Living with endometriosis is not easy. For many people, it means years of managing persistent pain, heavy periods, and the emotional toll of a condition that is often misunderstood or difficult to treat. If you've reached a point where other treatments haven't given you the relief you were hoping for, a hysterectomy may be one of the options your doctor discusses with you.
Surgery is a significant decision, especially when it affects your fertility and hormones. Understanding what the procedure involves, what recovery looks like, and what outcomes you can expect can help you navigate this decision with more clarity.
What is a hysterectomy for endometriosis?
Endometriosis is a condition where tissue similar to the lining of your uterus grows outside your uterus. It is often found on your ovaries, fallopian tubes, or the lining of your pelvis.
This tissue still behaves like it is inside your uterus. It thickens, breaks down, and bleeds each month during your cycle. Because the blood cannot leave your body, it becomes trapped. Over time, this can lead to inflammation and persistent pain.
If your symptoms are severe or do not improve with other treatments, your doctor may recommend a hysterectomy, which is surgery to remove your uterus.
When might a hysterectomy be recommended?
A hysterectomy may be considered when your symptoms have not improved with other treatments and continue to significantly affect your quality of life.
Your doctor may suggest this surgery if you experience:
Ongoing pelvic pain that affects your daily activities, work, or relationships
Heavy menstrual bleeding that does not improve with medication
Endometriosis affecting your bowel, bladder, or other pelvic organs, causing symptoms such as bowel pain or urinary issues
Symptoms that keep coming back even after previous surgeries
Every woman's situation is different. When deciding if this surgery is right for you, your doctor will consider your age, symptoms, and how much endometriosis affects your daily life. A hysterectomy is a permanent step, and it deserves careful consideration. If you are younger or hope to have children in the future, your doctor will usually explore other treatment options first.
Our gynaecologists in Singapore
Loading...
What type of hysterectomy is used for endometriosis?
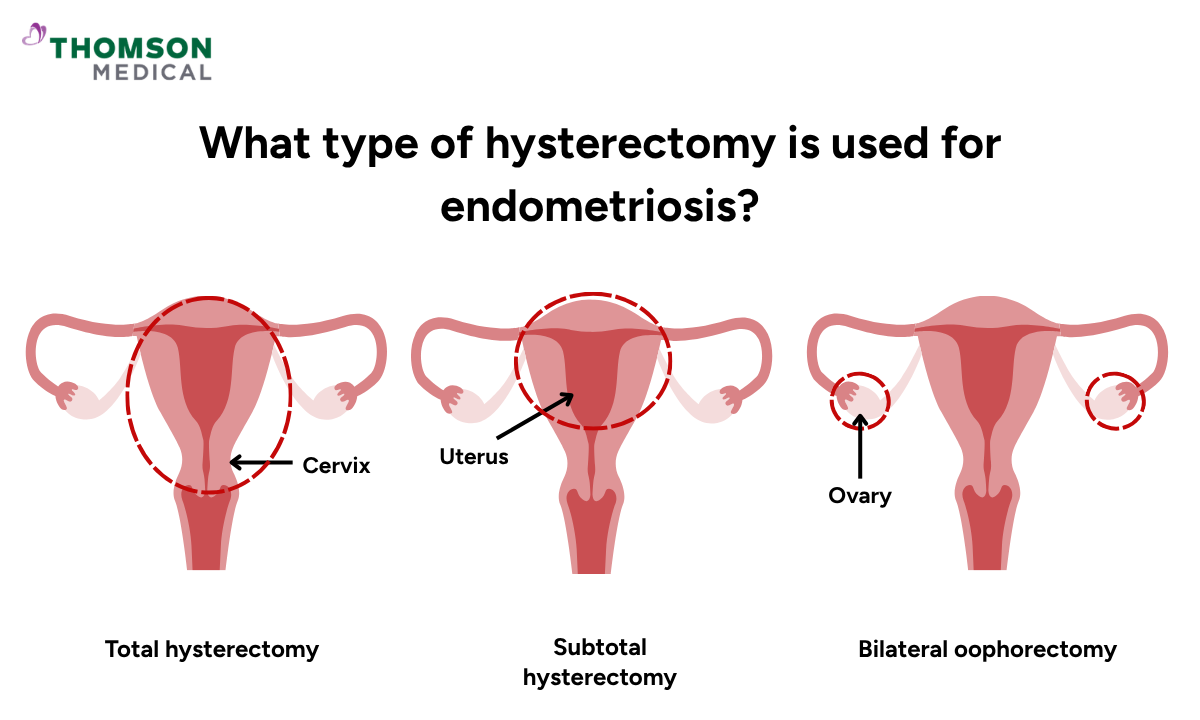
Hysterectomy for endometriosis is not a one-size-fits-all procedure. The type of surgery your doctor recommends will depend on how extensive your endometriosis is, your age, your fertility goals, and your overall health.
