Heavy periods. Cramping that feels sharper than usual. A dull ache in your pelvis or lower back that comes and goes. If this describes what you have been going through each month, you may be wondering whether fibroids could be behind it.
The short answer is yes, fibroids can cause pain, though it does not look the same for every woman. Knowing what kind of pain points fibroids have and what it might mean for your day-to-day life can help you feel ready to speak with your doctor about what to do next.
What are uterine fibroids?
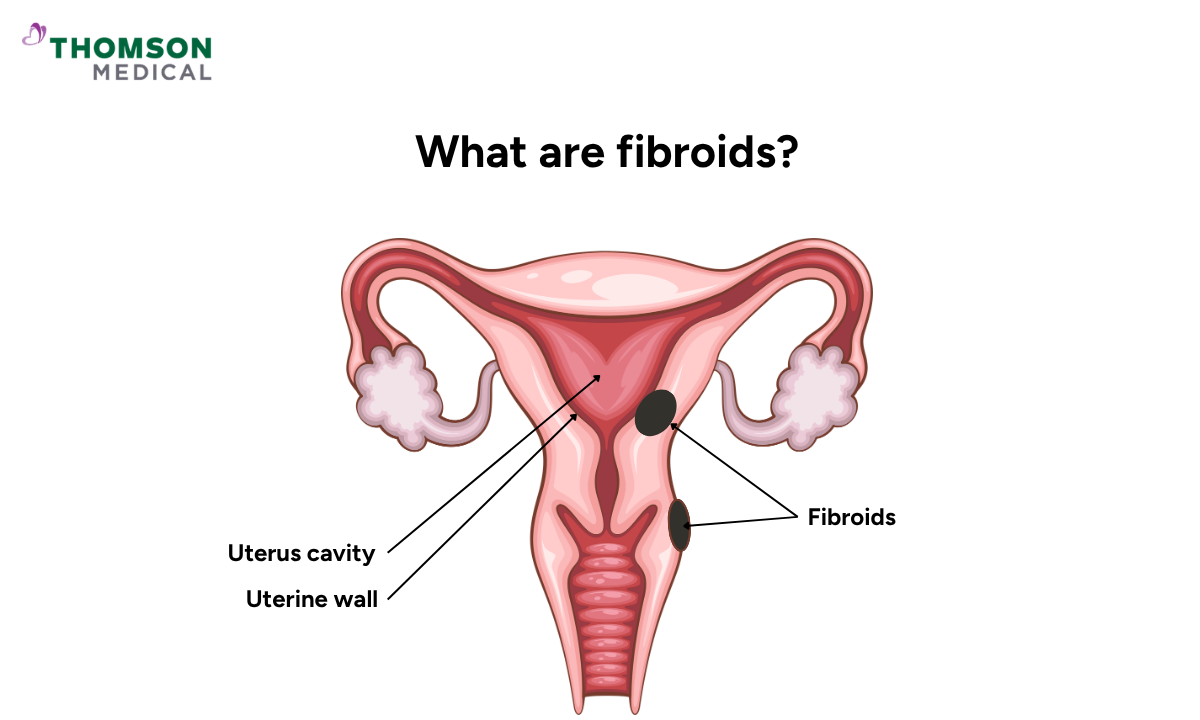
Uterine fibroids are non-cancerous growths made up of muscle and fibrous tissue, and they develop in or around the uterus.
They are sensitive to the hormones oestrogen and progesterone. This is why they tend to grow during the reproductive years and often shrink naturally after menopause.
Can fibroids cause pain?
Yes, fibroids can cause pain. But many women with fibroids never feel any discomfort. When pain does happen, every woman's experience is different.
You might notice it as:
Pain that is mild or severe
Discomfort that is constant, or that comes and goes
A sensation that feels sharp, dull, or cramping
Pain tends to occur when fibroids grow large enough to press on nearby organs. It can also happen when they affect how the uterus normally works.
If any of these sensations feel familiar, speaking with your doctor is a good first step toward understanding what might be causing them.
Our gynaecologists
Loading...
Why do fibroids cause pain?
When pain does occur, it is often due to the size and position of the fibroids within the uterus. These factors influence how noticeable the symptoms are.
