Being told that you may need surgery for an ovarian cyst can feel worrying. Many women wonder how the procedure works, how long recovery takes, and whether it could affect their fertility.
An ovarian cystectomy is a surgery that removes the cyst while preserving the ovary whenever possible. Understanding how the procedure works and when it is recommended can help you feel more prepared when discussing treatment options with your doctor.
What is an ovarian cystectomy?
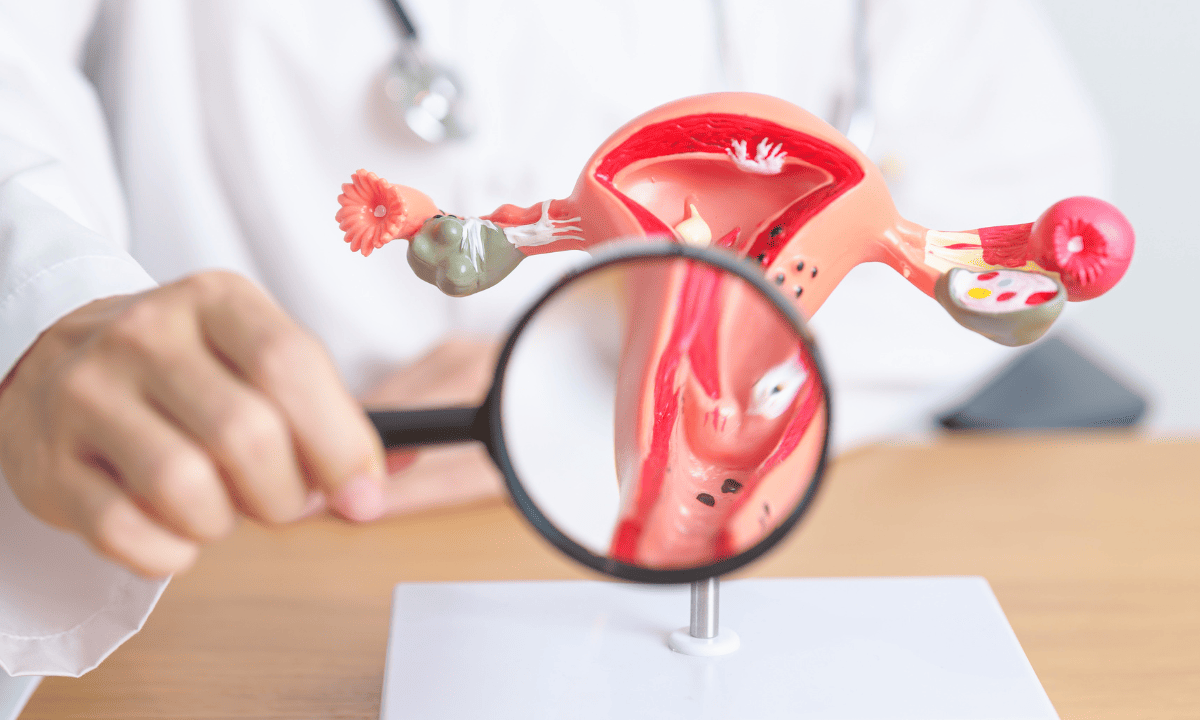
An ovarian cystectomy is a surgical procedure that removes an ovarian cyst while preserving the healthy ovarian tissue. Unlike an oophorectomy, which removes the entire ovary, this approach focuses on treating the cyst while maintaining hormone production and fertility whenever possible.
This approach is especially important if you are of reproductive age, as it helps protect your ovarian tissue. By preserving the ovary, your doctor aims to maintain normal hormone production and support your potential for future pregnancy.
An ovarian cystectomy is most commonly recommended for ovarian cysts that are benign, meaning they are non-cancerous. The goal is to relieve symptoms such as pain or reduce potential risks while keeping your reproductive system as healthy and intact as possible.
When is ovarian cyst removal needed?
It can be reassuring to know that most ovarian cysts do not need surgery. Many are functional cysts, such as follicular cysts, which form naturally during your menstrual cycle and often go away on their own without any treatment.
That said, there are situations where your doctor may advise removing the cyst. This is usually because your cyst might pose certain risks or is causing ongoing symptoms that cannot be managed with observation alone.
Surgery may be recommended if:
The cyst is large and continues to grow
You have persistent or severe pelvic pain that interferes with your daily life
The cyst looks complex or unusual on an ultrasound scan
There is a risk of complications, such as twisting of the ovary (torsion) or rupture
The cyst is suspected to be an endometrioma linked to endometriosis, or a dermoid cyst
Doctors generally prefer a conservative approach whenever it is safe, carefully monitoring the cyst over time. However, if a cyst does not shrink or continues to cause symptoms, surgery may be the best way to address the issue early and prevent further complications.
