It is natural to wonder how infections like HPV spread, especially when it comes to everyday intimacy with a partner. Many people worry whether even something as simple as kissing could put them at risk.
HPV is very common, and most people will come into contact with it at some point in their lives. Understanding how it spreads – and how much risk is actually involved in activities like kissing – can help you feel more reassured and make informed decisions about your health.
Can you get HPV from kissing?
Yes, but it is uncommon.
The human papillomavirus (HPV) spreads primarily through skin-to-skin contact, particularly during sexual activity.
Deep kissing may carry a small risk if the virus is present in the mouth and there are tiny cuts or sores. However, compared to other forms of contact such as oral sex, the risk from kissing alone is considered low.
This makes kissing alone among the low-risk activities for this virus, meaning you do not need to avoid kissing your partner.
What increases your risk of getting HPV through kissing?
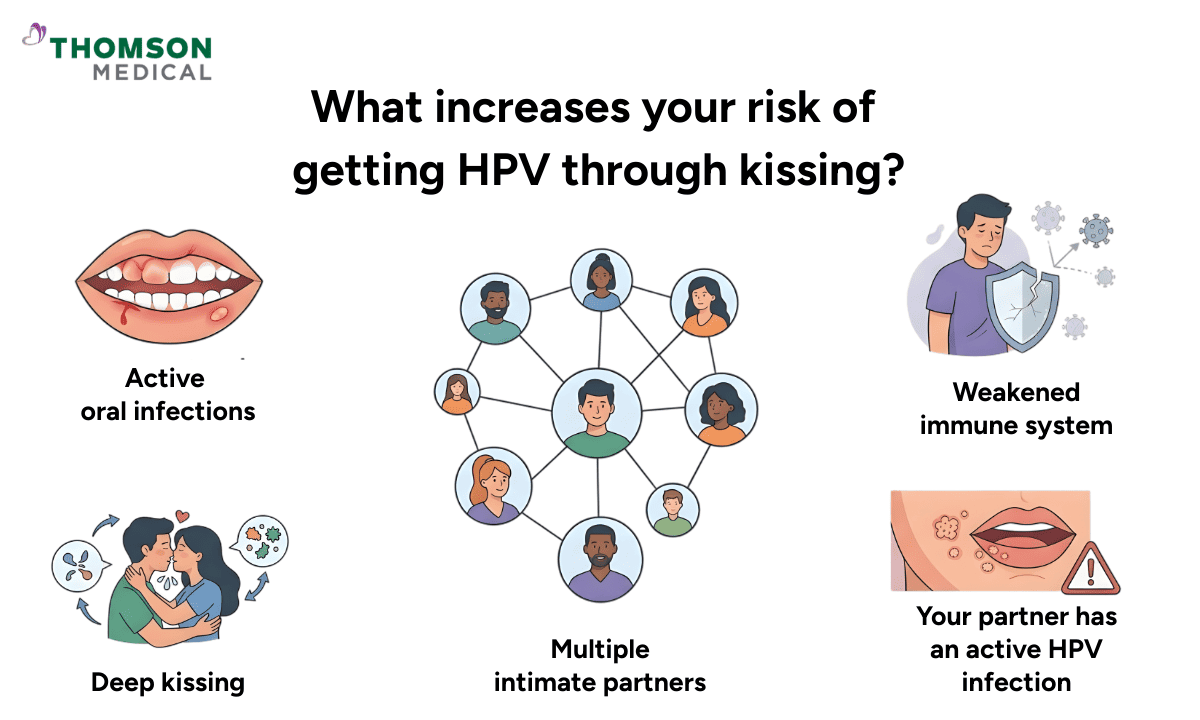
While the overall risk is very low, certain situations can make the transmission of an oral infection slightly more possible.
Your risk is slightly higher if:
You or your partner have active oral sores, bleeding gums, or sensitive dental ulcers.
You engage in passionate kissing or French kissing.
You have multiple intimate partners, which naturally increases exposure to various HPV types.
Your immune system is currently weakened, making it harder to stop viral replication.
Your partner has a known, active oral infection with the virus.
Even when these factors are present, the overall risk remains low. Maintaining good daily oral hygiene and treating any cuts or bleeding gums swiftly can help keep this risk under control.
If you have concerns about oral HPV transmission or would like advice on prevention and screening, you may arrange a consultation with Thomson Medical to discuss your risk factors and next steps.
