Finding out you need surgery can feel overwhelming, especially when you are faced with unfamiliar terms like 'laparoscopy' and 'laparotomy'. It is natural to want to know what each procedure involves and what to expect.
Both are surgical procedures used to treat conditions in the abdomen or pelvis. The key difference is how your surgeon accesses your body during the operation. Knowing what sets them apart can help you feel more prepared and confident going into your conversations with your doctor.
What is laparoscopy?
Laparoscopy is a minimally invasive surgery. Your surgeon makes several small cuts, each about 0.5 to 1 cm, near your abdomen or pelvis.
Through one of these small cuts, a thin tube with a tiny camera called a laparoscope is inserted. This gives the surgeon a clear view of your internal organs on a screen.
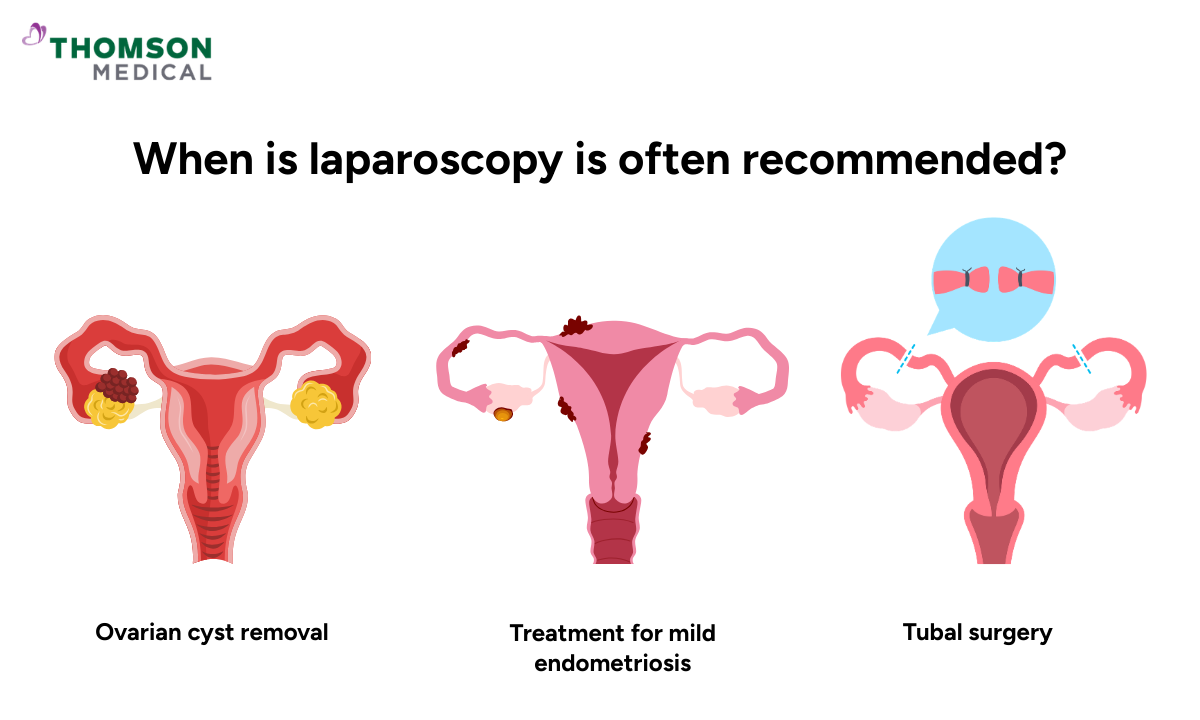
Laparoscopy is often recommended when:
The condition is smaller or less complex
You need removal of an ovarian cyst
Treatment for mild endometriosis or fibroids is needed
Your doctor needs to investigate unexplained pelvic pain
Fertility-related procedures such as tubal surgery or hysterectomy are planned
If you have been recommended laparoscopy, it is a sign that your condition may be manageable through smaller cuts. This can mean a smoother recovery and a quicker return to your daily routine.
What is laparotomy?
Laparotomy is open surgery. Your surgeon makes a single, larger cut across your lower abdomen to directly access your organs.
This approach provides a full, clear view and more space to operate, which can be important in complex situations.
