Hearing that you may need breast surgery can feel overwhelming. It is natural to have questions, especially when terms like 'lumpectomy' and 'mastectomy' are introduced.
You may be wondering how these surgeries differ and which option is right for you. While it is common to assume that one is safer than the other, the reality is more nuanced.
Understanding what each procedure involves and when it may be recommended can help you feel more prepared when discussing your options with your doctor.
What is a lumpectomy?
A lumpectomy removes a breast tumour along with a small amount of the tissue around it. The goal is to treat the cancer while preserving as much of the breast as possible.
You may also hear this referred to as ‘breast-conserving surgery’ or a ‘wide local excision’. These terms describe the same approach.
What is a mastectomy?
While a lumpectomy removes only the affected area, a mastectomy removes all of the breast tissue. Depending on your condition, this may also include the nipple, areola, surrounding skin, or nearby lymph nodes.
Your surgeon may discuss one of the following types with you:
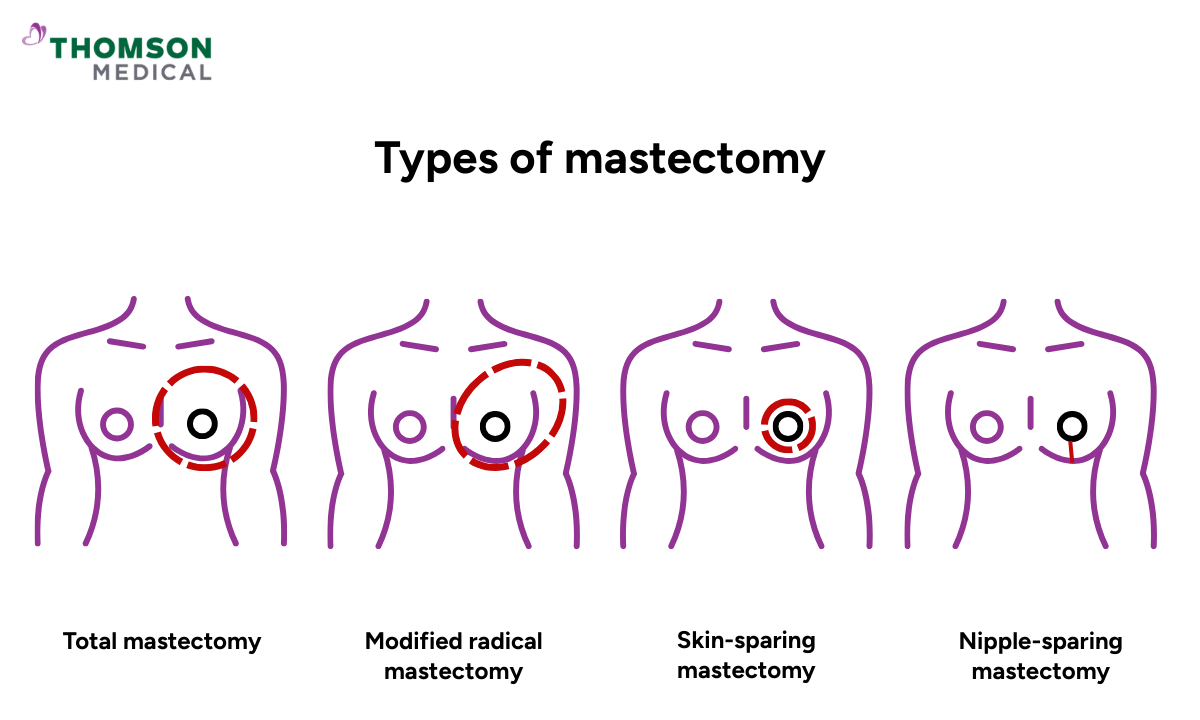
Total mastectomy:
Removes all breast tissue, the nipple, and the areola (dark area of skin surrounding a nipple)
Modified radical mastectomy:
Removes all breast tissue, the nipple, the areola, and most of the lymph nodes from your armpit
Skin-sparing mastectomy:
Removes breast tissue, the nipple, and the areola but keeps most of the breast skin to support reconstruction
Nipple-sparing mastectomy:
Removes breast tissue whilst keeping the skin, nipple, and areola intact, and tends to give the most natural appearance after reconstruction
Which type your surgeon recommends depends on where the cancer is located in your breast. If the tumour is close to the nipple, for example, a nipple-sparing approach may not be safe.
