Heavy periods, ongoing pelvic pain, or discomfort that keeps coming back can be worrying, especially when you are not sure what is causing it. Many women quietly put up with these symptoms, assuming they are just part of life.
Two common conditions that may be behind these symptoms are adenomyosis and fibroids. While they can feel similar, they are quite different in how they develop and how they are treated.
Knowing the difference can help you feel more confident when speaking with your doctor and deciding on the next steps.
What is adenomyosis?
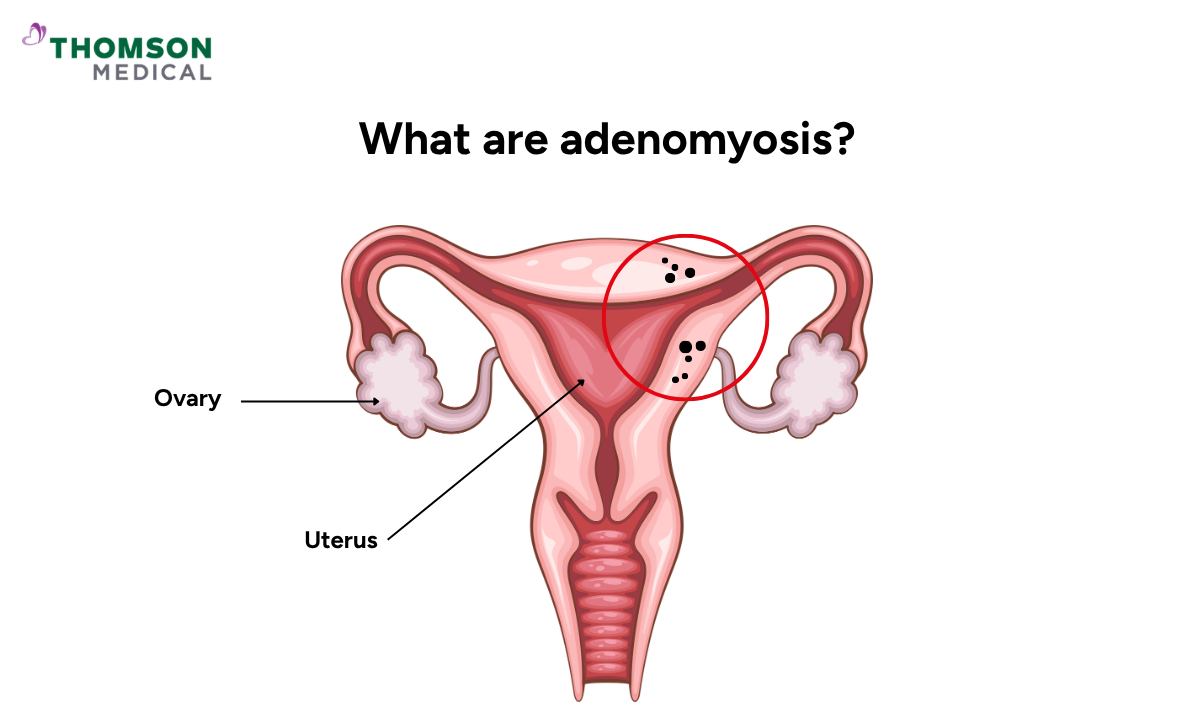
Adenomyosis happens when the tissue that lines the inside of your uterus (the endometrium) grows into its muscle wall. This can cause your uterus to become thicker or enlarged.
It can affect anyone with a uterus and is most commonly diagnosed in women aged 35 to 50, especially those who have had children.
