Many women only find out they have fibroids by accident, picked up during a routine ultrasound or a scan for something else entirely. Others discover them only after years of heavy periods or pelvic discomfort.
So how do doctors confirm whether fibroids are behind your symptoms? The diagnostic process involves more than a single test, and the right approach often depends on where the fibroids are located, their size, and the symptoms you're experiencing.
What are fibroids?
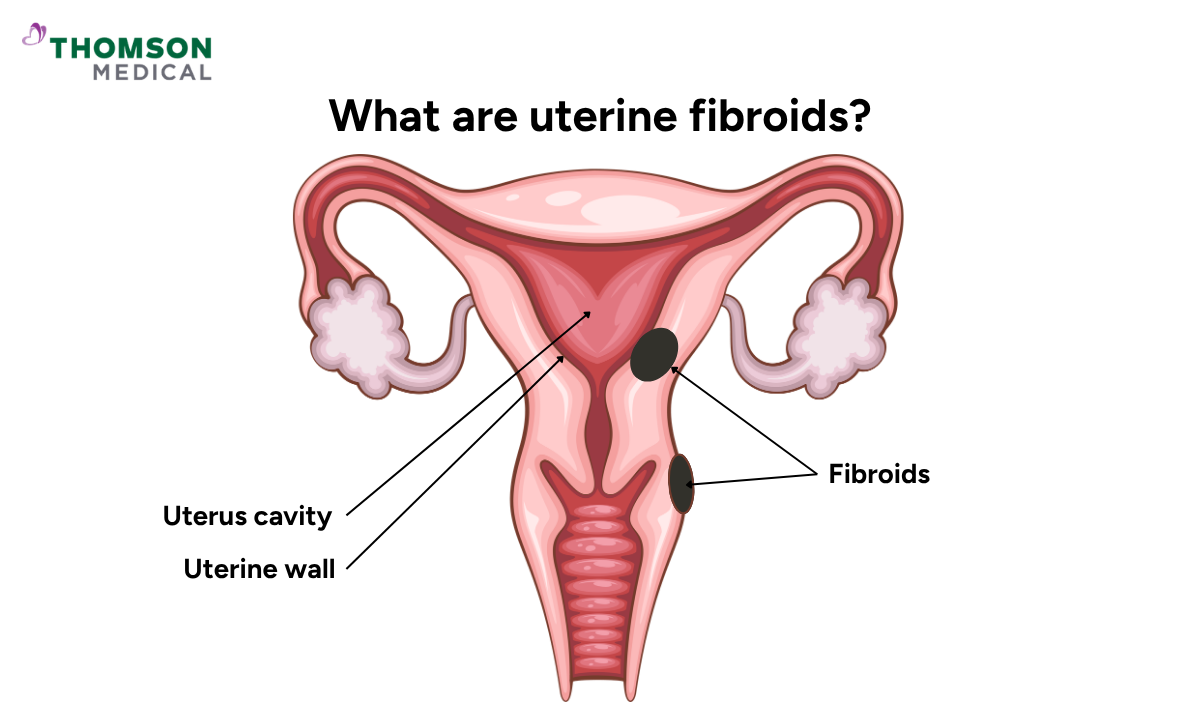
Uterine fibroids are usually benign (non-cancerous) growths that develop within the muscular wall of your uterus, on its lining, or on its outer surface. They are made up of muscle and fibrous tissue and can vary in size, number, and location.
Many women with fibroids have no symptoms and may only discover them during a routine check or scan. When symptoms do occur, they depend on where the fibroids are located and how they affect nearby organs.
What symptoms might lead to a fibroid diagnosis?
Fibroids do not always cause symptoms. Some women live with them for years without any noticeable signs. For others, a gradual change in how their body feels is often the first clue.
You may notice:
Heavy menstrual bleeding or periods lasting longer than usual
Pelvic pain or a feeling of pelvic pressure, heaviness, or a dull ache in your lower abdomen
Needing to urinate more often than usual
Bloating or constipation
Discomfort or pain during sexual intercourse
Lower back pain that does not settle with rest
In some cases, fibroids are first identified during investigations for fertility concerns or repeated pregnancy loss, even when no other symptoms are present. In other situations, they are found by chance during a routine pelvic exam or an unrelated scan.
