If you’ve been running to the toilet more often, feeling that familiar pressure in your lower abdomen, it’s easy to assume it is a bladder issue. The surprising part? Your bladder might not be the problem at all.
If treatments aimed at your bladder have not brought relief, the real cause may be sitting right next to it. Fibroids, which grow in and around the uterus, can press against the bladder and trigger symptoms that look exactly like a urinary condition.
Understanding the connection between fibroids and urinary symptoms can help you make sense of what you are experiencing and feel more prepared when speaking with your doctor.
What are uterine fibroids?
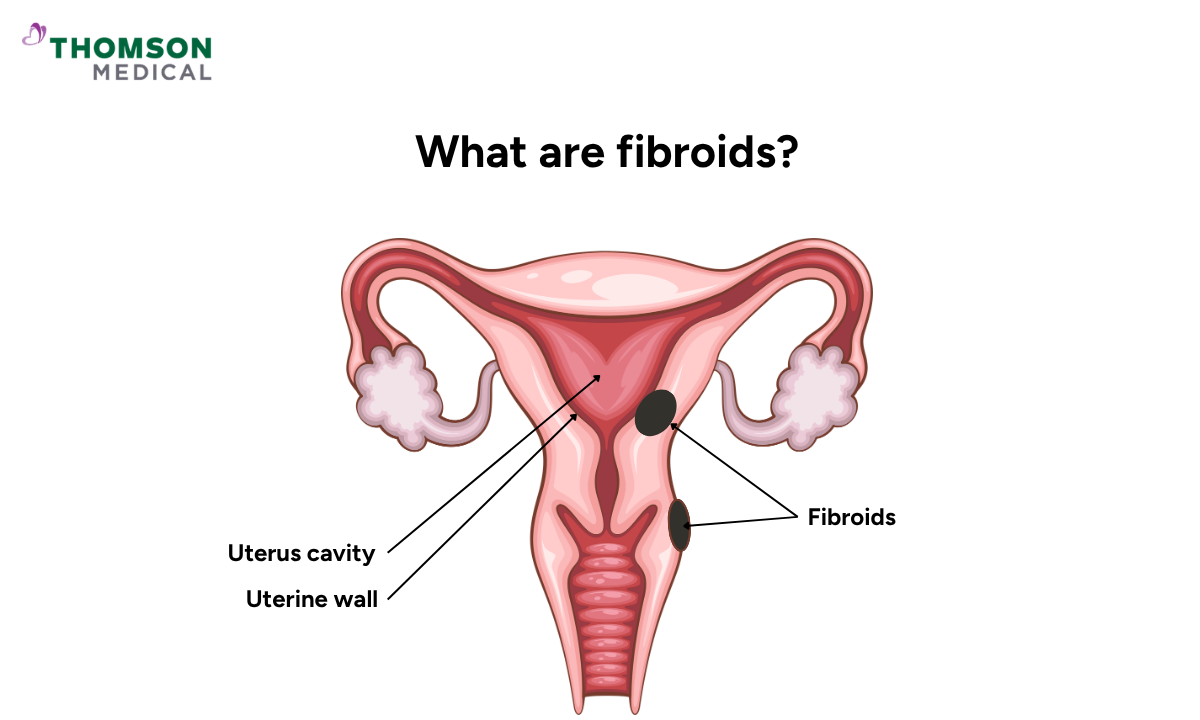
Uterine fibroids are non-cancerous growths that develop in the wall of the uterus. They are made up of muscle and fibrous tissue, and they vary in size.
Fibroids are very common in women of reproductive age, and some women have them without any symptoms at all.
You might experience:
Heavy menstrual bleeding or painful periods
Pelvic pain or pressure
Abdominal bloating or a feeling of fullness
Fertility issues, depending on the size and location of the fibroids
Your symptoms depend on the number, size, and position of your fibroids. This is why two women with fibroids can have very different experiences.
How fibroids can affect the bladder
The bladder and uterus sit very close together in the pelvic area. When fibroids grow large or develop near the front wall of the uterus, they can press directly against the bladder.
