Hearing medical terms like "polyps" and "pseudopolyps" after a scan or procedure can feel a little confusing. If your doctor has mentioned either of these, it is completely natural to want to understand exactly what they mean for your body.
Knowing the difference between the two can help you feel more informed about what your doctor has found.
What are polyps?
A polyp is an abnormal growth of tissue that develops from the lining of an organ. They can develop in different parts of your body, including the colon and rectum, the stomach, the uterus, the cervix, the nose, and the throat.
Polyps are true tissue growths caused by an overgrowth of cells. Some polyps are harmless, but others can develop into cancer over time.
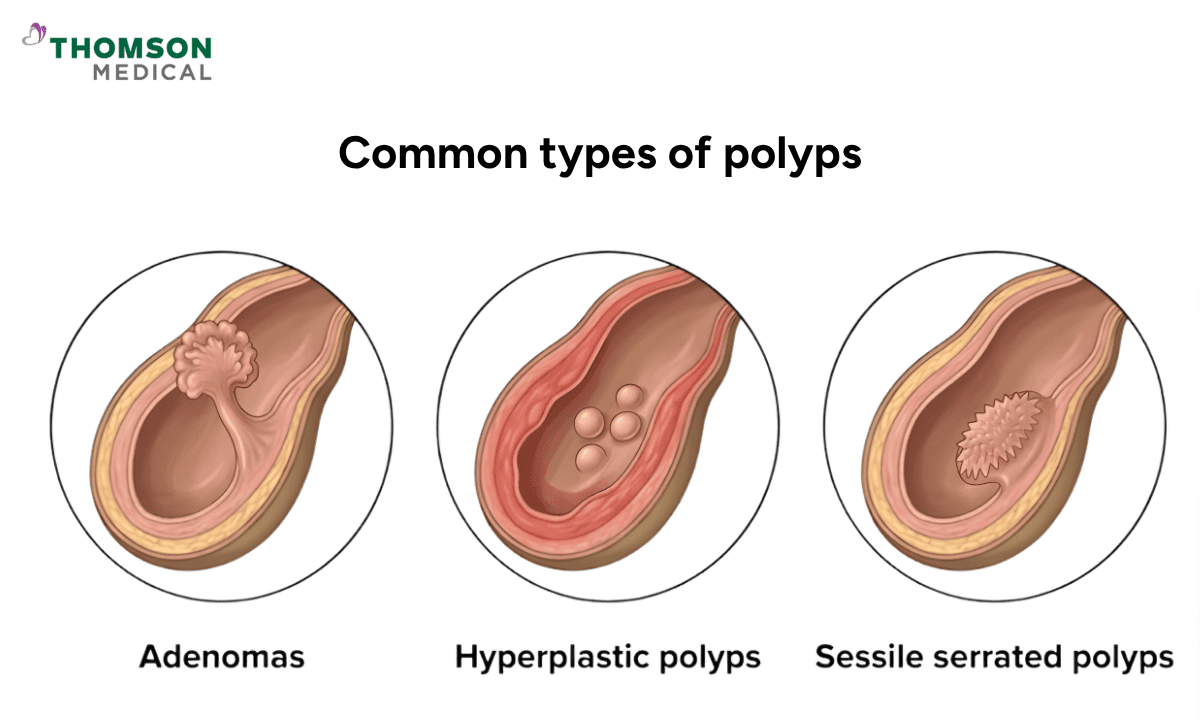
Common types include:
Adenomas, which are precancerous and may turn into cancer if left untreated
Hyperplastic polyps, which are usually harmless, though larger ones may require removal
Sessile serrated polyps, which are precancerous and need monitoring
Understanding the specific type of polyp you have helps your doctor tailor the suitable care plan for you.
What are pseudopolyps?
Pseudopolyps, sometimes called "false polyps", are not true growths. Instead, they are areas of regenerating or inflamed tissue that form after repeated injury to your intestinal lining.