The type of surgery also affects which reconstruction options are available to you, which is why discussing reconstruction beforehand with your doctor matters if you're considering it.
Our breast cancer specialists in Singapore
Loading...
Who is each surgery recommended for?

Every woman's situation is different, and your doctor's recommendation will be shaped by your medical history, personal risk factors, and overall health. Your doctor will recommend a treatment based on your individual situation.
Lumpectomy
A lumpectomy is most often recommended when the cancer is caught early and contained within one specific area of the breast.
Your doctor may suggest it if:
The tumour is small relative to your breast size
The cancer has not spread beyond the breast
You have not had previous radiation to the same breast
If the tumour is too large relative to your breast size, a lumpectomy may not be suitable, as removing enough tissue would significantly alter the breast's appearance.
It may also not be an option if there are multiple areas of cancer, since removing all of the cancer with a single surgery can be difficult in these cases.
Mastectomy
A mastectomy may be recommended when removing just the tumour would not be enough to reduce the risk of cancer returning.
Your doctor may suggest it if:
The tumour is large or affects more than one area of the breast
You carry a BRCA1 or BRCA2 gene mutation that raises your lifetime risk of breast cancer
You have had previous radiation to the chest and cannot safely have further radiation treatment
You have a strong family history of breast cancer and want to reduce your future risk through preventive surgery
In some cases, both surgeries may be suitable for you. If that is the case, your surgeon will talk you through what each option means so you can make the appropriate choice.
Choosing the right surgery depends on your individual diagnosis, breast size, genetic risk, and personal preferences. Request an appointment with the Thomson Breast Centre to discuss whether a lumpectomy or a mastectomy is most suitable for you.
How effective is each surgery?
For many women with early-stage breast cancer, long-term survival outcomes are similar whether treatment involves a lumpectomy followed by radiation or a mastectomy.
Advances in treatment have also reduced the risk of cancer returning after a lumpectomy. While a mastectomy may lower the risk of recurrence in the treated breast, it does not always lead to better overall survival.
As radiation and medications have improved over the years, the risk of cancer returning after a lumpectomy has fallen from around 5–10% to about 4.2–4.7% within five years. After a mastectomy, the risk of recurrence is around 1% or less.
Your doctor will help you understand what these differences mean in the context of your specific diagnosis.
What should you expect after surgery?
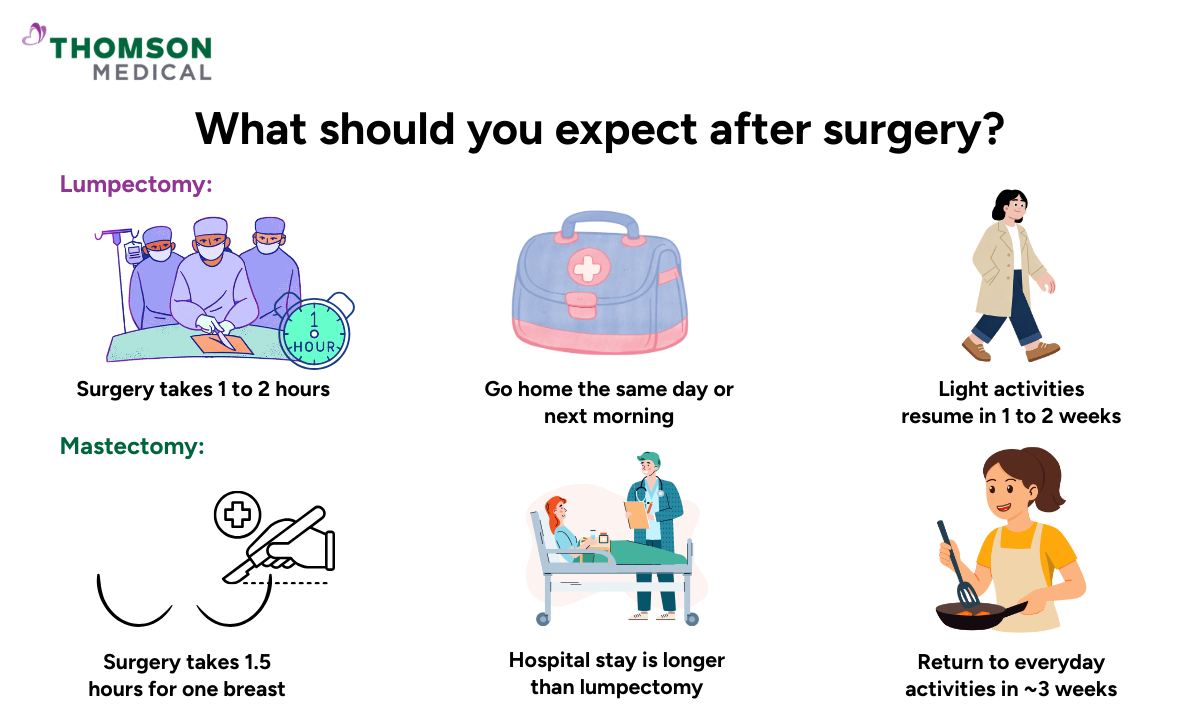
