Many people usually confuse HPV with herpes or assume that they are the same infection. However, the truth is that these are caused by two entirely different viruses. As a result, they differ in symptoms, how they spread, and what they mean for your health.
Knowing the difference between HPV and herpes can help you make more informed decisions about testing, treatment, and protecting your long-term sexual health.
What is the difference between HPV and herpes?
Although both are common viral infections, they affect your body in unique ways.
Here’s a breakdown of the core differences between these two:
Feature | Human papillomavirus (HPV) | Herpes (HSV) |
Full name | Human papillomavirus | Herpes simplex virus |
Virus type | A DNA virus with over 200 different types | A DNA virus with two main types, HSV-1 and HSV-2 |
Main effect | May cause skin and cellular changes, such as genital warts. Persistent, long-term cases can also lead to issues like cervical cancer | Causes skin and mucosal infections that may recur periodically |
Typical symptoms | Often has no symptoms | May cause painful fluid-filled blisters or sores
|
Can it be cleared naturally? | Yes, your immune system usually clears it. | No, the virus lies dormant in nerve tissue and may reactivate over time. |
Cancer risk | Yes, certain types carry a cancer risk. | No, it does not cause cancer. |
Vaccine | Vaccines are highly recommended. | There is currently no vaccine. |
By knowing these basic differences, you can become more aware of what you are dealing with. This also helps your doctor choose the suitable care plan for you.
How do HPV and herpes spread?
Both viruses are easily transmitted through skin-to-skin or sexual contact, especially during vaginal, anal, and oral sexual activities. They are more likely to spread if you have visible lesions, although transmission can still occur without any visible symptoms.
Mother-to-child transmission is also possible for both HPV and herpes.
Herpes can also be passed on through saliva. This means that kissing or sharing the same drinks may expose you to this virus. It is also important to know that transmission of herpes is still possible even when there are no noticeable symptoms.
If you are concerned about HPV or herpes transmission or would like guidance on testing and prevention, you may arrange a consultation with Thomson Medical to discuss your risks and appropriate next steps.
What are the symptoms of HPV vs herpes?
Both HPV and herpes can remain in the body for long periods without causing any noticeable symptoms, which is one reason regular sexual health screening is important.
When symptoms do occur, herpes tends to cause more noticeable signs than HPV. Both infections may produce lesions around the genitals, anus, or mouth. In some cases, HPV-related growths may also appear in the throat, although this is less common.
Common symptoms of HPV
Many may never know that they have HPV unless they’re tested. However, there are still signs that it may be present in your body.
Possible signs include:
Genital warts, which look like painless, soft, cauliflower-like bumps
Abnormal cell changes that can only be observed during routine screenings
Keep in mind that this virus does not usually cause any physical pain. If you have painless genital lesions, it is worth speaking with your doctor, who can assess whether HPV or another cause may be involved.
Common symptoms of herpes
Both viruses may cause lesions. However, people with herpes are likely to experience more noticeable symptoms.
Possible symptoms include:
Tingling or burning on your skin, which often happens right before a outbreak appears
Clusters of fluid-filled blisters that may break open and form painful sores
Pain during urination, as your urine may touch the open sores and cause a sharp stinging sensation
General flu-like symptoms during the first infection, such as fever, body aches, or swollen lymph nodes
Herpes sores are usually very painful and sensitive to the touch, unlike painless warts. If you are experiencing discomfort, reaching out to your doctor quickly can help you find relief at the right time.
Our sexual health specialists
Loading...
Who is at risk of getting HPV or herpes?
