If you have been experiencing pelvic pain, heavy periods, or symptoms that do not feel quite right, it can be difficult to know what might be causing them.
Two conditions that are often discussed are endometriosis and fibroids. Both are common, both affect the reproductive system, and both can have a noticeable impact on daily life.
Understanding how they differ, what symptoms to look out for, and how they are diagnosed can help you feel more prepared and reassured when speaking with your doctor.
What is endometriosis?
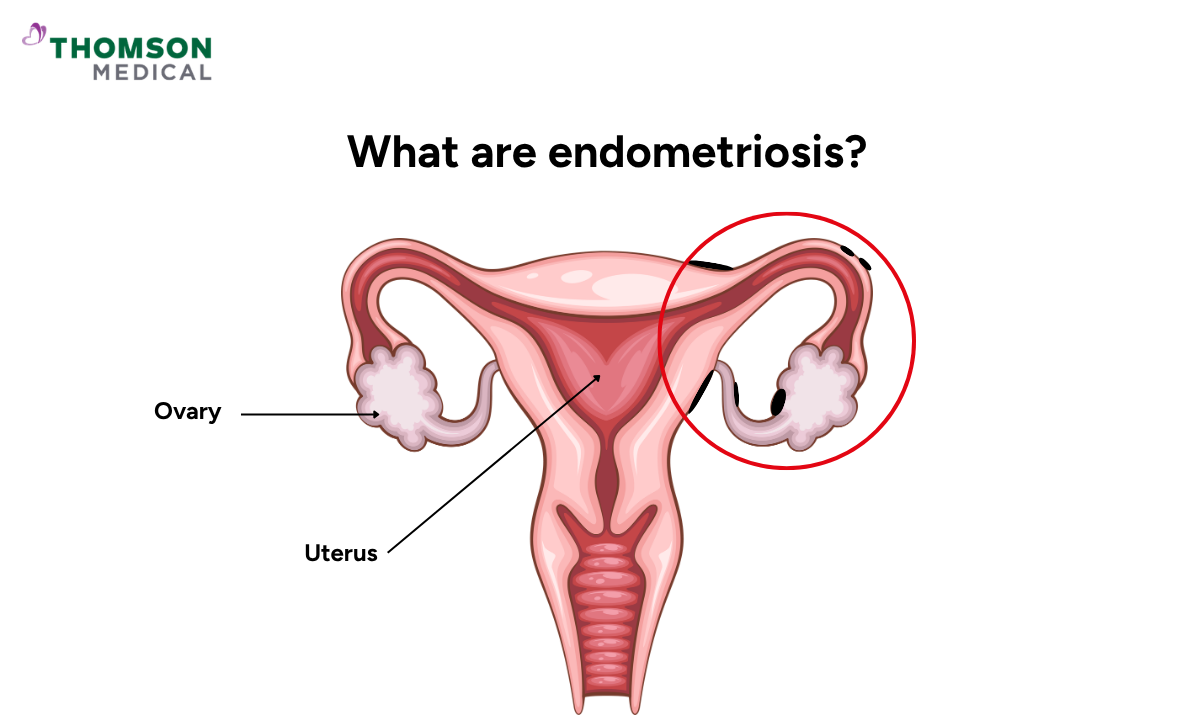
Endometriosis happens when tissue similar to the lining of your uterus grows outside of it. This tissue can attach to your ovaries, fallopian tubes, the outer surface of your uterus, your intestines, or the lining of your pelvis.
During your period, this tissue behaves like it would inside your uterus. It swells and breaks down. But because it has nowhere to leave your body, it becomes trapped. This is what causes the inflammation, scarring, and pain that many women with endometriosis live with day to day.
What causes endometriosis?
There is no clear reason why endometriosis develops, and it is often linked to a combination of factors.
Possible factors include:
Retrograde menstruation, where menstrual blood flows backwards into the pelvis rather than leaving your body
Changes in the immune system that may allow misplaced tissue to survive and grow
Genetics, as it can run in families
Starting periods at a young age, or having shorter menstrual cycles
What these factors have in common is their link to oestrogen. Endometriosis depends on this hormone, which is why symptoms often improve during pregnancy and after menopause when oestrogen levels drop.