If you have any concerns about an ovarian cyst or are noticing ongoing symptoms, you can request an appointment at Thomson Medical. During a consultation, our doctor can help you understand your individual situation and discuss any suitable management options.
How are ovarian cysts diagnosed before surgery?
Before recommending surgery, your obstetrics and gynaecology (O&G) specialist will carry out a careful and thorough evaluation to understand exactly what is happening in your body. This step-by-step process helps ensure that surgery is the right option for you.
The assessment usually includes:
Medical history and symptoms:
Your doctor will talk through your symptoms, such as pelvic pain or bloating, and review your medical and menstrual history.
Physical examination:
A pelvic examination may be performed to check for tenderness or any noticeable masses.
Pelvic ultrasound:
This is the main imaging tool used to examine the ovaries.
A transvaginal ultrasound often provides the clearest view, allowing your doctor to assess the size, shape, and features of the cyst.
Blood tests:
Your doctor may use certain blood tests to check hormone levels and tumour markers such as CA125.
A higher CA125 level does not automatically mean cancer. It can also be raised in common, non-cancerous conditions such as endometriosis.
CT scan or MRI scan:
In more complex cases, a computed tomography (CT) scan or magnetic resonance imaging (MRI) scan may be recommended to give a clearer, more detailed view of the cyst and surrounding pelvic cavity.
Together, these investigations help your medical team distinguish between simple fluid-filled cysts and more complex growths, such as dermoid cysts or endometriotic cysts, so you can receive the most appropriate and personalised care plan.
Our women’s health specialist
Loading...
What is minimally invasive (laparoscopic) cystectomy?
In Singapore, ovarian cysts are most often removed using minimally invasive surgery (MIS) (also known as laparoscopic surgery or keyhole surgery). This modern approach allows surgeons to work with great precision, without the need for large cuts.
The benefits of MIS include:
Minimal scarring due to the small incisions
Less pain during recovery
A shorter hospital stay, often as a day surgery
A quicker return to daily activities
For most benign ovarian cysts, this technique is considered the gold standard because it focuses on faster recovery while keeping your comfort front and centre.
How does laparoscopic cystectomy compare to open surgery?
While laparoscopic surgery is the most common approach, it is helpful to understand how it differs from open surgery (laparotomy) so you can feel fully informed about your options.
Type | Laparoscopic surgery | Open surgery |
Incisions | 3 to 4 tiny cuts (0.5 to 1 cm) | A single larger incision (similar to a C-section cut) across your abdomen |
Usage | Commonly used for most ovarian cyst removals | Reserved for very large cysts, suspected ovarian cancer, or when laparoscopic removal is not safe |
Recovery | Faster recovery, with most women returning to light activities within 1 to 2 weeks | Longer recovery, usually involving several days in hospital and a few weeks of rest at home |
Discomfort | Generally less post-operative pain, often requiring less medication | More postoperative discomfort due to the larger incision |
Both surgical approaches are widely used and carefully chosen based on what is safest and most appropriate for your individual situation. Your doctor will consider factors such as the size and nature of the cyst, your symptoms, and your overall health before recommending the best option.
While the idea of surgery can feel overwhelming, many women recover well with the right support, guidance, and time to heal.
What happens during an ovarian cystectomy procedure?
Knowing what happens in the operating theatre can help ease anxiety and make the experience feel less daunting. The procedure is carried out under general anaesthesia, which means you will be fully asleep and will not feel any pain during the surgery.
The process generally includes the following steps:
Preparation:
Once you are asleep, your abdomen is gently inflated with gas to create space for the surgeon to see clearly.
Access:
Small incisions are made to insert a camera and specialised surgical instruments.
Removal:
Your surgeon carefully identifies the cyst and separates it from the healthy ovarian tissue.
They take great care to peel the cyst wall away while protecting the ovary’s blood supply.
Preservation:
The remaining ovarian tissue is preserved as much as possible.
If needed, your ovary is carefully stitched back into its natural shape.
Closure:
The cyst is placed into a protective bag and removed through one of the small incisions.
Your surgeon then closes the cuts using dissolvable stitches or surgical glue.
The procedure typically lasts around 1 to 2 hours, depending on your individual situation. While you sleep, the surgical team keeps a close watch on your vital signs and works together to ensure your safety and wellbeing throughout the surgery.
If you want to discuss your condition and possible management options, you may request a consultation at Thomson Medical. Our specialists can assess your individual medical situation and explain the available options to help you make an informed decision about your care.
What are the risks and possible complications?