This pressure can:
Reduce the bladder's capacity to hold urine
Interfere with how the bladder fills and empties
Contributing to urinary frequency, urgency, or difficulty emptying
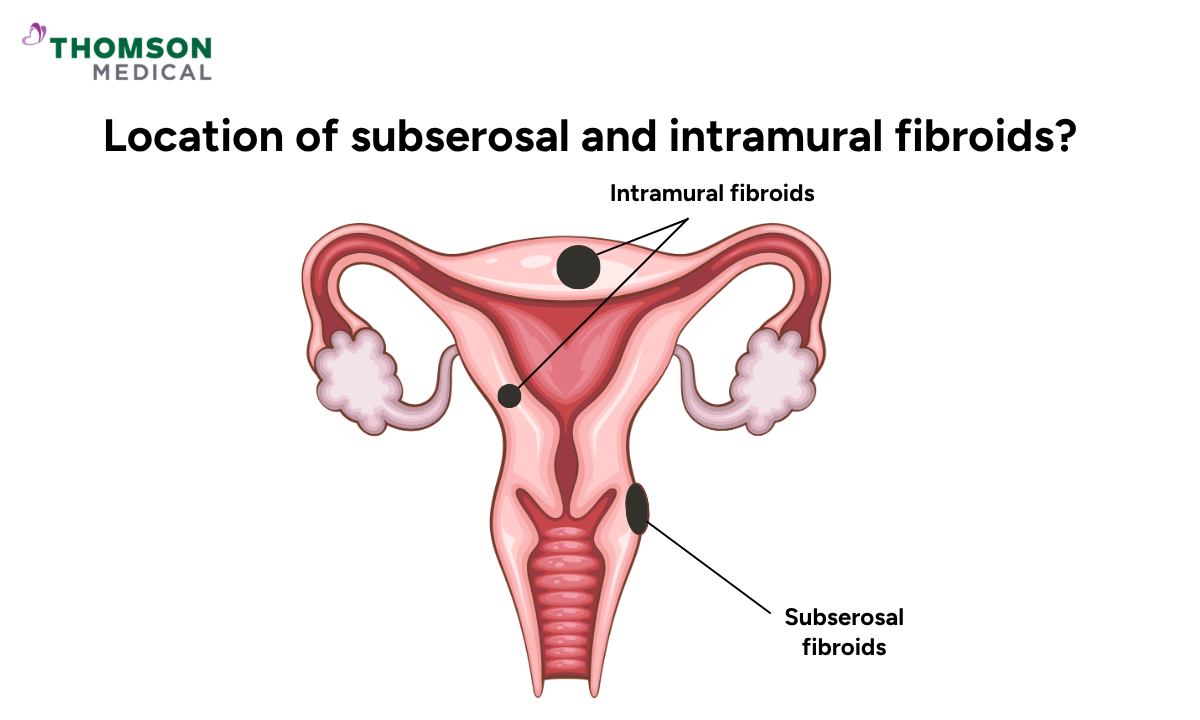
The fibroids most likely to cause bladder issues are subserosal fibroids (which grow on the outer surface of the uterus) and intramural fibroids (which grow within the uterine wall and expand toward the bladder).
The larger the fibroid, or the closer it sits to the bladder, the more likely it is to affect your bladder function.
What bladder symptoms might you notice?
