Hearing medical terms after a scan can feel overwhelming. If your doctor mentioned a sessile polyp during your check-up, it is completely normal to wonder what that means for your body and your health.
Taking a moment to understand what is happening inside your digestive system can help you feel more at ease and in control.
What is a sessile polyp?
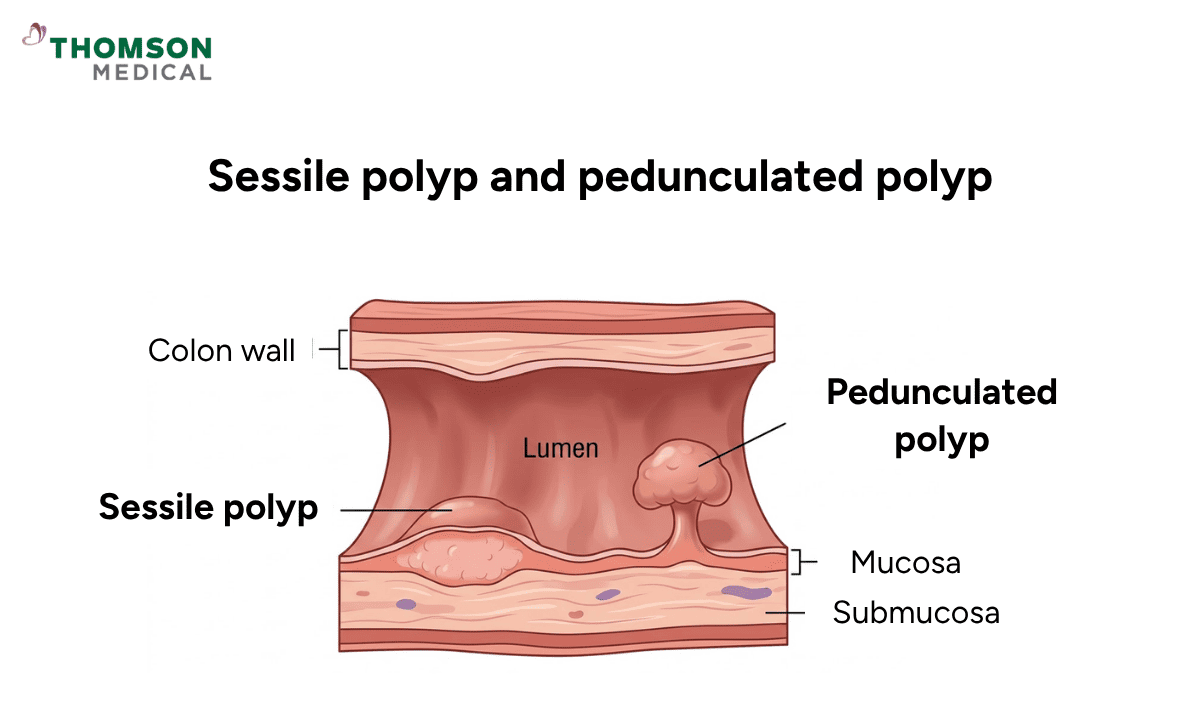
A sessile polyp is a flat or slightly dome-shaped growth of abnormal tissue that sits directly on the tissue lining of an organ, without a stalk. Unlike pedunculated polyps, which look like small mushrooms with a stem, these have a broad base and only rise a little above the surface.
Because of their flat shape, they can be harder to detect during routine screening tests. They are most often found in the large intestine, where they are referred to as colon polyps or colorectal polyps. Depending on the type, some sessile polyps may carry a higher cancer risk.
What are the causes and risk factors?
These flat growths form when cells start to change in abnormal ways. This can happen because of genetic mutations, long-term inflammation, or simple DNA copying errors that build up over time. Certain molecular features can also contribute to their development.
Your risk increases as you get older, especially after 40 to 50 years old.
