It can be worrying when your baby’s mild sniffle develops into a deeper cough, especially if you notice a rattling sound in their chest or faster breathing. Many parents wonder whether it is simply a common cold or something more concerning.
Bronchitis refers to inflammation of the airways and is often caused by viral infections. While many coughs improve with supportive care, certain signs may require medical assessment.
Understanding how bronchitis presents in babies, what symptoms to monitor, and when to seek medical advice can help you respond calmly and ensure your baby receives appropriate care.
What is bronchitis?
Bronchitis occurs when the bronchial tubes, which carry air into your lungs, become inflamed. The inflammation causes the tubes to swell and produce excess mucus. This can narrow the breathing passages and make it harder for your baby to breathe.
In babies and toddlers under two years old, bronchiolitis is more common than bronchitis. This condition causes the bronchioles (tiny airways deeper in the lungs) to narrow and fill with mucus. The symptoms can look very similar, which is why you may hear these terms used interchangeably.
What causes bronchitis in babies?

Respiratory infections in babies can develop for several reasons, from everyday viruses to environmental triggers.
Because babies have smaller and more delicate airways, inflammation can occur more easily than in older children or adults. When your baby develops a chest infection, it is completely natural to wonder what may have caused it.
Common causes include:
Viral infections:
Respiratory syncytial virus (RSV) is a very common cause.
Influenza, adenovirus, and rhinovirus can also affect the airways.
They spread easily through coughs, sneezes, or close contact.
These infections become more common during flu seasons or when family members are unwell.
Environmental irritants:
If your baby inhales cigarette smoke, they’ll be more likely to catch bronchitis.
Smoke irritates your child’s respiratory tract and weakens their lungs’ ability to fight infections.
Underlying conditions:
Your baby could be more at risk if they were born prematurely or have underlying conditions such as congenital heart disease, chronic lung disease, or cystic fibrosis.
Chest infections are common in babies, and most recover well with rest and supportive care. Understanding the common causes can help you take simple steps at home and know when it may be worth checking in with a doctor.
Respiratory symptoms in babies can have many causes. Request an appointment with doctors at Thomson Paediatric Centre to review your baby’s symptoms and discuss appropriate care.
What are the symptoms?

Bronchitis often begins with symptoms similar to a common cold and may gradually worsen over a few days.
Early signs include:
Runny nose and nasal congestion
Mild fever
Dry, persistent cough
Worsening symptoms include:
Rapid breathing, often above 50–60 breaths per minute in young infants
Wheezing, which may sound like a high-pitched whistling noise when breathing out
Shortness of breath or visible effort when breathing
Difficulty feeding due to blocked or irritated airways
Increased irritability or unusual tiredness
It can be distressing to see your baby uncomfortable or struggling with breathing symptoms. Trust your instincts as a parent. If something feels unusual or concerning, seeking medical advice early can help ensure your baby receives timely care and reassurance.
How is bronchitis diagnosed?
If your baby has breathing issues or a cough that doesn’t stop, a paediatric assessment can help determine the cause and how serious it is.
During the consultation, the doctor will examine your baby and listen carefully to their chest. They will use a stethoscope to check for signs such as wheezing or crackling sounds in the lungs.
If further evaluation is needed, your doctor may recommend additional tests to confirm the diagnosis and rule out other conditions such as pneumonia.