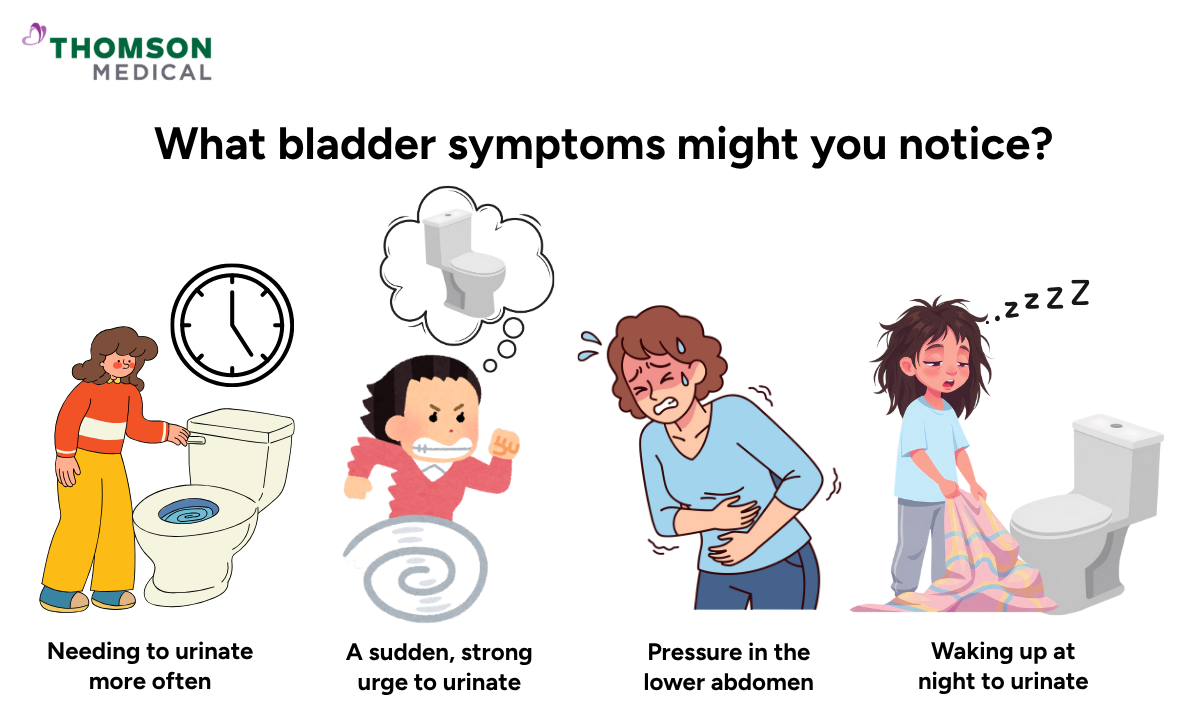
Bladder problems caused by fibroids can feel frustrating, especially if the cause is not immediately obvious. If fibroids are pressing on your bladder, you might notice one or more of the following.
Needing to urinate more often
You may find yourself going to the toilet far more frequently than usual, sometimes even shortly after you have just been. This happens because the fibroid reduces the space your bladder has to expand, so it reaches capacity much sooner than it normally would.
A sudden, strong urge to urinate
Some women feel an urgent need to urinate that can be difficult to control. You might also notice that even after going, your bladder does not feel completely empty. This can lead to repeated trips to the bathroom and a sense of ongoing discomfort throughout the day.
Pressure or discomfort in the lower abdomen
A feeling of heaviness, fullness, or constant pressure in the lower abdomen is common when fibroids are pressing on the bladder. This may come with mild pelvic pain, especially if the fibroid is large or positioned close to the bladder.
Waking up at night to urinate
This is known as nocturia (waking up one or more times during the night to use the toilet). Because fibroids can reduce bladder capacity even when you are lying down, your sleep can be significantly disrupted over time. Over time, disrupted sleep can affect your energy, mood, and general wellbeing.
If any of these symptoms sound familiar, it is worth exploring whether fibroids could be the cause, especially if other common explanations like a urinary tract infection (UTI) have already been ruled out.
Bladder symptoms such as urgency or frequent urination can sometimes be linked to fibroids. Request an appointment with Thomson Medical for a thorough evaluation and personalised care plan.
Could your bladder symptoms be related to fibroids?
Bladder symptoms can have many causes, including UTIs, an overactive bladder, or other pelvic conditions.
However, fibroids may be worth considering if:
Your symptoms are persistent or getting worse over time
You also have heavy periods, pelvic pain, or bloating
No infection has been found on urine tests
Your symptoms have not improved with standard bladder treatments
When bladder issues appear alongside other signs like heavy menstrual bleeding or pelvic discomfort, it often points toward a gynaecological cause rather than a bladder condition on its own.
Writing down all your symptoms, including those that seem unrelated, gives your doctor a clearer picture when assessing whether fibroids may be the cause.
Our gynaecologists
Loading...
How are fibroids diagnosed?
