Finding a lump in your breast during a self-examination can be alarming, and it is understandable to want to know what it means as soon as possible. Most breast lumps are non-cancerous, and many are linked to normal hormonal changes in the body.
Two conditions that are often confused are fibrocystic breast changes and breast cancer. While both can cause lumps, they are very different in nature, behaviour, and what they mean for your health.
Knowing the differences between the two, what each one looks and feels like, and when to seek medical advice can help you feel more informed and prepared if you ever notice a change in your breasts.
What are “fibroid cysts” in the breast?
Fibrocystic breast changes are a common, non-cancerous condition where your breast tissue develops lumps or fluid-filled sacs, often in response to the natural hormone shifts of your menstrual cycle.
You may have come across the term 'fibroid cyst', but it is not a standard medical term. Fibroids actually refer to growths in the uterus, not the breast.
You might notice:
General breast tenderness or soreness, especially in the days before your period
Lumps or areas of thickened tissue, which may be smooth and movable, or firm and fixed.
Clear or milky nipple discharge from both breasts
Although these symptoms can be uncomfortable, they are usually harmless and reflect your body's normal hormonal cycle.
What is breast cancer?

Breast cancer develops when cells in your breast start to grow in an uncontrolled way, most often in the milk ducts (known as ductal carcinoma, the most common type) or the lobules, which are the milk-producing glands (known as lobular carcinoma).
Signs you may notice include:
A firm, persistent lump that does not change with your menstrual cycle
Spontaneous nipple discharge, particularly if it is bloody or only from one breast
Skin changes such as dimpling, puckering, redness, or a texture similar to orange peel
Nipple inversion or any change in nipple position
A noticeable change in the size or shape of one breast
Early detection is important. Finding breast cancer at an earlier stage generally means more treatment options are available to you and outcomes are better. Regular breast screenings and consulting a doctor promptly if anything unusual appears are important steps.
Fibrocystic breast changes vs breast cancer: What are the key differences?
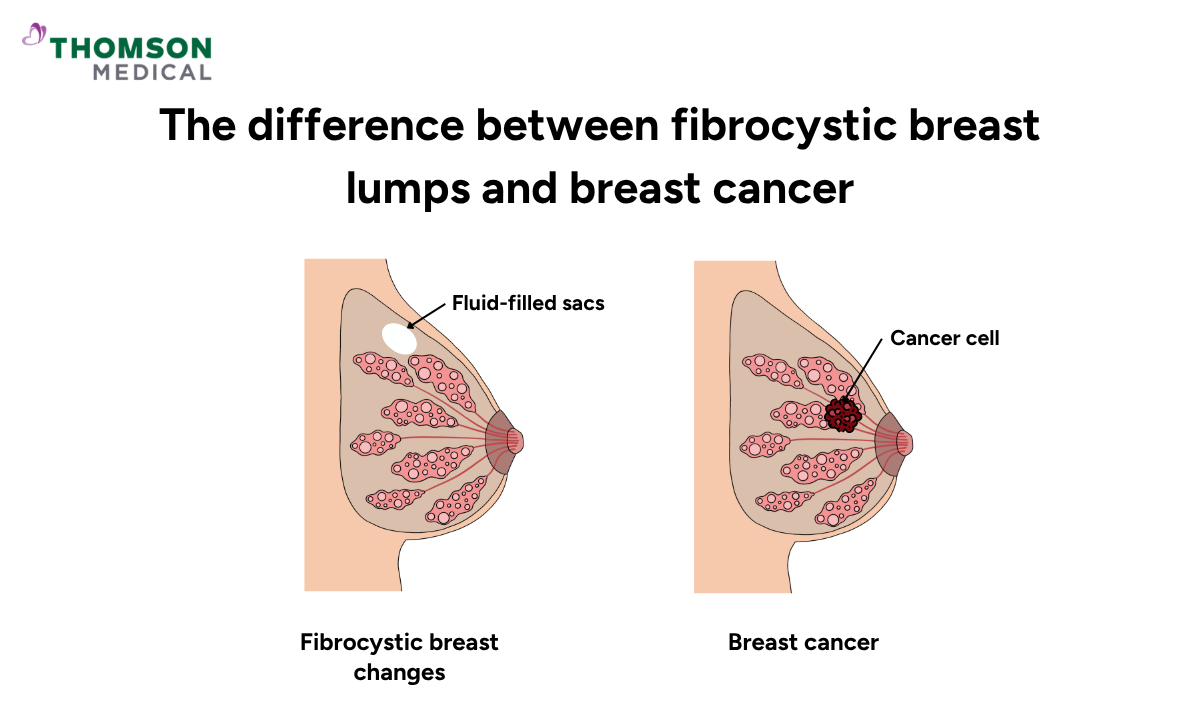
The table below shows general patterns to help you understand the differences. However, only your doctor can give you a definitive answer.