Other factors that can raise your chances include:
A family history of polyps or colorectal cancer
Having a higher body weight or not getting much physical activity
Smoking
Eating a diet high in red and processed meats
Not getting enough fibre-rich foods, such as wholegrains, fruits, and vegetables
Having type 2 diabetes
Living with inflammatory bowel disease (IBD), such as Crohn’s disease or ulcerative colitis
Having inherited conditions like Lynch syndrome
Some types, such as sessile serrated polyps (also called sessile serrated adenomas or sessile serrated lesions), are more strongly linked to a higher risk of developing colorectal (bowel) cancer. These are flat polyps with a sawtooth pattern under the microscope that can be harder to detect.
If you have risk factors for colorectal polyps or concerns about your bowel health, it is advisable to seek medical advice for appropriate screening. You may arrange a consultation with Thomson Medical to discuss your risk and preventive care options.
What are the symptoms of sessile polyps?
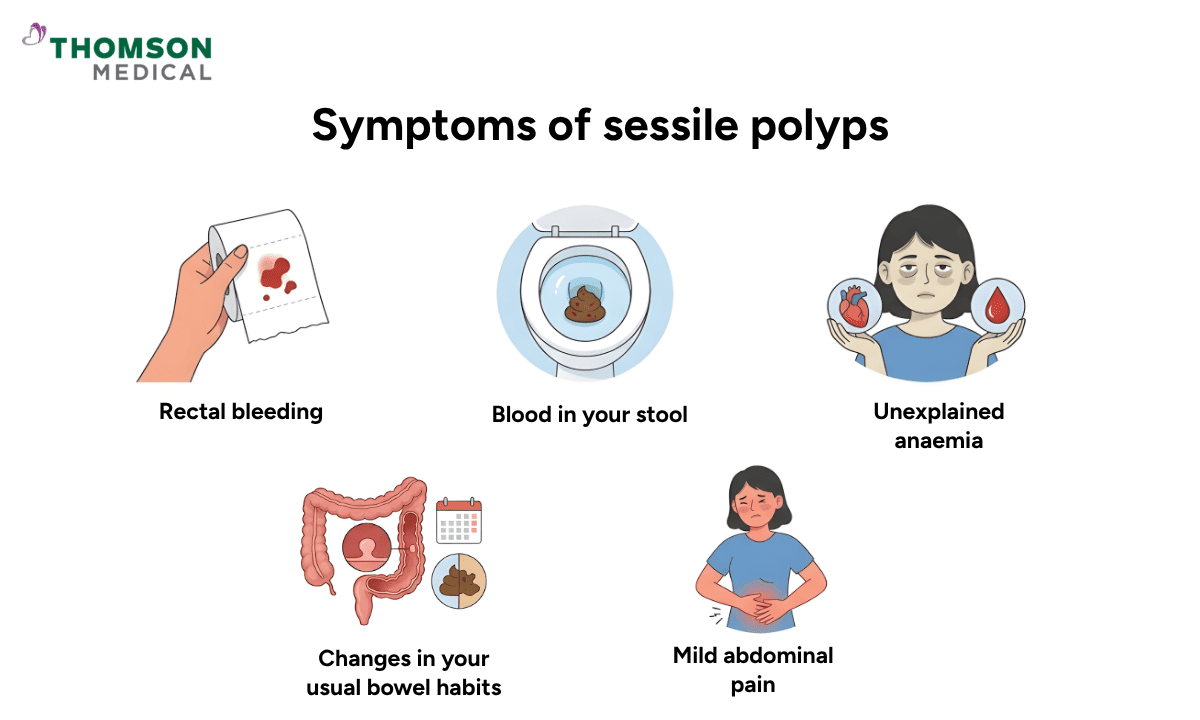
Most of the time, these flat growths do not cause any symptoms, especially when they are small.
If symptoms do appear, they may include:
Blood in your stool or rectal bleeding, which may look bright red or dark and tarry
Unexplained anaemia, which can leave you feeling tired all the time
Changes in your usual bowel habits, such as diarrhoea, constipation, or stools that are narrower than usual.
