After going through a myomectomy, it’s completely normal to feel both hopeful and anxious. You might be wondering whether it’s truly safe to start trying to conceive while also doing everything you can to set yourself up for a healthy pregnancy.
Myomectomy does affect fertility and pregnancy planning in some ways, but the good news is that most women who have the procedure go on to conceive and carry healthy pregnancies.
Understanding when to start trying, what risks to be aware of, and how your pregnancy will be monitored can help you move into the next chapter feeling more prepared.
What is a myomectomy?
A myomectomy is a surgery that removes uterine fibroids while preserving your uterus (womb). Many women choose it because they want relief from fibroid symptoms without giving up the option of a future pregnancy.
There are three main types:
Hysteroscopic myomectomy:
Fibroids are removed through the cervix, with no incision made in your uterine wall.
Laparoscopic or robotic myomectomy:
Laparoscopic myomectomy is a minimally invasive approach using small abdominal incisions.
Open myomectomy:
Your surgeon makes a larger abdominal incision, usually when there are multiple fibroids or fibroids that are too large to remove any other way.
The type of surgery you had determines how long your womb needs to heal, how scar tissue forms, and whether you'll need a planned caesarean delivery.
How long should you wait before trying to conceive?
It's natural to want to know how soon you can safely start trying after a myomectomy. The answer depends on the type of surgery you had.
Most doctors suggest waiting at least 3–6 months before trying to conceive, but the healing process isn't the same for everyone.
How long your uterus needs to fully recover depends on several factors, such as:
How deep the fibroids were
How much of the uterine wall was repaired
How well has your recovery progressed
Waiting can feel hard, especially when you're already feeling ready. But giving your body enough time to heal properly lowers the risk of complications during pregnancy.
Unsure whether your womb has healed fully enough to try conceiving?Request a consultation with our gynaecologists at Thomson Medical to review your surgical details and receive personalised advice.
Chances of getting pregnant after myomectomy
It's understandable to worry that surgery may have affected your fertility. But many women who actively try to conceive after a myomectomy are able to become pregnant, especially when fibroids were the main factor affecting fertility before surgery.
Some women conceive naturally. Others go through assisted reproductive techniques. Both paths remain possible after surgery.
If fibroids were distorting your uterine cavity (space within your uterus) before the procedure, removing them often improves your chances by restoring a healthier environment for implantation.
In some cases, scar tissue can develop after surgery and may affect fertility. However, this isn't common. If you're having difficulty conceiving, your doctor can check for scar tissue using a procedure called hysteroscopy, which allows them to look inside your uterus and remove any adhesions if needed.
Risks during pregnancy after myomectomy
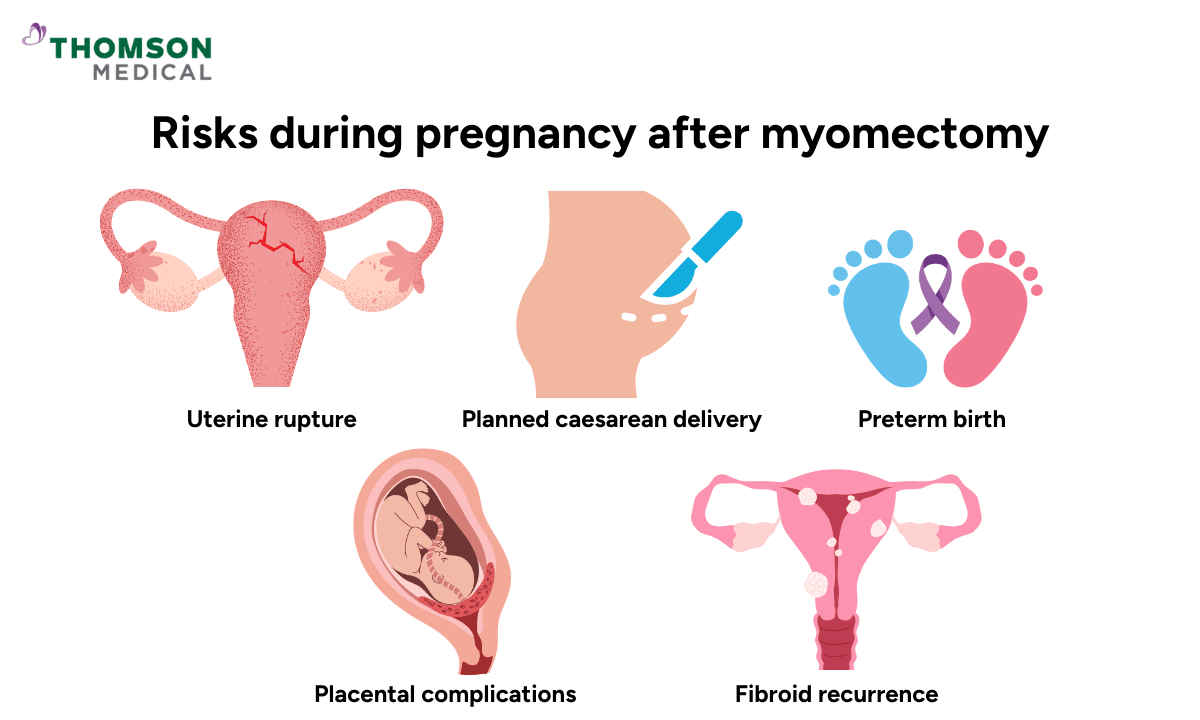
Most pregnancies after myomectomy go well. That said, because your uterus has been surgically repaired, your doctor will monitor you more closely.
