You may have heard the terms “polyps”, “cysts”, or “fibroids” during a doctor’s visit or while searching for answers online. When these terms relate to your own health, it’s natural to feel unsure about what they mean.
The good news is that these are common conditions affecting the female reproductive system, and most are not serious.
Understanding how they differ can help you feel more confident when discussing your diagnosis and deciding on the next steps.
What are polyps, cysts, or fibroids?
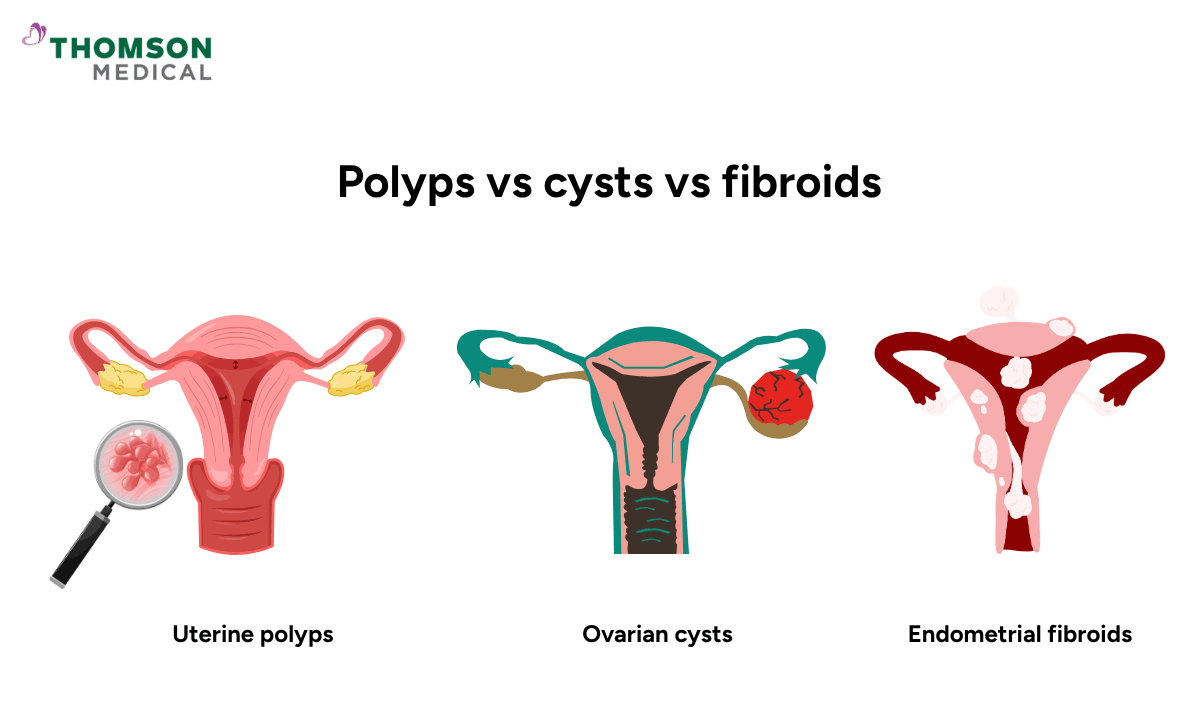
Uterine polyps, ovarian cysts and endometrial fibroids are growths that most often affect the reproductive organs in women, but they are not the same. The key difference lies in what they are made of and where they develop.
Here is a basic comparison to help you understand the differences:
Feature | Uterine polyps | Ovarian cysts | Endometrial fibroids |
What they are | Small growths from the lining of the uterus (endometrium) | Fluid-filled sacs in or on the ovary | Solid, non-cancerous muscle tumours in the uterus |
Where they occur | Inside the uterus | In the ovaries | Within or around the uterus |
Texture | Soft, flat or on a stalk | Fluid-filled | Firm, solid |
While they may share some similarities, knowing these key differences can help you understand what your doctor is saying and how it affects your health.
How do you tell if you have polyps, cysts, or fibroids?
Many women don't notice any symptoms, especially when the growths are minor.
When symptoms do appear, they often relate to your menstrual cycle or pelvic area:
Uterine polyps:
Irregular periods
Spotting between periods
Heavier periods in some cases
Ovarian cysts:
Pelvic pain or a dull ache on one side
Bloating or a feeling of fullness
Sudden pain if a cyst ruptures
Endometrial fibroids:
Heavy or prolonged menstrual bleeding
Pelvic pressure or fullness
Frequent urination or constipation
Your doctor may recommend the following to confirm the diagnosis:
Pelvic ultrasound
Hysteroscopy (for uterine polyps)
MRI in selected cases
These tests help your doctor identify the type of growth and whether treatment is needed
If you’ve noticed unusual symptoms or changes in your body, request an appointment with Thomson Medical. Our doctors can perform a physical examination to assess any growths you may have and determine whether it requires any treatment.
Our gynaecologists in Singapore
Loading...
What causes polyps, cysts, or fibroids?
You might be wondering why you get cysts, polyps, or fibroids. These conditions are often linked to hormonal changes, particularly oestrogen, although other factors may also play a role.