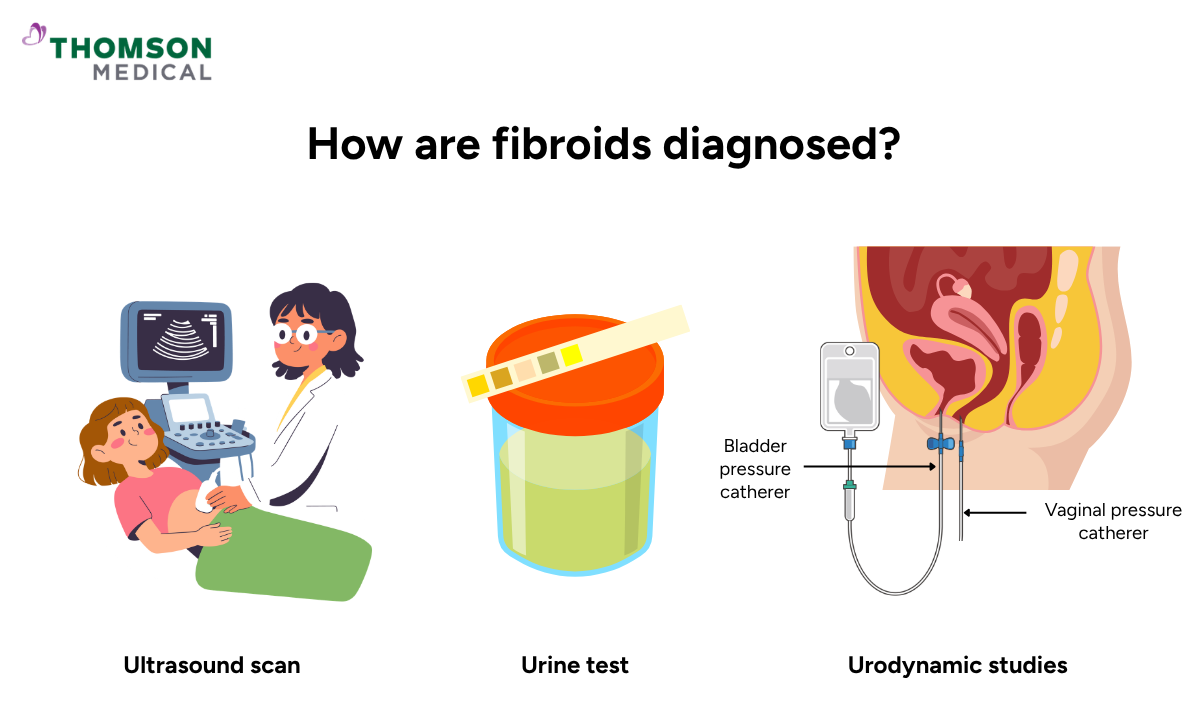
If your doctor suspects fibroids, they will usually begin with a pelvic exam to check for any changes in the size or shape of your uterus. From there, they may recommend further tests to better understand what is causing your symptoms.
These might include:
An ultrasound scan, which identifies fibroids and shows their location
An MRI scan, which provides a more detailed picture of the fibroids and surrounding structures
A urine test to rule out infection or other bladder conditions
Urodynamic studies, which in some cases assess how well your bladder is functioning
Getting a clear diagnosis is an important first step, because it helps your doctor understand the size, number, and position of your fibroids before recommending the most appropriate care for you.
What are your treatment options?
Treatment options vary and may include monitoring, medication, or procedures depending on your symptoms and overall goals.
Monitoring and symptom management
If your symptoms are mild, your doctor may suggest a monitoring and waiting approach.
Some simple adjustments that may help include:
Going to the toilet at set intervals rather than waiting until the urge becomes strong (sometimes called timed voiding)
Limiting fluids before bedtime to reduce night-time trips to the bathroom
Pelvic floor exercises to support better bladder control
This approach may be suitable if your symptoms are manageable and your fibroids are not growing quickly.
Medication
Medications can help manage symptoms or reduce fibroid size, though they are not a permanent solution.
Your doctor might discuss options such as:
Hormonal therapy such as GnRH agonists are injections that temporarily reduce oestrogen and shrink fibroids by lowering oestrogen levels. However, they are usually used short-term, such as before surgery, because symptoms and fibroid size may return after treatment stops
Oral contraceptives or a levonorgestrel-releasing intrauterine system may help control heavy bleeding in some women, though they do not usually shrink fibroids or relieve pressure symptoms directly
Pain relief to manage day-to-day discomfort
Medications are often used as a short-term measure, or alongside other treatments.
