You've just been through major surgery, and now you're home, exhausted, staring at your bed and wondering how on earth you're going to get through the night comfortably. Maybe you're a natural side sleeper, or you usually curl up, and now those positions feel off-limits.
A few small adjustments to how you sleep can make a real difference to your comfort and recovery. Knowing which sleeping positions work best after a hysterectomy, and which ones to avoid, can help you wake up feeling a little more rested each day.
What to expect when sleeping after a hysterectomy
Sleep after a hysterectomy often feels harder than expected. Your body has just been through major surgery, and while rest is essential for healing, getting there can take some adjustment.
Many women find sleep is disrupted in the first few weeks. Knowing why can make it easier to manage.
Why sleep feels different after surgery
Several factors tend to overlap in the early weeks, each making restful sleep a little harder to come by:
Physical discomfort:
You may feel soreness or pressure in your lower abdomen, and even shifting positions in the night can be uncomfortable.
Pain medication and anaesthesia:
These can throw off your sleep cycle, leaving you drowsy during the day and restless at night.
Hormonal shifts:
If your ovaries were removed, a sudden drop in oestrogen can trigger night sweats and make it harder to stay asleep.
Emotional recovery:
Anxiety and low mood are common after a hysterectomy, and both can make winding down at night more difficult.
These are simply your body responding to a significant change. For many women, these disruptions ease gradually as the body heals, though the timeline looks different for everyone.
How long recovery takes before sleep improves
Every woman's recovery is different, but knowing a general idea of what to expect can help you understand whether you're progressing normally.
How sleep often evolves across the recovery stages:
In the first one to two weeks, discomfort is usually at its peak. Sleep may be broken, and you may need to wake up to take pain medication or reposition yourself. This is normal.
By weeks three to four, most women notice a gradual improvement. The soreness begins to ease, and longer stretches of sleep become more achievable.
By six to eight weeks, many women are sleeping much more comfortably, though this can vary depending on the type of hysterectomy you had and whether your ovaries were removed.
If hormonal changes such as night sweats or hot flushes are disrupting your sleep, these may take a little longer to settle. Your doctor can discuss options to help manage these symptoms.
A few things that can slow sleep recovery include:
Overdoing activity during the day
Poorly managed pain
Unaddressed emotional stress or anxiety
Be patient with yourself. Healing is rarely linear, and a difficult night does not mean you are not progressing.
Best sleeping position after hysterectomy
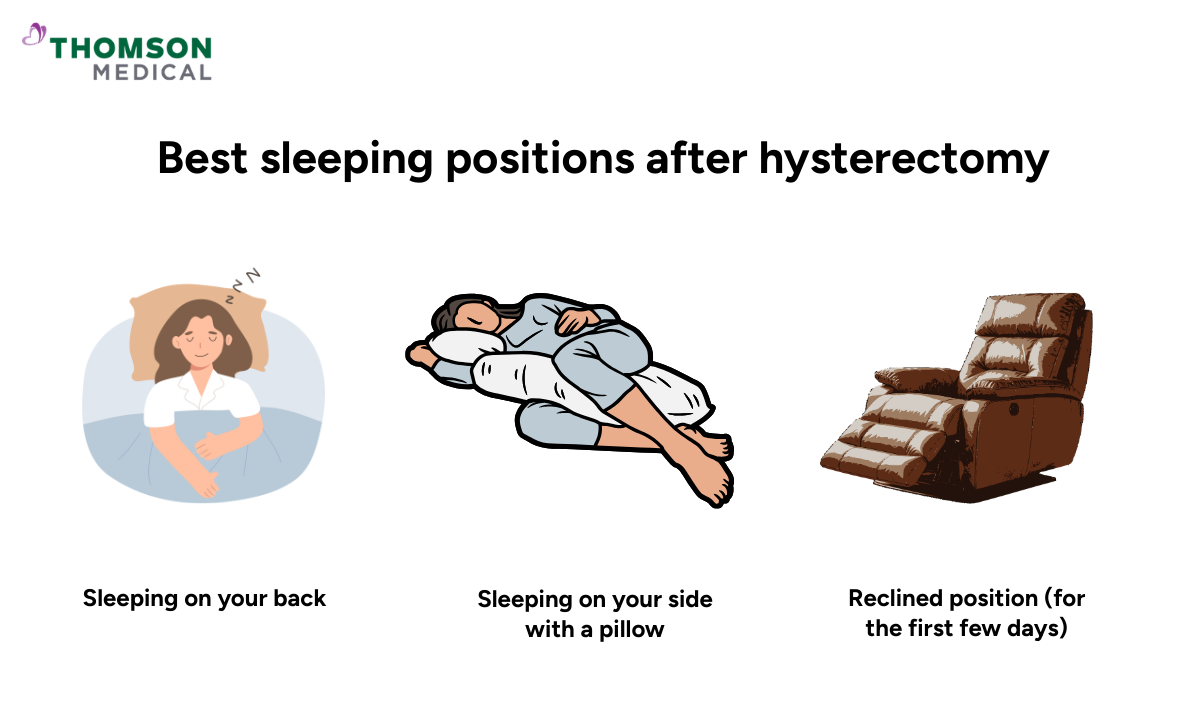
Finding a comfortable position is probably one of the biggest challenges in the first weeks of recovery. The right position can reduce pressure on your abdomen, protect your incision site, and help you get the rest your body needs to heal.