Uterine polyps | Ovarian cysts | Fibroids |
|
|
|
These growths frequently grow slowly and can happen even if you're otherwise healthy. That's why it’s best to see your doctor for regular checkups and to get medical care as soon as you notice any unusual symptoms.
How might polyps, cysts, and fibroids affect your health?
Hearing that you may have a polyp, cyst, or fibroid can naturally raise concerns about your health.
In many cases, these growths are small and do not cause significant issues.
When they do have an impact, it is often related to:
Menstrual changes (heavier, irregular bleeding)
Pelvic discomfort or pressure
Fertility challenges in some cases
Many women continue to live normally with these conditions, especially when they are monitored appropriately.
Can they turn into cancer or be harmful?
It is natural to worry about whether these growths could be cancerous. The good news is that most polyps, cysts, and fibroids are not cancerous.
Fibroids are almost always benign
Ovarian cysts are usually benign, especially functional cysts
Uterine polyps are usually harmless, though a small number may require closer evaluation
It’s important to remember that having one of these growths doesn't guarantee you have cancer. Your doctor usually monitors for any changes to identify early signs that may need closer attention and recommends treatment as necessary.
With regular checkups and prompt care, any possible concerns may usually be found early and managed well.
How are polyps, cysts, or fibroids treated?
Not all of these growths need immediate treatment.
Your doctor usually considers:
The size and type of growth
Whether it is causing symptoms
Your age, overall health, and future plans (such as fertility)
In many cases, your doctor will recommend one of the following:
Monitoring
You might not need treatment immediately if the growth is minor and not causing any problems.
Your doctor might instead recommend:
Regular ultrasound follow-up
Monitoring for any changes in size or symptoms
Many cysts, especially functioning ovarian cysts, might resolve on their own over time.
Medication
Medications are often used to manage symptoms or control underlying causes, rather than remove the growth completely.
This may include:
Hormone therapy to help regulate periods or reduce fibroid size
Pain relief for discomfort
Medications to control bleeding
Your doctor often uses this method to treat uterine fibroids and various kinds of cysts.
Minimally invasive procedures
There are several minimally invasive treatment options available that have shorter recovery times, such as:
Hysteroscopic removal of uterine polyps
Laparoscopic surgery of ovarian cysts
Selected procedures for uterine fibroids
These methods let your doctor treat the problem while preserving surrounding healthy tissue. As such, recovery is often straightforward, and most women may go back to their daily activities in a few days to a couple of weeks.
Surgery
Surgery, such as the removal of fibroids (myomectomy), may be recommended if:
The growth is large
Symptoms are significant
There is uncertainty about the diagnosis
Other treatments have not been effective
Even in these cases, your doctor will carefully go over all of your alternatives with you so you may choose the one that best meets your needs and goals.
What should you do if you suspect polyps, cysts, or fibroids?
If you are unsure about your symptoms or diagnosis, it can help to take a step-by-step approach:
Here’s a simple, practical way to help you decide what to do next:
Pay attention to persistent or unusual symptoms
Avoid self-diagnosing based on online information
Seek a medical evaluation when needed
Follow up regularly if monitoring is recommended
Taking these steps can help you feel more confident about what you’re experiencing and when to get help.
If you’ve been told you may have a polyp, cyst, or fibroid, request an appointment with Thomson Medical for a personalised assessment. Our doctors can help you understand your condition and decide whether monitoring or treatment is the right next step.
FAQ
Can polyps, cysts, and fibroids go away on their own?
It depends on the type of growth:
Polyps: These usually don’t go away on their own and may need to be monitored or removed.
Cysts: Many cysts, especially functional ovarian cysts, can resolve naturally over time without treatment.
Fibroids: Fibroids typically don’t disappear on their own, but they often shrink after menopause as hormone levels decline.
Do lifestyle changes help reduce the risk of developing polyps, cysts, and fibroids?
Maintaining a healthy weight, staying physically active, managing stress, and eating a balanced diet can help regulate hormone levels and overall health. While these steps may not completely prevent polyps, cysts, or fibroids, they can contribute to lowering the risk and supporting better long-term wellbeing.
Can polyps, cysts, or fibroids cause the same type of pelvic pain?
Yes, they can sometimes cause similar symptoms. Pelvic pain, pressure, or discomfort may feel alike across these conditions, which can make it difficult to tell them apart based on symptoms alone.
Do hormonal birth control methods affect polyps, cysts, and fibroids the same way?
Hormonal contraception may help regulate menstrual cycles, reduce bleeding, or prevent certain types of cysts. However, the effects can vary depending on the condition and the individual. Your doctor can help determine whether this option is suitable for you.
Can these conditions come back even after treatment?
Yes, polyps, cysts, or fibroids may return, especially if underlying factors such as hormones or genetics are still present. Regular follow-up can help detect any recurrence early and guide further management if needed.
Why don’t you always need to remove polyps, cysts, or fibroids immediately?
Not all growths require immediate treatment. Many are small, harmless, and do not cause symptoms. In these cases, monitoring may be a safe and appropriate approach.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and advice based on your unique situation, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
