Finding out you have an endometrial polyp while trying to conceive can feel unsettling, especially when you're already carrying the emotional weight of the journey. It's natural to wonder whether this concern is what's been standing in the way and what it means for your chances of pregnancy.
Polyps are common and treatable, and addressing them can significantly improve your chances of conception. Knowing how they affect fertility and what your options are is a good place to start.
What is an endometrial polyp?
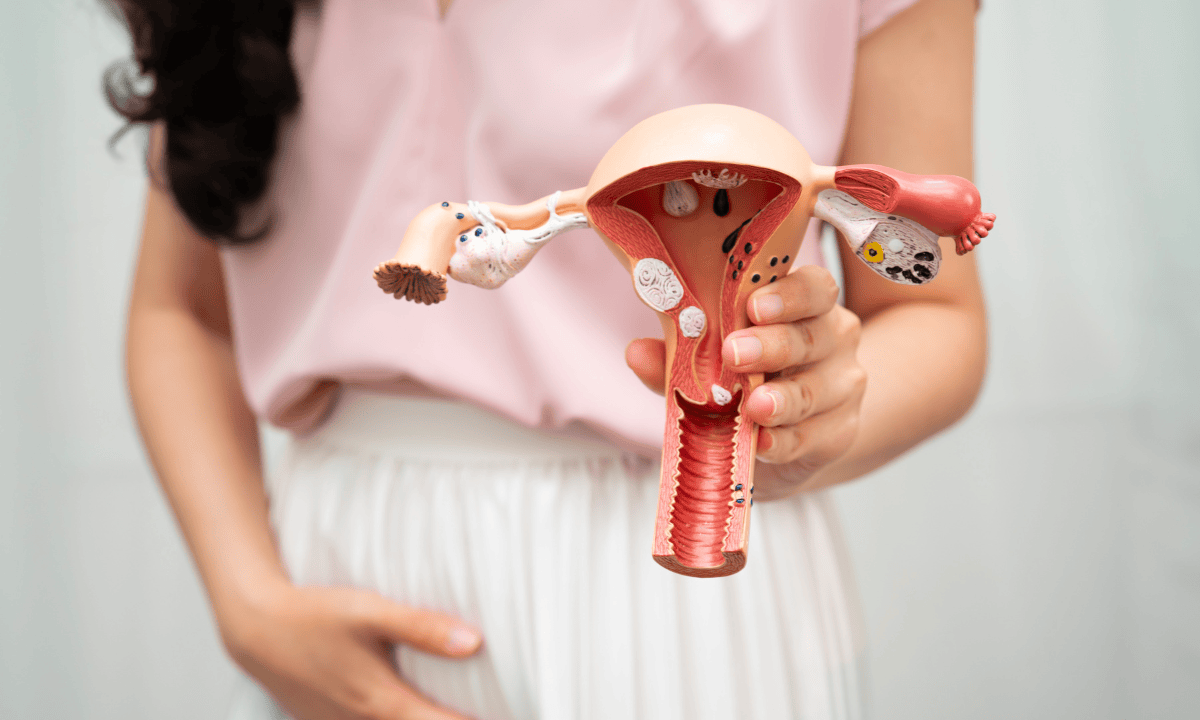
An endometrial polyp is a soft overgrowth of tissue from your uterine lining (the endometrium). It attaches to the inner wall of your uterus, ranging from a few millimetres to a few centimetres, and you may have one or several.
They form when oestrogen overstimulates localised areas of the lining, which is why they become more common as hormones shift with age.
Polyps are not fibroids. Fibroids grow from muscle tissue within the uterine wall, while polyps grow from the lining inside the cavity. Both are usually benign, but they are different conditions managed differently.
Who is most likely to get endometrial polyps?
Polyps are most common in women aged 35-50, though younger women can also develop them.
Your risk may be higher if you:
Have polycystic ovary syndrome (PCOS) or a hormonal imbalance
Are in perimenopause
Have a higher body weight (BMI 30 or above)
Take tamoxifen (used in breast cancer treatment) or hormone replacement therapy (HRT)
Have hypertension
Many women, however, have no identifiable risk factors at all. Having one or more of these factors does not mean you will develop a polyp. It simply means it is worth discussing with your doctor during your next visit.
How are endometrial polyps diagnosed?
