If you are preparing for a hysterectomy, it is natural to have questions about recovery and what to expect in the months ahead. Some women also wonder whether pelvic organ prolapse can occur after the uterus is removed.
While this concern can feel unsettling, there are practical steps you can take to support your pelvic floor and reduce the risk. Understanding why prolapse may happen after a hysterectomy and learning how to protect your pelvic floor during recovery and beyond can help you feel more confident about your long-term health.
Why prolapse may happen after hysterectomy
Pelvic organ prolapse happens when one or more pelvic organs shift from their usual position and press downward toward the vaginal canal. This occurs when the muscles and tissues that normally support these organs – the pelvic floor – become weakened or stretched.
For many women, prolapse is not life-threatening, but it can bring a constant sense of heaviness or discomfort in the pelvic area. Over time, this pressure can make everyday activities feel less comfortable. Standing for long periods, exercising, or even simple daily routines may become bothersome.
After a hysterectomy, the structure of the pelvis shifts slightly. The surrounding tissues still provide support, but the pelvic floor muscles need time to adjust to those changes.
Certain factors that can put extra strain on your pelvic floor and raise the chance of prolapse over time include:
Weak or stretched pelvic floor muscles:
These muscles can lose strength gradually due to pregnancy, childbirth, ageing, or inactivity.
Changes to connective tissue during surgery:
Some of the tissue that helps support the pelvic organs can be stretched or affected during the procedure.
Ongoing pressure in the abdomen:
Things like obesity, a persistent cough, or chronic constipation can repeatedly push down on the pelvic floor, adding strain over time.
Ageing and menopause:
As oestrogen levels drop, pelvic tissues can become thinner and less flexible, which gradually reduces natural support.
Lifting too soon after surgery:
Picking up heavy objects before the body has properly healed can put unnecessary pressure on the pelvic floor and the surgical repair.
That said, many women recover well after a hysterectomy and maintain good pelvic support. With the right recovery approach, regular pelvic floor exercises, and a few lifestyle adjustments, you can protect yourself going forward.
Lifestyle changes to reduce prolapse risk
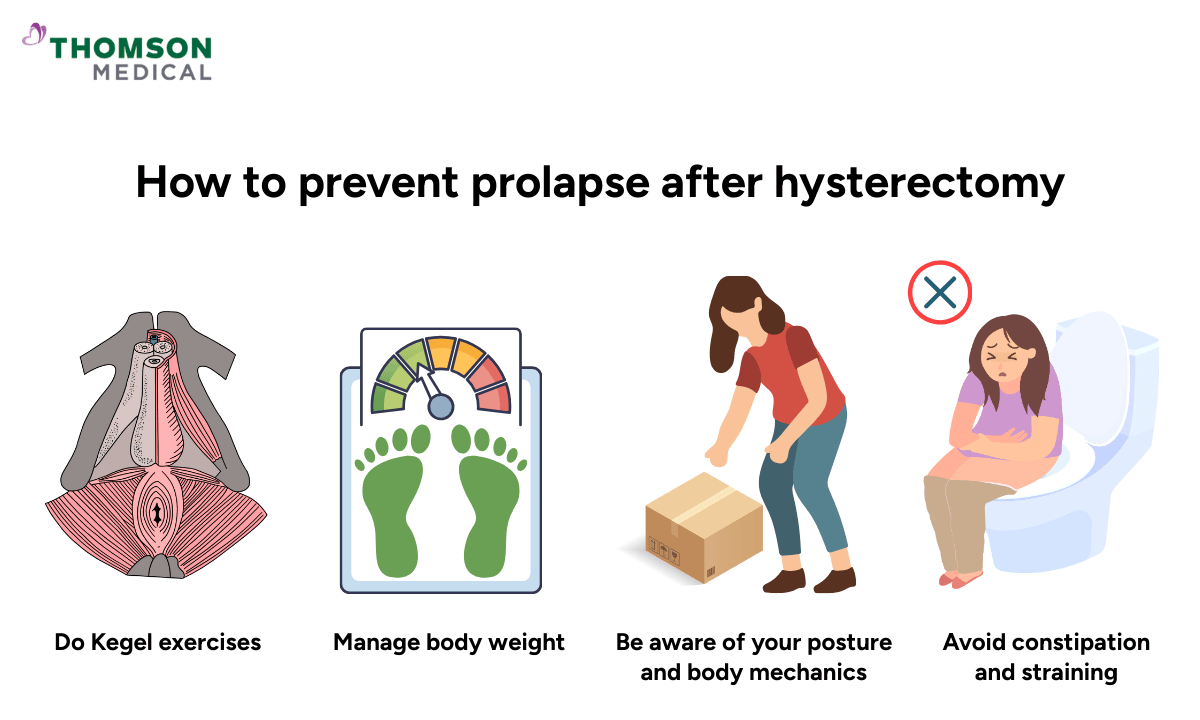
Several everyday habits can help reduce pressure on your pelvic floor and support your recovery over the long term.
