That burning sensation when you urinate, the constant urge to go even when your bladder feels empty, and the cloudy or strong-smelling urine – these symptoms can be uncomfortable and worrying, especially if it's your first time experiencing them.
If these signs sound familiar, you may be dealing with a urinary tract infection (UTI). Getting prompt treatment can quickly clear the infection and prevent it from spreading to your kidneys, where it can lead to more serious complications.
What is urinary tract infection (UTI)?
A UTI happens when bacteria travel into your urinary system and start to multiply, which is what triggers that uncomfortable burning and urgency you may be feeling. UTIs can affect different parts of the urinary tract, resulting in various symptoms and severity.
Anatomy of the urinary tract
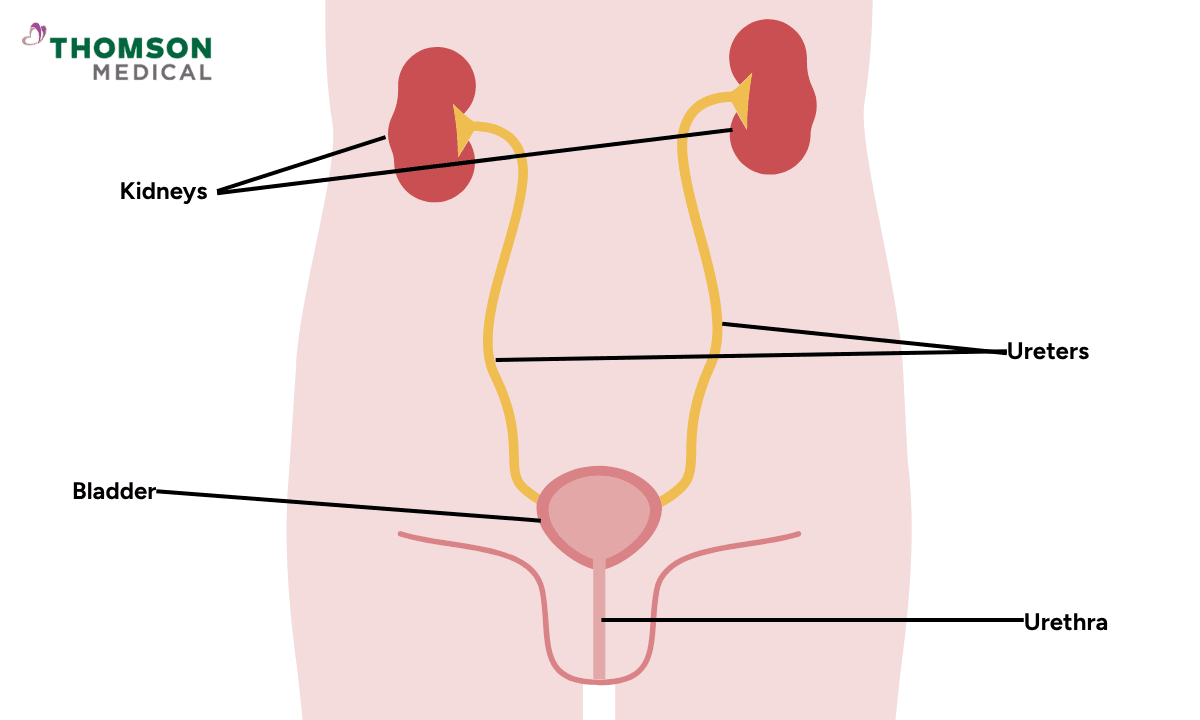
Your urinary tract is made up of four parts: your kidneys (which filter your blood and make urine), your ureters (the tubes that carry urine down to your bladder), your bladder (where urine is stored), and your urethra (the short tube that lets urine leave your body). A UTI can happen anywhere along this pathway, though it most often starts in the bladder.
Kidneys
Bean-shaped organs located in the upper abdominal cavity, one on each side of the spine.
Filter blood to remove waste products and excess substances, producing urine.