How is HPV usually transmitted?
HPV spreads most easily through direct skin-to-skin contact, especially during sexual activity. It thrives in warm, moist environments and infects epithelial cells (protective cells that cover all inner and outer surfaces) through friction.
Common ways it can be transmitted include:
Vaginal sexual intercourse
Anal sexual intercourse, which carries a higher risk of transmission
Oral sexual intercourse, which is the primary way the virus reaches your mouth, throat, and base of your tongue
Genital-to-genital contact, even if no other acts occur
Sharing sex toys without proper cleaning or barrier methods
It can also spread without penetration, as contact between skin surfaces may be enough.
Using condoms or a dental dam is still a very helpful way to lower your risk. They create a protective barrier during intimate contact. However, they cannot offer complete protection because HPV can live on the surrounding skin that is not covered by the barrier.
HPV is not spread through everyday contact such as sharing utensils, toilets, or public spaces.
Symptoms of oral HPV to look out for
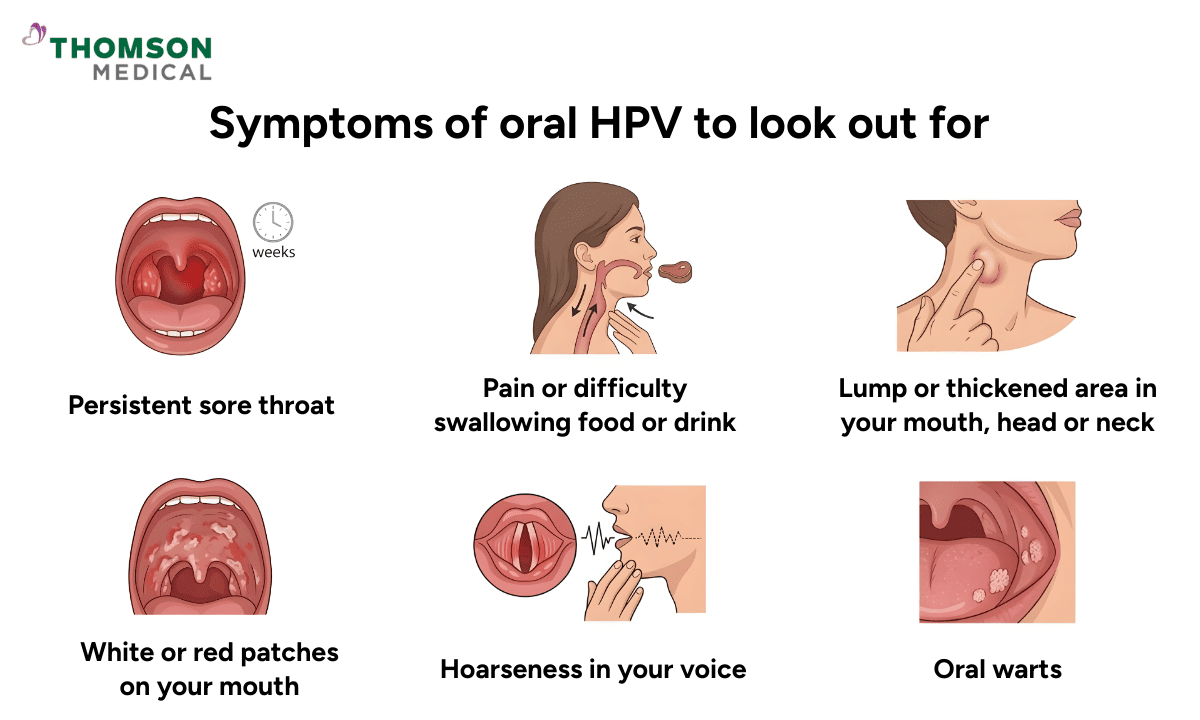
What makes recognising HPV difficult is its long incubation period, meaning it often does not cause noticeable symptoms. Most people who contract an oral infection show no symptoms at all.
However, when symptoms do occasionally appear, they may include:
A persistent sore throat that does not seem to respond to normal care
Pain or difficulty swallowing food or drink
A noticeable lump or thickened area forming inside your mouth, head or neck
Unusual white or red patches appearing on the mucous membrane of your mouth
Hoarseness in your voice that lasts for more than two to three weeks
The appearance of oral warts, though genital warts are much more common
These symptoms are not specific to the virus and could simply be a sign of a common cold. However, if they persist, getting them checked by a healthcare provider may help to monitor for any signs of serious problems, such as throat cancer.