If you've noticed changes in your cycle or persistent pelvic discomfort, request an appointment with Thomson Medical. Our specialist can help you understand whether further investigation may be useful.
How are fibroids diagnosed?
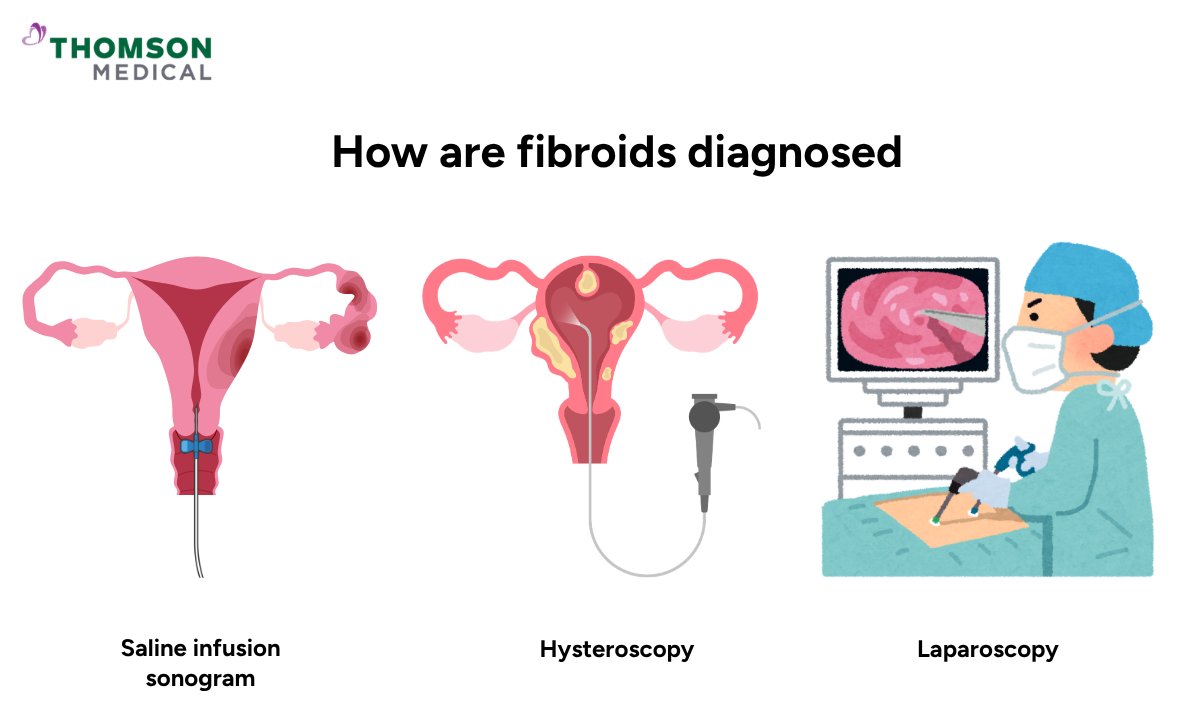
Your doctor will usually begin with a physical examination to check whether your uterus feels enlarged or irregular. If further investigation is needed, one or more tests will be recommended to better understand the size, number, and position of your fibroids.
Ultrasound scan
An ultrasound scan is usually the first test used to look for fibroids and rule out other possible causes of your symptoms. It uses sound waves to create images of your uterus.
You may have:
A transabdominal ultrasound, where a probe is moved gently over your abdomen
A transvaginal ultrasound, where a probe is gently inserted into the vagina for a closer view
The type of ultrasound used depends on what your doctor needs to assess. In some cases, both are performed during the same visit to get a clearer evaluation.
Saline infusion sonogram
This is a more detailed type of ultrasound. A small amount of sterile saline fluid is gently introduced into the uterus to help improve the clarity of the images. It is especially useful for detecting fibroids that grow just inside the uterine cavity, which can be harder to see on a standard scan.
Magnetic resonance imaging (MRI) scan
An MRI scan uses strong magnetic fields and radio waves to produce detailed images of your uterus and does not involve radiation.