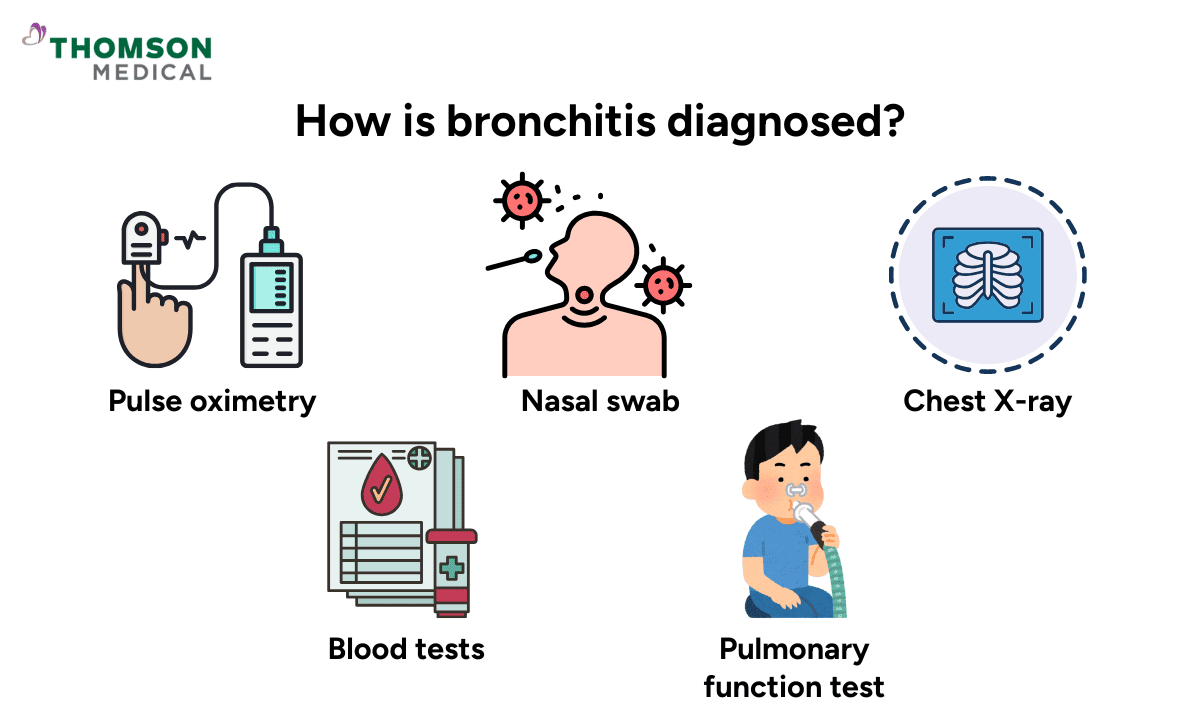
The tests may include:
Pulse oximetry:
A small sensor (pulse oximeter) is gently placed on your baby’s finger or toe to measure oxygen levels in the blood (oxygen saturation).
This test is painless and helps doctors assess how well your baby is breathing.
Nasal swab:
A swab is taken from your baby’s nose to test for specific viruses like RSV or the flu.
Chest X-ray:
Your doctor may suggest this if pneumonia or other lung conditions are suspected.
Blood tests:
These are usually performed if your doctor suspects a bacterial infection or if the illness appears severe.
Getting your baby checked early helps doctors evaluate how serious the infection is and decide on the best care for your little one. It can also help reassure you that your baby is receiving safe and appropriate care.
How is bronchitis treated?
Since bronchitis is usually caused by a virus, antibiotics usually won’t help. Instead, care focuses on keeping your baby comfortable while their immune system clears the infection.
What can you do at home?
If your baby has mild bronchitis symptoms, caring for them at home is usually enough to help them get better.
Some simple home care steps you can try include:
Use a nasal aspirator or saline spray to gently clear mucus, especially before feeding or sleep
Offer smaller, more frequent feeds to keep your baby hydrated
Use a cool-mist humidifier to help soothe their airways
Avoid over-the-counter cough medicines unless prescribed by a doctor, as they may be unsafe and are usually not effective for infants
Do not give aspirin due to the risk of Reye syndrome, which is a rare but serious condition
Most babies slowly get better with enough rest, fluids, and care. Once you notice something unusual or getting worse, home care may not be enough, and it’s best to check with your doctor.
Medical treatment
If your baby has difficulty breathing or becomes dehydrated, hospital care may be needed. Treatment will focus on supporting their breathing, keeping them well-hydrated, and ensuring they receive adequate nutrition.
Common medical treatments include:
Oxygen therapy:
If your baby’s oxygen levels fall below a safe range, doctors may provide supplemental oxygen to support their breathing.
