A hysterectomy is one of the most common gynaecological surgeries, yet many people find themselves wondering what is actually happening inside their body once it is done. It is completely natural to feel curious, or even a little anxious, about changes you cannot see. The healing process involves far more than just a surgical wound closing over.
Your organs gently shift into new positions, scar tissue forms to stabilise things, and your pelvic floor adapts to its new role. For some people, hormone levels may change too. All of this happens quietly, over weeks and months.
Knowing what to expect can make recovery feel far less uncertain and help you recognise what is normal along the way.
How your organs settle after a hysterectomy
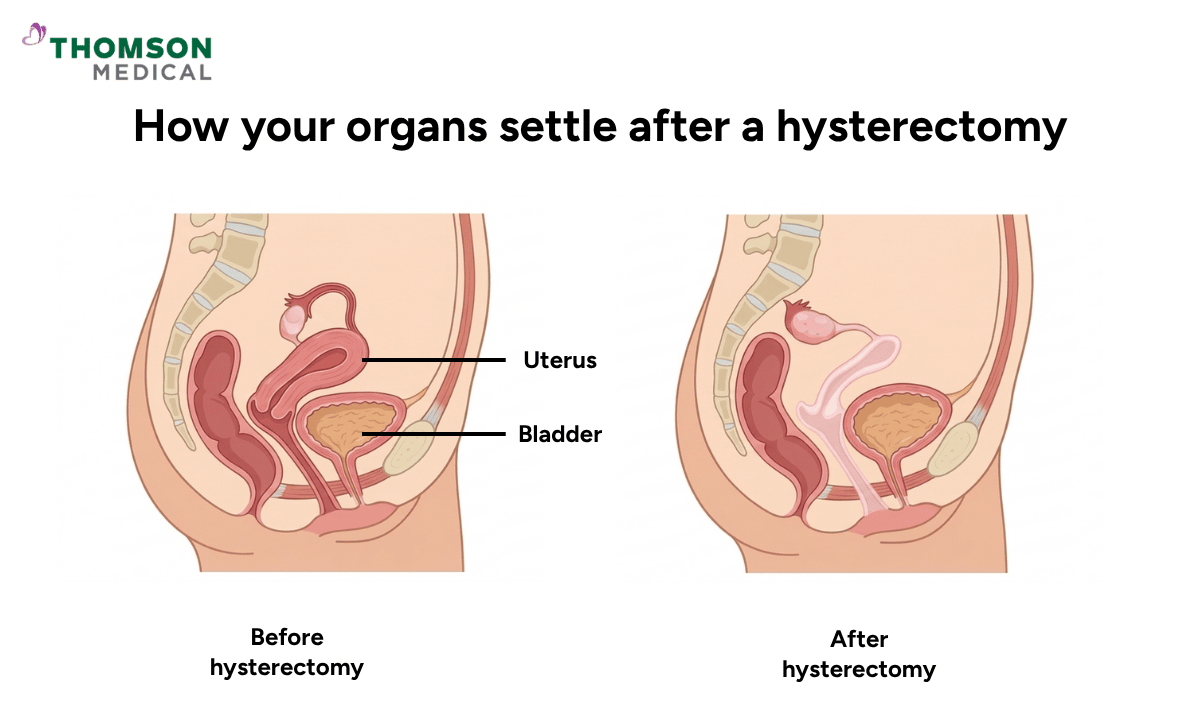
Your uterus normally sits between your bladder at the front and your rectum at the back. When it's removed through a hysterectomy, that space doesn't simply stay empty.
Here's what happens:
Your bladder shifts slightly downward, now sitting closer to where your uterus used to be
The top of your vagina is closed with stitches to form a vaginal cuff
Scar tissue forms to help hold everything in its new position
This repositioning happens slowly and naturally, and you are unlikely to feel your organs moving. In the early weeks, some people notice mild pressure or fullness in the pelvis. For most people, this condition settles by 6 to 8 weeks.