Recovery looks different depending on which surgery you have. Where the two procedures differ most is in how long you will need to rest, what follow-up care involves, and how your body may change as a result.
Lumpectomy
A lumpectomy typically takes 1 to 2 hours. Most people go home the same day or the following morning and are back to light activities within 1 to 2 weeks. Because only the tumour and a small amount of surrounding tissue are removed, the overall shape of your breast is usually preserved.
You may notice some change in the area where the tissue was taken out, especially if the tumour was large compared to your breast size. However, most women can continue wearing their usual bras and do not need breast reconstruction.
Radiation therapy is usually recommended afterwards as part of the overall treatment plan.
Mastectomy
A mastectomy takes longer, ranging from 1.5 hours for one breast to around 3 hours for both. If breast reconstruction is performed at the same time, surgery can take 4 to 6 hours, and your hospital stay will be longer.
Most people are able to return to everyday activities in around 3 weeks, with full healing taking up to 6 weeks. Whether radiation is needed will depend on the findings from your surgery, such as whether cancer was found in your lymph nodes or close to the chest wall.
If you have concerns about how your body will look after a mastectomy, breast reconstruction is an option. This can be done at the same time as your mastectomy (immediate reconstruction) or months to years later (delayed reconstruction).
Discussing this with your surgeon before your mastectomy is important because the type of mastectomy performed affects which reconstruction approaches are possible for you.
Lumpectomy vs mastectomy compared at a glance
Both surgeries differ across several important areas. The table below summarises these differences to help you see both options side by side.
Lumpectomy | Mastectomy | |
What is removed | A tumour and a small surrounding margin | All breast tissue may include nipple, areola, lymph nodes |
Surgery duration | 1 to 2 hours | 1.5 to 6 hours depending on type and reconstruction |
Hospital stay | Same day or 1 night | 1 to 2 days; longer if reconstruction is performed |
Recovery | Light activities in 1 to 2 weeks. Full recovery in 2 to 4 weeks | Everyday activities in around 3 weeks. Full healing up to 6 weeks |
Breast appearance | Largely preserved | A breast removal and reconstruction is an option |
Follow-up treatment | Radiation is usually required | Radiation may or may not be needed |
Risk of local recurrence | Small chance cancer may return in the same breast | Lower risk of recurrence in the treated breast |
Some figures may vary depending on whether reconstruction is involved or if lymph nodes need to be removed. Your surgeon will give you a more precise estimate once your treatment plan is confirmed.
How do you decide between the two?