Symptoms of endometriosis
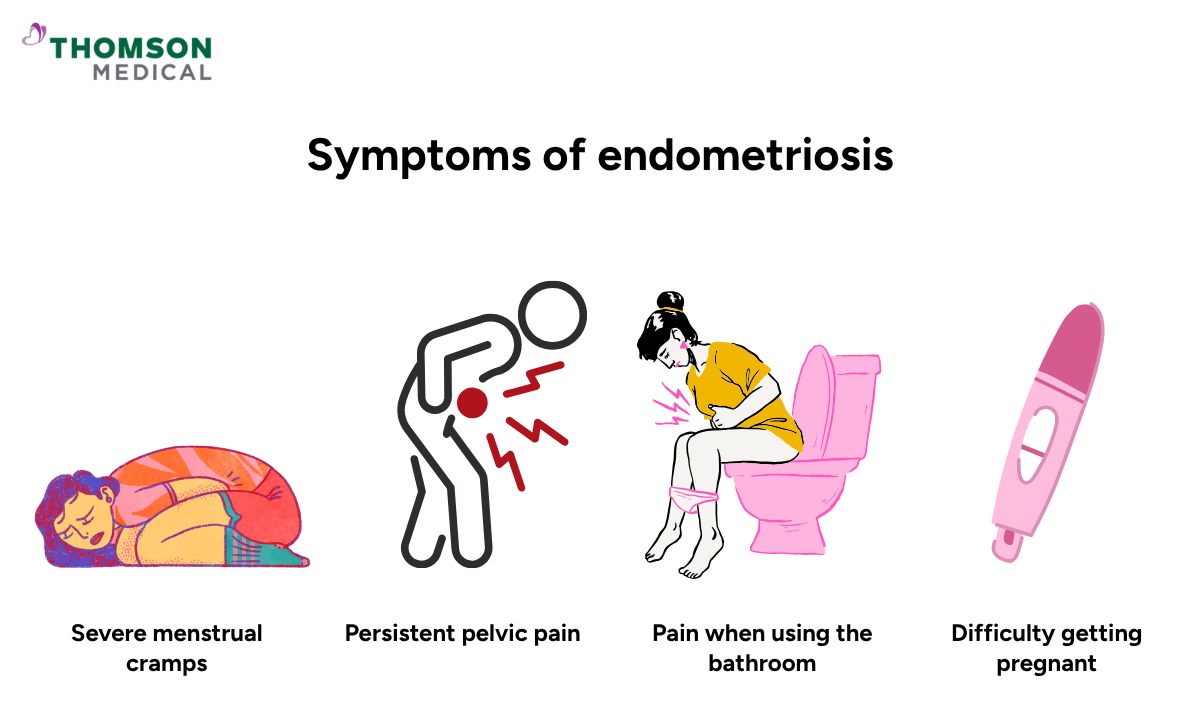
The most noticeable symptom of endometriosis is pain. For many women, it can feel much more intense than typical period discomfort.
You might experience:
Severe menstrual cramps that interfere with your daily life
Persistent pelvic pain, even outside of your period
Pain during or after sexual intercourse
Pain when using the bathroom, especially during your period
Heavy or irregular bleeding
Bloating and fatigue
Difficulty getting pregnant
The level of pain you feel does not always reflect how widespread endometriosis is. Some women experience severe symptoms even with mild disease, while others may have fewer symptoms despite more widespread endometriosis.
Stages of endometriosis
Not all endometriosis looks the same. The condition is classified into four stages that describe how far it has spread and how deeply it has grown into surrounding tissue.
These stages are:
Stage I (Minimal):
At this stage, there are a few small, shallow implants on your pelvic lining, with no significant scar tissue involved yet.
Stage II (Mild):
Implants become more numerous than in Stage I and extend slightly deeper into the tissue. Some minor scarring may begin to form.
Stage III (Moderate):
This stage involves many deep implants. You may also have small cysts on your ovaries, commonly called "chocolate cysts", and bands of scar tissue known as adhesions, which can cause pelvic organs to stick together.
Stage IV (Severe):
This is the most advanced stage. It involves deep implants, larger cysts on the ovaries, and more significant scarring. In some cases, the tissue may also affect the bladder or bowels.
However, the stages do not remain fixed. Without treatment, endometriosis can progress from one stage to the next over time, which is why early diagnosis and treatment matter.