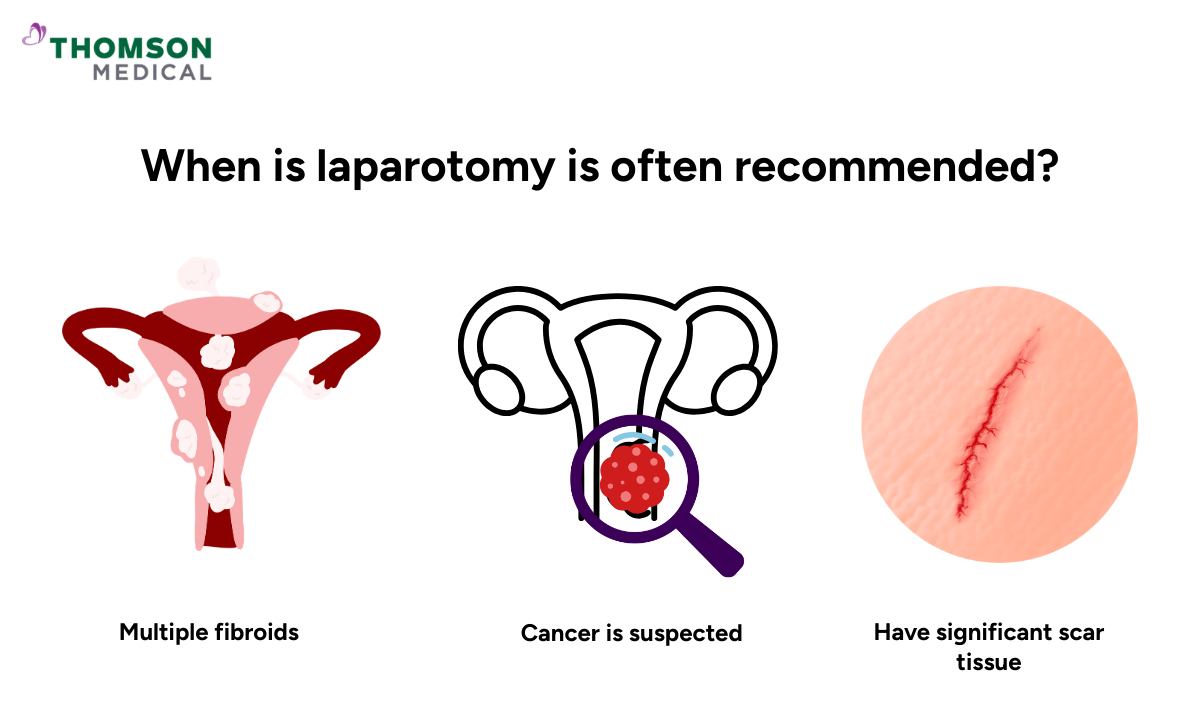
Laparotomy is often recommended when:
You have large or multiple ovarian cysts or fibroids
Cancer is suspected or diagnosed
You have significant scar tissue from previous surgeries
Direct access is needed for safety or precision
Hearing that you need open surgery can feel worrying. However, in certain cases, this approach offers better control during the operation and allows your surgeon to manage complex conditions effectively.
Key differences between laparoscopy and laparotomy
Both procedures treat conditions in the abdomen or pelvis. The table below summarises the main differences to help you understand what each approach involves.
Aspect | Laparoscopy | Laparotomy |
Incision size | Several small cuts (0.5 to 1 cm) | One large cut across the lower abdomen |
How it works | The camera guides the surgery on a screen | The surgeon works directly with full visibility |
| Duration of surgery | Usually 30 minutes to 1 hour, depending on the procedure | Usually 1 to 3 hours, depending on complexity |
Scarring | Minimal | More noticeable |
Pain after surgery | Usually mild | More significant |
Hospital stay | Often same day or 1 to 2 days | 3 to 7 days |
Suited for | Smaller or straightforward conditions | Larger, complex, or high-risk conditions |
These differences matter because they affect your day-to-day recovery. Smaller incisions mean less pain when moving, coughing, or getting out of bed. The choice between procedures depends on your condition and what will give you the appropriate treatment.
If you’re unsure which procedure is right for your condition, request an appointment with Thomson Medical. Our specialists can assess your situation, explain the differences between laparoscopy and laparotomy, and help you understand the recovery, risks, and benefits of each option.
What happens before your procedure
Before either procedure, your doctor will carry out a thorough assessment to make sure you are fit for surgery. This may include blood tests, imaging scans, or a physical examination depending on your condition.
Your preparation will likely include:
Fasting:
You will be asked to stop eating and drinking for several hours before surgery, usually from midnight the night before.
This reduces the risk of complications during anaesthesia.
Medication review:
Your doctor may ask you to temporarily stop certain medications such as blood thinners before the procedure.
This is because some medications can increase the risk of bleeding during surgery.
Bowel preparation:
In some cases, your doctor may prescribe bowel clearing medication before your procedure.
This helps reduce the risk of infection during surgery.
Before your surgery goes ahead, your doctor will walk you through a consent form covering the procedure and its risks. This is also a good opportunity to ask any remaining questions so you feel fully prepared and at ease.
How each procedure is performed
Knowing what happens during surgery can help ease any worries you may have about the procedure itself.
Laparoscopy
You will be given a general anaesthetic. Your surgeon makes a small cut near your navel (belly button) and inserts the laparoscope.