Ovarian cystectomy is generally considered a very safe procedure. Still, like any surgery, it comes with some potential risks, and understanding them can help you feel more prepared.
Possible complications include:
Infection:
You may develop a mild infection at the incision sites or in the bladder.
Doctors can usually treat these effectively with antibiotics.
Bleeding:
You might notice some minor bleeding after surgery, which is common.
Blood clots:
Surgery can slightly increase your risk of blood clots forming in your legs.
To lower this risk, your care team may give you compression stockings or preventive medication.
Injury to nearby organs:
In very rare cases, surgery may affect nearby organs such as the bladder or bowel.
Recurrence:
In some cases, ovarian cysts can return in the future, especially if you have conditions such as endometriosis.
Serious complications remain uncommon, particularly when the procedure is performed by experienced gynaecologists. Your medical team carefully plans every step of the procedure and takes active measures to reduce risks, prioritising your safety and recovery throughout your care.
Treatment options and facilities in Singapore
In Singapore, care for ovarian cysts is provided by doctors trained in women’s health in both public hospitals and private medical centres.
Your care plan will be based on your individual medical needs. During consultations, your doctor may talk with you about your symptoms, age, medical history, and any future fertility considerations so that you can make informed decisions about your treatment options together.
The cost of an ovarian cystectomy can vary depending on the hospital setting, the size and complexity of the cyst (for example, cysts larger than 5 cm), and your insurance coverage.
The costs listed below are estimated fees based on 2026 figures and may vary depending on the hospital, doctor, and individual treatment requirements.
Hospital setting | Estimated costs & fees |
Public hospitals | ~SGD 520 |
Private hospitals | Total: SGD 6,200 – SGD 14,000+
|
From your first consultation through recovery and follow-up, your care team focuses on your safety, comfort, and long-term wellbeing. You can ask questions, discuss your options openly, and feel reassured that your care team is guiding you at every step.
Financing your care
While surgical costs can feel overwhelming at first, several financial schemes can help reduce the burden:
MediSave:
You can use your MediSave savings to cover hospitalisation expenses such as ward charges, investigations, and medications.
MediShield Life and Integrated Shield Plans:
Insurance can significantly lower your out-of-pocket costs. In some cases, comprehensive coverage reduces expenses to a few hundred dollars.
Before your procedure, your doctor or a hospital financial counsellor will walk you through the estimated costs and available payment options. This conversation gives you time to ask questions, understand your coverage, and prepare for surgery with greater peace of mind.
FAQ
What can I expect after ovarian cystectomy?
After surgery, it is normal to notice some temporary changes as your body heals. You may experience mild to moderate pain for a few days, which usually improves with rest and prescribed pain relief.
Most people gradually return to their usual activities within 1 to 2 weeks. Recovery may take a little longer if you have open surgery. Recovery varies by individual and many patients start to feel significantly better within 2 to 4 weeks.
Will ovarian cystectomy affect my fertility or hormones?
In most cases, ovarian cystectomy does not affect fertility or hormone levels. During the procedure, the surgeon aims to preserve as much healthy ovarian tissue as possible. As a result, your hormones usually remain stable, and your ability to conceive typically stays the same. Protecting ovarian function is one of the main goals of this surgery.
What is the chance of ovarian cysts coming back after surgery?
Some cysts can return, particularly if you have underlying conditions such as hormonal imbalances or endometriosis, or if you have had ovarian cysts before. In certain situations, your doctor may recommend hormonal treatment to help reduce the risk of recurrence.
Can doctors perform cystectomy during pregnancy?
Doctors generally avoid surgery during pregnancy unless it is clearly necessary. If you have severe symptoms or complications, your care team will carefully consider the timing and approach. In many cases, doctors monitor pregnancy-related cysts closely instead of operating.
How do doctors decide between surgery and conservative treatment?
Your doctor looks at several factors before recommending treatment. These include your age, symptoms, the size and appearance of the cyst, and whether it changes over time on ultrasound. Many ovarian cysts do not require surgery and can be safely monitored with regular follow-up.
Do all ovarian cysts need surgery?
No. Most ovarian cysts are harmless, cause few or no symptoms, and resolve on their own over time. Doctors usually recommend surgery only when specific medical concerns arise.
Is ovarian cystectomy a major operation?
Ovarian cystectomy is usually considered minor to moderate surgery, especially when performed laparoscopically. Hospital stays are short, recovery tends to be smooth, and most people return to their normal routine relatively quickly.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) - Jurong:
6262 8588 (Call), 6262 8588 (WA) - Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
Notice
The range of services may vary between TWC/TS locations. Please contact your preferred branch directly to enquire about the current availability.
Request an Appointment