Mild abdominal pain, though this is rare and usually only happens when the growth is larger
Because symptoms are often subtle or absent, it can be easy to overlook early signs. Paying attention to changes in your body and seeking medical advice when something feels off can help ensure nothing important is missed.
How do doctors diagnose sessile polyps?
Your doctor has a few well-established ways to check your digestive system.
Common diagnosis methods include:
Colonoscopy:
This is the most widely used method for colorectal cancer screening.
Your doctor uses a small camera to examine the inside of your colon. Because sessile polyps are flat, they may use enhanced techniques like narrow-band imaging to spot subtle changes in the lining.
Biopsy:
During the procedure, your doctor can safely remove a small sample of tissue.
This sample is then sent to a lab to identify the exact type and assess any potential risks.
Other diagnostic tests:
CT colonography uses detailed X-ray imaging to detect polyps by shape and size.
Stool-based tests such as the faecal immunochemical test (FIT) check for traces of blood in your stool.
Both are less reliable for detecting flat sessile polyps, and your doctor may still recommend a colonoscopy if results are abnormal.
Each of these methods gives your doctor different information, working together to build a clear and accurate understanding of what is happening and how to move forward.
Our specialist
Loading...
What are the treatment options for sessile polyps?
Your care team will guide you toward the right treatment plan based on your unique situation.
Polypectomy (removal during colonoscopy)
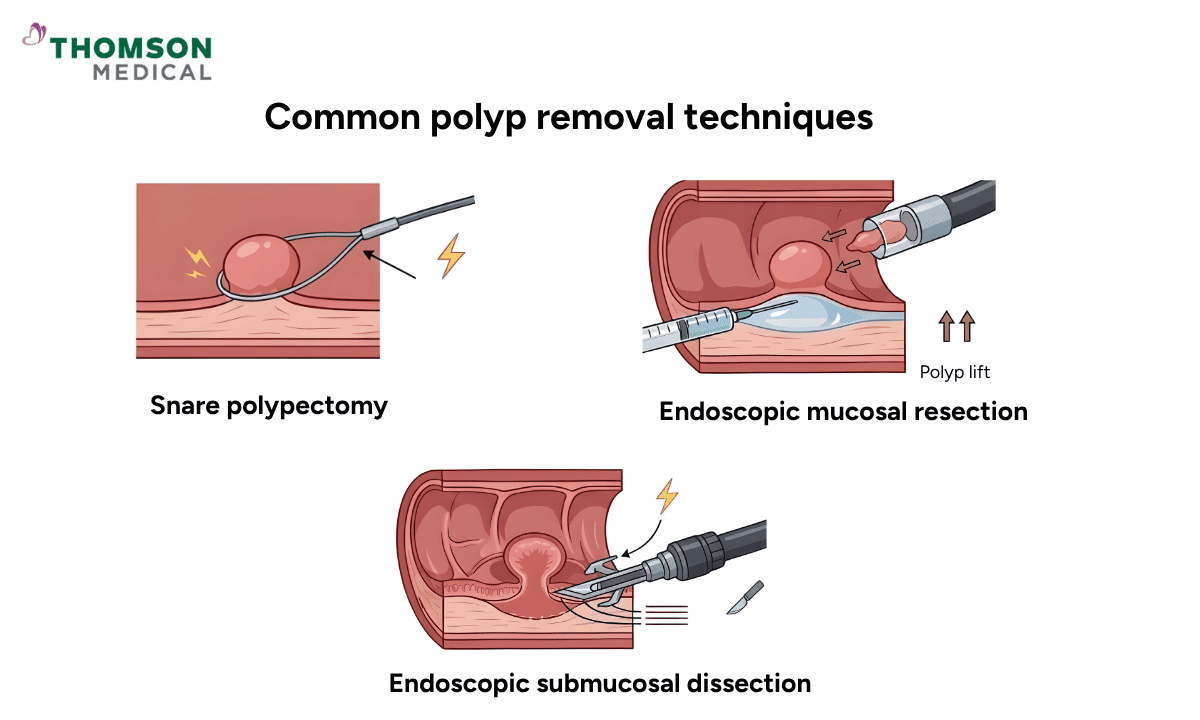
Most sessile polyps can be removed during a colonoscopy using specialised polypectomy techniques, such as:
Snare polypectomy, where a thin wire loop is placed around the polyp and tightened to remove it. For larger polyps, your doctor may remove it in sections using a technique called piecemeal resection.