Size and growth
As fibroids grow, they stretch the surrounding uterine tissue. The larger or faster a fibroid grows, the more pressure it can place on nearby areas, which is often what causes the discomfort you feel. This is also why symptoms can change over time, even if your fibroids have been present for a while.
Location
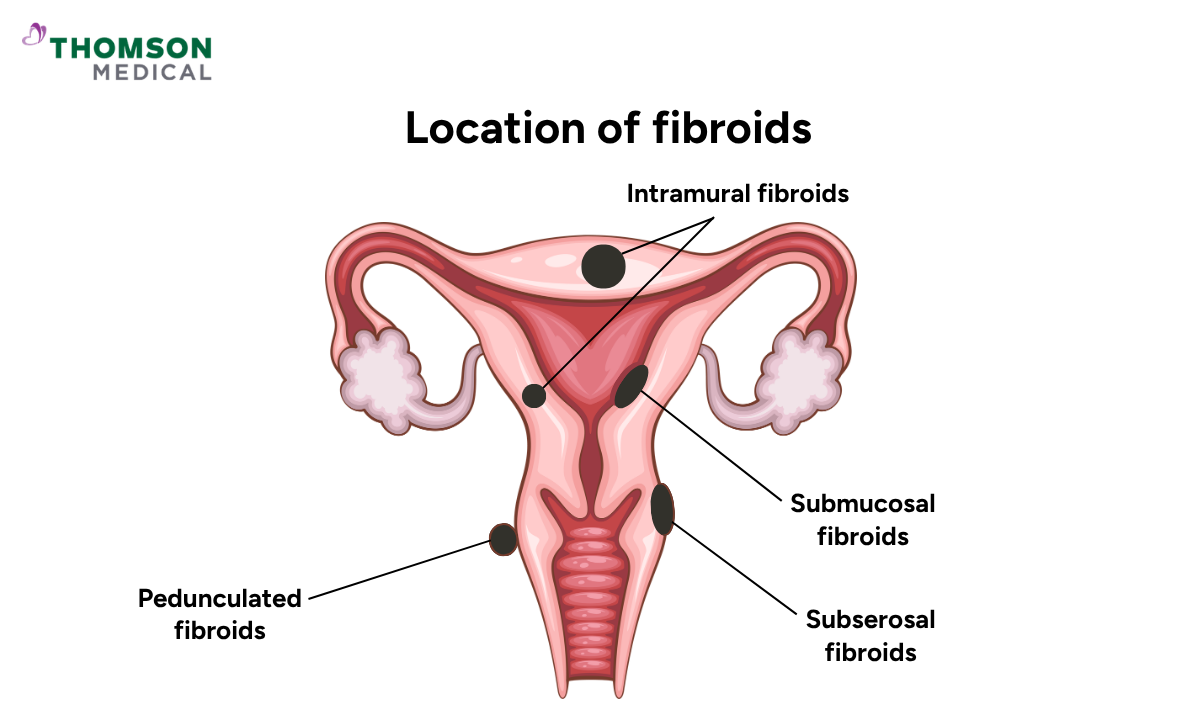
Fibroids can grow in different places within or around the uterus, and their location often influences the symptoms you experience.
Common types include:
Submucosal fibroids, which grow just beneath the inner lining of the uterus
Intramural fibroids, which grow within the muscular wall of the uterus
Subserosal fibroids, which grow on the outer surface of the uterus
Pedunculated fibroids, which grow on a stalk, either inside or outside the uterus
This is why two women with the same type of fibroid can have quite different experiences. Understanding your specific situation matters when discussing treatment with your doctor.
Degeneration or twisting
Although it is uncommon, fibroids can occasionally break down or change in a way that causes more sudden symptoms.
When a fibroid grows faster than its blood supply can support, it begins to break down. This process is known as degeneration, and it can cause sudden, sharp pain and sometimes fever or nausea. In some cases, a pedunculated fibroid can twist on itself, cutting off its blood supply and causing intense pain.
If you notice sudden or severe pain, speaking to your doctor can help you understand what is causing it and what care you may need.
What types of pain can fibroids cause?