What are fibroids?
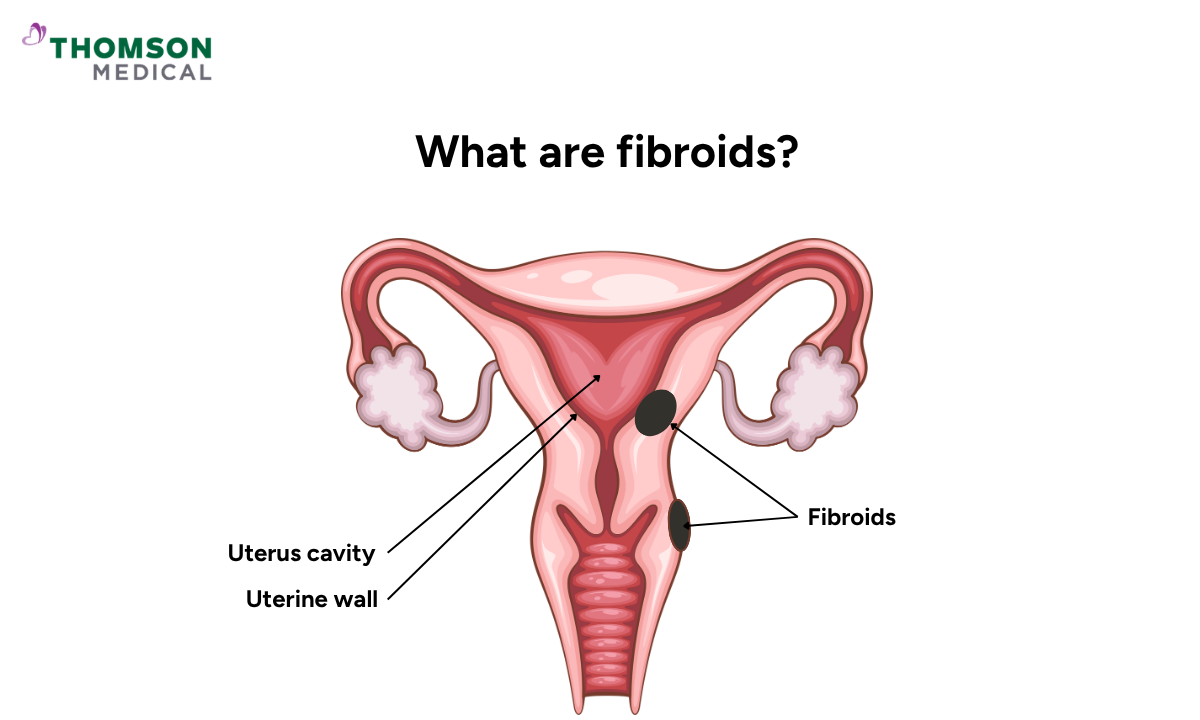
Uterine fibroids are non-cancerous growths made of muscle and fibrous tissue that develop within or on your uterus.
They are very common during the reproductive years. Many women have them without ever knowing it, because fibroids do not always cause noticeable symptoms.
What causes fibroids?
Fibroids are linked to hormones, especially oestrogen and progesterone. They tend to grow during the reproductive years and may shrink after menopause.
You may be more likely to develop fibroids if you:
Have a family history of fibroids
Started your periods at a younger age
Have a higher body weight
However, fibroids can develop without these factors, and having them does not guarantee that you will develop fibroids.