Feature | Fibrocystic breast changes | Breast cancer |
| Nature | Benign (non-cancerous) | Malignant (cancerous) |
Feel and texture | Smooth, round, soft or firm | Often hard or firm, with an irregular shape |
Mobility | Moves easily under the skin | Often fixed to nearby tissue or skin |
Pain | Often tender, especially before your period | Usually painless, though not always |
Changes over time | Size may rise and fall with your cycle | Tends to grow steadily, independent of your cycle |
Skin changes | No skin change | Possible dimpling, redness, or nipple inversion |
These are general patterns rather than strict rules, and they cannot be confirmed on your own. Your doctor can help assess your symptoms and arrange the right tests if needed.
If you notice a breast lump or are concerned about changes in your breasts, speak to your doctor promptly. You may request an appointment with Thomson Medical to discuss your concerns and receive professional guidance on the next steps.
Types of benign breast lumps
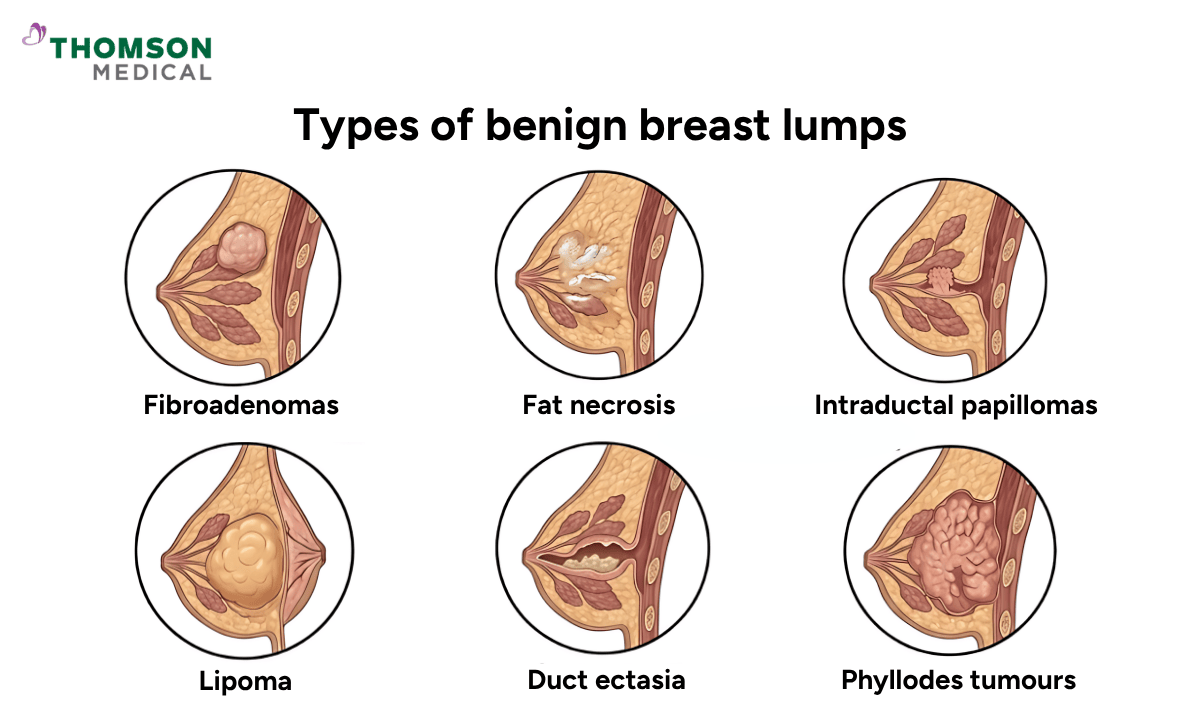
Other than fibrocystic breast changes, most lumps in the breast turn out to be non-cancerous, which is reassuring for many women. Knowing what kinds exist can help you have a more informed conversation with your doctor.
The most common are:
Fibroadenomas:
Smooth, firm lumps that move easily under your skin.
They are most common in women in their 20s and 30s and are almost always non-cancerous.
Fat necrosis:
Firm, round lumps that may feel tender when you press on them.
They often develop after an injury or surgery to your breast and are not cancerous.
Intraductal papillomas:
Small growths inside your milk ducts.
They may cause clear or bloody nipple discharge, usually from one breast only.
Lipomas:
Soft, painless lumps made of fatty tissue that sit just beneath your skin.
They tend to grow slowly and rarely cause any discomfort.
Duct ectasia
A condition where your milk ducts widen and may fill with fluid.
It is more common in women in their 40s and 50s and may cause nipple discharge or mild discomfort around your nipple.
Phyllodes tumours:
Rare growths that develop in the supporting tissue of your breast.