What happens to the vaginal cuff?
When the uterus is removed, the surgeon stitches the top of the vagina closed. This sealed area is called the 'vaginal cuff'. It is a normal part of the procedure and plays an important role in keeping your pelvic organs supported after surgery.
During this time, your doctor will advise you to avoid anything that puts pressure on the area, including sexual intercourse, heavy lifting, and intense exercise, until they confirm it is safe to resume.
How your pelvic floor is affected
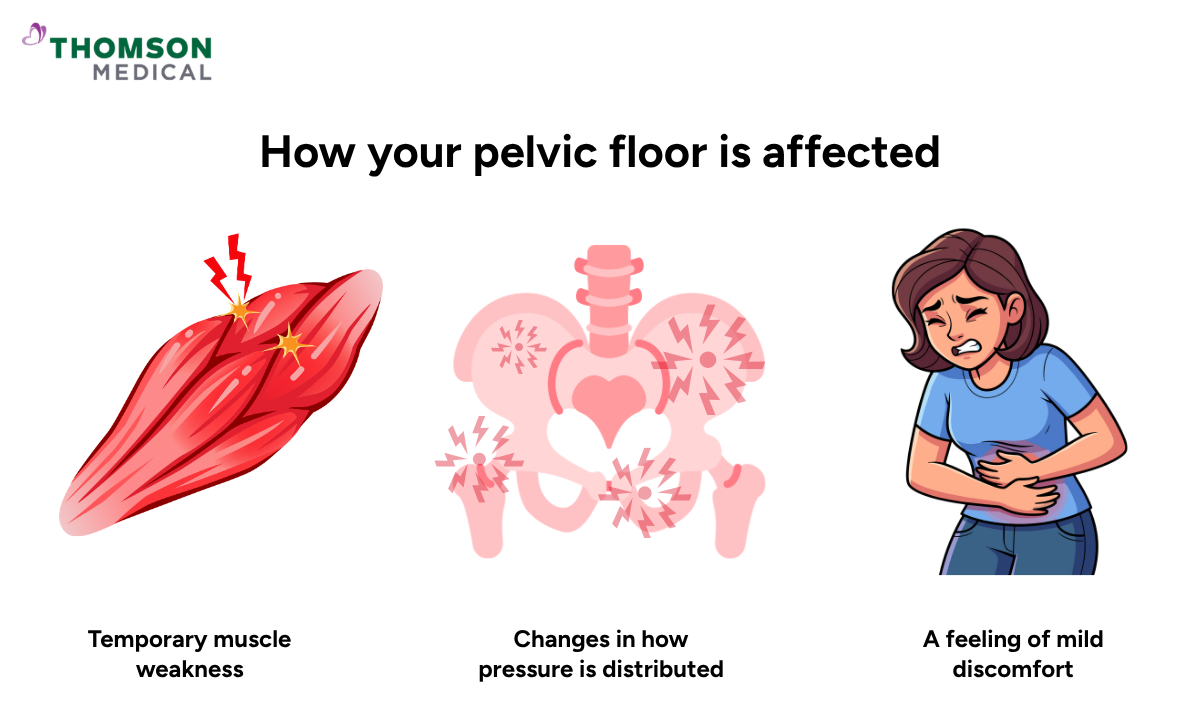
Your pelvic floor is a group of muscles and connective tissues at the base of your pelvis that support your bladder, bowel, and vagina.
Before surgery, your uterus helped support your pelvic organs. Once the uterus is removed, your pelvic floor takes on more of the load.
You may experience:
Temporary muscle weakness while tissues heal
Changes in how pressure is distributed across the pelvis
A feeling of heaviness or mild discomfort
If the pelvic floor muscles are weak, there's a slightly higher chance of pelvic organ prolapse developing over time. Keeping up regular pelvic floor exercises helps reduce the risk of prolapse over time and supports bladder control as you age.
What happens to your ovaries after a hysterectomy?