Symptoms of fibroids
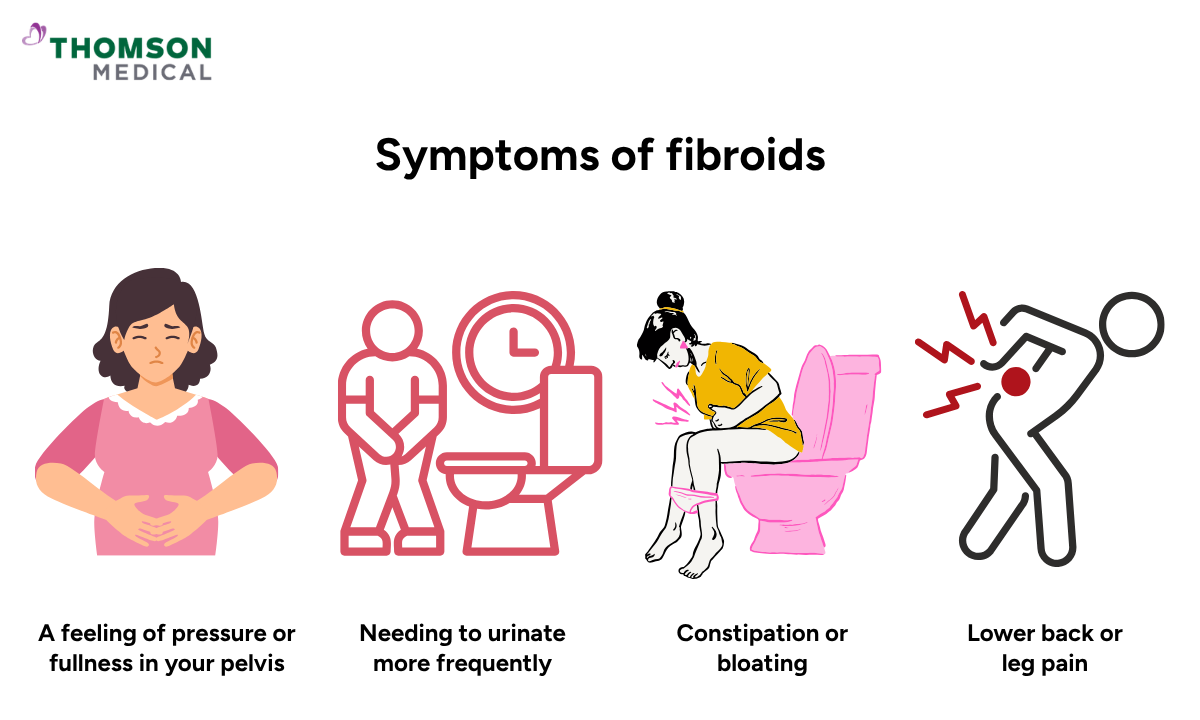
Unlike endometriosis, fibroid symptoms tend to be related to pressure and heavy bleeding rather than sharp or inflammatory pain.
You might notice:
Heavy or prolonged periods
A feeling of pressure or fullness in your pelvis
Needing to urinate more often
Constipation and bloating
Lower back or leg pain
Pain during sexual intercourse
The severity of your symptoms often depends more on the size and position of your fibroids rather than their number. Even one fibroid in a sensitive area can cause noticeable symptoms, while several smaller ones in other places may not affect you as much.
Types of fibroids
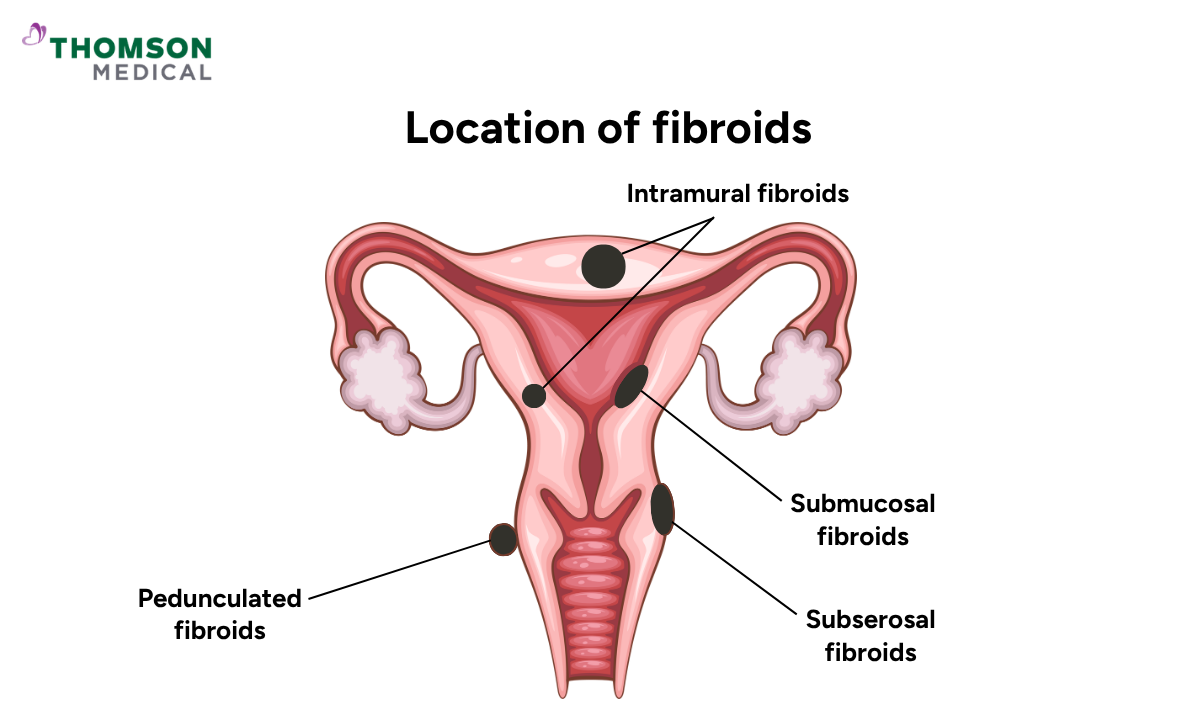
Fibroids are classified by where they grow in or around your uterus. Their location largely determines which symptoms you are most likely to experience.