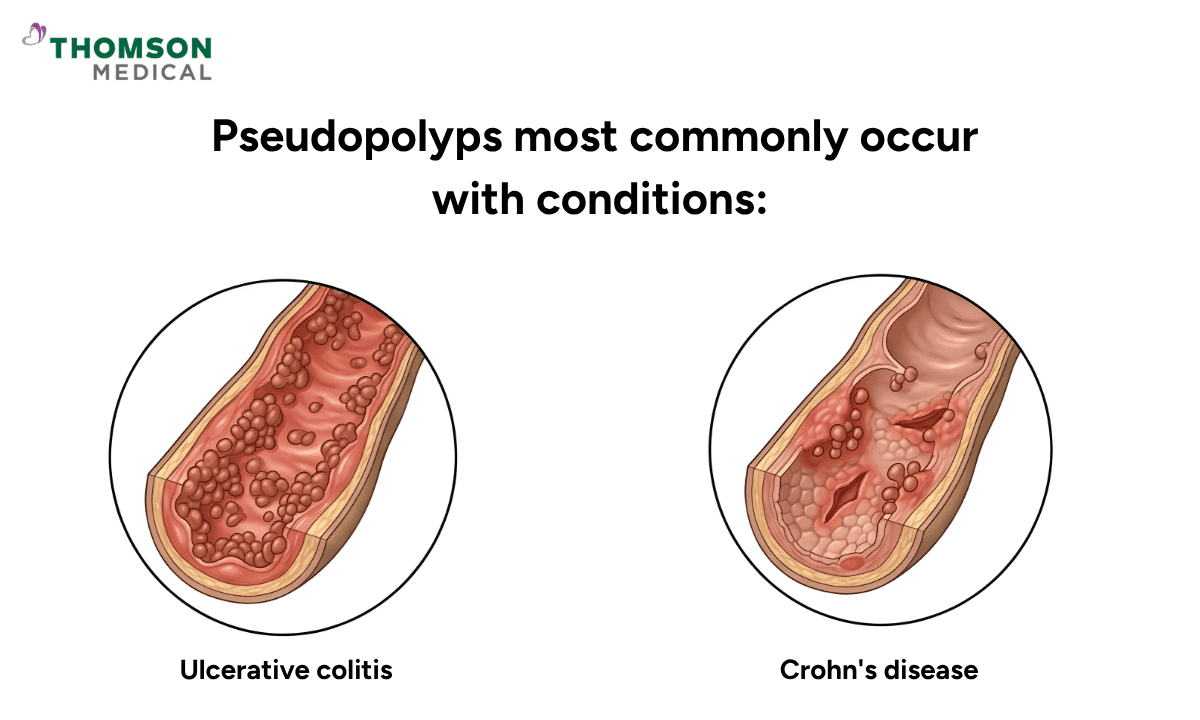
They most commonly occur in people managing conditions like:
Ulcerative colitis, a long-term condition where the lining of your large intestine becomes inflamed and develops ulcers
Crohn's disease (inflammatory bowel disease or IBD), a chronic inflammatory condition that can affect any part of your digestive tract
When your intestines are healing between episodes of inflammation, these pseudopolyps can form. They’re not caused by abnormal growth, but by your body repairing and rebuilding the lining of your gut.
Understanding this can be reassuring. These changes are simply a sign that your body is working hard to heal itself.
Pseudopolyps vs polyps: key differences
While they may sound similar, pseudopolyps and polyps are actually quite different. They vary in how they form, what they mean for your health, and how they are managed, so it’s important to understand the distinction between the two.
Causes
True polyps develop when cells grow more than they should. This can happen due to genetic changes, ageing, lifestyle factors, and sometimes hormonal influences, such as those affecting your uterus.
Pseudopolyps, on the other hand, form as a response to ongoing inflammation. When the lining of the intestine is repeatedly damaged and healed, these growths can appear. They are most commonly linked to IBD.
