That uncomfortable itch, the unusual discharge, the burning when you pee – if these symptoms sound familiar, you're likely dealing with a vaginal yeast infection. It's one of the most common conditions affecting women, and most of us will experience it at least once in our lives.
While the symptoms can feel distressing and even a little embarrassing, knowing what's actually happening in your body and how to treat it can help you find relief and prevent it from coming back.
What is a vaginal yeast infection?

A vaginal yeast infection is a fungal infection caused by an overgrowth of yeast organisms, most commonly Candida albicans, in the vaginal area. While Candida species are naturally present in the vagina, an overgrowth can cause an imbalance and lead to infection.
These yeast organisms thrive in warm, moist environments, such as the vaginal area, especially when conditions favour their growth. Vaginal yeast infections are very common, and most women will experience at least one episode in their lifetime.
What are the signs and symptoms of vaginal yeast infection?
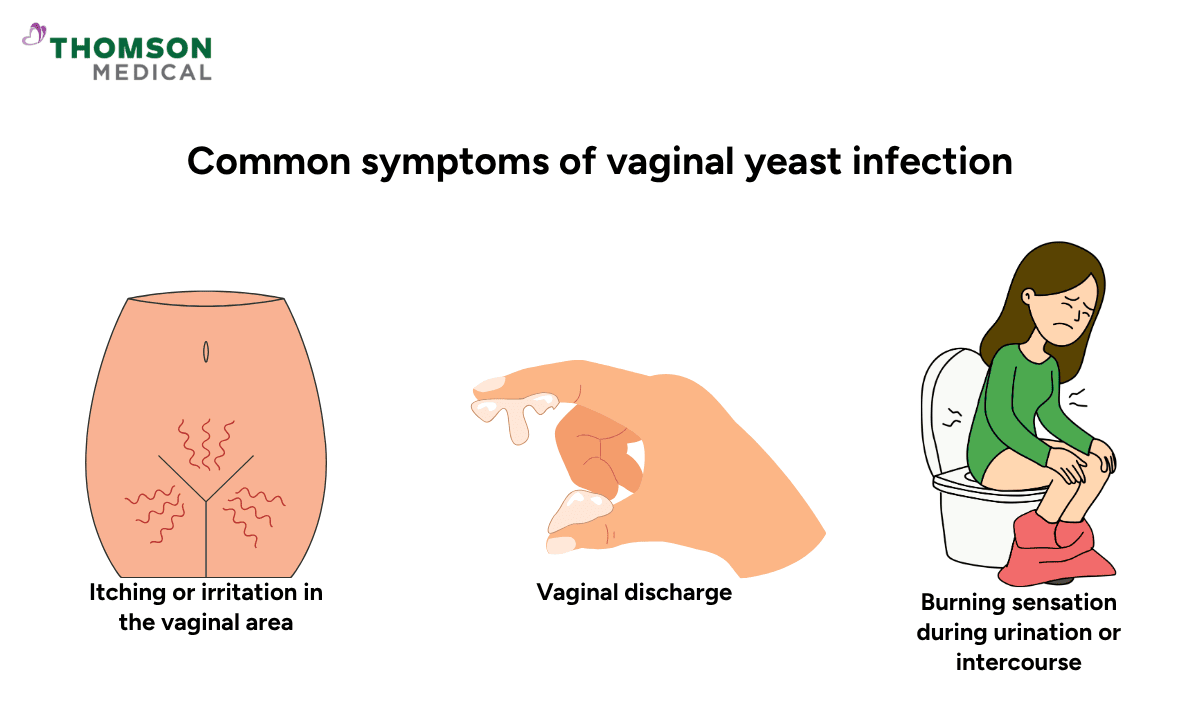
Common symptoms can range from mild to moderate and may include:
Itching or irritation in the vaginal area
Vulvar redness and swelling (vulvovaginal inflammation)
Vaginal discharge that usually appears thick and white
Burning sensation during urination or intercourse
Soreness or discomfort in the vaginal area
If you are unsure whether your symptoms are caused by a yeast infection or if symptoms persist despite treatment, schedule an appointment with Thomson Medical to help clarify the cause and seek appropriate care.
Who is at risk of vaginal yeast infection?
Several factors may increase the risk of developing vaginal yeast infections, including:
Antibiotic use
Antibiotic use can disrupt the normal balance of bacteria in the body, including in the vagina. They may kill beneficial bacteria that help keep yeast levels in check, allowing yeast to proliferate and cause an infection.
Hormonal changes
Hormonal changes that occur during pregnancy, menstruation, or use of oral contraceptives can alter the vaginal environment and make it more conducive to yeast growth. Pregnancy hormones, in particular, can increase vaginal glycogen levels, providing a food source for yeast.
Medical conditions
Conditions like diabetes that weaken the immune system can make individuals more susceptible to infections, including vaginal yeast infections.
Sexual activity
Sexual activities, particularly with a new partner or multiple partners, can disrupt the vaginal microbiota and increase the risk of yeast overgrowth.