The four main types are:
Submucosal fibroids grow inside your uterine cavity
Intramural fibroids grow within the wall of your uterus
Subserosal fibroids grow on the outer surface of your uterus and are more likely to press on nearby organs such as the bladder or bowel
Pedunculated fibroids are attached to your uterus by a stalk and may cause sudden pain if the stalk becomes twisted
Knowing where your fibroids are located helps explain the symptoms you are experiencing and gives your doctor a clearer picture when you discuss your treatment options.
Experiencing pelvic pain, heavy periods, or difficulty conceiving can be linked to endometriosis or fibroids. Request an appointment with Thomson Medical so our specialists may provide a thorough evaluation and explain the differences between these conditions.
Our gynaecologists
Loading...
The differences between endometriosis and fibroids
Both conditions affect your uterus and can impact your periods and fertility, but they work in very different ways.
Here is a quick comparison:
Endometriosis | Fibroids | |
What it is | Tissue growing outside your uterus | Non-cancerous growths on or inside your uterus |
Main type of pain | Inflammatory, often sharp and severe | Pressure-related, dull and heavy |
Periods | Often painful and irregular | Often heavy and prolonged |
Bowel symptoms | Pain when using the bathroom | Constipation from pressure |
Appearance on imaging | Not always visible | Often detectable as a mass |
Fertility impact | Can affect fertility | Can affect fertility in some cases |
If you are trying to understand which condition may apply to you, keeping a note of when your symptoms happen, how long they last, and what they feel like can help your doctor make a clearer assessment.
If your symptoms are worse around your period, this may suggest endometriosis. If they feel constant or are related to pressure in your pelvis, it might be linked to fibroids.
Can you have both at the same time?
Yes, it is possible to have both endometriosis and fibroids at the same time. When this happens, symptoms can overlap and feel harder to tell apart. Getting a clear diagnosis can take longer, which can be frustrating. However, it does not mean that treatment is impossible.
One common misconception is that the two conditions are linked. Endometriosis does not lead to fibroids, and fibroids do not cause endometriosis. They are two separate conditions that can happen together in some people.
If you have both, your doctor will usually look at each condition separately to understand how much it is affecting your symptoms. From there, your treatment plan may address both together or focus more on the one that is having the biggest impact on your daily life.
How are they diagnosed?
Finding out whether you have fibroids or endometriosis requires more than symptom assessment alone. The tests needed and the time it takes can vary depending on your condition.
Diagnosing endometriosis
Endometriosis can be hard to diagnose because its symptoms often overlap with those of other conditions, and there is currently no single blood test that can confirm it.
The process usually involves:
Initial imaging:
Your doctor may begin with an ultrasound or MRI scan to check for ovarian cysts, which can sometimes be associated with endometriosis.
These scans are a helpful starting point but cannot confirm the condition on their own.
Laparoscopy:
A laparoscopy remains the most reliable way to confirm endometriosis.
During this procedure, your surgeon makes a small incision and uses a tiny camera to examine the inside of your abdomen and pelvis directly.
It is performed under general anaesthesia and is often carried out as a day procedure.
