Finding out human papillomavirus is a group of over 200 viruses can feel concerning given how common this virus is. However, the majority of these viruses do not actually cause serious harm and generally fade away on their own.
Understanding the different types of HPV and which types to be more careful about can help you better understand your risks and the steps you can take to protect your health.
What is human papillomavirus (HPV)?
Human papillomavirus (HPV) is one of the most common sexually transmitted infections (STIs) in the world. This virus infects your skin and mucous membranes (the moist inner linings of areas such as the mouth and genital region). HPV is mainly transmitted through skin-to-skin contact during sexual activity.
There are over 200 types of HPV. They are generally grouped into low-risk and high-risk types, and more than 40 of them can infect the genital area.
Low-risk HPV types
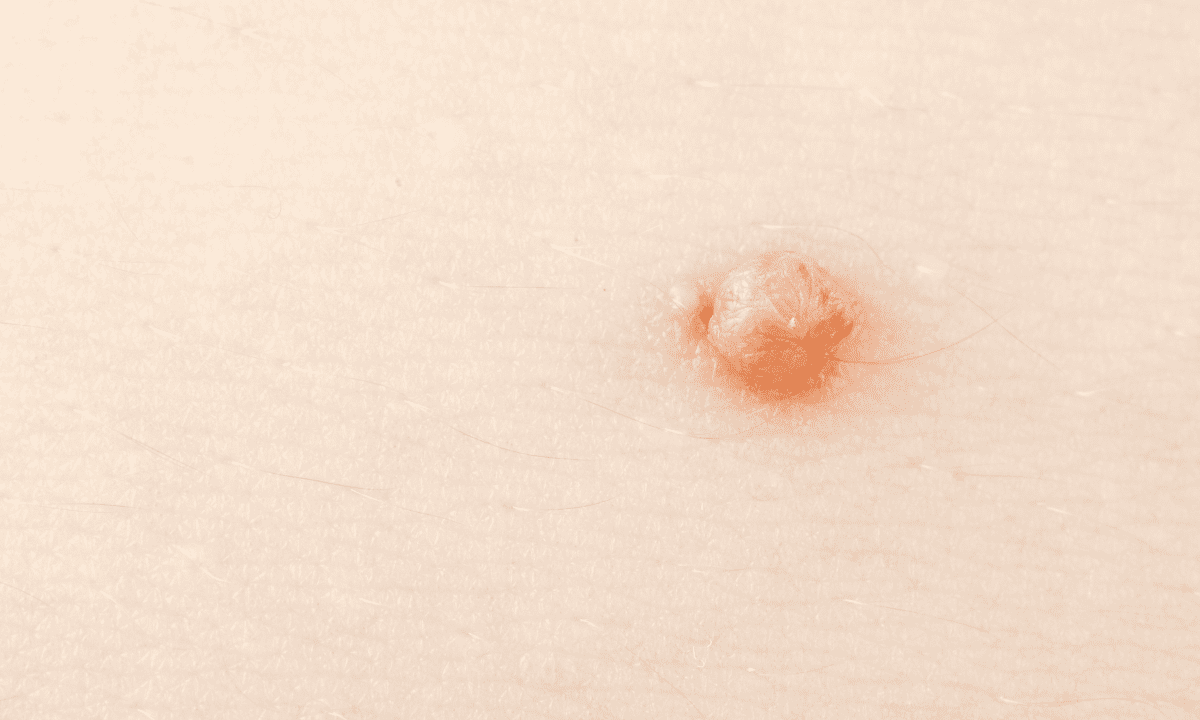
When your doctor talks about low-risk HPV types, they’re referring to strains that typically don't cause cancer. These types infect the outer layers of your skin and mucosal surfaces.
Although they are not life-threatening, they may still cause physical discomfort and emotional stress from conditions such as genital warts. The good news is that with the right care, these conditions are usually manageable.
Type 6
HPV type 6 is one of the most common low-risk strains and is responsible for most cases of genital warts in both men and women.
Although it does not cause cancer, the warts it leads to can sometimes return and may need treatment. This can be uncomfortable or frustrating, but these growths are generally manageable with proper care.
In rare cases, HPV type 6 has also been linked to a condition called recurrent respiratory papillomatosis (RRP), where wart-like growths develop in the airway. While this may affect breathing or voice, it is uncommon and usually benign.