Total hysterectomy
This removes both your uterus and cervix. It is the most common type performed for endometriosis, particularly when the cervix is involved or when more complete treatment is needed.
Subtotal hysterectomy
This removes only the upper part of your uterus, while the cervix is left in place. It may help to reduce surgical complexity in certain cases, though it is less commonly performed for endometriosis.
Bilateral oophorectomy
In some cases, your surgeon may also remove both ovaries, especially if your endometriosis is severe or driven by hormonal activity. This can reduce the chances of the condition returning, although it also means your body will no longer produce oestrogen and progesterone naturally.
If your ovaries are removed, you will experience surgical menopause, which can bring on symptoms such as hot flushes, mood changes, and vaginal dryness. If they are kept, your hormones will continue functioning as normal, though some subtle changes in mood or energy may still occur. Your doctor will discuss which option is most appropriate for you.
If you are unsure whether a hysterectomy is appropriate for your situation, speaking with a gynaecologist who specialises in endometriosis can help you understand your options and next steps. Request an appointment with Thomson Medical to discuss your personalised care plan.
How to prepare for your hysterectomy
Preparing thoughtfully before surgery can help ease your worries and support a smoother recovery.
Before your hysterectomy, you'll typically have:
Blood tests and imaging scans to assess your overall health
A review of your current medications
Fasting and bowel preparation before the operation
A detailed conversation with your surgeon about what to expect, including which organs will be removed, the surgical approach, and what your recovery timeline will look like
All of this is decided with you in mind. Your doctor will use this information to tailor the surgery to your needs and ensure you feel prepared and informed before the procedure.
What happens during the procedure?
A hysterectomy is performed under general anaesthesia and typically takes between one and three hours. The exact duration will depend on the surgical approach your doctor uses and the complexity of your individual case.
Abdominal hysterectomy
An incision is made in your lower abdomen to access and remove your uterus. This open approach offers the best visibility for complex cases, especially when you have extensive endometriosis or adhesions (scar tissue that can cause nearby organs to stick together).
Vaginal hysterectomy
Your uterus is removed entirely through your vagina, with no external incisions, which means no visible scarring on your abdomen. This approach is suitable when your uterus is smaller and your endometriosis is less extensive. Many women find the recovery from this approach a little more comfortable.
Laparoscopic or robotic hysterectomy
Small incisions are made in your abdomen, and a tiny camera alongside specialist instruments is used to guide the procedure. This minimally invasive approach generally means less pain and a faster recovery, and it is often recommended when your surgeon is experienced in laparoscopic surgery.
During surgery, your surgeon may also remove endometriotic deposits, adhesions, or fibroids depending on what they find and what has been discussed with you beforehand.
What is recovery like after a hysterectomy for endometriosis?
Your body needs time to adjust after surgery, and the pace of recovery can vary depending on the type of hysterectomy and the surgical approach used.
How quickly you recover depends on your surgical approach:
For an abdominal hysterectomy, full recovery usually takes six to eight weeks
After a vaginal or laparoscopic hysterectomy, most women can return to normal activities within four to six weeks
In the first few days, you may stay in the hospital for one to three days. You might notice pain, tiredness, and mild vaginal bleeding or discharge during the first week, but these are all normal signs that your body is healing. They usually ease gradually over the first week.
Returning to normal activities
What feels “normal” for one person may be very different for another. So it’s important to listen to your body and progress at a pace that feels safe and comfortable.
Here is a general guide to help you plan:
Activity | Typical recovery time | Notes |
Desk work | 2 to 4 weeks | Return once you feel comfortable sitting for long periods |
Physical work (heavy lifting and standing) | 6 to 8 weeks | Only resume when you can do so without pain |
Driving | 2 to 3 weeks | When you can brake comfortably and are no longer taking strong pain relief |
It is generally advisable to avoid sexual intercourse for around six weeks after surgery, giving your body the time it needs to heal fully. Your follow-up appointment at this point gives your doctor the chance to check on your recovery and address any questions or concerns you may have.