Intravenous fluids:
An intravenous drip (IV) may be used to provide fluids if the baby cannot feed well.
Tube feeding:
In some cases, a small feeding tube may be placed through the nose into the stomach.
This helps ensure your baby gets enough milk or nutrients when they cannot feed on their own.
Medications:
Bronchodilators (nebulisers) may be tried to open the airways, though they don't work for every baby.
Your baby will be closely watched by healthcare professionals to make sure they are safe and comfortable while they recover.
When to seek urgent medical care
While many babies recover from bronchitis with home care, breathing problems can sometimes get worse quickly. It is important to know the warning signs that require immediate medical attention.
Seek medical urgency immediately if your baby:
Has pauses in breathing (apnoea)
Develops a bluish colour around the lips, skin, or fingernails (cyanosis)
Makes grunting sounds with each breath
Shows severe chest retractions (visible pulling-in of the skin around the ribs or neck during breathing)
Becomes extremely drowsy, weak, or difficult to wake
Although these warning signs can feel frightening, they are also clear signals that help you know when to seek medical intervention.
Our Paediatricians
Loading...
How to prevent bronchitis

You may be wondering if you can protect your child from bronchitis. While it cannot completely prevent viruses, a few simple precautions can reduce the risk of respiratory infections and help keep your baby healthier.
Here are steps you can take to prevent bronchitis:
Wash your hands often and use hand sanitizer before holding the baby
Ensure your baby receives the influenza vaccine (from 6 months of age) and discuss RSV prevention options with your paediatrician
Keep your baby away from tobacco smoke
Avoid crowded places or contact with sick people during peak flu and RSV seasons
Taking simple precautions and staying attentive to your baby's symptoms can make a meaningful difference. If your baby does become unwell, early advice from a healthcare provider can help support a smoother recovery.
If you ever feel unsure about your baby’s breathing or overall condition, it is always best to seek medical advice. You may schedule an appointment at Thomson Paediatric Centre to receive a medical diagnosis that can help support your baby’s recovery and wellbeing.
FAQ
Is bronchitis the same as asthma?
No. They can share symptoms like wheezing and coughing, but bronchitis is usually a temporary infection. Babies who have severe respiratory illnesses, such as bronchiolitis, may have a higher chance of developing asthma later in life, especially if there is a family history of respiratory or heart conditions.
Can I use a steam bowl for my baby?
It is safer to use a cool-mist humidifier. Steam from hot water can cause burns. Sitting with your baby in a steamy bathroom, with the hot shower running but not placing your baby in the shower, may sometimes help loosen mucus.
How long does the cough usually last?
Symptoms are usually most noticeable during the first week, but the cough may last 2 to 3 weeks while the airways heal. This is usually normal if your baby is feeding well and breathing comfortably.
Do antibiotics help treat bronchitis?
Antibiotics treat bacterial infections, not viruses. Since most cases of bronchitis are viral, antibiotics usually do not help and may cause side effects. They are only used when tests or examinations suggest a secondary bacterial infection, such as pneumonia.
What is the difference between a cold and bronchitis?
A cold usually affects the nose and throat, which are part of the upper respiratory tract. Bronchitis and bronchiolitis affect the bronchial tubes and smaller airways in the lungs. When a cold spreads to the chest and causes wheezing or faster breathing, it may have developed into a lower respiratory infection.
Is bronchitis contagious?
Bronchitis symptoms are not what spread, but the viruses causing the illness are contagious. These viruses can spread through coughing, sneezing, or close contact, especially among babies and young children.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
Reference
Walsh, R., Costello, L., DiCosimo, A., Doyle, A.-M., Kehoe, L., Mulhall, C., O’Hara, S., Elnazir, B., Meehan, J., Isweisi, E., Semova, G., Branagan, A., Roche, E., & Molloy, E. (2024). Bronchiolitis: Evidence-based management in high-risk infants in the intensive care setting. Pediatric Research, 96, 1560–1567. https://doi.org/10.1038/s41390-024-03340-y