Symptoms of adenomyosis
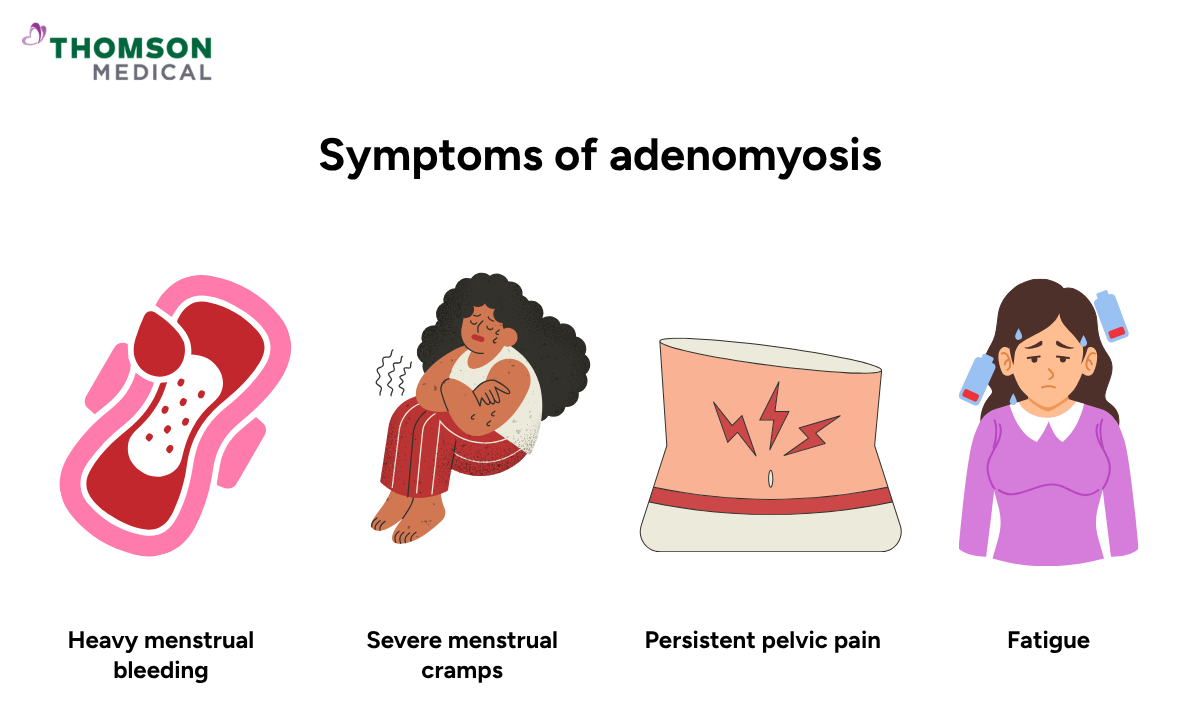
These symptoms can range from mild to more severe, and they may change over time.
You might notice:
Prolonged and heavy menstrual bleeding
Severe menstrual cramps (dysmenorrhoea)
Persistent pelvic pain, even outside of your menstrual cycle
A uterus that feels enlarged and tender
Fatigue or anaemia caused by significant blood loss
Not everyone with adenomyosis experiences the same symptoms. You may have mild discomfort, while others experience more noticeable symptoms. These symptoms don’t always reflect how extensive your condition is internally.
What causes adenomyosis?
The exact cause of adenomyosis is not fully understood, but certain factors may make it more likely for you to develop the condition.
Possible factors include:
Previous uterine surgery, such as a caesarean section or dilation and curettage (D&C)
Having given birth
Prolonged oestrogen exposure
Chronic inflammation of your uterine lining
Older age, as it tends to be more common in the years leading up to menopause
These factors may increase your risk, but having them does not mean you will develop the condition. If any of these apply and you have symptoms, your doctor can help clarify the cause.
Our gynaecologists
Loading...
What are fibroids?