Your hormone levels after a hysterectomy depend largely on whether your ovaries are removed.
If your ovaries are kept
Your ovaries continue producing oestrogen and other hormones as normal. Your hormone levels should remain stable. You are likely to go through natural menopause at some point in the future. The hysterectomy itself is not causing menopause, though for some people it may arrive a little earlier than expected.
Because you no longer have a uterus, you may not have periods, so you may not notice exactly when menopause begins. If you're unsure, your doctor can use a blood test to better understand where you are in the menopausal transition.
If your ovaries are removed
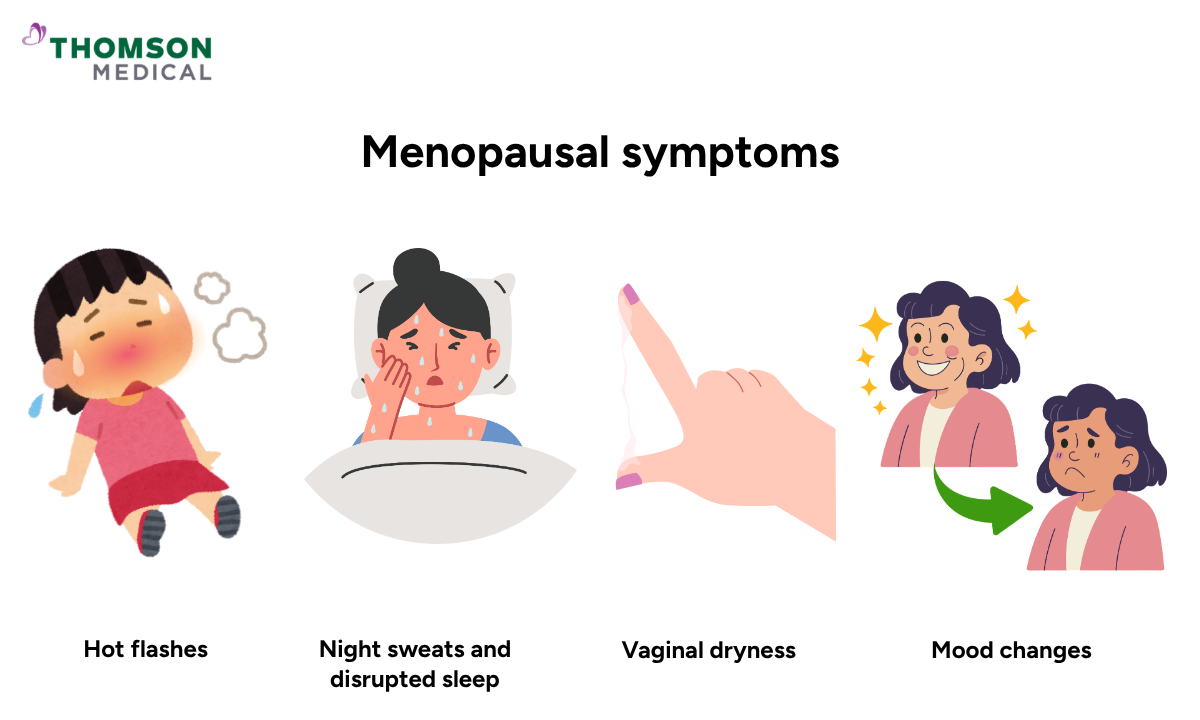
Removal of ovaries causes hormone production to stop abruptly. This is known as surgical menopause, and symptoms can begin within days to weeks after surgery.
These may include:
Hot flashes
Night sweats and disrupted sleep
Mood changes
If these symptoms feel familiar, your doctor may discuss hormone replacement therapy (HRT) to help manage your condition. You may discuss with your doctor whether HRT is appropriate for you based on your medical history.
If you are experiencing menopausal symptoms after your surgery, request an appointment with Thomson Medical. Our specialists can assess your hormone levels and advise whether treatments such as hormone replacement therapy may be suitable for you.