Each kidney contains millions of functional units called nephrons, which consist of renal tubules and glomeruli.
Ureters
Narrow, muscular tubes connecting each kidney to the bladder.
Their role is to transport urine from the kidneys to the bladder through peristaltic contractions of smooth muscle in the ureter walls.
Bladder
Hollow, muscular organ located in the lower pelvis, behind the pubic bone.
Stores urine until it is voluntarily expelled during urination.
Can expand and contract to accommodate varying volumes of urine.
Urethra
Thin tube extending from the bladder to the exterior of the body.
In males, it also serves as a passage for semen during ejaculation.
Urethral sphincter muscles help control the flow of urine.
What causes UTIs?
UTIs are usually caused when bacteria enter your urinary tract through the urethra.
Most UTIs are caused by bacteria, with Escherichia coli (E. coli) being the most common culprit. Other bacteria that can cause UTIs include Klebsiella, Proteus, Enterococcus, and Staphylococcus species.
Women have a shorter urethra than men, which is why women have a higher risk of getting a UTI.
Things that increase the risk of bacteria getting into the bladder include:
Pregnancy
Wiping from back to front after using the toilet
Conditions that block the urinary tract, such as kidney stones
Conditions that make it difficult to fully empty the bladder, such as an enlarged prostate in men and constipation in children
Urinary catheters (a tube in your bladder used to drain urine)
Having a weakened immune system (for example, if you have poorly controlled diabetes or you are having chemotherapy)
Using spermicide with contraception
Not drinking enough fluids
UTI symptoms: what you may notice
Common symptoms of UTIs include:
Frequent urination
Pain or burning sensation during urination (dysuria)
Urgency to urinate
Cloudy or foul-smelling urine
Blood in the urine (haematuria)
Pelvic or lower abdominal discomfort
Fever and chills (in cases of pyelonephritis)
If left untreated, UTIs can lead to complications such as:
Kidney damage or infection (pyelonephritis)
Sepsis (life-threatening systemic infection)
Preterm birth or low birth weight (in pregnant women)
Increased risk of UTI-related hospitalisations and mortality in older adults
Types of UTIs
Lower UTI (Cystitis and urethritis)
Infections of the bladder (cystitis) and urethra (urethritis).
Symptoms include frequent urination, pain or burning during urination, and cloudy or bloody urine.
Upper UTI (Pyelonephritis)
Infections of the kidneys, which are more serious.
Symptoms include fever, chills, flank pain, nausea, and vomiting.
Ureteritis
Inflammation of the ureter, which is rare and often associated with cystitis or pyelonephritis.
Who is at risk of UTIs?
Several factors can increase the risk of developing UTIs, including:
Being female (shorter urethra)
Pregnancy
Menopause
Urinary catheterisation
Urinary tract abnormalities or obstructions
Conditions that weaken the immune system (e.g., diabetes, HIV/AIDS)
If you have concerns about urinary tract infections or need more information, schedule an appointment with Thomson Medical to get tested.
Our urologists in Singapore
Loading...
How UTIs are diagnosed
Examination of a urine sample to detect signs of infection, such as the presence of white blood cells, red blood cells, or bacteria.
Urine culture
Identifies the specific bacteria causing the infection and determines the most effective antibiotic treatment.
Imaging studies
In cases of complicated or recurrent UTIs, imaging studies such as ultrasound, CT scan, or MRI may be recommended to evaluate the urinary tract for abnormalities or obstructions.
How UTIs are treated
If you've been diagnosed with a UTI, the good news is that most infections respond well to treatment, and many women start to feel noticeably better within a few days of starting the right medication.
Most UTIs are treated with a short course of antibiotics. Your doctor will choose the most suitable one for you based on a few things – the type of bacteria involved (often identified through a urine test); whether the infection is in your bladder or has reached your kidneys; any allergies you have; and whether you're pregnant or taking other medications.