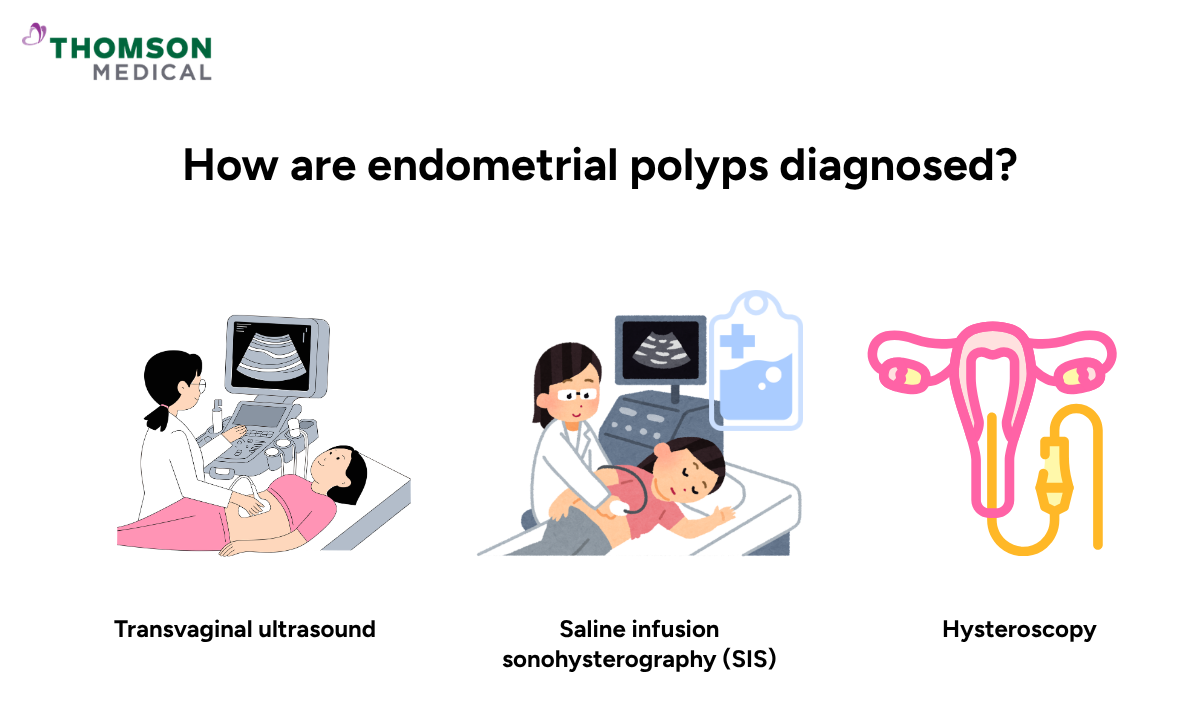
Endometrial polyps are often found during a routine scan or fertility workup, before causing any noticeable symptoms.
If one is suspected, your doctor may use one or more of the following to investigate:
Transvaginal ultrasound:
Transvaginal ultrasound is usually the first step. A small probe is gently placed into the vagina to produce images of your uterus.
It is widely available, though smaller polyps can sometimes be missed.
Saline infusion sonohysterography (SIS):
SIS builds on a standard ultrasound by introducing a small amount of saline into the uterine cavity before scanning.
The fluid creates contrast that makes polyps easier to see.
Hysteroscopy:
Hysteroscopy allows your doctor to see inside the uterus directly.
A thin, flexible camera is passed through your cervix to examine the inside of your uterus.
It also allows the polyp to be removed at the same time, making it both a diagnostic and treatment option in one procedure.
Your doctor will recommend the appropriate approach based on your symptoms, fertility goals, and scan findings.
If you're unsure whether you might have a polyp or aren't sure which diagnostic approach is right for you, schedule an appointment with Thomson Medical. Our doctors can assess your situation and guide you through the next steps.
How do endometrial polyps affect implantation?
If you're trying to conceive, you're probably wondering why a polyp makes it harder to get pregnant. The answer is that it can interfere in more than one way, and understanding this can help make sense of why your doctor may recommend addressing it.
The endometrium needs to be in the right condition for an embryo to implant and grow.
Polyps can disrupt this in a few ways:
Physical obstruction:
A polyp takes up space inside the uterus, which can get in the way of where an embryo needs to settle.
Disrupted uterine lining:
Polyps can interfere with the signals your uterine lining sends to a fertilised egg, making it harder for it to attach.
Local inflammation:
Polyp tissue can cause low-level irritation in the surrounding lining, creating conditions that are less welcoming for an embryo.
Sperm transport:
Larger polyps near the cervical canal may affect how sperm travel through the uterus.
It is worth noting that not every polyp will cause fertility problems. The degree of impact depends on a number of individual factors, which is why your doctor's assessment matters.
Why the location of the polyp matters
Size alone does not tell the whole story. Where a polyp sits inside the uterus is just as important as how big it is:
Near the tubal openings (ostial polyps):
These sit close to where the fallopian tubes meet the uterus and are considered the most likely to interfere with both natural conception and assisted fertility treatment.