It is usually recommended when a more detailed view is needed, such as when there are multiple fibroids or when surgery is being planned. It helps your doctor map the fibroid size, number, and position of fibroids more precisely.
Hysteroscopy
A hysteroscopy involves passing a thin camera through the vagina and cervix into the uterus so your doctor can view the inside of the uterine cavity directly. It is particularly useful for fibroids that grow into the cavity. In some cases, small fibroids can be removed during the same procedure.
Laparoscopy
A laparoscopy is a minor surgical procedure carried out under general anaesthetic. A small camera is inserted through a tiny cut in the abdomen, allowing your doctor to view the outside of the uterus and surrounding organs.
It is usually recommended when other scans have not provided enough information or when outer wall fibroids are suspected.
Biopsy
A biopsy involves taking a small tissue sample for testing. It is rarely needed for fibroids and is usually only considered if a fibroid has unusual features or if your doctor needs to rule out other conditions.
This is because a biopsy does not usually confirm fibroids themselves. However, it may be used to rule out other conditions when symptoms or imaging findings are unusual. For most women, it is not part of the diagnostic process.
Not every test on this list will be needed. Your doctor will start with the least invasive option and progress to more detailed investigations only if more information is needed.
Our gynaecologists
Loading...
How to prepare for your appointment
Your doctor will ask about your symptoms, menstrual cycle, and medical history. Having this information ready before you arrive saves time and helps the conversation stay focused.
Before your visit, it helps to:
Track your symptoms including how heavy your menstrual bleeding is, how long it lasts, and any pain or pressure you feel
Note any other changes, such as needing to urinate more often, bowel changes, or discomfort during sex
List your medications and supplements, including anything you take regularly
Bring your medical history, including any previous gynaecological conditions, surgeries, or imaging results
Note your family history and let your doctor know if close relatives have had fibroids
It also helps to write down any questions beforehand. Many women leave an appointment and realise there was something else they meant to ask.
How doctors identify the type and location of fibroids
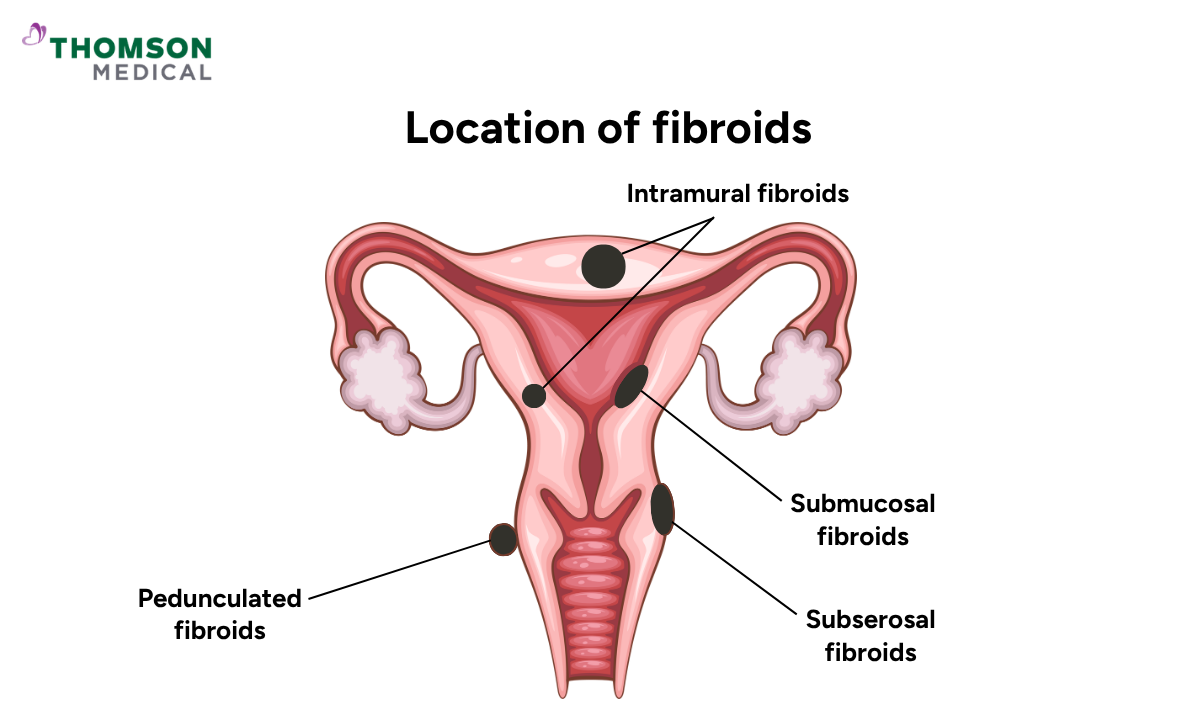
Not all fibroids are the same, and where yours are located can influence how they affect you and what treatment may be considered. Your doctor will use your test results to determine the position and characteristics of your fibroids.