Sleeping on your back
Sleeping on your back is generally the most recommended position after a hysterectomy. It distributes your body weight evenly and keeps pressure off your abdominal muscles and incision site.
To make this position more comfortable:
Place a pillow under your knees to reduce strain on your lower back
Keep a pillow nearby to press gently against your abdomen if you need to cough or sneeze
Make sure your mattress offers enough support. A surface that is too soft may cause your lower back to sink and add discomfort.
Some women find sleeping flat on their back difficult at first. If that is the case, a slightly reclined position using extra pillows can help ease the pressure while still protecting the surgical area.
Sleeping on your side with a pillow
Side sleeping can be a comfortable option once the initial soreness begins to ease, usually after the first week or two. Many women find sleeping on their side more natural, especially if it was their preferred position before surgery.
To do this safely:
Place a pillow between your knees to keep your hips aligned and reduce strain on your pelvis
Hug a pillow gently against your abdomen for extra support and to cushion any sudden movements
Alternate sides if you can, to avoid stiffness from staying in one position too long
If one side feels more comfortable than the other, it is perfectly fine to favour it. Your body will naturally guide you toward what feels right.
Reclined position (for the first few days)
In the very early days after surgery, lying completely flat may feel uncomfortable. A reclined position where your upper body is slightly elevated can feel much more manageable.
You can achieve this by:
Propping yourself up with two to three pillows behind your back and head
Using a wedge pillow if you have one, as it provides more stable and even support
Reclining in an adjustable chair if getting in and out of bed is too difficult at first
This position can also help reduce postoperative bloating and ease any pressure on your incision site. As your recovery progresses, you can gradually lower the incline as comfort allows.
If you're unsure whether your sleep disruption is a normal part of recovery or something that needs attention, schedule an appointment with Thomson Medical. Our doctors can assess your symptoms and recommend a suitable approach for your recovery.
Sleeping positions to avoid after hysterectomy

Just as important as finding a comfortable position is knowing which ones to avoid. Certain positions can strain your abdominal muscles, put pressure on your incision site, or slow your recovery.
Sleeping on your stomach:
This is the main one to avoid, particularly in the first six to eight weeks. It places direct pressure on your abdomen and surgical site, which can cause pain and affect healing.
Twisting or sleeping at an angle where your upper and lower body face different directions:
This position can strain your abdominal muscles and pelvic floor. Keep your body as aligned as possible.
Curling tightly into a foetal position:
While side sleeping is generally fine, drawing your knees too close to your chest compresses the abdominal area and can aggravate discomfort.
If you are unsure what is safe for your specific situation, your surgeon or care team can give you personalised guidance based on your type of hysterectomy.
Gynaecologists at Thomson Medical
Loading...
Tips to sleep better during hysterectomy recovery
Recovery is tiring, but poor sleep can make it feel even harder. A few simple adjustments to your routine and sleep environment can make a real difference in how rested you feel each day.
Managing pain and discomfort at night
Pain might be one of the most common reasons sleep is disrupted after a hysterectomy. It’s recommended to manage it proactively rather than waiting until you are already uncomfortable.
A few steps that can help:
Take pain relief at the right time:
If your doctor has prescribed medication, take it before bed so it is working when you need it most. Do not wait until the pain wakes you up.
Use a pillow as a buffer:
Keeping a pillow pressed gently against your abdomen can ease discomfort when you cough, sneeze, or shift positions in the night.
Note what wakes you:
If you find yourself waking at a similar time each night, it may be a sign that your pain medication is wearing off.
Mentioning this to your doctor can help, as your dosage or timing may need adjusting.
If you're waking in discomfort, making small, careful adjustments is better for your recovery than staying still all night.
Pillows, mattress, and sleep setup
The right sleep environment can support your body and reduce unnecessary strain. You do not need to invest in anything expensive. Small changes go a long way.
Pillows are your best tool during recovery – stock up before your surgery so you are prepared. Your mattress matters too. A surface that is too soft can cause your lower back to sink, adding discomfort. If your mattress is very soft, placing a thin, firm topper underneath can help.
Keep essentials within easy reach. Water, medication, your phone, and anything else you might need overnight should be on your bedside table. Reducing the need to get up unnecessarily helps protect your rest and your recovery.
