed straightforwardly before they become bigger problems.
Understanding the possible risks can help you prepare for surgery and recovery more confidently. Request an appointment with the Thomson Breast Centre to discuss the potential complications of a double mastectomy, learn how your care team helps reduce these risks, and understand what signs to watch for during your postoperative recovery.
How much does a double mastectomy cost in Singapore?
Cost is one of the most practical questions people have, and it is completely reasonable to want a clear picture before making any decisions.
At public hospitals in Singapore, a subsidised mastectomy typically costs around SGD 1,744 to 3,860. At private hospitals, the inpatient bill for a mastectomy is around SGD 32,497.
On top of the hospital bill, the fees may include:
Surgeon fee: SGD 6,649 to SGD 13,080
Anaesthetist fee: SGD 1,962 to SGD 2,616
Daily doctor attendance: SGD 230 to SGD 450 per day
These estimated figures are for a single breast. For a double mastectomy, costs may be significantly higher depending on the complexity of your surgery, the type of mastectomy performed, and whether reconstruction is carried out at the same time.
Bill amounts are intended as a general guide by the Ministry of Health Singapore. The actual costs will vary based on your individual condition, surgical approach, hospital, and ward type. For a personalised estimate, speak with your surgeon and your hospital's financial counsellor.
FAQ
Why do some women choose a double mastectomy for cancer in only one breast?
Some people choose to remove both breasts even when only one is affected, mainly to reduce the risk of cancer developing in the other breast. This is often a personal decision influenced by factors such as carrying the BRCA gene mutation, a strong family history, or simply peace of mind.
How long does it take to recover from a double mastectomy?
Most people return to light daily activities within four to six weeks. Full recovery, particularly if reconstruction is involved, can take several months. Everyone heals at a different pace, and your surgeon will give you a timeline based on your specific situation.
Can you get breast reconstruction after a double mastectomy?
Yes. Reconstructive surgery can take place during the same operation or at a later date. Your surgeon can walk you through which options may be suitable for you.
Does a double mastectomy completely eliminate the risk of breast cancer?
It significantly reduces the risk, but it cannot eliminate it entirely. A small amount of breast tissue may remain, which means there is still a very small chance of cancer developing.
Is a double mastectomy painful?
Some pain and discomfort after surgery is expected, but this is managed with prescribed pain relief. Most people find the discomfort eases gradually over the first few weeks.
Can you live normally after a double mastectomy?
Yes, many people go on to live full and active lives after a double mastectomy. Adjusting to changes in your body can take time, and emotional support plays a big role in that journey. With the right care and support, most people find their footing again.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, request an appointment with Thomson Breast Centre today.
Reference:
Ministry of Health Singapore. (2023). SA824B - Breast, tumor (malignant various lesions), simple mastectomy with axillary clearance, with/without sentinel node biopsy. https://www.moh.gov.sg/managing-expenses/bills-and-fee-benchmarks/cost-financing/tosp-sa824b-bill-information/