Fibroids are categorised by where they grow:
Submucosal fibroids, which grow inside the uterine cavity
Intramural fibroids, which grow within the muscular wall of the uterus
Subserosal fibroids, which grow on the outer surface of the uterus
Pedunculated fibroids, which are attached to the uterus by a stalk, either inside or outside
Pedunculated fibroids have one risk worth being aware of. If the stalk twists, it can cause sudden severe pain and needs prompt medical attention.
What happens after a diagnosis?
A fibroid diagnosis does not automatically mean you need treatment. Many fibroids are small, cause no significant problems, and need only occasional monitoring.
The options your doctor may discuss with you include:
Regular monitoring with occasional scans if your fibroids are small and not causing symptoms
Medication to help manage heavy menstrual bleeding or to temporarily reduce the size of fibroids before further treatment
Procedures or surgery such as myomectomy, uterine artery embolisation, or hysterectomy for more significant cases
For women who are planning a pregnancy, the timing of any treatment matters. Your doctor will take your fertility goals into account when discussing the options that may suit you best.
A diagnosis, where needed, is simply the first step towards understanding your body. Request an appointment with Thomson Medical to have a conversation with our specialist who can guide you through the appropriate next steps.
FAQ
Do I need a referral to see a specialist for suspected fibroids in Singapore?
It depends on how you access care. In the public system, a doctor referral is usually required before seeing a gynaecologist. Through a private clinic or hospital, you can generally book directly with a specialist.
How long does it usually take to get a fibroid diagnosis?
It varies. If an ultrasound scan gives a clear picture, a diagnosis may be confirmed within one or two appointments. If further tests such as an MRI scan or hysteroscopy are needed, the process may take a few weeks longer.
Is a fibroid ultrasound scan painful or uncomfortable?
A transabdominal ultrasound is generally painless. A transvaginal ultrasound may feel slightly uncomfortable but should not be painful. A saline infusion sonogram may cause mild cramping when the fluid is introduced, similar to period pain, though this usually passes quickly.
Can fibroids be missed on a scan?
Yes, particularly small or awkwardly positioned ones. A saline infusion sonogram or MRI scan provides greater detail and is less likely to miss what a standard ultrasound may not clearly show.
Can ultrasound detect fibroids, or do I need an MRI?
For most women, an ultrasound scan is sufficient. An MRI scan is usually only needed when more detail is required, such as when fibroid size or location needs to be mapped precisely before surgery or when MRI-guided focused ultrasound surgery is being considered.
Can fibroids be found during a routine gynaecological check-up?
Yes. Fibroids are sometimes discovered by chance during a routine pelvic examination if the uterus feels enlarged or irregular. They may also be picked up incidentally during an ultrasound scan arranged for another reason.
What medications are available to manage fibroid symptoms without surgery?
Several medications can help manage symptoms without the need for surgery. Your doctor will recommend the most suitable option based on your symptoms and whether you are planning a pregnancy.
- Tranexamic acid helps reduce heavy period bleeding by encouraging the blood to clot more effectively during your cycle
- Non-steroidal anti-inflammatory drugs such as ibuprofen are commonly used to relieve pelvic pain and cramping
- Hormone therapy may help reduce heavy menstrual bleeding or manage symptoms, depending on the patient’s suitability and fertility plans.
- GnRH agonists temporarily lower oestrogen levels, which can cause fibroids to shrink ahead of surgery
- Other hormonal medicines may be considered in selected cases, depending on local availability, safety considerations and your doctor’s assessment.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