Here are the main things your gynaecologist will be watching for:
Uterine rupture:
Because the uterine wall was previously cut and repaired, there's a small risk of rupture, most often in late pregnancy or during labour.
Planned caesarean delivery:
Many women who've had a myomectomy are advised to have a C-section to avoid putting too much pressure on the repaired uterine wall.
Preterm birth:
Scarring in the uterine muscle can affect how your womb stretches and contracts as your pregnancy progresses, which slightly raises the risk of early delivery.
Placental complications:
Conditions like placenta praevia (where the placenta sits low and covers partially or completely the cervix) or abnormal placental attachment may be slightly more likely, since scar tissue can influence where the placenta settles.
Fibroid recurrence:
The hormonal changes of pregnancy may encourage fibroid growth but most are monitored throughout the pregnancy.
The risks sound serious, but with close monitoring, they are manageable. Your gynaecologist will create a monitoring and delivery plan specific to your surgical history. When you start trying to conceive, or as soon as you find out you're pregnant, your doctor will go through your surgical details and put together a plan tailored to you.
Our gynaecologists
Loading...
Tips for a healthy pregnancy after myomectomy
There are some practical steps you can take – both before you start trying and during pregnancy – to give yourself and your baby the best possible start.
Before you try to conceive
Before you actively start trying, it's worth making sure your body is truly ready.
A few things that may help include:
Check that healing is complete:
Schedule an appointment with your doctor to confirm your uterus has fully healed. Depending on your situation, this might involve reviewing your surgical report or having an ultrasound to look at the uterine wall.
Optimise your overall health:
Reaching a healthy weight, starting prenatal vitamins with folic acid, stopping smoking, and cutting back on alcohol all help lay the groundwork for implantation and early pregnancy.
Consider a fertility assessment if needed:
If you're over 35 or have been trying for 6–12 months without success, a fertility evaluation can give you clearer answers and help you get timely support.
Taking these steps before you conceive means you can go into pregnancy feeling informed and physically ready.
During pregnancy
Once you're pregnant, the focus moves from preparation to steady monitoring of how things are progressing.
It’s helpful to:
Start prenatal care early:
As soon as you get a positive pregnancy test, schedule an appointment to confirm where the pregnancy has been implanted and set a baseline for monitoring.
Monitor the uterine scar and placenta:
Your doctor will likely recommend regular ultrasounds to check the thickness of the uterine scar, the position of the placenta, and how your baby is growing – all of which feed into safe delivery planning.
Discuss delivery planning early:
While some new mothers wait till the third trimester, it is usually better to discuss whether a vaginal birth or planned caesarean is right for you during your second trimester.
Pay attention to abnormal symptoms:
Severe abdominal pain, unusual bleeding, or a sudden change in your baby's movements are all worth getting checked promptly.
Keep up the general good habits:
Balanced nutrition, steady weight gain, regular movement, enough sleep, and managing stress all support both uterine health and your baby's growth throughout pregnancy.
With careful monitoring and early planning, most women who've had a myomectomy move through pregnancy safely and deliver healthy babies.
If you would like personalised guidance on pregnancy after myomectomy, schedule a consultation with Thomson Medical. Our doctors can assess whether your womb is ready for pregnancy and create a tailored monitoring plan to support a safe and healthy journey ahead.
FAQ
Can you get pregnant naturally after a myomectomy?
Yes, many women conceive naturally after their womb has fully healed, especially if fibroids were the primary factor affecting fertility before surgery.
Does age affect fertility outcomes after myomectomy?
There isn’t a single best age. Fertility outcomes are influenced more by your age and ovarian reserve than by the surgery itself. In general, younger women tend to have higher natural fertility regardless of prior myomectomy.
Does myomectomy improve fertility?
It often does, especially if fibroids were distorting the uterine cavity or interfering with implantation. However, while surgery can remove a structural barrier, it cannot guarantee pregnancy.
Will I need a C-section if I had a myomectomy?
In many cases, a planned caesarean delivery is recommended, especially if the uterine wall was deeply incised during surgery. The final decision depends on your surgical details and your doctor’s assessment during pregnancy.
How is pregnancy monitored after myomectomy surgery?
In most cases, you will receive standard prenatal care, with a few additional checks tailored to your surgical history. Your doctor may:
Recommend periodic ultrasounds
Monitor fetal growth
Assess placental position
What are the risks of pregnancy after myomectomy?
Most pregnancies progress well, but there are some increased risks to be aware of. These include:
Uterine rupture
Planned cesarean delivery
Preterm birth
Placental positioning issues
With appropriate monitoring and planning, these risks are usually well managed.
The information is intended for general guidance only and should not be considered medical advice. For personalised recommendations and advice based on your unique situation, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