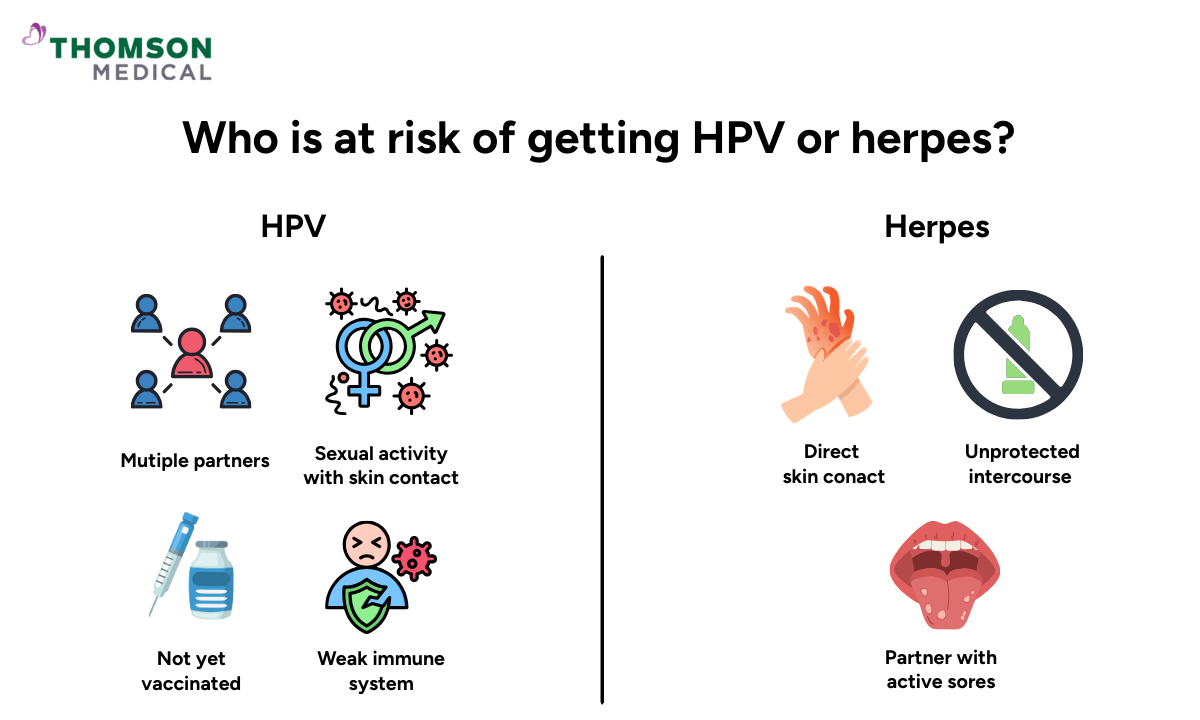
Because these viruses are so common, anyone who is sexually active may experience some level of risk. That doesn't mean an infection is inevitable, but understanding what increases risk can help you make informed choices and feel more in control.
HPV risk factors
You might be exposed to HPV if you:
Are sexually active in any way that involves skin-to-skin genital contact
Have multiple intimate partners
Haven’t received an HPV vaccination
Have a weakened immune system, which can make it harder for your body to clear the virus naturally
Nearly all sexually active adults will encounter HPV at some point in their lives. It is a normal part of being human and sexually active, so there is no need to feel ashamed if you are exposed.
Herpes risk factors
You might be exposed to HSV if you:
Have direct skin-to-skin contact with an infected person
Have unprotected vaginal, anal, or oral sex with an infected partner
Have a partner with active sores, though it's important to know that herpes can also be passed on even when no visible symptoms are present
Taking precautions and talking honestly with your partners may help manage your risk and protect your shared sexual wellness.
How are HPV and herpes diagnosed?
If you suspect you have either virus, proper laboratory testing is the only way to know for sure.
HPV diagnosis
Some common tests to diagnose HPV include:
Pap smear to check for early abnormal cell changes on the cervix
HPV DNA test to detect the virus's genetic material in cervical cells
Visual exam, which your doctor can identify external warts by looking at them
There is currently no routine HPV screening test for men without symptoms. Because of this, it is important to pay attention to any unusual changes, such as genital warts or persistent throat or anal symptoms and seek medical advice if they appear.
Herpes diagnosis
Some common tests to diagnose herpes include:
Swab test to collect a sample from an active sore, which is then tested using PCR or viral culture to detect the virus
Blood test to check for herpes antibodies, which may indicate past exposure to the virus
Clinical exam, where your doctor may identify a typical herpes outbreak based on the appearance of sores or blisters
Getting prompt testing when you have active symptoms gives your doctor the opportunity to take an accurate swab, leading to a clear and helpful diagnosis.
If you notice symptoms such as sores or blisters and would like a clear diagnosis, you may schedule a consultation with Thomson Medical to discuss appropriate testing and next steps.
How are HPV and herpes treated?