Most are non-cancerous, but a small number can be borderline or cancerous, so they are always assessed carefully by a specialist.
They can grow quickly, so it is important to have them checked promptly if your doctor suspects one.
Most of these lumps do not need treatment, but some require monitoring or removal depending on their size, behaviour, or any symptoms they cause. Your doctor will explain what is appropriate for your situation.
How are breast lumps diagnosed?
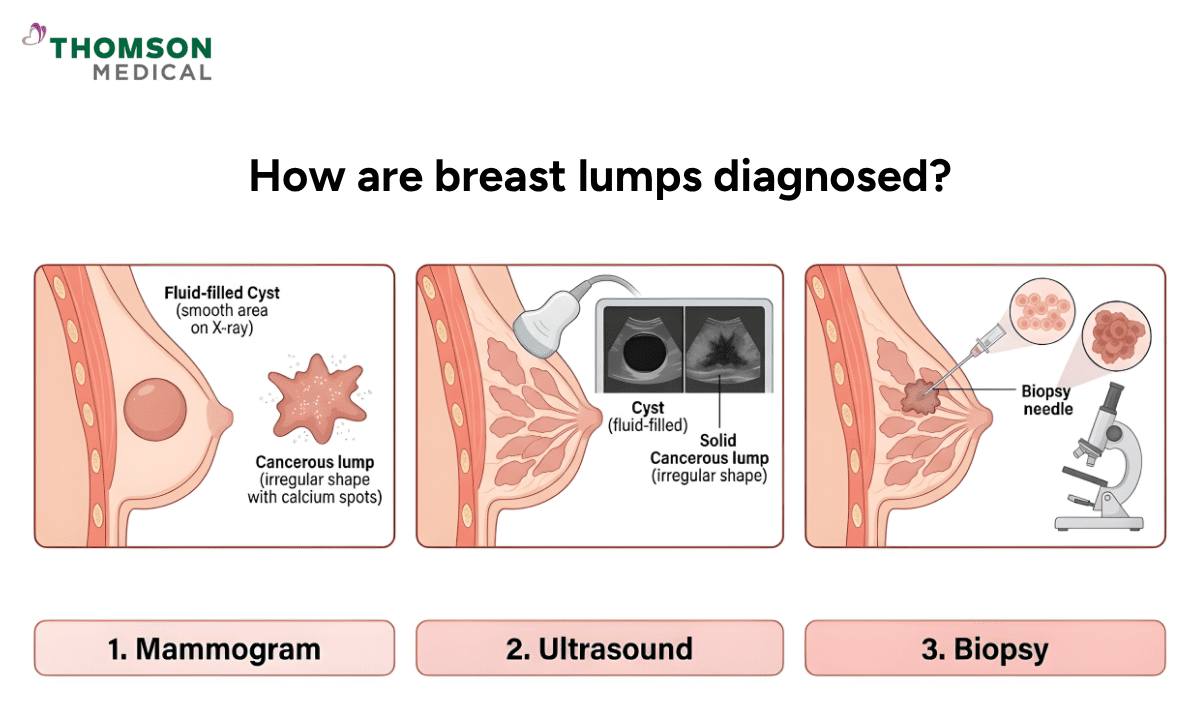
It is understandable to feel anxious about tests, but the diagnostic process is designed to give you clarity as quickly as possible. Your doctor may use a combination of imaging and, if needed, a small tissue sample to understand exactly what your lump is.
Mammogram
A mammogram is a low-dose X-ray of your breast that can pick up lumps and other changes, sometimes before you can feel them.
If you have fibrocystic breast changes, your lumps often appear as smooth, round areas on the scan. A mammogram cannot always tell whether a lump is fluid-filled or solid, so an ultrasound is usually used alongside it.
Cancerous lumps may look irregular or have an irregular, star-like shape (sometimes described as 'spiculated') and can sometimes show tiny specks of calcium (called 'microcalcifications', which can sometimes indicate abnormal cell activity).
Ultrasound
A breast ultrasound uses sound waves to create images of your breast and is a comfortable, radiation-free way to look at a lump more closely.
It is especially helpful for telling whether a lump is fluid-filled (a cyst) or solid. Cysts linked to fibrocystic breast changes usually appear smooth, round, and dark on ultrasound. Solid lumps vary.
Because it shows the inside of a lump in more detail, ultrasound is often used together with a mammogram for a clearer overall picture.
Biopsy
If imaging suggests further investigation is needed, your doctor will carry out a breast biopsy to remove a small sample of tissue for testing. It is the only way to know for certain whether a lump is cancerous.
Although the idea of a biopsy can feel daunting, it is usually a quick procedure done under local anaesthetic. Results will show whether the lump is non-cancerous or cancerous. If cancer is found, the biopsy also reveals the type, which helps your doctor plan the most appropriate care.