Type 11
This is another common low-risk HPV strain that is closely linked to genital warts. Like type 6, it does not cause cancer, but it can lead to visible lesions in your genital or anal areas that may feel uncomfortable or distressing. HPV type 11 is also more often associated with RRP.
As HPV type 6 and type 11 are the main causes behind genital warts, they are often the low-risk strains your doctor focuses on when diagnosing and managing these conditions.
If you notice symptoms such as unusual growths or persistent genital warts, it is advisable to seek medical evaluation. You may arrange a consultation with Thomson Medical to discuss appropriate treatment and management options.
High-risk HPV types
Unlike low-risk types, high-risk HPV strains have the potential to cause cancer. These viruses can sometimes stay in your body for a long time, leading to a persistent infection. When this happens, they may slowly cause abnormal changes in the cells they infect.
Over time, these changes can develop into precancerous lesions. If they are not detected or treated, they may eventually progress to cancer.
However, it is important to remember that the main concern is long-term persistent infection, not short-term exposure, as many HPV infections are cleared naturally by your body’s immune system within a year or two.
Type 16
HPV type 16 is considered one of the most cancer-causing strains of the virus. It is strongly linked to cervical cancer and is also associated with cancers of the anus, penis, and oropharyngeal region (the back of the throat).
In fact, according to the Centers for Disease Control and Prevention (CDC), HPV type 16 is associated with approximately 50% of cervical cancers worldwide.
Type 18
HPV type 18 is another major high-risk strain. It is often associated with cervical cancer and other anogenital cancers. Although it is slightly less common than type 16, it still carries a high risk of causing harmful cellular changes.
According to the World Health Organization (WHO), HPV types 16 and 18 combined are responsible for over 70% of cervical cancers globally. Because of this, most HPV vaccination programmes and cervical screening efforts focus on protecting against and detecting these two strains.
Our sexual health specialists
Loading...
How do you test for and prevent HPV?
Finding out whether you have HPV usually involves testing for viral DNA from affected tissues. While testing is helpful, taking preventive steps is still recommended to protect your health in the long run.
Here are common steps you can take to detect the HPV virus:
Cervical screening:
For women, routine cervical screening is a very effective way to check for early cellular changes.
These tests can spot potential problems early, often long before they develop into something more serious.
Targeted testing for men:
At the moment, there is no routine HPV screening programme for men.
HPV testing for men is usually recommended only if certain risk factors are present or if noticeable symptoms appear.
Vaccination:
HPV vaccines help protect you against several of the most common high-risk and low-risk strains.
These include well-known types such as 6, 11, 16, and 18.
Safe sexual practices:
Using condoms consistently can help lower your risk of transmission.
Because HPV spreads through skin-to-skin contact, condoms cannot provide complete protection.
Combining regular health check-ups with these preventive steps may help support your long-term reproductive and sexual health.