While neither virus has a cure that entirely clears it from the body, both are highly manageable with the right medical support.
HPV treatment
Although there is no treatment that removes HPV from your body, your doctor may help you manage the conditions it may cause.
Treatment usually focuses on the following:
Warts:
These can be managed with topical creams, freezing techniques, or specialised laser treatments.
Abnormal cells:
These are managed through careful monitoring or minor procedures to remove the affected tissue.
Natural clearance:
A healthy immune system will clear the virus on its own, often within one to two years. Your doctor may simply recommend regular monitoring during this time.
Herpes treatment
While herpes stays in the body after infection, treatment can help control symptoms and reduce outbreaks.
Common approaches include:
Antiviral medications:
Prescription medicines like aciclovir or valaciclovir help manage the virus.
Transmission reduction:
Taking antiviral tablets may lower your chance of passing the virus to your partner.
Suppressive therapy:
Daily antiviral treatments may be used to prevent outbreaks from happening.
With the right plan from your doctor, you may be able to control your symptoms and continue enjoying a healthy, fulfilling life.
How do HPV and herpes affect long-term health?
Looking toward the future is common when managing a new diagnosis. The long-term impacts of these viruses are very different.
HPV long-term effects
In most cases, HPV infections resolve on their own. However, certain strains may lead to complications if they persist for many years.
Possible long-term outcomes include:
It usually clears completely with no lasting problems.
Persistent high-risk HPV strains can cause cervical cancer, anal cancer, throat cancers, and penile cancer if left undetected and untreated.
In rare cases, if abnormal cells are not monitored and managed, they may progress to cervical cancer over time.
These serious risks are highly preventable. By combining the HPV vaccine with regular screening, you can protect yourself from the vast majority of long-term complications.
Herpes long-term effects
Herpes tends to follow a different pattern, remaining in the body and occasionally reactivating.
Common long-term experiences include:
You may experience recurrent outbreaks, though they usually become milder over time.
It can cause emotional stress or anxiety, especially around dating.
It poses a specific risk during pregnancy, known as neonatal herpes, a condition where the virus is passed to the newborn. Your obstetrician will guide you through this.
It does not cause cancer, and in otherwise healthy adults, it generally does not affect your fertility or lifespan.
While managing occasional outbreaks can be frustrating, the emotional side of a herpes diagnosis is just as real as the physical. With the right support system and medical care, it may simply become a small, manageable part of your routine.
If you are living with herpes and would like guidance on managing outbreaks or protecting your partner’s health, it may help to speak with a healthcare professional. You may schedule a consultation with Thomson Medical to discuss appropriate care and management options.
FAQ
Are HPV and herpes the same thing?
No. They are different viruses that belong to separate families. HPV refers to a group of papillomaviruses, while herpes is caused by HSV. They can lead to different symptoms and health concerns.
How do I know if it is HPV or HSV?
Some signs may offer clues. Painful blisters or sores are more commonly associated with herpes, while small growths or having no symptoms at all may be linked to HPV. However, only appropriate medical testing performed by a healthcare professional can confirm the cause.
Can herpes go away like HPV sometimes does?
Herpes remains in your body after infection. However, it may stay inactive for long periods, and many people experience long stretches without noticeable symptoms.
What are the first warning signs of HPV?
Many people do not notice any early physical symptoms. In some cases, small genital warts may appear, or changes may be detected during routine cervical screening.
Can HPV cause cramps or discomfort?
HPV itself does not usually cause pelvic cramps or pain. If you experience persistent discomfort, it is advisable to seek medical advice so the cause can be properly assessed. However, conditions linked to persistent HPV, such as advanced cervical changes, may cause discomfort over time.
Can HPV be completely cured?
There is currently no treatment that directly removes HPV from the body. In many cases, the immune system clears the virus naturally over time. Vaccination and regular screening can help reduce your risk of certain HPV-related conditions.
Does oral HPV cause cold sores?
Cold sores around your lips or mouth are usually linked to HSV. Oral HPV infections often do not cause noticeable symptoms, although certain high-risk strains may in some cases be associated with growths or changes in the throat.
Do HPV vaccines protect against herpes?
No. HPV vaccines are designed to protect against specific types of HPV. They do not protect against the herpes virus.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