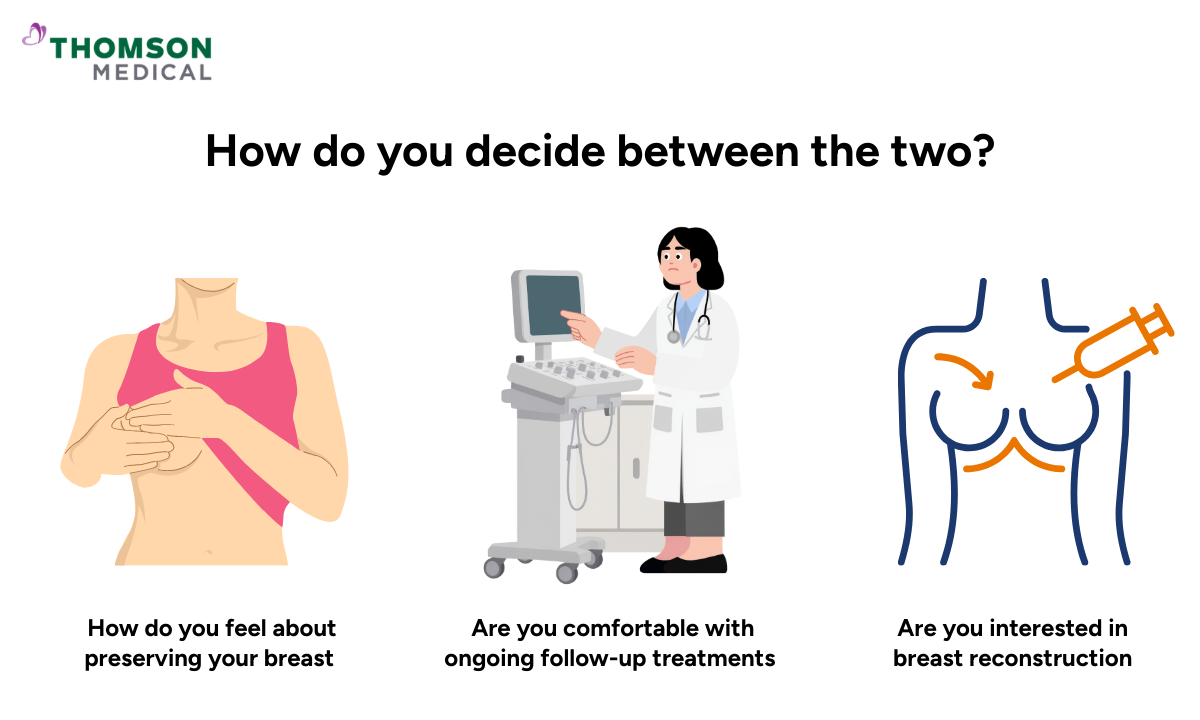
When both surgeries are medically suitable, the decision often comes down to what feels right for you.
It can help to reflect on a few things before your appointment:
How do you feel about preserving your breast versus reducing the risk of recurrence?
Are you comfortable with ongoing follow-up treatments such as radiation?
Are you interested in breast reconstruction, and when would you want it done?
What do your support network and home situation look like during recovery?
There is no single right answer, and your feelings deserve to be part of the conversation with your surgeon.
Cost comparison in Singapore
Having a sense of the costs involved beforehand can help you plan ahead with less stress. The figures below are from private hospitals in Singapore and are meant as a general guide.
Lumpectomy | Mastectomy | |
Typical hospital bill | SGD 23,760 to SGD 36,159 | From SGD 32,497 (with axillary clearance) |
Surgeon fee | SGD 6,322 to SGD 11,009 | SGD 6,649 to SGD 13,080 |
Anaesthetist fee | SGD 1,417 to SGD 2,071 | SGD 1,962 to SGD 2,616 |
Daily doctor attendance | SGD 230 to SGD 450 per day | SGD 230 to SGD 450 per day |
Costs may be higher depending on the complexity of your surgery, whether lymph nodes are removed, and the length of your hospital stay.