How do you manage HPV?
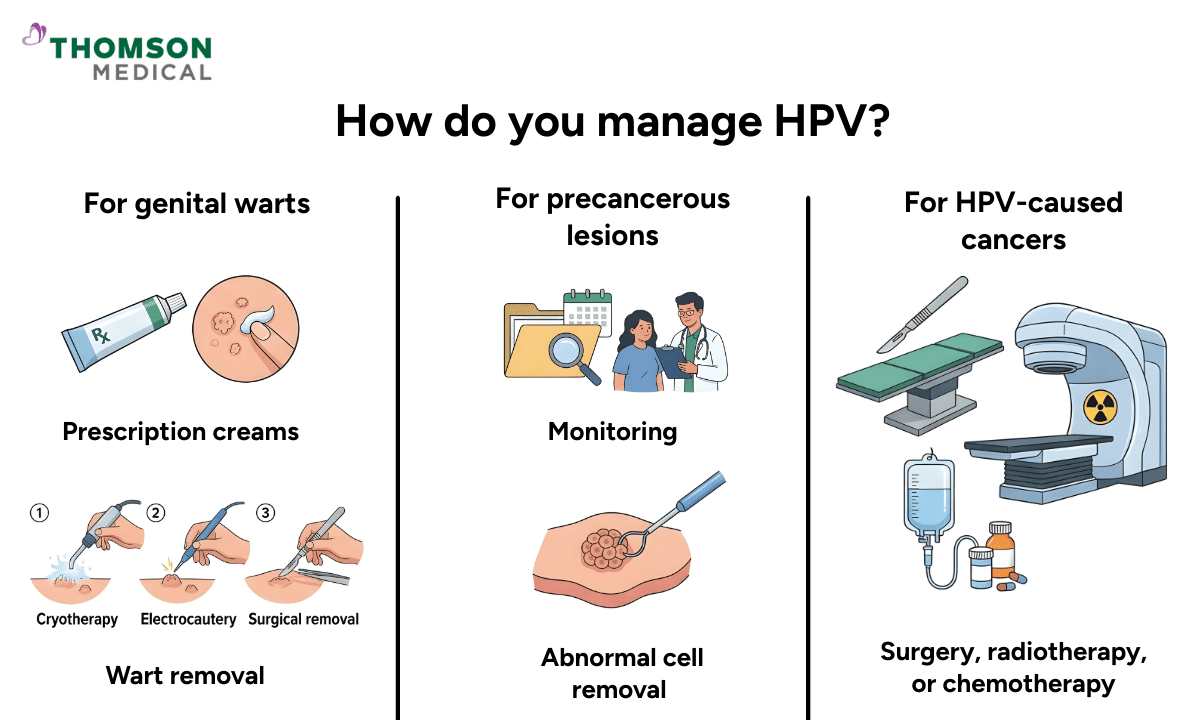
At the moment, there is no single medication that can completely remove HPV from your body. However, there are many effective ways to treat and manage the conditions it may cause.
Common ways HPV-related conditions may be managed include:
For genital warts:
Genital warts can often be treated with prescription creams.
Your doctor may also remove them using treatments such as freezing the wart (cryotherapy), using heat to remove it (electrocautery), or performing surgical removal.
For precancerous lesions:
If screening detects precancerous changes, your doctor may recommend closer monitoring.
In some cases, minor procedures may be used to remove abnormal cells before they develop into cancer.
For cancers caused by HPV:
If cancer develops, you may need surgery, radiotherapy, or chemotherapy.
The exact treatment depends on the stage of your condition and where it occurs in your body.
Your immune system often eliminates the infection naturally, meaning many people return to normal health without needing specific antiviral treatment.
If you have been diagnosed with HPV or would like guidance on managing HPV-related symptoms, you may schedule a consultation with Thomson Medical to discuss appropriate treatment and monitoring options.
FAQ
How do I know what type of HPV I have?
Only a laboratory test can identify your specific HPV type. In women, this may be detected during cervical screening. For men, routine typing tests are not commonly performed. Many people never learn their exact type because the infection clears on its own.
What can I expect if I have HPV?
Most people have no symptoms and never realise they are infected. In many cases, the immune system clears the virus within one to two years. Some people may develop genital warts, while high-risk types can cause cell changes over time.
How is HPV transmitted?
HPV spreads through direct skin-to-skin contact, most commonly during vaginal, anal, or oral sex. While not offering complete protection, using condoms may help reduce your risk.
Can HPV cause cramps?
HPV itself does not usually cause cramps. If you experience persistent pelvic pain, it is best to consult a healthcare provider to check for other causes.
When should I see a healthcare provider?
You should seek medical advice if you notice genital warts, unusual growths, unexplained bleeding, or persistent pain. Women should also keep up with routine cervical screening.
Should my partner be worried if I have HPV?
HPV is very common, and many sexually active people will be exposed at some point. A positive result does not necessarily mean a recent infection. Staying up to date with screening and vaccination can help reduce future risk.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
Reference
Centers for Disease Control and Prevention. (2024, April 23). Chapter 11: Human papillomavirus. In Epidemiology and prevention of vaccine-preventable diseases (The Pink Book). https://www.cdc.gov/pinkbook/hcp/table-of-contents/chapter-11-human-papillomavirus.html
World Health Organization. (2025, December 2). Cervical cancer. https://www.who.int/news-room/fact-sheets/detail/cervical-cancer
World Health Organization. (2024, March 5). Human papillomavirus (HPV) and cancer. https://www.who.int/news-room/fact-sheets/detail/human-papilloma-virus-and-cancer
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