When to ask your doctor about sleep issues
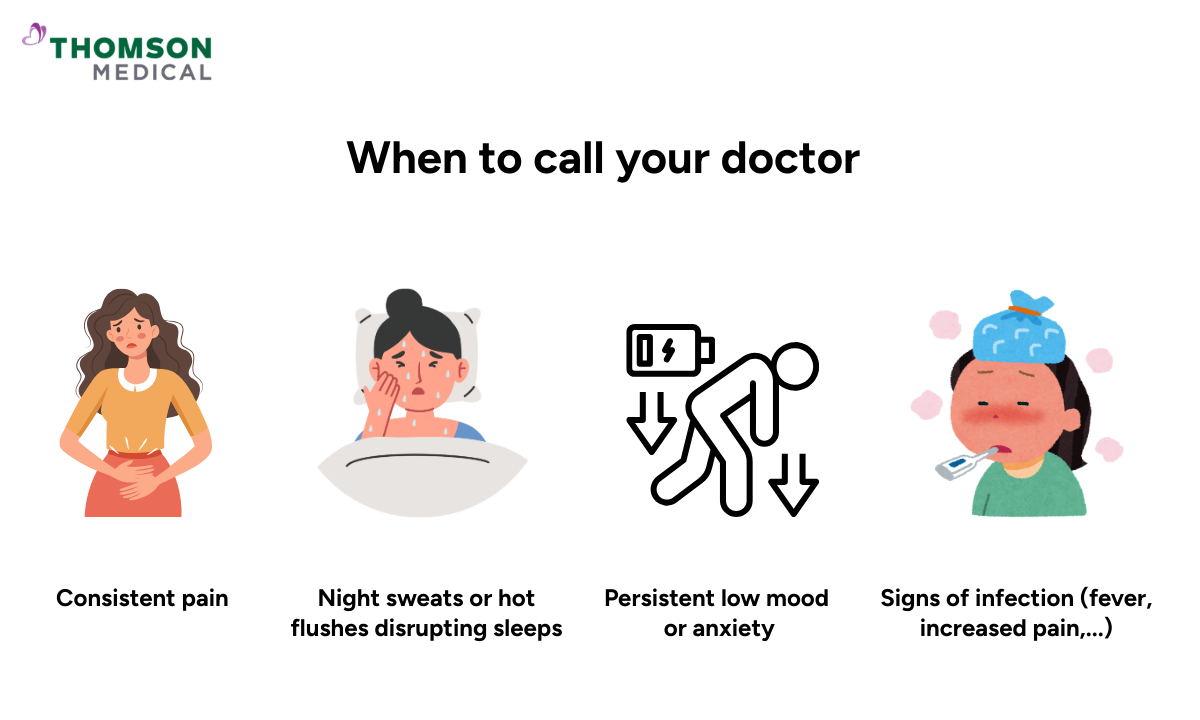
While some sleep disruption is expected after a hysterectomy, speak with your doctor if you notice:
Pain that consistently wakes you and is not improving over time
Night sweats or hot flushes that are severely disrupting your sleep
Persistent low mood or anxiety affecting your ability to rest
Signs of infection such as fever or increased pain around the incision site
Sleep that shows no improvement after four to six weeks
These symptoms do not always mean something serious, but checking in early means any underlying issues can be caught and addressed before they affect your wider recovery. You know your body best – if something feels off, your care team is there to help.
If pain or discomfort is still keeping you up despite your best efforts, schedule an appointment with Thomson Medical. Our doctors can review your pain management and help you get the rest you need to recover.
FAQ
What is the best sleeping position after a hysterectomy?
Sleeping on your back with a pillow under your knees is considered the most comfortable and supportive position during recovery. It reduces pressure on your abdomen and incision site.
Can I sleep on my side after a hysterectomy?
Yes, but usually after the first week or two when initial soreness begins to ease. Place a pillow between your knees and hug one against your abdomen for support.
How do I get out of bed without straining after surgery?
Roll onto your side first, then use your arms to push yourself up slowly. Avoid using your abdominal muscles to sit up directly, as this puts unnecessary strain on your incision site.
Is it normal to feel more tired than usual after a hysterectomy?
Completely normal. Your body is directing significant energy towards healing. Fatigue in the first few weeks is expected. Rest as much as you need to.
Can I sleep with a heating pad after a hysterectomy?
Speak with your doctor before using a heating pad. Heat can help ease discomfort, but it should not be applied directly to the incision site or used while you are asleep.
How many weeks after a hysterectomy can I return to normal sleeping positions?
Many women return to their usual sleeping positions between six and eight weeks post-surgery. Recovery varies depending on the type of hysterectomy, so follow your surgeon's guidance.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations based on your medical conditions, request an appointment with Thomson Medical.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) - Jurong:
6262 8588 (Call), 6262 8588 (WA) - Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
Notice
The range of services may vary between TWC/TS locations. Please contact your preferred branch directly to enquire about the current availability.
Request an Appointment