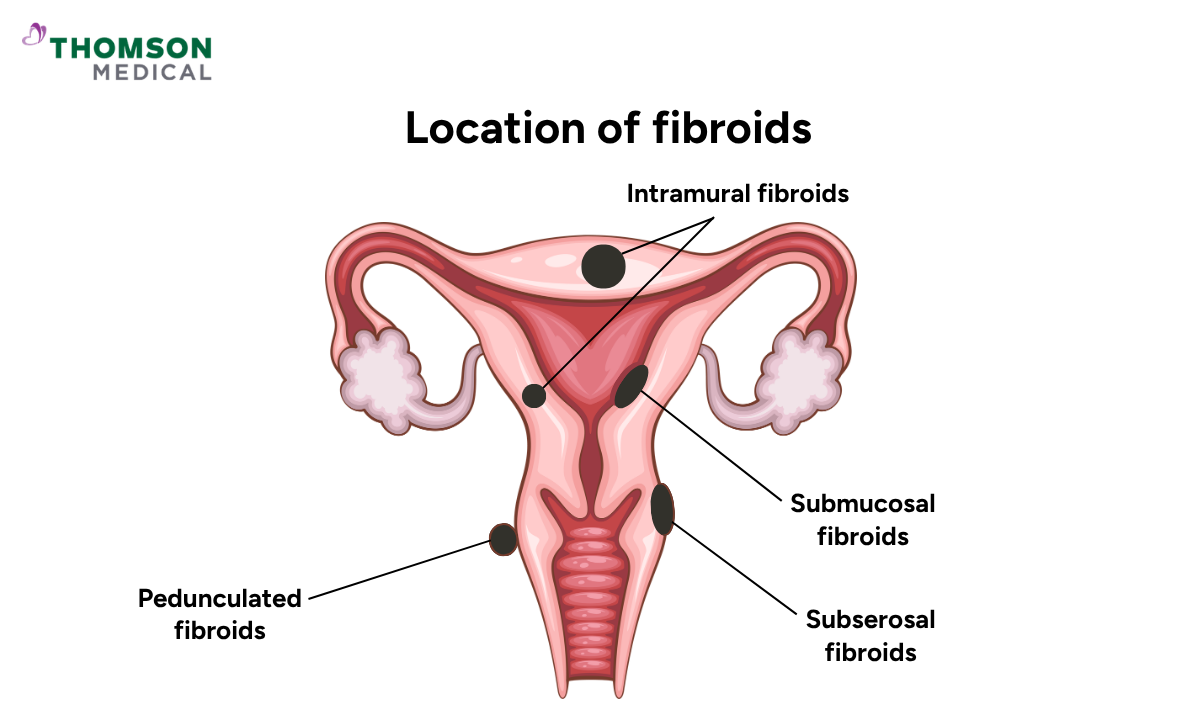
Fibroids are non-cancerous growths that develop from the muscle of your uterus. They can vary in size, from as small as a seed to as large as a melon, and may appear as a single growth or in clusters. Fibroids are very common, affecting up to 80% of women by age 50.
Fibroids are classified by location:
Intramural fibroids grow within your uterine wall and are the most common type
Submucosal fibroids grow into the inner cavity of your uterus
Subserosal fibroids grow outward from the outer surface of your uterus
Pedunculated fibroids are attached by a stalk and can be found either inside or outside your uterus
Knowing which type you have is useful because location plays a role in whether you develop symptoms and which ones.
Symptoms of fibroids
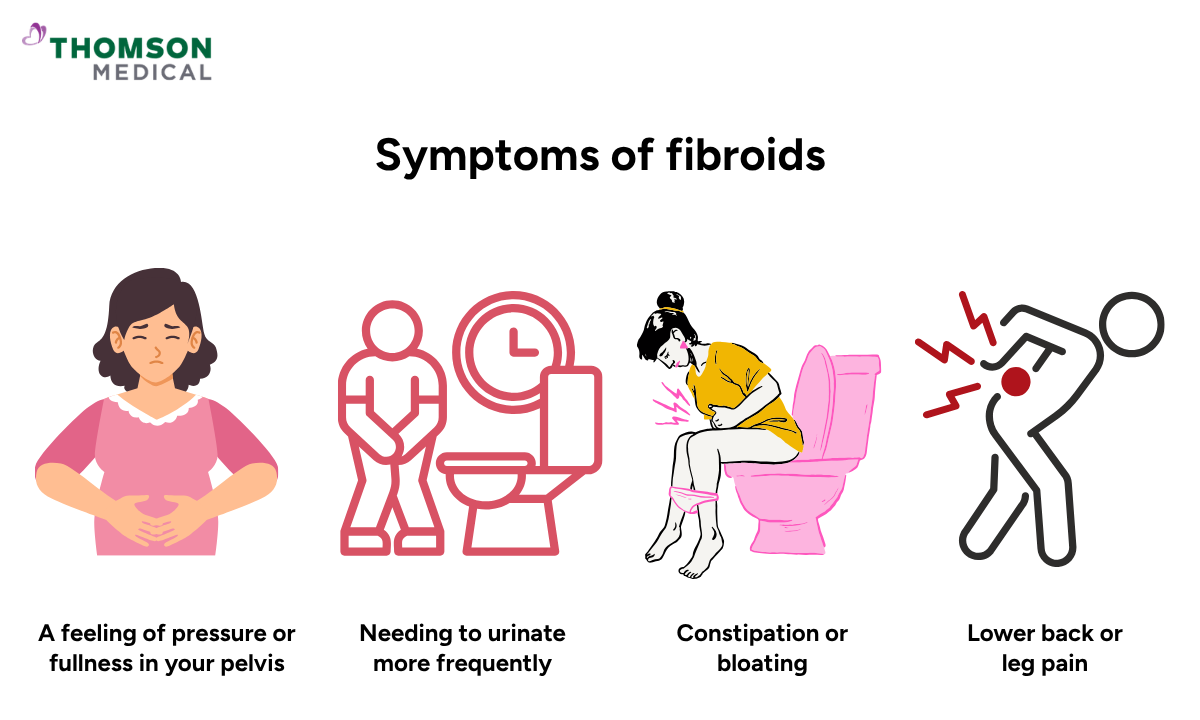
Like adenomyosis, you may have fibroids without noticing any symptoms. Many women only discover them after a routine scan.