Weight management
Carrying extra body weight adds ongoing pressure to the pelvic floor muscles, which over time can strain the tissues holding the pelvic organs in place.
Gradual lifestyle changes such as balanced nutrition and regular gentle exercise can help support both your pelvic health and your general wellbeing.
Posture and body mechanics
The way you move your body throughout the day can influence how much pressure is placed on your pelvic floor.
A few things worth building into your routine:
Avoid heavy lifting where you can
Bend your knees rather than your waist when picking something up
Gently engage your core and pelvic floor before lifting, even for lighter objects
After a hysterectomy, becoming more aware of how you move, especially how you lift, is one of the simpler protective steps you can take.
Avoid constipation and straining
Straining during bowel movements repeatedly pushes pressure into the abdomen, which puts stress on the pelvic floor. Keeping your digestion regular is therefore a quiet but important part of pelvic care.
Some practical ways to reduce the risk of constipation:
Drink enough water throughout the day
Include fibre-rich foods, such as fruits, vegetables, and whole grains, in your meals
Stay as active as your doctor allows
These habits help maintain regular bowel movements and reduce the need for straining.
Hormonal support
Hormonal shifts, especially during menopause, can affect how strong and elastic your pelvic tissues are. As oestrogen levels fall, these tissues can gradually thin and lose some of their natural support.
In some cases, your doctor may suggest local oestrogen therapy to help maintain vaginal and pelvic tissue health. It is not necessary for everyone, but it is worth discussing as part of longer-term pelvic care if it feels relevant to you.
Kegel exercises
One of the most practical things you can do to reduce the risk of prolapse after a hysterectomy is to work on strengthening your pelvic floor muscles.
Building their strength can help with:
Better support for the pelvic organs
Less pressure or bulging sensations
Improved bladder and bowel control
Better sexual function
More protection when lifting, coughing, or exercising
You do not need a complicated fitness routine to get there. Simple exercises like Kegels, done consistently, can gradually build both strength and support.
How to do Kegel exercises correctly
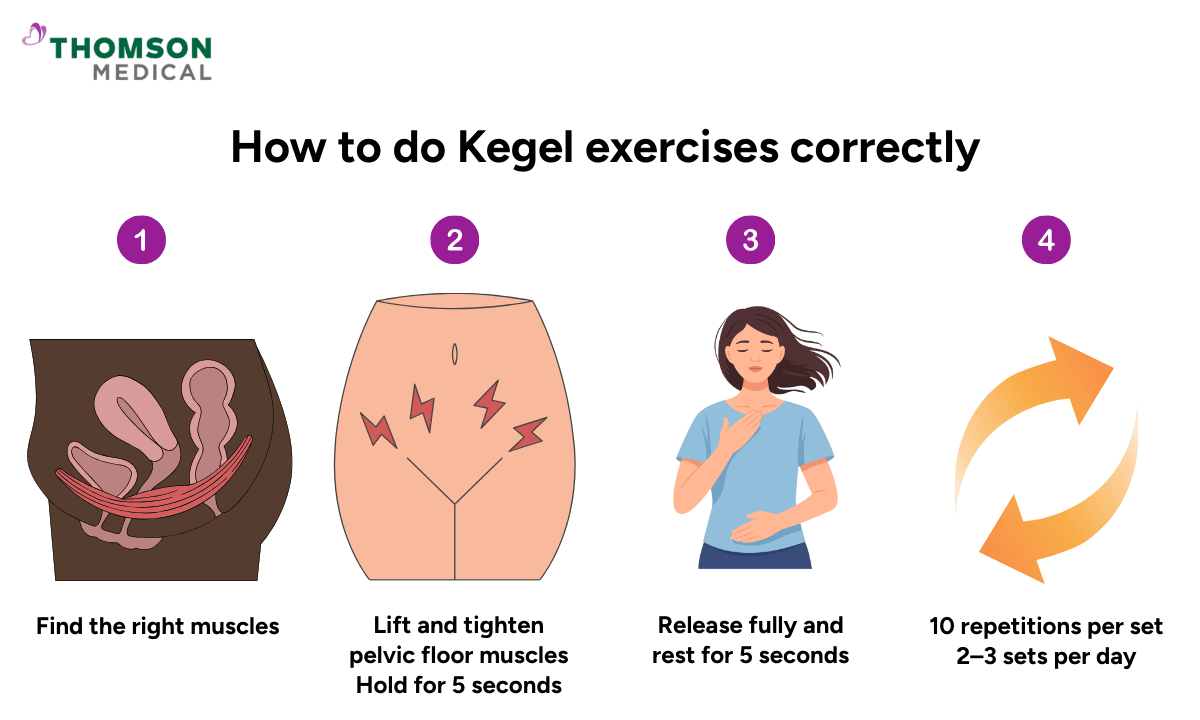
Kegel exercises are commonly recommended after pelvic surgery to help strengthen the muscles that support the bladder, bowel, and vagina. Even so, many women aren’t quite sure how to do them properly.