Appearance
True polyps can appear either flat (sessile) or grow on a small stalk (pedunculated). They are usually smooth, uniform in shape, and have clearly defined borders.
Pseudopolyps tend to look quite different. They are often irregular and jagged and usually appear in clusters rather than on their own. Because they form in areas of ongoing inflammation, they are surrounded by damaged tissue and may look like small “islands” of tissue between ulcers.
Underlying conditions
True polyps can develop even in otherwise healthy individuals. They tend to become more common with age and may occur randomly or be linked to inherited conditions.
Pseudopolyps, in contrast, are closely associated with chronic inflammatory conditions of your bowel. They are most often seen in people with ulcerative colitis or Crohn’s colitis and are very rare outside of these conditions.
Cancer risk
With true polyps, some types, such as adenomas and sessile serrated lesions, can be precancerous. The risk of cancer increases as they grow larger or if there are signs of dysplasia.
Pseudopolyps themselves are not precancerous. However, IBD can increase your overall risk of colon cancer over time. In other words, the risk comes from long-term inflammation, not the pseudopolyp itself.
Staying proactive with regular check-ups and screenings could be effective to manage these risks and protect your health.
Summary of key differences
Here’s a table on their key differences:
Feature | True polyp | Pseudopolyp |
Nature | Abnormal growth | Inflammatory or regenerative tissue |
Cause | Cell overgrowth | Chronic inflammation |
Cancer risk | Some types are precancerous | Not precancerous |
Linked to IBD | Not necessarily | Strongly linked |
Removal needed | Usually yes | Usually not |
True polyps and pseudopolyps have very different implications, and your doctor will guide you on the appropriate care based on your individual situation.
If you have been diagnosed with polyps or pseudopolyps and would like clarity on what it means for your health, it is helpful to speak with a doctor. You may arrange a consultation with Thomson Medical to discuss your diagnosis and appropriate next steps.
How doctors identify each type
Both types are usually found during a routine colonoscopy. To tell them apart, your doctor will first look closely at the area during the procedure and then take a small tissue sample (biopsy) for further testing.
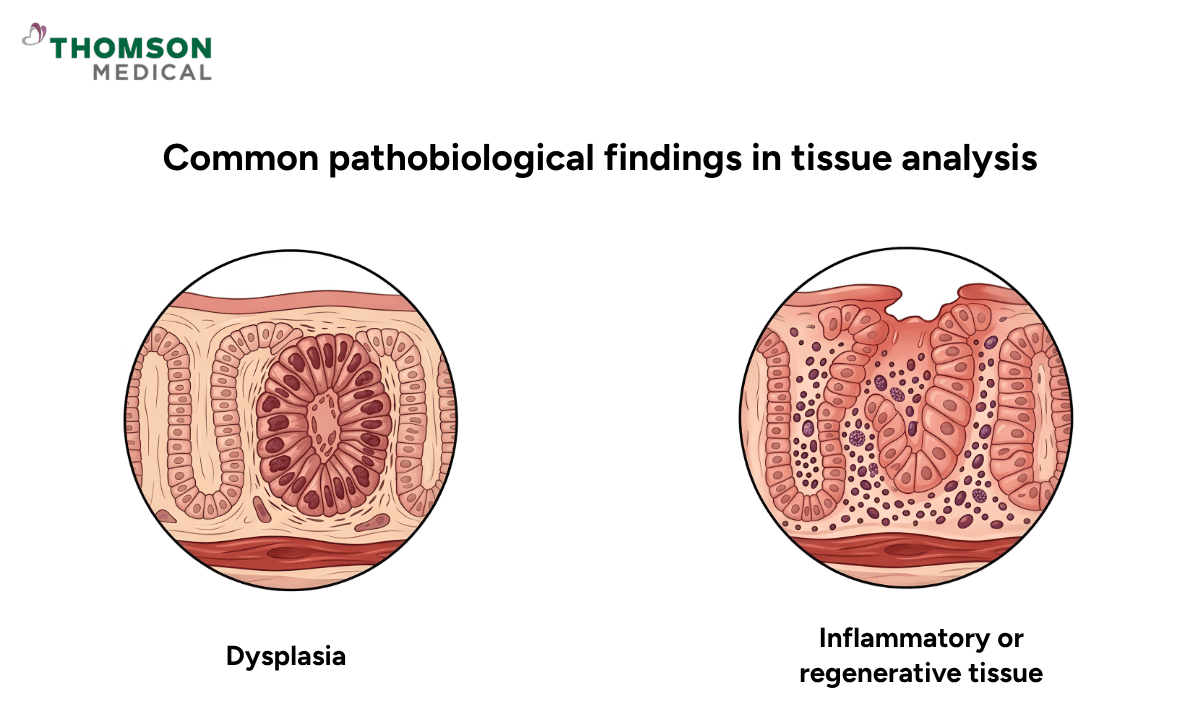
A pathologist will look closely at the tissue to see if it shows:
Dysplasia, which indicates precancerous changes and points to a true polyp
Inflammatory or regenerative tissue, which points to a pseudopolyp
Our specialist
Loading...
Treatment approaches
The way your doctor manages this depends on what the test results show.
For true polyps, treatment is usually more direct. They are often removed during a colonoscopy in a procedure called a polypectomy. In some cases, if a polyp is larger or looks more concerning, surgery may be needed, followed by regular check-ups to monitor your health.