Mid-cavity or fundal polyps:
These are located in the upper part of the uterus and are closely associated with implantation failure.
Lower uterine segment or cervical polyps:
These are less likely to affect implantation directly but may impact sperm movement.
That said, polyps larger than 1 cm tend to be considered more clinically significant. However, a smaller polyp in a critical location can be just as relevant. Your specialist will consider both size and position together when deciding on the right next step for you.
Gynaecologists at Thomson Medical
Loading...
Does removing an endometrial polyp improve your chances of conceiving?

If your doctor has recommended removing a polyp, you may be wondering whether it will actually make a difference.
For many women, it does.
Removing a polyp can meaningfully improve your chances of conceiving – whether you're trying naturally or through fertility treatments. It clears a potential barrier inside the uterus and helps restore the endometrium to a healthier state for implantation.
That said, endometrial polypectomy is not a guarantee of pregnancy. Other factors, such as ovarian reserve, sperm quality, and tubal health, remain part of the picture. Your doctor will help you understand what role the polyp may be playing for you specifically.
What to expect after polypectomy
Hysteroscopic polypectomy is a minimally invasive, outpatient procedure carried out under general or local anaesthesia. Most women go home the same day.
In the days that follow, you may experience:
Light spotting or cramping
Mild bloating or discomfort
A return to normal activities within 24-48 hours for most women
The removed tissue is routinely sent for analysis to give your doctor the full picture and guide any further care if needed.
How soon can you try to conceive after removal?
The waiting period is often shorter than people expect. For natural conception, one to three menstrual cycles is a typical guide. For IVF, your doctor may recommend moving forward after just one – it depends on how your body is healing.
It may feel like a frustrating pause, especially if you've already been patient. But a well-recovered uterine lining gives an embryo the best possible environment to implant. Your doctor will be able to advise on the right timing for you.
Endometrial polyps and in-vitro fertilisation (IVF)
Finding out you have a polyp while preparing for in-vitro fertilisation (IVF) can feel like an unwelcome setback, but it is one that can be addressed before your cycle begins.
Here is what to expect:
Most fertility specialists recommend removing a polyp before embryo transfer, as even a small polyp can affect how well the uterine lining receives an embryo
If a polyp is found mid-cycle, your doctor will likely suggest postponing the transfer to allow time for removal and recovery
Polypectomy before IVF is usually done in the cycle before your planned transfer, followed by a short recovery period
Once your uterine lining has healed, you can move forward with your IVF cycle
Having a polyp does not disqualify you from IVF. For many women, addressing it beforehand is simply one extra step, and it gives your embryo a better chance of implanting successfully.
If you're weighing whether to proceed with polypectomy before your fertility treatment or have questions about recovery and timing, schedule an appointment with Thomson Medical. Our doctors can walk you through your options and help you plan the right next step.
FAQ
What are the chances of getting pregnant with an endometrial polyp?
It is possible to conceive with a polyp, but it may reduce your chances – particularly if it sits in a location that interferes with implantation. If you are concerned, speaking to your doctor is a good first step.
Should I have my endometrial polyp removed before trying to conceive?
This depends on the size, location, and how long you have been trying. For many women with fertility concerns, removal is a straightforward step to improve conditions for implantation. Your specialist will help you decide the right approach for your situation.
Can a small endometrial polyp affect fertility?
Possibly. Even smaller polyps can affect the endometrium depending on where they sit – size is only part of the picture. Your doctor will consider both size and location when advising you.
Will an endometrial polyp go away on its own?
While small polyps can occasionally regress on their own, this is not reliable – particularly in women who are trying to conceive. Removal is generally a more predictable path forward than waiting.
How is an endometrial polyp removed, and is it safe?
The standard approach is hysteroscopic polypectomy, a minimally invasive outpatient procedure where a thin camera is passed through the cervix to locate and remove the polyp. It has a low complication rate and most women go home the same day.
Can endometrial polyps cause miscarriage?
There is some evidence linking polyps to early pregnancy loss, likely due to inflammatory changes in the endometrium they can create. Removing the polyp is thought to reduce this risk, though other factors also play a role.
How long after polyp removal can I start trying to get pregnant?
For natural conception, most specialists suggest waiting one to three menstrual cycles. For IVF, your doctor may be comfortable moving forward after just one. Your care team will advise based on how you are recovering.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations based on your medical conditions, request an appointment with Thomson Medical.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) - Jurong:
6262 8588 (Call), 6262 8588 (WA) - Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
Notice
The range of services may vary between TWC/TS locations. Please contact your preferred branch directly to enquire about the current availability.
Request an Appointment