You might experience:
Heavy menstrual bleeding and prolonged periods
A feeling of pressure or fullness in your pelvis
Needing to urinate more frequently
Constipation or bloating
Lower back or leg pain
Pain during sexual intercourse
Your experience may be different from others, and the size or number of fibroids doesn’t always determine how severe your symptoms will be.
What causes fibroids?
Fibroids often grow during your reproductive years and tend to shrink after menopause, showing how hormones influence their development.
Your risk of developing fibroids may be higher if you have:
High oestrogen and progesterone levels
A family history of fibroids
Started your periods at an early age
A higher body weight
Low vitamin D levels
Having these risk factors does not guarantee you will develop fibroids. If you have symptoms that concern you, speaking with your doctor is a good first step.
Experiencing heavy periods, pelvic pain, or pressure symptoms? Request an appointment with Thomson Medical to determine whether adenomyosis or fibroids may be the cause and explore suitable treatment options.
Key differences between fibroid and adenomyosis
Although adenomyosis and fibroids share several symptoms, knowing their key differences can help you and your doctor identify what is affecting you and why treatment approaches differ.
Here is how the two conditions compare:
Feature | Adenomyosis | Fibroids |
What it is | Endometrial tissue within the uterine muscle | Non-cancerous muscle growths |
Where it grows | Within the wall of your uterus | Inside, on, or outside your uterus |
Effect on your uterus | Diffusely enlarged and soft | Irregular or lumpy in shape |
Pain type | Severe period cramping is common | Pressure or fullness more common |
Bleeding | Heavy, painful periods | Heavy or irregular bleeding |
How it feels on examination | Diffuse tenderness throughout | Distinct, palpable lumps possible |
You can have both conditions at the same time. When they happen together, symptoms may feel more severe, but they can still be managed with support from your doctor.
How are they diagnosed?
Because these conditions share many similar symptoms, it is not always possible to tell the difference on your own. Your doctor will help clarify things using an exam and imaging tests.
During your assessment, you may expect:
A pelvic exam to assess the size and texture of your uterus
A pelvic or transvaginal ultrasound, which is usually the first imaging test
An MRI scan, which provides detailed imaging and is useful for confirming adenomyosis
Blood tests to check for anaemia if heavy bleeding is present
What imaging may show for adenomyosis
Because adenomyosis affects your muscle wall rather than appearing as a distinct lump, it can be harder to spot on a scan.
Your doctor will look for:
A generally enlarged uterus
Thickening of your uterine wall
Areas within your uterine muscle that are less clearly defined
Thickening of the junctional zone on an MRI, which is a specific inner layer of the uterine wall
In some cases, adenomyosis is only confirmed after a hysterectomy, when your uterine tissue can be examined directly.
What imaging may show for fibroids
Fibroids tend to be more straightforward to identify on imaging because they appear as distinct growths.
Your doctor will look for:
Well-defined, round masses with clear borders
Changes to the shape or contour of your uterus
Growths that vary in size and location within or around your uterus
Based on the imaging test, your doctor will guide you on the next steps and suitable treatment options.
Treatment options for adenomyosis and fibroids
Treatment for adenomyosis and fibroids can look different for each person. The approach usually depends on your symptoms, age, and whether you plan to have children.