If you notice persistent symptoms, it is advisable to seek medical evaluation. You may schedule a consultation with Thomson Medical to discuss your symptoms and receive an appropriate assessment.
How can you protect yourself from HPV?
There are several practical steps you can take to lower your risk of HPV and the cancers linked to it.
There are simple steps you can take to reduce your risk of HPV:
Getting the HPV vaccine, which helps prevent infection even if you are already sexually active
Limiting your number of sexual partners to reduce your overall exposure to new viral strains
Using condoms and dental dams consistently and correctly during oral contact
Avoiding smoking, as tobacco use may worsen oral viral infections and head and neck cancers
Attending regular health screenings, including cervical cancer screening, an anal Pap smear, or an anal swab test if recommended
Looking after your health does not require drastic changes. Small, consistent habits can make a meaningful difference over time.
When to see a doctor
While most oral issues simply need a little rest, it is always best to listen to your body. Seeking professional advice is a practical step for your wellbeing.
You should consider seeing a doctor or dentist if:
Your mouth or throat symptoms last for more than two to three weeks without improvement
You notice unexplained lumps, bumps, or discoloured patches during your daily routine
You know you have been exposed to the virus and feel concerned
Your immune system is weakened or you have a condition that affects immunity
If something in your mouth or throat does not feel quite right, it is important to get it checked. Getting advice early often makes things much simpler and helps you feel more at ease.
Our sexual health specialists
Loading...
FAQ
What other sexually transmitted infections (STIs) can be transmitted through kissing?
A few STIs can spread through kissing, especially if there is deep saliva exchange or if someone has active sores. The most common is the herpes simplex virus (HSV), which causes oral herpes and cold sores.
Kissing may also pass illnesses such as mononucleosis and, in rare cases, syphilis if open sores are present. Some studies suggest that gonorrhoea could occasionally spread through deep, open-mouth kissing when a partner has an active throat infection, though the risk is still much lower than with other forms of intimate contact.
Can I kiss my partner if he has HPV?
Yes. HPV is extremely common and most sexually active adults will encounter it at some point. If your partner does not have visible oral warts, the chance of spreading the virus through kissing is very low. Open communication and vaccination can help you feel more protected.
Can you get HPV non-sexually?
It is uncommon but possible. HPV can occasionally spread through close skin-to-skin contact or from a mother to her baby during childbirth. However, intimate contact remains the main way the virus spreads.
When is HPV no longer contagious?
There is no exact timeline. In most people, the immune system clears the virus within one to two years. Once the virus is suppressed, the likelihood of passing it on becomes much lower.
Should I panic if I have HPV?
No. HPV is very common, and most infections clear on their own without treatment. Only a small number of cases ever develop into HPV-related cancers. Regular health screening helps detect any changes early.
Can HPV cause rashes?
Not usually. HPV typically causes small raised warts rather than flat rashes. If you notice a widespread rash, it is more often linked to other skin conditions such as allergies or fungal infections.
Does oral HPV go away on its own?
In most cases, yes. The immune system often clears the infection within one to two years. Persistent infections are more likely in people who smoke, which is why regular dental check-ups and health screenings are helpful for long-term monitoring.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
Reference
Charleson F, Tran J, Kolobaric A, Case R, Fairley CK, Hocking JS, Chow EPF. A Systematic Review of Kissing as a Risk Factor for Oropharyngeal Gonorrhea or Chlamydia. Sex Transm Dis. 2023 Jul 1;50(7):395-401. doi: 10.1097/OLQ.0000000000001777. Epub 2023 Feb 3. PMID: 36735907; PMCID: PMC10259206.
Cook, R. L., Thompson, E. L., Kelso, N. E., Friary, J., Hosford, J., Barkley, P., Dodd, V. J., Abrahamsen, M., Ajinkya, S., Obesso, P. D., Rashid, M. H., & Giuliano, A. R. (2014). Sexual behaviors and other risk factors for oral human papillomavirus infections in young women. Sexually transmitted diseases, 41(8), 486–492. https://doi.org/10.1097/OLQ.0000000000000159
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