Your internal healing timeline
Healing after a hysterectomy takes place in stages.
Weeks 1 to 2: Inflammation and swelling
Your immune system responds immediately with inflammation, which begins the repair process. Swelling is normal and expected at this stage.
Weeks 3 to 6: Tissue repair
Your body starts laying down new tissue to repair the surgical areas. Internal stitches begin dissolving within the first few weeks and are usually fully absorbed by week 6.
Weeks 6 to 12: Scar tissue matures
Scar tissue forms, strengthens, and gradually helps support your organs in their new positions.
By 12 weeks, most people notice an improvement in their energy levels and comfort. Your internal healing continues well beyond this point, with your scar tissue softening and remodelling for up to 12 months or longer.
What scar tissues does and how they feel
Scar tissue plays an important role in your recovery. It seals surgical areas, helps secure organs in place, and supports the healing of surrounding tissues.
In the early weeks, you may notice the area feeling tight, tender, or sore, especially with certain movements. This is normal as your body heals.
Over time, your scar tissue softens and settles. Gentle movement and walking help this process along. In some cases, excess scar tissue can form and cause ongoing discomfort, though this does not affect most people. If you notice persistent or worsening pain beyond the early weeks, don’t hesitate to speak with your doctor.
Our hysterectomy surgeons in Singapore
Loading...
How bladder and bowel change after hysterectomy
Because your bladder and bowel sit so close to the uterus, they are often affected in the weeks following surgery. Most changes are temporary and settle as your body adjusts.
Bladder
Bladder function can feel different in the early weeks of recovery.
You may notice:
A more frequent urge to urinate than usual
Mild leakage while healing takes place
If fibroids were pressing on your bladder before surgery, you may find your symptoms improve after the operation
These bladder symptoms usually resolve within 6 to 12 weeks. If bladder symptoms continue beyond 12 weeks, or if you notice difficulty passing urine or pain, it helps to check with your doctor.
Bowel
Your bowel is also likely to feel sluggish in the first few weeks as your gut recovers from surgery and anaesthesia.
Common experiences include:
Constipation in the first few weeks
Gas and bloating as your gut recovers
Staying well hydrated, eating plenty of fibre from fruits, vegetables, and whole grains, and going for short walks each day all support bowel recovery. Bowel function usually returns to normal within 2 to 4 weeks.
What to expect in the longer term after a hysterectomy
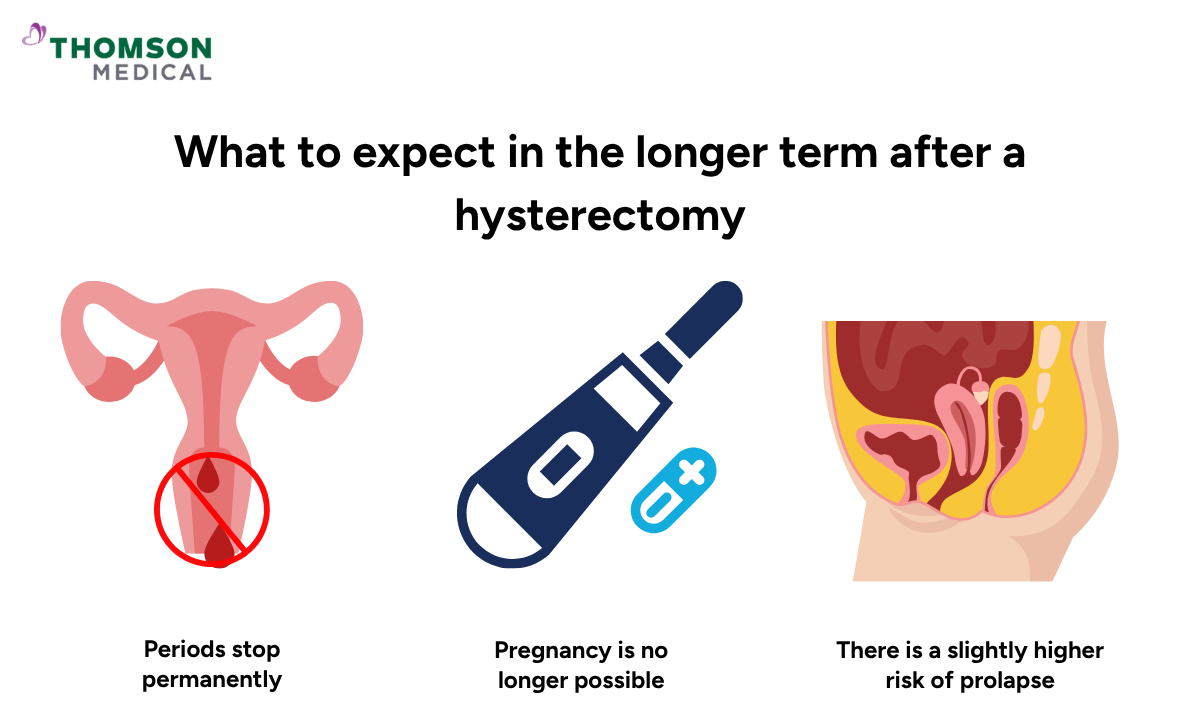
Once your body has fully healed, most people go on to feel well and comfortable.
Here is what longer-term life after a hysterectomy generally looks like:
Periods stop permanently
Pregnancy is no longer possible