Our breast health specialist
Loading...
What are the treatment options for fibrocystic breast changes?
Most lumps or cysts linked to fibrocystic breast changes do not need treatment at all. They often settle on their own as your hormones shift through your cycle.
If a cyst becomes uncomfortable or noticeably large, the following options may help ease your symptoms:
Taking pain relief to ease discomfort
Wearing a well-fitting supportive bra for added daily comfort
Taking medication if your doctor recommends it
If your cysts persist or keep coming back, a minor procedure may help:
Fine needle aspiration (a quick procedure where your doctor uses a thin needle to draw out the fluid), which often relieves discomfort straight away
Surgical removal, which is rare and usually only considered for cysts that keep returning, are unusually large, or cause ongoing concern
Most women can continue with their usual daily activities. It is still worth paying attention to any changes in your breasts. If you notice a lump increasing in size, new symptoms, or persistent discomfort, see your doctor promptly.
What are the treatment options for breast cancer?
Your treatment depends on several factors, including the stage of the cancer, its type, your overall health, and in some cases your BRCA gene status.
Surgery
Surgery is often a key part of your treatment, used to remove the tumour and lower the chance of cancer spreading.
Depending on the size and location of the cancer, this may involve:
Lumpectomy:
Removing the tumour while preserving as much of the breast as possible
Mastectomy:
Removing all of the breast tissue, sometimes with options for reconstruction
The choice between lumpectomy and mastectomy depends on tumour size, location, cancer type, and your personal preferences. In many cases, both options offer similar long-term outcomes, and your surgical team will help you consider what matters most to you.
Other treatments (before or after surgery)
Many women receive additional treatments alongside surgery, either to prepare for it or to reduce the risk of the cancer returning afterwards.
Before surgery (neoadjuvant therapy):
Treatments such as chemotherapy or hormone therapy may be used to shrink your tumour before surgery. This can sometimes make breast-conserving surgery possible.
After surgery (adjuvant therapy):
Further treatment may be recommended to lower the chance of your cancer coming back.
These additional treatments can include:
Chemotherapy:
Uses medication to target cancer cells throughout the body and may be used at different stages of breast cancer.
Radiotherapy:
Uses targeted energy beams to lower the chance of cancer returning in your breast, chest wall, or nearby lymph nodes after surgery.
Hormone therapy:
For cancers that are sensitive to oestrogen or progesterone, this treatment helps slow or stop their growth.
Targeted therapy:
Works on specific features of the cancer cells, such as certain proteins or genes, and is sometimes given alongside chemotherapy.
Immunotherapy:
A newer option that helps your immune system recognise and respond to cancer cells, used for certain types of breast cancer.
Throughout your treatment, your care team will explain each step, address your concerns, and help you understand the options available to you. Treatment plans are tailored to each woman's individual circumstances, and yours will be no different.
If you would like a clearer understanding of your diagnosis and treatment options, request an appointment with Thomson Medical. Our specialists can help you make informed decisions about your care.
FAQ
Can fibrocystic breast changes increase the risk of breast cancer?
For most women, no. These changes do not cause cancer, but they can sometimes make your breast tissue appear denser, which makes it a little harder for doctors to interpret your mammogram results.
If a separate finding called atypical hyperplasia (an unusual overgrowth of cells in the breast tissue) is identified alongside the fibrocystic changes, the risk of developing breast cancer is somewhat higher than average.
Are fibrocystic breast changes dangerous?
No. Fibrocystic breast changes are generally harmless for most women. They often rise and fall with your menstrual cycle and may settle on their own.
Can you have fibrocystic breast changes and breast cancer at the same time?
Yes, although this is uncommon. Having fibrocystic changes does not protect you from breast cancer, and the two can coexist independently. This is one reason your doctor may recommend imaging even when a lump seems likely to be benign. It helps confirm the nature of the lump and rule out anything else.
If atypical hyperplasia is identified alongside fibrocystic changes, the risk of breast cancer is slightly higher than average.
Do the cysts associated with fibrocystic breast changes go away on their own?
Often, yes. These cysts can decrease in size or resolve naturally over time. If you are premenopausal, your cysts may fluctuate with each cycle, sometimes more noticeable, sometimes less. After menopause, fibrocystic changes often ease as your hormone levels settle.
What does a cancerous lump feel like compared to a cyst from fibrocystic breast changes?
As a general pattern, cancerous lumps are often hard, irregular in shape, and feel fixed to the surrounding tissue. Cysts linked to fibrocystic breast changes tend to feel smoother and rounder and move more easily under the skin.
Can fibrocystic breast changes cause breast pain?
Yes, they often can. Fibrocystic breast changes can cause tenderness or discomfort, especially in the days leading up to your period. This is usually linked to the natural rise and fall of your hormones during the menstrual cycle, and it tends to ease once your period begins.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