Here is a simple way to get started:
Step 1: Find the right muscles
Before starting the exercise, it is important to identify your pelvic floor muscles.
A good way to find them is to imagine you are stopping the flow of urine or holding in gas. The muscles you gently tighten in that moment are the ones you are looking for.
When you activate them, focus on lifting and tightening without tensing your abdomen, thighs, or buttocks.
Step 2: Practise the proper technique
Once you identify where the muscles are, you can start practising by following these steps:
Breathe normally and keep the rest of your body relaxed
Gently lift and tighten the pelvic floor muscles
Hold for about 5 seconds
Release fully and rest for 5 seconds
The movement should feel like a quiet internal lift – not a push or a strain.
Step 3: Repetitions
Start with 10 repetitions per set, two to three times a day. Doing a smaller number consistently tends to work better than occasional large sessions. Over time, your muscles will become stronger and more responsive.
Common mistakes to avoid
When doing Kegel exercises, a few small adjustments can help make the exercise more effective:
Holding your breath instead of breathing normally
Bearing down or pushing outward instead of gently lifting the pelvic floor
Squeezing continuously without letting the muscles fully relax
If you are not sure whether you are engaging the right muscles, a physiotherapist can walk you through the technique and make the process a lot more comfortable.
When to start exercising Kegel after surgery
Many doctors suggest starting with gentle pelvic floor activation once the early recovery phase has passed – often around one to two weeks after surgery. Structured Kegel exercises are often introduced between two and six weeks.
However, the right time depends on the type of procedure you had and how your recovery is going. It’s best to consult and follow your doctor's advice to ensure your body is ready before you start any exercise.
Want to protect your pelvic floor after a hysterectomy? Schedule a consultation with our gynaecologists at Thomson Medical to learn how pelvic floor exercises, lifestyle changes, and tailored care can support your recovery and reduce the risk of prolapse.
Our gynaecologists in Singapore
Loading...
Signs your pelvic floor needs attention
Even with the best preventive habits in place, it’s important to know what to look out for. Some symptoms can be a sign that your pelvic floor needs a closer look.
Speak to your doctor if you notice any of the following:
A feeling of pressure or heaviness in the pelvis
A bulge or sensation of tissue in the vaginal area
Difficulty emptying your bladder or bowel
Urinary leakage or worsening bladder control
Discomfort during physical activity
These symptoms don’t always mean prolapse is present, but getting checked early can help identify any issues and address them appropriately before they progress.
If you notice any of these signs and are worried about pelvic organ prolapse, schedule a consultation with Thomson Medical. Our gynaecologists can assess your symptoms, provide personalised advice, and guide you on the most appropriate care for your pelvic health.
FAQ
How soon after a hysterectomy can I start pelvic floor exercises?
Gentle pelvic floor awareness exercises may begin about 1 and 2 weeks after surgery, if your doctor approves. Structured Kegel exercises are often introduced between 2 and 6 weeks, depending on your recovery.
How much weight can I lift after a hysterectomy?
During the first 6 weeks, your doctor usually recommends lifting no more than 2–4.5 kg. After your doctor clears you, you can gradually return to heavier lifting. Try to breathe normally and avoid holding your breath while lifting.
Can I prevent prolapse if I'm overweight?
Yes, losing excess weight can reduce pressure on the pelvic floor and may lower the risk of prolapse.
What are the first signs of prolapse after hysterectomy?
Early signs of prolapse after hysterectomy may include:
A feeling of pressure or heaviness in your pelvis
A bulging sensation in the vagina
Difficulty with bladder or bowel control
Can coughing or sneezing cause prolapse after surgery?
Occasional coughing or sneezing is usually not a problem. However, frequent or forceful coughing can increase pressure on your pelvic floor. Gently engaging your pelvic floor before coughing may help provide support.
Do I need to do Kegel exercises forever after a hysterectomy?
Pelvic floor exercises are most helpful when practised regularly over time. Many doctors recommend continuing them as part of long-term pelvic health, like maintaining other healthy habits.
The information is intended for general guidance only and should not be considered medical advice. For personalised recommendations and advice based on your unique situation, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