For a straightforward infection, a course may last around three to seven days. More complicated infections, or those affecting the kidneys, often need a longer course and sometimes stronger antibiotics. Symptoms like burning and urgency usually begin to ease within the first day or two, though this can vary from person to person.
Why finishing your full course matters
It can be tempting to stop taking your antibiotics once you start feeling better, but finishing the full course is important, even if your symptoms have cleared.
Stopping early can:
Allow some bacteria to survive and cause the infection to return
Lead to a more stubborn infection that's harder to treat next time
Contribute to antibiotic resistance, which affects how well these medicines work for you and others in the future
Take every dose as prescribed, at roughly the same times each day, and try not to skip any. If you experience side effects that concern you, speak with your doctor before stopping to discuss alternative measures.
Recurrent UTIs
Recurrent UTIs – which are two or more infections in six months, or three or more in a year – can feel exhausting, frustrating, and sometimes isolating. If this is your experience, please know you're not alone, and there are options that can help.
Your doctor may suggest:
A longer review of possible triggers, including sexual activity, contraception methods (particularly spermicides), hydration habits, and any other medical conditions
Low-dose preventive antibiotics taken daily or after intercourse, depending on the pattern of your infections
Vaginal oestrogen therapy for women going through perimenopause or menopause, as lower oestrogen levels can make the urinary tract more vulnerable to infection
Further investigation to rule out underlying causes, such as kidney stones or anatomical factors
Lifestyle and self-care strategies tailored to your situation
Recurrent UTIs are not something you simply have to live with. A thoughtful conversation with your doctor can help you understand what's driving the pattern and put a plan in place that fits your life.
How to prevent UTIs?
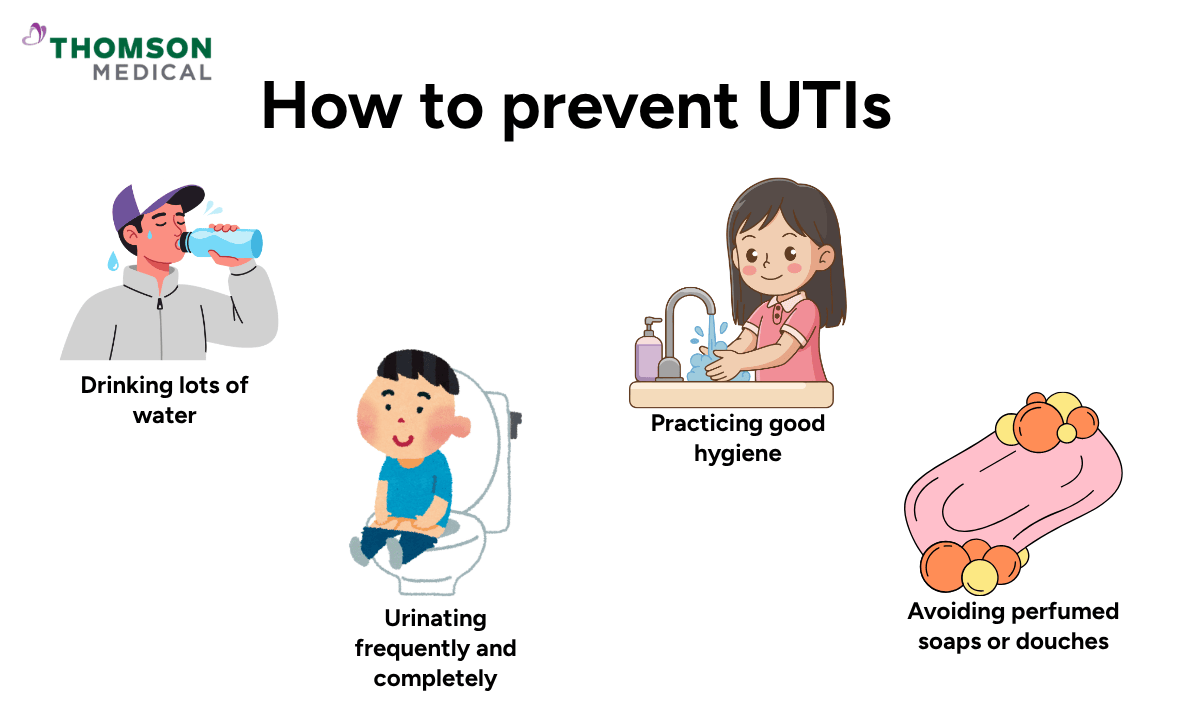
There are several simple, everyday steps that can help lower your risk of UTIs, including:
Drinking plenty of water to stay hydrated
Urinating frequently and completely
Wiping from front to back after using the bathroom
Avoiding irritating substances such as perfumed soaps or douches
Practising good hygiene, especially before and after sexual activity
Emptying the bladder soon after sexual intercourse
Using cranberry products, juice, or supplements (evidence for effectiveness is mixed)
Alternative and complementary therapies for UTIs
Some individuals may explore alternative or complementary therapies for UTI prevention or management.