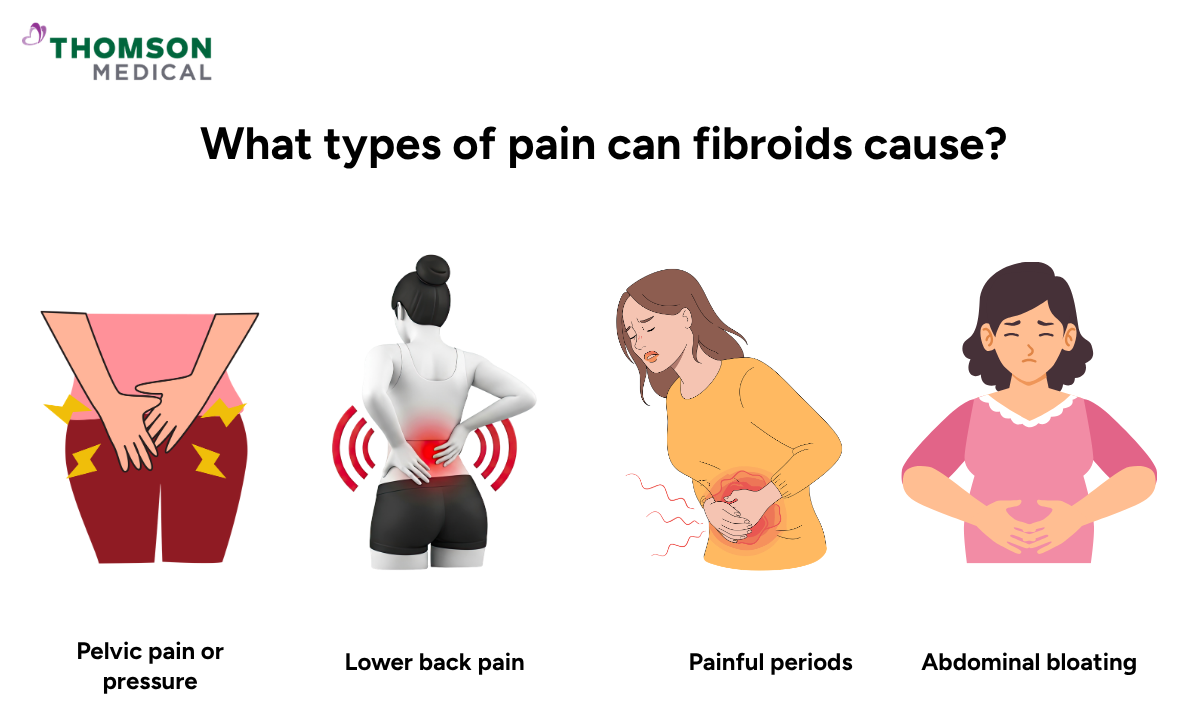
The type of pain fibroids cause depends largely on where they are growing and which nearby areas they are pressing against.
Pelvic pain or pressure
This is one of the most common experiences for women with fibroids.
When fibroids press against pelvic organs, you may notice:
A feeling of heaviness or fullness in the lower abdomen
A dull, aching pain that lingers
Discomfort when sitting or standing for long periods
This kind of pressure can be easy to dismiss as general bloating, so it is worth paying attention if it keeps coming back.
Lower back pain
If a fibroid sits at the back of the uterus, it may contribute to hip, leg, or lower back pain by creating pressure in the pelvis. This can show up as persistent pain without an obvious cause, or pain that spreads into your hips or legs.
Lower back pain from fibroids is often mistaken for a muscular problem or poor posture. That is one reason it can take time to link it to a gynaecological cause.
Painful periods
Fibroids can make your periods more painful than they used to be. They may increase uterine contractions and lead to heavier, longer bleeding. If your menstrual cramps have worsened over time and no longer feel like your usual discomfort, fibroids may be contributing to the change.
Pain during sexual intercourse
Some women experience deep pelvic pain during intercourse, which can feel distressing and have an impact on your daily life and relationships. This may happen when fibroids distort the shape of the uterus or press on the cervix.
Abdominal bloating or swelling
Larger fibroids can cause visible swelling in the lower abdomen.
Alongside that, you might notice:
A sensation of pressure or fullness, similar to trapped wind
Difficulty getting comfortable when bending or trying to sleep
Bloating from fibroids is different from bloating caused by diet or digestion. It tends to stay for longer and does not ease after a bowel movement or change with what you eat.
These pain patterns can overlap, and it is not unusual to experience more than one at the same time. If several of these occur together and begin to affect your daily comfort or quality of life, it may be worth getting an assessment.