Medications
Use of medications such as corticosteroids or immunosuppressants can weaken the immune system and lead to increased risk of infections.
Poor personal hygiene
Practices such as wearing tight-fitting, non-breathable clothing, staying in wet or damp clothing for extended periods, or using harsh soaps or douches in the vaginal area can disrupt the natural balance of vaginal flora and promote yeast growth.
Types of vaginal yeast infections
Uncomplicated yeast infections
These refer to mild to moderate yeast infections that occur sporadically and typically respond well to treatment. It typically occurs in people with a prior confirmed diagnosis and classic symptoms.
Recurrent yeast infections
Recurrent yeast infections are characterised by three or more episodes within a year and may require longer or maintenance treatment to prevent recurrence.
How to diagnose vaginal yeast infections?
Your healthcare provider may perform the following steps to provide a diagnosis:
Clinical examination
Perform a pelvic examination to assess the appearance of the vaginal discharge and evaluate for signs of inflammation or infection.
Vaginal pH testing
Yeast infections typically do not alter vaginal pH, which is usually acidic (pH < 4.5).
Microscopic examination
Microscopic examination of vaginal discharge samples may reveal the presence of yeast cells and pseudohyphae, characteristic of Candida infection.
Our gynaecologists in Singapore
Loading...
How to treat a vaginal yeast infection?
Treatment for vaginal yeast infections typically involves antifungal medications to eliminate the overgrowth of yeast and relieve symptoms. Your treatment options will depend on factors such as uncomplicated vs recurrent disease and on pregnancy status and local resistance patterns.
Commonly prescribed fungal treatments for yeast infections include:
Over-the-counter antifungal creams or suppositories:
For treatment of simple yeast infections, these medications are available without a prescription and include clotrimazole, miconazole, and tioconazole.
Prescription oral antifungal medications:
In cases of severe or recurrent yeast infections, healthcare providers may prescribe oral antifungal medications such as fluconazole.
How to prevent vaginal yeast infections?

To reduce the risk of vaginal yeast infections and prevent recurrence, individuals can take several preventive measures, including:
Avoiding unnecessary antibiotics
Only use antibiotics when necessary.
Good hygiene practices
Wear breathable cotton underwear, avoid tight clothing, and change out of wet clothes promptly.
Healthy lifestyle habits
Manage blood sugar levels, especially for those with diabetes, and reduce sugar intake.
Careful use of vaginal products
Avoid douching and use gentle, unscented products to maintain the natural balance of vaginal flora.
When should you see a doctor?

Most mild vaginal yeast infections settle within a few days of treatment with an over-the-counter antifungal cream or pessary. However, there are situations where speaking with a GP, O&G doctor, or community pharmacist is a good idea – both to confirm the diagnosis and to choose a treatment that suits your situation.
Consider seeking medical advice if any of the following apply:
It is your first suspected episode:
Symptoms of vaginal yeast infections (such as itching, burning, and changes in discharge) can also be caused by other conditions, including bacterial vaginosis or sexually transmitted infections (STIs). A clinical assessment helps confirm what is going on before starting treatment.
Your symptoms do not improve with an over-the-counter antifungal:
If discomfort persists despite treatment, or if symptoms return shortly after finishing the course, a healthcare provider can review whether the diagnosis is correct or whether a different antifungal may be more appropriate.
You experience recurrent vaginal yeast infections:
For example, having several episodes within a year. Recurrent infections may benefit from a longer course of treatment or maintenance therapy, and there may be underlying factors (such as poorly controlled diabetes) worth checking for.
You are pregnant:
Vaginal yeast infections during pregnancy are common and are usually not harmful, but some treatments are more suitable than others at different stages of pregnancy. Having your symptoms reviewed can help you choose an option that is appropriate for you.
You have diabetes, a weakened immune system, or are taking immunosuppressant medication:
In these situations, yeast infections can be more persistent or slower to clear, and a tailored treatment plan may be helpful.
Your symptoms are severe or unusual:
For example, intense pain, marked swelling, sores or blisters, fever, or lower abdominal or pelvic pain. These signs are not typical of a straightforward yeast infection and warrant prompt assessment to rule out other causes.
You notice unusual vaginal bleeding:
Particularly bleeding between periods or after intercourse.
You are concerned about a possible STI:
For example, after a change in sexual partner. Some STIs share symptoms with vaginal yeast infections, and testing can provide clarity and reassurance.
If you are unsure, there is no harm in seeking advice. A short consultation with a GP or O&G doctor can help clarify the cause of your symptoms, rule out other conditions, and guide you towards a treatment that suits your situation.
If you experience recurrent episodes, request an appointment with Thomson Medical to review possible underlying factors and discuss longer-term management options that may suit your situation.
FAQ
What are the complications of vaginal yeast infections?
While vaginal yeast infections are generally not associated with serious complications, untreated or recurrent infections may lead to:
Chronic or recurrent symptoms
Persistent or frequently occurring symptoms can affect quality of life.
Vulvovaginal candidiasis
More severe or extensive vulvovaginal inflammation (often termed complicated or more severe candidiasis).