These alternate treatments may include:
Probiotics
Certain strains of beneficial bacteria may help maintain a healthy balance of vaginal and urinary tract flora.
Cranberry products
While evidence for their effectiveness is mixed, some studies suggest that cranberry products may help prevent UTIs by inhibiting bacterial adhesion to the urinary tract lining.
Herbal remedies
Herbs such as uva-ursi, d-mannose, and goldenseal are sometimes used for UTI prevention or treatment, although their efficacy and safety require further research.
When should you see a doctor?
You should see a doctor once you notice common UTI symptoms such as burning pain or blood in urine, especially if they persist or worsen.
While UTIs can usually be managed with the right treatments, you should seek out urgent care if you experience any of the following:
Symptoms do not improve within 24-48 hours of starting antibiotics.
You have fever, chills, blood in your urine, or back/side pain (signs of a possible kidney infection)
You are currently pregnant (an untreated infection can cause complications for both mother and baby)
You have an underlying health condition such as diabetes, which could increase the risk of complications
If you have concerns about urinary tract infections or need more information, schedule an appointment with Thomson Medical. Our team is here to assist you with any questions and provide the support you need.
FAQs
What are the main causes of UTI?
Urinary tract infections (UTIs) are primarily caused by bacteria, most commonly E. coli, entering the urinary tract through the urethra and multiplying in the bladder. This can be caused by bacteria spreading from the anus/vagina, sexual activity, poor hygiene, or urinary retention.
What is the fastest way to get rid of a urinary tract infection?
The most effective approach is to see a doctor for an assessment. If a UTI is confirmed, a short course of antibiotics is usually prescribed, and most women notice their symptoms easing within a few days. Staying well-hydrated and using over-the-counter pain relief can help you feel more comfortable in the meantime.
Can you cure a urinary tract infection without going to the doctor?
While home remedies like water, cranberry juice, and heating pads can help manage symptoms, they usually do not cure the infection. While mild UTIs can sometimes clear up on their own, it is not recommended to treat them without medical advice, as untreated UTIs can lead to severe kidney infections.
How long does a UTI usually last?
A UTI usually lasts for about a week, with symptoms improving within 1 to 2 days of taking antibiotics. With the right antibiotic, many women start feeling better within a few days, though recovery times vary depending on individual circumstances. Those with weakened immune systems, diabetes, or pregnancies may take longer to recover.
What foods should I avoid with a UTI?
The main things you want to avoid are foods that are high in sugar or may cause bladder irritation. These include:
Caffeine and alcohol
Citrus fruits (orange, lemons, grapefruit, etc.)
Spicy foods
Sugar and artificial sweeteners
Carbonated beverages (sodas or sparkling drinks)
What are three symptoms of a UTI?
The three most common symptoms of a UTI include:
A strong, persistent urge to urinate
A burning sensation when urinating (dysuria)
Urine with a dark colour (may indicate blood) and a strong odour
The information provided is for general guidance only and should not be considered as medical advice. For a personalised consultation and tailored advice, schedule an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