For pseudopolyps, the approach is usually more conservative:
They often do not need to be removed.
Treatment is only considered if they cause symptoms like bleeding, become very large, lead to a rare blockage, or if there is any uncertainty about the diagnosis.
The main focus is on managing IBD with medications such as biologics or immunosuppressants.
Your care team will always guide you toward the gentlest and most effective option for your specific situation.
If you have been diagnosed with pseudopolyps or have ongoing inflammatory bowel symptoms, it is helpful to seek medical advice for proper monitoring. You may arrange a consultation with Thomson Medical to discuss your condition and long-term management.
FAQ
Can pseudopolyps turn into cancer?
No. Pseudopolyps themselves are not precancerous. However, people with long-standing ulcerative colitis or Crohn's disease do have an increased colon cancer risk due to the chronic inflammation.
Do pseudopolyps need to be removed?
Not usually. Most are safely left alone. Removal may only be considered if they bleed, are particularly large, cause concern about dysplasia, or interfere with your regular colonoscopy surveillance.
Can I have both at the same time?
Yes. A person with inflammatory bowel disease can certainly have pseudopolyps from inflammation alongside true adenomatous polyps or dysplasia-related lesions. This is exactly why biopsies and careful surveillance are so essential.
Do pseudopolyps cause pain?
Pseudopolyps themselves do not usually cause pain. Any pain you experience typically comes from active inflammation, ulceration, or IBD flare-ups.
Can diet affect pseudopolyp formation?
Diet does not directly cause pseudopolyps. However, poorly controlled inflammation increases their formation. Enjoying a balanced, anti-inflammatory diet may help support your overall IBD management, though medical therapy remains the main treatment for preventing new ones from forming.
What is the recovery like after pseudopolyp removal?
If one is removed during a colonoscopy, it is usually a simple outpatient procedure. You might experience mild bloating or cramping for 1 to 2 days, with a very rare risk of bleeding or perforation.
Most people comfortably resume their normal activities within 24 hours. Your overall recovery depends much more on your underlying IBD activity than the removal itself.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Medical Concierge
- 8.30am - 5.30pm
- WhatsApp: 9147 2051
Need help finding the right specialist or booking for a group?
Our Medical Concierge is here to help you. Simply fill in our form, and we'll check and connect you with the right specialist promptly.
Notice:
The range of services may vary between Thomson clinic locations. Please contact your preferred branch directly to enquire about the current availability.
Get In Touch