Secondary bacterial infections
Scratching or excessive moisture in the vaginal area may lead to skin irritation or secondary bacterial infections.
What will happen if I get a vaginal yeast infection during pregnancy?
Experiencing a vaginal yeast infection during pregnancy is relatively common and usually does not pose a significant risk to the mother or the foetus. However, it's essential to manage the infection promptly to alleviate symptoms and prevent potential complications.
Here's what may happen if you get a vaginal yeast infection during pregnancy:
Increased discomfort
Symptoms of vaginal yeast infections like itching, irritation and abnormal vaginal discharge may be more pronounced during pregnancy due to hormonal changes and increased vaginal moisture.
No direct harm to the baby
Vaginal yeast infections generally do not directly harm the developing foetus. The infection is confined to the vaginal area and does not typically affect the baby in the womb.
Risk of complications
While vaginal yeast infections are usually harmless, untreated or recurrent infections may increase the risk of complications, such as:
Premature labour or preterm birth
Increased discomfort and impact on quality of life
Risk of neonatal candidiasis (thrush) in newborns if the infection is not adequately managed before delivery, though appropriate management of maternal symptoms before delivery may help
How long does a vaginal yeast infection take to clear up?
Most uncomplicated vaginal yeast infections begin to improve within a few days of starting antifungal treatment, with symptoms typically clearing up within about a week.
Over-the-counter antifungal creams or pessaries (such as those containing clotrimazole or miconazole) are available in different course lengths, ranging from a single dose to treatments used over several days. A short course of oral antifungal medication, such as fluconazole, may also be prescribed in some cases.
If your symptoms have not improved after about a week, return after finishing treatment, or worsen at any point, it is worth speaking with a GP or O&G doctor. Persistent symptoms may suggest that the diagnosis needs to be reviewed, that a different treatment is needed, or that there are underlying factors contributing to the infection.
Is vaginal yeast a sexually transmitted infection (STI)?
A vaginal yeast infection is not classified as a sexually transmitted infection. Small numbers of Candida yeast live naturally in the vagina, and an infection occurs when the usual balance of vaginal flora is disrupted and the yeast multiplies — not because the yeast has been "caught" from a partner.
That said, sexual activity can sometimes contribute to symptoms. Friction, changes to the vaginal environment, or activity with a new partner may upset the natural balance of vaginal flora and make a yeast infection more likely in some women.
In most cases, sexual partners do not need to be treated, although a partner who develops symptoms (such as itching or a rash) may benefit from speaking with a healthcare provider.
Because some sexually transmitted infections share symptoms with vaginal yeast infections, it is sensible to seek medical advice if you are unsure of the cause, particularly after a change in sexual partner.
What's the difference between a yeast infection and bacterial vaginosis?
Vaginal yeast infections and bacterial vaginosis (BV) are both common causes of vaginal discomfort and changes in discharge, but they are caused by different organisms and have different features.
A vaginal yeast infection is a fungal infection caused by an overgrowth of Candida yeast. It typically causes:
Itching and irritation in and around the vagina
A thick, white, often "cottage cheese-like" discharge that is usually not strong-smelling
Redness, soreness, and sometimes a burning sensation during urination or intercourse
Bacterial vaginosis, by contrast, is caused by an imbalance in the bacteria that normally live in the vagina, with a reduction in protective lactobacilli and an overgrowth of other bacteria. It typically causes:
A thin, greyish-white discharge
A distinctive "fishy" odour, which may be more noticeable after sex
Mild irritation, although many women have no symptoms at all
Treatment also differs: vaginal yeast infections respond to antifungal medication, whereas bacterial vaginosis is usually treated with antibiotics.
Because the two conditions can look similar at first glance (and sometimes occur together), a clinical assessment is often the most reliable way to tell them apart, especially if it is your first episode or if symptoms are unclear.
Can recurrent yeast infections be treated?
Yes, recurrent vaginal yeast infections can be treated, although they often require a different approach to single, uncomplicated episodes.
Recurrent vaginal yeast infections refer to repeated episodes occurring over the course of a year.
Management usually focuses on two areas:
A longer initial course of antifungal treatment to bring the current infection under control. This may involve antifungal creams or pessaries used over a longer period or several doses of an oral antifungal such as fluconazole, taken under medical guidance.
Maintenance therapy to reduce the chance of further episodes. This typically involves taking a low-dose antifungal regularly (for example, weekly) over several months. Your doctor will discuss whether this approach is suitable for you.
Alongside medication, a healthcare provider may also look for and address underlying factors that can contribute to recurrent vaginal yeast infections, such as poorly controlled blood sugar in diabetes, certain medications, or hormonal influences. Lifestyle measures – such as wearing breathable cotton underwear, avoiding douching, and changing out of damp clothing promptly – may also help reduce the risk of further episodes.
If you experience repeated vaginal yeast infections, it is worth speaking with a GP or O&G doctor rather than relying on over-the-counter treatments alone. A proper assessment can help confirm the diagnosis, identify contributing factors, and guide a treatment plan that suits your situation.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