Endoscopic mucosal resection (EMR), which involves lifting the polyp with a fluid injection before removing it, making it suitable for larger or flatter lesions
Endoscopic submucosal dissection (ESD), which is an advanced method where the polyp is carefully cut out in one piece from deeper tissue layers, often used for larger or more complex cases
Because sessile polyps do not have a stalk, they can be more difficult to remove than raised ones. However, they are routinely treated using safe, well-established techniques by trained doctors.
Not all sessile polyps need to be removed straight away. If a polyp is small and considered low risk, your doctor may recommend a watchful waiting approach, where you have regular follow-up colonoscopies to monitor any changes over time. Your care team will discuss the appropriate plan for your specific situation.
Can sessile polyps be prevented?
While they cannot be prevented completely, there are simple steps you can take to lower your risk and support your overall health.
Practical steps you can take include:
Attend regular screenings, starting from age 45, or earlier if you have a higher risk
Eat a high-fibre diet with plenty of vegetables and whole grains
Limit red and processed meats
Maintain a healthy weight and stay physically active
Avoid smoking and limit alcohol intake
Work with your doctor to manage any chronic inflammatory conditions
Regular check-ups are especially important, as finding and removing benign polyps early can prevent them from progressing further.
If you are concerned about your risk of sessile polyps or when to start screening, it is helpful to speak with a doctor. You may arrange a consultation with Thomson Medical to discuss personalised prevention and screening plans.
FAQ
How long does it take for a flat growth to become cancerous?
It usually takes 5 to 10 years, or longer, for precancerous polyps to develop into cancer. Some types, such as serrated or sessile serrated growths, may follow a slightly different pathway, but they still tend to change gradually over years rather than months.
Are sessile polyps considered precancerous?
Not all sessile polyps are precancerous. Some types, such as adenomatous polyps and traditional serrated adenomas, do carry a risk of becoming cancer over time. Others, like hyperplastic polyps and certain hamartomatous polyps, are usually benign. A pathology report is the most accurate way to understand the specific risk in your case.
Are sessile polyps difficult to remove?
They can be slightly more challenging to remove than raised polyps because they are flat, have a wider base, and may blend into the surrounding tissue. Even so, most can be removed safely during a routine procedure by an experienced specialist.
What happens if a removed growth is cancerous?
If cancer is found, your doctor will assess how deep it has grown and whether it has been fully removed. If it is caught early and confined to the surface, careful monitoring may be all that is needed.
If it has spread deeper, your doctor may first explore further endoscopic options or refer you to an oncologist before surgery to remove part of the colon is considered. Early detection gives your doctor more options for treatment and management.
What size of sessile polyps is most concerning?
In general, the larger the polyp, the higher the risk. Growths under 5 millimetres carry very low risk, those between 6 and 9 millimetres have a low but present risk, and those 10 millimetres or larger are more concerning. Polyps over 20 millimetres have a significantly higher risk, although size alone does not determine whether cancer is present.
Are sessile polyps fast-growing?
Most sessile polyps grow slowly over many years. Some types may develop more quickly than others, depending on individual risk factors and genetics. Keeping up with regular screening helps ensure any changes are detected early, regardless of growth rate.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Medical Concierge
- 8.30am - 5.30pm
- WhatsApp: 9147 2051
Need help finding the right specialist or booking for a group?
Our Medical Concierge is here to help you. Simply fill in our form, and we'll check and connect you with the right specialist promptly.
Notice:
The range of services may vary between Thomson clinic locations. Please contact your preferred branch directly to enquire about the current availability.
Get In Touch