When pain patterns change or become more frequent, it is worth getting checked. Request an appointment with Thomson Medical to understand what is causing your symptoms and the next steps for care.
How is fibroid pain diagnosed?
Because fibroid pain can overlap with symptoms from other conditions, your doctor will use a combination of examination and imaging to get a clearer picture of what is causing your symptoms.
The process is usually straightforward, and your doctor will guide you through each step.
They may suggest one or more of the following:
A detailed conversation about your symptoms and medical history
A pelvic examination
A transvaginal or pelvic ultrasound
An MRI scan for a more detailed look at fibroid size and location
Blood tests to check for anaemia, which can develop if you have heavy periods
Your doctor may also consider other causes of pelvic pain, such as endometriosis, adenomyosis, ovarian cysts, pelvic infection, urinary conditions, or bowel conditions.
In some cases, fibroids are found while looking into an unrelated symptom. If this happens to you, your doctor can help work out whether they might be linked to any pain or discomfort you have been feeling.
Treatment options for fibroid pain
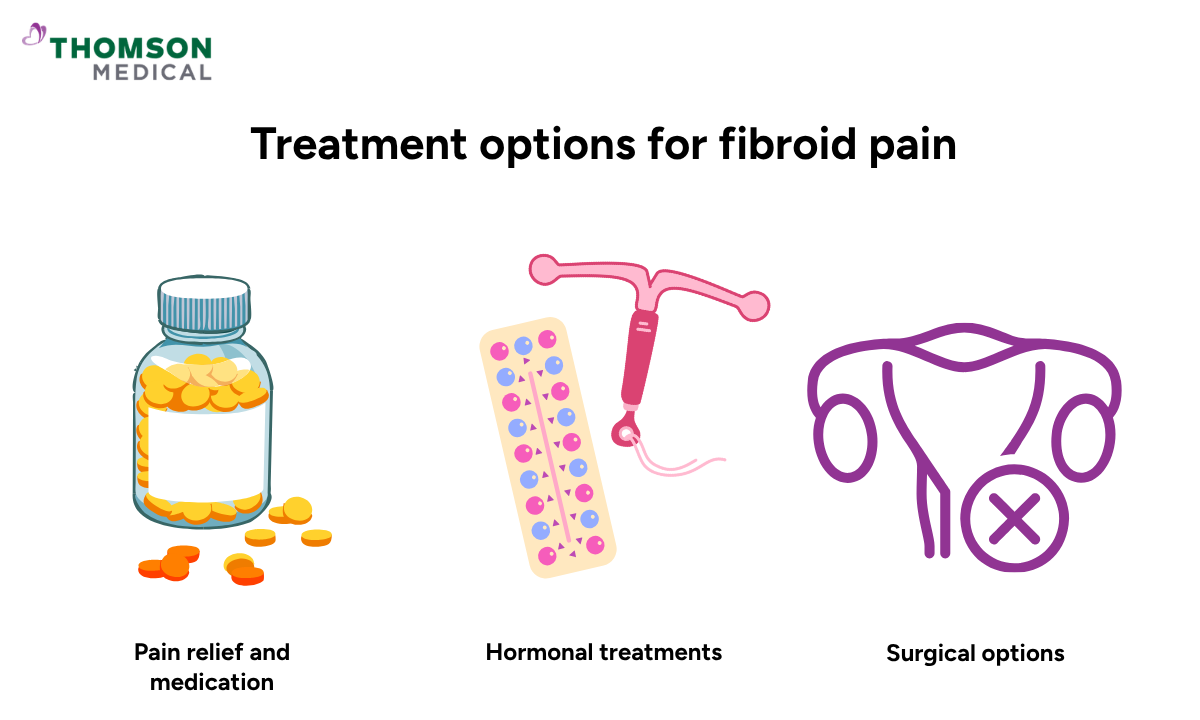
There are several ways to manage fibroid pain, ranging from simple pain relief to procedures that reduce or remove fibroids entirely. The right approach for you will depend on your symptoms, your age, and whether you are planning a future pregnancy.
Pain relief and medication
Medication is usually the first step, particularly when symptoms are manageable and a procedure is not yet needed.