Treating adenomyosis
Adenomyosis is usually managed rather than cured, unless the uterus is removed. Most treatments focus on relieving symptoms and improving quality of life.
Medications to help manage symptoms include:
Hormonal contraceptives (such as the pill, patch, or hormonal coil like the Mirena IUD) to help reduce bleeding and pain
Progestins or GnRH agonists to lower oestrogen levels and ease symptoms
Anti-inflammatory medicines such as ibuprofen for pain relief
Tranexamic acid to reduce heavy menstrual bleeding
Procedures to consider include:
Uterine artery embolisation, which blocks blood flow to affected areas and may reduce symptoms in some women
Hysterectomy, which is the removal of your uterus. This is generally considered when other treatments have not provided enough relief and you are not planning a future pregnancy
Because adenomyosis is influenced by hormones, symptoms may return if treatment is stopped before menopause. This is worth discussing when planning longer-term care with your doctor.
Treating fibroids
There are several ways to manage fibroids, including options that can shrink or remove them while preserving the uterus.
Medications to help manage fibroids include:
Hormonal contraceptives such as the pill or a hormonal coil
Hormone injections that temporarily shrink fibroids before a procedure
Tranexamic acid
Treatment procedures may include:
Uterine artery embolisation, which cuts off the blood supply to fibroids to shrink them
Myomectomy, which removes fibroids surgically while keeping your uterus intact. This is an option to explore if you still want to get pregnant
MRI-guided focused ultrasound, which uses sound waves to break down fibroid tissue without surgery
Hysterectomy
Fibroids can sometimes come back after a myomectomy, especially before menopause. Regular follow-up with your doctor may help you keep track of any changes and manage them early.
When should you see a doctor?
Some symptoms are worth checking early, especially if they are affecting your daily life or getting worse over time.
See your doctor if you experience:
Periods that are very heavy or last longer than 7 days
Severe pelvic or period pain that affects your daily life
Pain during sexual intercourse
Difficulty getting pregnant
Symptoms such as frequent urination, bloating, or lower back pain that are getting worse
Getting checked early means more options for treatment and can help you avoid complications, such as anaemia from blood loss. You do not have to manage these symptoms on your own, and your doctor is there to guide you.
If your symptoms are affecting your daily life or not improving, request an appointment with Thomson Medical. Early assessment can help you explore more treatment options and prevent complications.
FAQ
Is adenomyosis more painful than fibroids?
Adenomyosis is often more painful. It commonly causes strong menstrual cramps and a deep, aching pelvic pain. Fibroids, on the other hand, are more likely to cause a feeling of pressure or heaviness in the lower abdomen, though they can also be painful in some cases.
Can adenomyosis or fibroids affect my ability to get pregnant?
Yes, both conditions can affect fertility. Fibroids, especially those that grow inside the uterine cavity, are linked to difficulty getting pregnant. Adenomyosis may also make it harder by affecting how the uterus functions, but its impact can vary from person to person.
Do fibroids and adenomyosis go away after menopause?
Symptoms often improve after menopause because hormone levels, especially oestrogen, become lower. However, existing fibroids may shrink rather than disappear completely, and adenomyosis usually becomes less active rather than fully going away.
What is the main cause of adenomyosis and fibroids?
Both conditions are influenced by hormones, particularly oestrogen. Other factors such as genetics and past uterine procedures or injury may also play a role, but the exact cause is not always clear.
Can birth control help with adenomyosis or fibroids?
Yes, birth control and other forms of hormonal therapy can help manage symptoms like heavy bleeding and pain. However, it does not remove fibroids or cure adenomyosis but mainly helps control how the symptoms affect your daily life.
Can you have adenomyosis and fibroids at the same time?
Yes, it is possible to have both conditions at the same time. When this happens, symptoms may feel more intense, and it may take a bit more careful evaluation to decide on the most suitable treatment.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
Reference:
Marsh, E. E., Al-Hendy, A., Kappus, D., Galitsky, A., Stewart, E. A., & Kerolous, M. (2018). Burden, prevalence, and treatment of uterine fibroids: A survey of U.S. women. Journal of Women S Health, 27(11), 1359–1367. https://doi.org/10.1089/jwh.2018.7076
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