Minimally invasive procedures
For more significant symptoms, there are procedures that can treat fibroids without major surgery.
Two options that are commonly offered include:
Uterine artery embolisation (UAE):
A procedure that blocks the blood supply to fibroids, causing them to shrink over time and relieve pressure on the bladder.
MRI-guided focused ultrasound:
Uses targeted sound waves to destroy fibroid tissue and may be an option depending on the size and location of your fibroids.
Both options keep the uterus in place, but they may not be suitable for everyone, especially women planning future pregnancies. They generally involve a shorter recovery time than traditional surgery, which many women find reassuring. However, it’s important to discuss your fertility considerations before proceeding.
Surgical treatment
Surgery may be recommended if fibroids are large, causing significant symptoms, or have not responded to other treatments.
The two main surgical options are:
Myomectomy:
Removes the fibroids while keeping your uterus intact. Myomectomy is worth considering if you would like to preserve your fertility.
Hysterectomy:
Removes the uterus entirely, which means fibroids cannot return. Hysterectomy is more commonly considered when fertility is no longer a priority or when fibroids are very extensive.
Your doctor will explain which option suits your situation, and do not hesitate to ask questions before making any decisions.
When should you see a doctor?
Some urinary concerns are worth getting checked, especially if they are new, getting worse, or affecting your sleep and daily routine.
Speak to your doctor if you notice any of the following:
Urinary frequency or urgency that is disrupting your daily routine
Difficulty emptying your bladder fully
Waking up multiple times a night to urinate
Bladder discomfort alongside heavy periods or pelvic pain
Any difficulty passing urine at all
Burning pain when urinating
Seeing your doctor sooner rather than later means any fibroids can be identified and managed before symptoms become more difficult to deal with.
If your bladder symptoms are disrupting sleep, work, or daily activities, request an appointment with Thomson Medical to determine the underlying cause and appropriate management.
FAQ
Can small fibroids affect the bladder?
Small fibroids usually do not cause bladder problems because they are not large enough to exert significant pressure. Bladder symptoms are more commonly linked to larger fibroids or those located on the front wall of the uterus, where they can press directly on the bladder. In some cases, multiple small fibroids may still contribute to mild urinary discomfort.
Do bladder symptoms go away after fibroid treatment?
Yes, bladder symptoms often improve or resolve after effective fibroid treatment. Treatments such as medication, myomectomy, uterine artery embolisation, or other procedures can reduce pressure on the bladder. The improvement depends on the size, number, and location of the fibroids, as well as how long the bladder has been affected.
What are the symptoms of a fibroid pressing on the bladder?
Fibroids pressing on the bladder may cause frequent urination, urgency, difficulty fully emptying the bladder, a feeling of pelvic pressure or fullness, and increased urination at night.
How can bladder pressure from fibroids be relieved?
Bladder pressure can be managed through medical treatments, minimally invasive procedures, or surgery that reduces or removes fibroids.
Hormonal medications may temporarily shrink fibroids, while procedures like uterine artery embolisation or myomectomy offer more lasting relief. Lifestyle measures such as timed urination, pelvic floor exercises, and reducing fluid intake before bedtime may also help manage symptoms.
What organs are affected by uterine fibroids?
Uterine fibroids can affect nearby organs such as the bladder and bowel. Pressure on the bladder can cause urinary symptoms, while pressure on the rectum may lead to constipation or difficulty passing stool. In rare cases, very large fibroids may also affect surrounding nerves or blood vessels in the pelvis.
Can uterine fibroids cause UTI-like symptoms?
Yes, fibroids can sometimes mimic UTI symptoms such as frequent urination, urgency, or a feeling of incomplete bladder emptying. However, unlike UTIs, fibroid-related symptoms are usually not associated with burning urination, fever, or positive urine tests. A medical evaluation is needed to differentiate these two conditions.
Can fibroids return after treatment?
Yes, fibroids can return after treatment, particularly after procedures like myomectomy or medical management. The risks depend on factors such as age, hormone levels, number of fibroids, and individual circumstances.
A hysterectomy completely eliminates recurrence because the uterus is removed. Regular follow-up may be recommended for monitoring.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