Emotional recovery after surgery
Some people feel relieved to finally be free of pain. Others may feel uncertain about changes to their body or have concerns about intimacy.
You may experience:
Grief or sadness, particularly around fertility
Anxiety about sexual function or body image
Changes in mood, especially if menopause is triggered
These feelings are valid and deserve attention. You may speak to your doctor if you are struggling emotionally after surgery.
Taking good care of yourself during recovery, including rest, nourishing food, and gentle activity as you heal, can support both your physical and emotional wellbeing.
What are the risks of hysterectomy for endometriosis?
Like any major surgery, a hysterectomy carries some risks. Your surgeon will always take the time to walk you through everything before your operation.
Possible complications can include:
Bleeding during or after surgery
Infection at the surgical site
Injury to nearby organs such as the bladder or bowel
Blood clots
Temporary difficulties with urination or bowel movements
Most women come through surgery without experiencing these complications. Your surgical team will monitor you closely throughout and after the procedure to pick up on and address any concerns as quickly as possible.
How much does a hysterectomy cost in Singapore?
Understanding the costs involved can help you plan ahead and go into surgery feeling more at ease. In Singapore, costs vary depending on hospital type, case complexity, ward class, and length of hospital stay.
Based on Ministry of Health (MOH) benchmarks for complicated hysterectomy with severe endometriosis at private hospitals:
Surgeon fee: SGD 7,848 to SGD 12,535
Anaesthetist fee: SGD 2,398 to SGD 3,488
Doctor attendance: SGD 230 to SGD 450 per day
Bill amounts are intended as a general guide by the Ministry of Health Singapore. Actual costs may vary depending on your condition, treatment plan, and choice of hospital. Please check with your hospital for a more accurate estimate.
Your hospital's billing or patient services team can provide a personalised estimate based on your specific clinical needs and insurance coverage. Request an appointment with Thomson Medical to discuss your hysterectomy options and get guidance on the costs and payment plans tailored to your situation.
FAQ
Can a hysterectomy cure endometriosis?
A hysterectomy is not considered a cure for endometriosis, but it can significantly reduce or eliminate symptoms, particularly period-related pain, when the uterus and ovaries are removed. If endometriosis has spread to other organs such as the bladder or bowel, some symptoms may remain, and further treatment could be needed.
How does a hysterectomy for endometriosis affect fertility and hormonal balance?
A hysterectomy means a woman can no longer become pregnant. If the ovaries are removed at the same time, the body enters surgical menopause, which can bring on hot flushes, night sweats, vaginal dryness, and mood changes. Women who keep their ovaries are less likely to experience these effects, though some hormonal changes may still occur.
What are the potential risks and benefits?
For many women, the main benefit is lasting relief from pelvic pain, heavy periods, and the need for ongoing medication or repeated procedures. On the other hand, risks include bleeding, infection, injury to nearby organs, and blood clots. If the ovaries are removed, women may also experience hormonal changes, pelvic floor weakness, and changes in sexual function.
Does endometriosis grow back after a hysterectomy?
It can. If the ovaries are kept or if affected tissue remains on the bowel, bladder, or surrounding areas, the condition may return. Regular follow-up is advisable after surgery.
Is a hysterectomy the only option for severe endometriosis?
No. A hysterectomy is generally considered when symptoms are severe, significantly affect quality of life, and have not improved with other treatments. Other options, including hormonal therapies and laparoscopic surgery to remove affected tissue, may be explored first, particularly for women who wish to preserve fertility.
What type of hysterectomy is recommended for endometriosis?
The most common approach is a total hysterectomy, where the uterus and cervix are removed. In some cases, the ovaries and fallopian tubes are removed as well, particularly if they are affected by endometriosis. The extent of the procedure depends on the severity of the disease and the woman's individual circumstances.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and advice based on your unique situation, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
Reference:
Ministry of Health, Singapore. (n.d.). TOSP-SI731U bill information. https://www.moh.gov.sg/managing-expenses/bills-and-fee-benchmarks/cost-financing/tosp-si731u-bill-information/
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