Your abdomen is gently filled with gas to create space, which allows the surgeon to see clearly and work safely. A few additional small cuts are then made so surgical instruments can be inserted. The surgeon carries out the operation while viewing a magnified image on a screen.
Laparotomy
You will also receive a general anaesthetic. Your surgeon makes one larger incision across your lower abdomen, giving direct access to the organs. This allows for more extensive work, such as removing large tissue or repairing or rebuilding affected tissue.
Both procedures are performed under full anaesthesia, so you won't feel anything during the operation. The main difference is in how your surgeon accesses the area that needs treatment.
What to expect when recovering?
A recovery of several weeks can feel overwhelming, especially if you have work or family commitments. But the recovery looks different depending on which procedure you have.
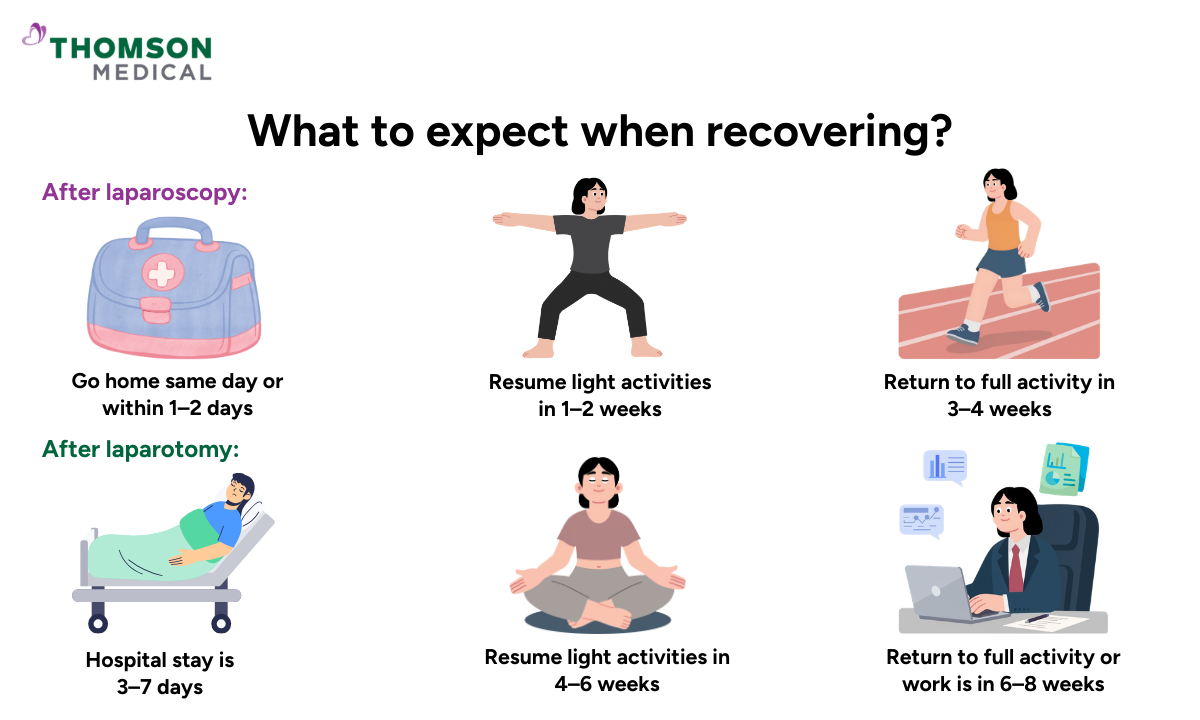
After laparoscopy:
You may go home the same day or after 1 to 2 days
Light activities can often resume within 1 to 2 weeks
Most people return to full activity within 3 to 4 weeks
Pain is usually manageable with standard pain relief
Laparoscopy recovery is faster because the smaller incisions heal more quickly and cause less disruption to your abdominal muscles.
After laparotomy:
You may stay in hospital for 3 to 7 days
Light activities may resume after 4 to 6 weeks
Full return to work or intense activity can take 6 to 8 weeks
Recovery includes looking after your wound and slowly getting back to normal movement
The longer recovery allows your abdominal wall to heal properly and regain its strength. You may find they feel considerably better within the first few weeks, even though full healing takes longer.
Everyone heals at their own pace. If you are unsure what to expect after your surgery, your doctor can give you a clearer picture based on your procedure.
Gynaecologists at Thomson Medical
Loading...
What are the risks and complications?
Both laparoscopy and laparotomy are safe procedures performed routinely by experienced surgeons. Like all surgery, it carries some risk, and understanding these can help you feel more prepared.