The pelvic organs settle into stable positions
There is a slightly higher risk of prolapse
However, many people notice improvements in quality of life, especially if symptoms such as pain, heavy bleeding, or pressure are relieved.
Your body goes through a lot after a hysterectomy, so it’s natural to have questions or feel unsure at times. If something doesn’t feel right, you can always check in with your doctor. You don’t have to go through recovery on your own, and the right support can make a big difference.
Every recovery time is different, and so is long-term healing. Request an appointment with Thomson Medical to understand what to expect after recovery and receive personalised advice for your next stage of care.
FAQ
How long does it take for internal stitches to dissolve after a hysterectomy?
Most dissolvable stitches dissolve within six to eight weeks. Some may take up to twelve weeks. Your body handles this issue naturally on its own. You do not need to do anything to help the process along.
Do your other organs move after a hysterectomy?
Yes, but only slightly. Your bladder and bowel shift a little to fill the space where your uterus was. Scar tissue and muscles keep everything stable and in place. Most people do not feel this happening.
Can you feel the internal changes after a hysterectomy?
Some people notice a mild pressure, pulling sensation, or feeling of fullness in the lower abdomen during recovery. This is normal and usually settles over the coming weeks. If the sensation is sharp, worsens, or does not improve, please speak with your doctor.
What happens to your cervix after a hysterectomy?
- Total hysterectomy: Both the uterus and cervix are removed. The top of the vagina is stitched closed to form a vaginal cuff.
- Subtotal hysterectomy: Only the uterus is removed. The cervix remains in place. You may still need to attend cervical screening appointments as usual.
If you are unsure which type of hysterectomy you had, your doctor can confirm this for you.
Does your stomach shrink after a hysterectomy?
Not significantly. The uterus is relatively small, so its removal does not noticeably change the size or shape of your abdomen. Some bloating in the first few weeks is common. This is usually due to post-surgical swelling or trapped gas, and it tends to settle as your body heals.
Will I still have discharge after a hysterectomy?
These are generally considered normal:
- Light, clear or white discharge
- Pink or brown spotting for four to six weeks after surgery
- Occasional light spotting if your cervix was kept in place
- Reduced discharge over time if your ovaries were removed
Please speak with your doctor if you notice any of the following:
- Discharge with an unpleasant smell
- Green- or yellow-coloured discharge
- Heavy bleeding
- Discharge that continues beyond six to eight weeks alongside pain or fever
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and advice based on your unique situation, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