A mastectomy with reconstruction performed at the same time will also affect the overall bill. If you have health insurance, check with your insurer before your procedure so you have a clear picture of what is covered and what you may need to pay yourself.
Bill amounts are intended as a general guide by the Ministry of Health Singapore. Actual costs may vary depending on your condition, treatment plan, and choice of hospital. Please check with your hospital for a more accurate estimate.
Both a lumpectomy and a mastectomy are effective surgical treatments for breast cancer, and there is no single answer that suits everyone. The right choice depends on your diagnosis, your body, and what matters most to you.
Speaking openly with your surgeon and taking the time you need to decide are all part of finding a path you feel confident in.
Understanding the potential costs can help you plan your treatment with confidence. Request an appointment with the Thomson Breast Centre to discuss your options, get a personalised cost estimate based on your situation, and explore how insurance or payment plans may support your care.
FAQ
Is a lumpectomy safer than a mastectomy?
Both surgeries are considered safe and are carried out under general anaesthetic in a hospital setting. The risks differ slightly, as a lumpectomy is a shorter operation with a quicker recovery, while a mastectomy is more involved.
Which surgery has a faster recovery?
A lumpectomy generally has a faster recovery. Most people return to light activities within 1 to 2 weeks. After a mastectomy, most people need around 3 weeks before returning to everyday activities, and longer if reconstruction is performed at the same time.
Is mastectomy more effective than lumpectomy for breast cancer?
For many people with early-stage breast cancer, studies have shown that a lumpectomy followed by radiation offers survival rates comparable to a mastectomy. A mastectomy does lower the risk of cancer returning in the same breast, but this does not always mean better overall outcomes.
How do doctors decide between lumpectomy and mastectomy?
Your doctor will look at several factors, including the size and location of your tumour, whether the cancer has spread, your medical history, and whether you carry any genetic mutations such as BRCA1 or BRCA2. In some cases, both options may be suitable, and the decision will also take your personal preferences into account.
Will I need a second operation after a lumpectomy or mastectomy?
After a lumpectomy, a second operation may be needed if the initial surgery did not remove all of the cancer cells with a clear margin. After a mastectomy, some people choose to have a separate breast reconstruction procedure at a later stage.
Can I breastfeed after a lumpectomy or mastectomy?
It depends on which surgery you have. After a lumpectomy, breastfeeding may still be possible, though it can be affected by the location of the tumour and whether radiation therapy is given afterwards. After a mastectomy, breastfeeding on the treated side will not be possible, as all breast tissue is removed.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, request an appointment with Thomson Breast Centre today.
References:
Doyle, C. (n.d.). Recurrence rates after lumpectomy significantly improved in patients receiving ‘Modern-Era’ therapy. https://ascopost.com/issues/june-10-2018/recurrence-rates-after-lumpectomy-significantly-improved-with-modern-era-therapy/
Ministry of Health Singapore. (2023). SA824B - Breast, tumor (malignant various lesions), simple mastectomy with axillary clearance, with/without sentinel node biopsy. https://www.moh.gov.sg/managing-expenses/bills-and-fee-benchmarks/cost-financing/tosp-sa824b-bill-information
Ministry of Health Singapore. (2023). SA823B - Breast, tumor (malignant), wide excision/lumpectomy/segmental mastectomy/partial mastectomy, with axillary clearance, with/without sentinel node biopsyhttps://www.moh.gov.sg/managing-expenses/bills-and-fee-benchmarks/cost-financing/tosp-sa823b-bill-information/
Schumacher, J. R., Wiener, A. A., Greenberg, C. C., Hanlon, B., Edge, S. B., Ruddy, K. J., Partridge, A. H., Le-Rademacher, J. G., Yu, M., Vanness, D. J., Yang, D., Havlena, J., Strand, C., & Neuman, H. B. (2022). Local/Regional recurrence rates after Breast-Conserving therapy in patients enrolled in legacy trials of the Alliance for Clinical Trials in Oncology (AFT-01). Annals of Surgery, 277(5), 841–845. https://doi.org/10.1097/sla.0000000000005776