Your doctor may recommend starting with:
Anti-inflammatory medicines such as ibuprofen or naproxen may help ease period pain. If heavy bleeding is also present, your doctor may discuss treatments such as tranexamic acid or hormonal options.
Paracetamol for milder pain that does not need stronger relief
Iron supplements if heavy periods have led to anaemia
These options help manage symptoms and reduce discomfort, but they do not shrink your fibroids or treat the underlying cause.
If pain continues despite medication, or if your symptoms seem to be getting worse, it may be worth speaking to your doctor again to discuss whether a more targeted treatment is appropriate.
Hormonal treatments
Hormonal treatments may help reduce heavy bleeding and menstrual pain. Some treatments, such as GnRH agonists, can temporarily shrink fibroids, but other hormonal options mainly help control symptoms.
Your doctor may discuss:
The contraceptive pill, which can help regulate the hormones that drive the menstrual cycle. By doing so, it may reduce the heaviness and duration of periods, making symptoms more manageable
An intrauterine device (IUD) that slowly releases the hormone progestogen
GnRH agonists (a type of hormone-regulating medication), which temporarily lower oestrogen levels and can help shrink fibroids before other treatments
The length of treatment will depend on your symptoms and how your body responds.
Minimally invasive procedures
If medication alone is not giving you enough relief, there are procedures that can reduce fibroids while keeping your uterus intact.
These include:
Uterine artery embolisation (UAE):
A procedure that blocks the blood supply to fibroids by injecting tiny particles into the arteries that feed them, causing the fibroids to shrink over time.
MRI-guided focused ultrasound:
Uses precisely directed sound waves, guided by an MRI scan, to heat and reduce fibroid tissue, without the need for surgery.
Radiofrequency ablation:
A minimally invasive procedure that uses controlled heat energy delivered through a small probe to break down fibroid tissue from within.
These procedures tend to have shorter recovery times than surgery. However, there is a chance fibroids may return afterwards, particularly in younger women who are still in their reproductive years.
Surgical options
For more significant cases, surgery may be the most appropriate option.
Your doctor might recommend:
Myomectomy:
Myomectomy surgery removes fibroids while leaving the uterus in place. This is often preferred for women who wish to preserve their fertility.
Hysterectomy:
Hysterectomy surgery involves the removal of the uterus and is the only option that ensures fibroids do not return.
It is usually considered when other treatments have not provided enough relief and you are not planning a future pregnancy.
The type of surgery will affect how long recovery takes. Your surgical team will discuss what to expect based on your individual circumstances.
When should fibroid pain concern you?
Some fibroid pain is manageable day to day, but certain symptoms are a sign that you should see your doctor sooner rather than later.
Speak to your doctor if you notice any of the following:
Sudden or severe pelvic pain
Pain that is steadily getting worse over time
Heavy bleeding alongside your pain
Pain accompanied by fever or vomiting
Symptoms that are disrupting your daily life
These symptoms do not always point to something serious, but they are worth taking seriously. Seeing your doctor early means any changes can be picked up and addressed sooner.
If your symptoms are affecting your daily life or you are unsure what is causing them, you can request an appointment with Thomson Medical. Our specialists can help you understand what is going on and guide you toward the right next steps.
FAQ
Can small fibroids cause pain?
Yes. Smaller fibroids are less likely to cause pressure-related pain, but they may still cause symptoms depending on their location, especially if they affect the uterine cavity.
Does fibroid pain get worse over time?
It can. Pain may worsen if fibroids grow or increase in number, and hormonal changes can also influence the severity of symptoms.
Can fibroid pain come and go?
Yes, fibroid pain can be intermittent. It may become more noticeable during menstruation or ovulation and ease at other times.
How do I know if my pain is caused by fibroids?
Imaging tests such as ultrasound or MRI are needed to confirm whether fibroids are the cause of your pain and to assess their size and location.
Can fibroid pain affect daily activities?
Yes. Ongoing pain can interfere with daily life, including work, sleep, exercise, and sexual activity.
Will fibroid pain go away after menopause?
In many cases, yes. Fibroids often shrink after menopause due to lower hormone levels, which can lead to symptom relief.
Is sudden severe pain from fibroids an emergency?
Yes. Sudden and intense pain may indicate complications such as fibroid degeneration or torsion and should be evaluated promptly by your doctor.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