Biopsy:
If any suspicious tissue is found during the laparoscopy, a small sample is taken and examined under a microscope. This confirms whether the tissue is consistent with endometriosis.
The results give your doctor a clearer picture to work from, including whether surgery to remove the tissue may be an option for you.
Diagnosing fibroids
Fibroids are generally easier to detect and can often be confirmed without surgery.
Your doctor may use:
An ultrasound to show the size, number, and location of fibroids
An MRI for a more detailed picture, especially if surgery is being considered
A hysteroscopy, where a small camera is gently placed inside your uterus to examine it more closely
Blood tests to check for anaemia if you have been experiencing heavy menstrual bleeding
Sometimes fibroids are spotted during a routine scan carried out for a different reason. If this has happened to you, please know that nothing was overlooked. This shows how common it is for fibroids to cause no symptoms at all.
Unsure what’s behind your pelvic discomfort? Request an appointment with Thomson Medical. Our specialists can recommend the suitable imaging or procedures to confirm a diagnosis and guide your care.
What are the treatment options?
Treatment for both conditions depends on your symptoms, your age, and whether you are planning to have children.
Treating endometriosis
Managing endometriosis often focuses on relieving pain and slowing the growth of tissue.
Your doctor may recommend:
Hormonal birth control, such as the pill or hormonal coil, to manage pain and reduce bleeding
GnRH agonists or antagonists, which are medicines that lower oestrogen levels in your body to help slow tissue growth
Progestogens to help slow the progression of the condition
Pain relief medication for day-to-day symptom management
Laparoscopic surgery to remove or destroy endometriotic tissue
For some people, a combination of treatments works best. It is also worth knowing that endometriosis can return after surgery, which is why hormonal treatment is often continued afterwards to reduce the chances of the condition returning.
Treating fibroids
Fibroid treatment depends on the size and location of your fibroids, your symptoms, and whether preserving fertility is your priority.
You may consider:
Hormonal therapy to help manage symptoms and reduce fibroid growth
Tranexamic acid to reduce heavy bleeding during your period
Uterine artery embolisation, a procedure that blocks the blood supply to fibroids, causing them to shrink
Myomectomy, which is surgery to remove fibroids while keeping the uterus intact
Hysterectomy, which is the removal of your uterus. This is usually considered when other options have not provided relief and you do not plan to have any more children
Treatment is not always a one-time decision. As fibroids can change in size over time, your treatment may need to be reviewed and adjusted as your symptoms change. Your doctor will guide you through what to expect at each stage.
Both endometriosis and fibroids are manageable conditions. If you have been experiencing symptoms that concern you, speaking with your doctor is the most effective next step toward getting the right diagnosis and care.
FAQ
Which is more painful, endometriosis or fibroids?
Endometriosis often causes more intense pain that feels deep and persistent, such as severe menstrual cramps or pelvic discomfort. Fibroids usually lead to pressure, bloating, or heavy bleeding, though large fibroids can sometimes be painful as well.
Can endometriosis or fibroids cause infertility?
Yes. Both conditions can affect fertility by interfering with egg movement, implantation, or the uterine environment, depending on their size, number, and location.
Do endometriosis and fibroids go away on their own?
In most cases, they do not resolve on their own. They may improve after the menopause due to lower hormone levels, but they rarely disappear during the reproductive years without treatment.
Can birth control help treat endometriosis or fibroids?
Yes. Hormonal birth control can help reduce pain caused by endometriosis and control heavy bleeding from fibroids. However, it does not permanently cure either condition.
Is a hysterectomy the only cure for endometriosis or fibroids?
For fibroids, a hysterectomy is considered a lasting treatment option for women who do not plan to have more children. For endometriosis, it may help reduce symptoms, but it is not always a guaranteed cure, especially if endometriotic implants remain outside the uterus.
Can diet and lifestyle changes help manage endometriosis or fibroids?
- Regular exercise, which can support hormone balance and reduce discomfort
- An anti-inflammatory diet, such as one rich in vegetables, grains, and oily fish, may help reduce pain and bloating
- Maintaining a healthy weight, as excess body fat can influence oestrogen levels
- Stress management, including rest, gentle movement, or mindfulness practices
- Limiting alcohol and processed foods, which may worsen hormonal symptoms
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