Risks common to both procedures include:
Bleeding or infection
Injury to nearby organs such as the bladder or bowel
Anaesthetic complications
Rarely, you may also experience temporary bloating or shoulder discomfort from the gas used during surgery.
There are also additional risks specific to laparotomy:
Wound infection or hernia at the incision site
More noticeable scars and discomfort that may last longer
Because the incision is larger, the overall risk of complications is slightly higher with laparotomy.
Your surgical team takes precautions to reduce risks and monitors carefully during recovery. Most complications can be treated if identified early. If you notice anything unusual after surgery, contact your doctor promptly.
Choosing the right procedure for you
Other than medical factors, there are personal factors that are also considered in deciding which surgery is suitable.
Key things to discuss include:
Recovery time:
If returning to work or daily life quickly is a priority, laparoscopy may be more suitable where clinically appropriate.
Fertility:
Both procedures can preserve fertility, but laparoscopy causes less scar tissue, which may reduce the risk of adhesions (internal scar tissue).
Surgical history:
Previous operations or significant scar tissue may affect what is safely possible.
Your overall health:
Other medical conditions may influence which approach is the most appropriate for you.
If any of these points are important to you, discuss them with your doctor before the procedure. It is easier to address concerns at the planning stage than after. Your surgeon will review your scans, symptoms and medical history to determine which approach is most appropriate for you.
Cost comparison between laparoscopy and laparotomy in Singapore
Understanding the potential costs can help you plan ahead and explore your payment options.
Costs can vary depending on the hospital, the complexity of your surgery, and any additional procedures required.
Note that these are based on 2025/2026 prices and that the exact cost can shift depending on your individual circumstances.
Procedure | Typical cost at private hospitals |
SGD 7,200 to SGD 11,750 | |
Laparotomy | SGD 6,000 to SGD 10,000 |
Several things can influence your final bill:
More complex surgery takes longer and uses more resources, increasing the cost
A longer hospital stay adds to the overall bill
Surgeon and anaesthetist fees vary, and experienced specialists may charge more
Additional procedures such as biopsies or fibroid removal increase the total cost
Postoperative care, including medications and follow-up, can also raise the final amount
It is worth speaking to your hospital's billing team before your procedure to get a cost estimate tailored to your situation. They can also explain payment plans or insurance coverage options that may be available to you.
If you want a clearer idea of what your surgery might cost and what your payment options are, request an appointment with Thomson Medical. Our team can provide a personalised estimate and guide you on insurance coverage, hospital fees, and any additional procedures that may affect your total bill.
FAQ
Which procedure is less invasive?
Laparoscopy is the less invasive option. It uses small cuts of about 0.5 to 1 cm, while laparotomy requires a much larger incision. This means less tissue disruption, smaller scars, and less pain after surgery.
Which has a shorter recovery?
Laparoscopy has a shorter recovery. Most people can return to light activities within 1 to 2 weeks and feel fully recovered in 3 to 4 weeks. Laparotomy recovery can take 6 to 8 weeks, depending on the complexity of the surgery and your individual healing.
Can both procedures be used for fertility treatments?
Yes, both can be used for fertility-related surgery, such as removing cysts or fibroids or treating endometriosis. Laparoscopy is often preferred because it causes less scar tissue, which may reduce the risk of adhesions that could affect conception. Laparotomy may be necessary if the problem is large or complex.
Are there size or condition limitations for laparoscopy?
Yes. Large cysts, multiple large fibroids, extensive scar tissue from previous surgeries, or suspected cancer may make laparoscopy difficult or unsafe. In these cases, laparotomy may be the more appropriate option.
Can the surgeon switch from laparoscopy to laparotomy during the operation?
Yes, this can happen. If your surgeon encounters unexpected complications during laparoscopy, such as excessive bleeding or difficulty seeing clearly, they may convert to laparotomy to keep you safe. This is a precautionary step taken for your safety.
Are there longer-term risks with either procedure?
Both procedures are safe, but some longer-term risks are worth knowing. With laparoscopy, there is a small chance of developing adhesions, which may rarely cause pain or affect fertility. With laparotomy, the risk of adhesions is slightly higher, and there is also a risk of hernia at the incision site and longer-lasting discomfort.
The information is intended for general guidance only and should not be considered medical advice. For personalised recommendations and advice based on your unique situation, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
Reference:
Ministry of Health. (2026). SI701L - Laparotomy Debulking (Advanced Disease, Primary/Recurrent) – Bill information. Singapore Ministry of Health. Retrieved March 2, 2026, from https://www.moh.gov.sg/managing-expenses/bills-and-fee-benchmarks/cost-financing/tosp-si701l-bill-information/
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) - Jurong:
6262 8588 (Call), 6262 8588 (WA) - Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
Notice
The range of services may vary between TWC/TS locations. Please contact your preferred branch directly to enquire about the current availability.
Request an Appointment