When a fibroid causes sudden, severe pain, your first instinct might be that something has gone seriously wrong. In some cases, though, this pain can actually mean the fibroid is starting to shrink on its own.
This process is called ‘fibroid degeneration’, and it happens when a fibroid outgrows its blood supply. While the discomfort can feel alarming, knowing what's behind it can help you decide when home care is enough and when to see your gynaecologist.
What are fibroids?
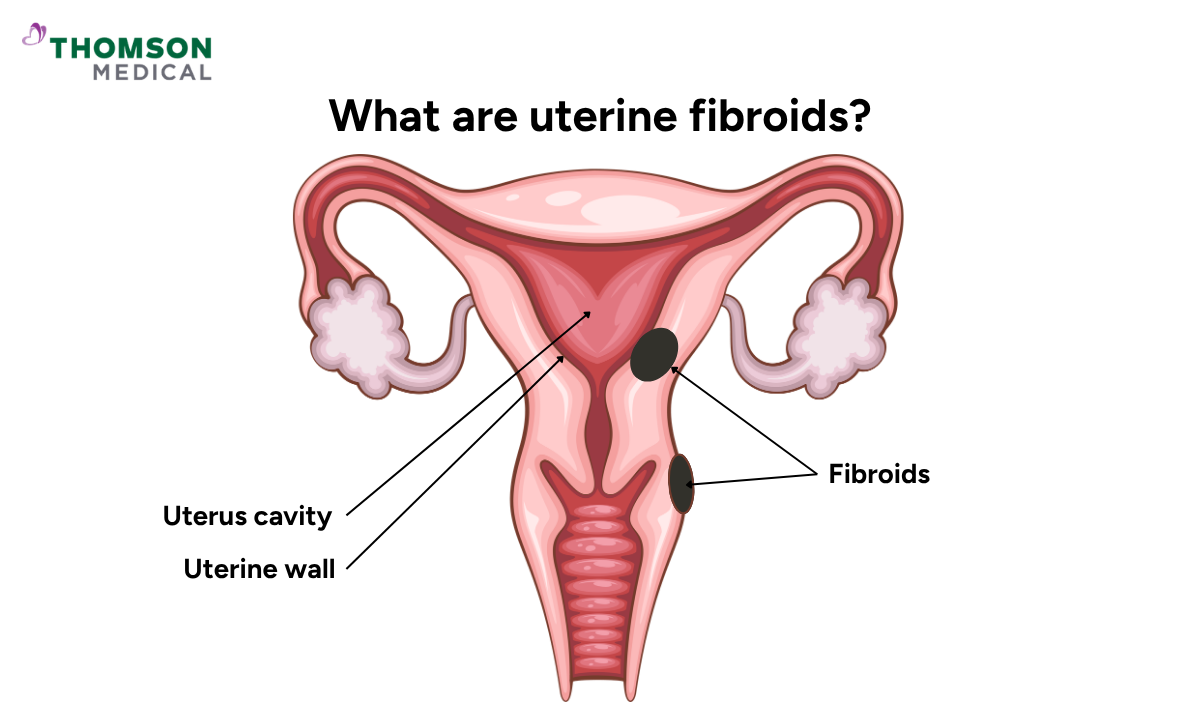
A uterine fibroid is a non-cancerous growth made of muscle and fibrous tissue that develops in or on the uterus. Many fibroids are small and cause no symptoms.
What is fibroid degeneration?
Fibroid degeneration happens when a fibroid outgrows its blood supply, causing parts of its tissue to break down or lose structure. This is a recognised change that can occur within fibroids. It is not cancerous, but it can cause pain or other symptoms in some women.
What causes fibroid degeneration?
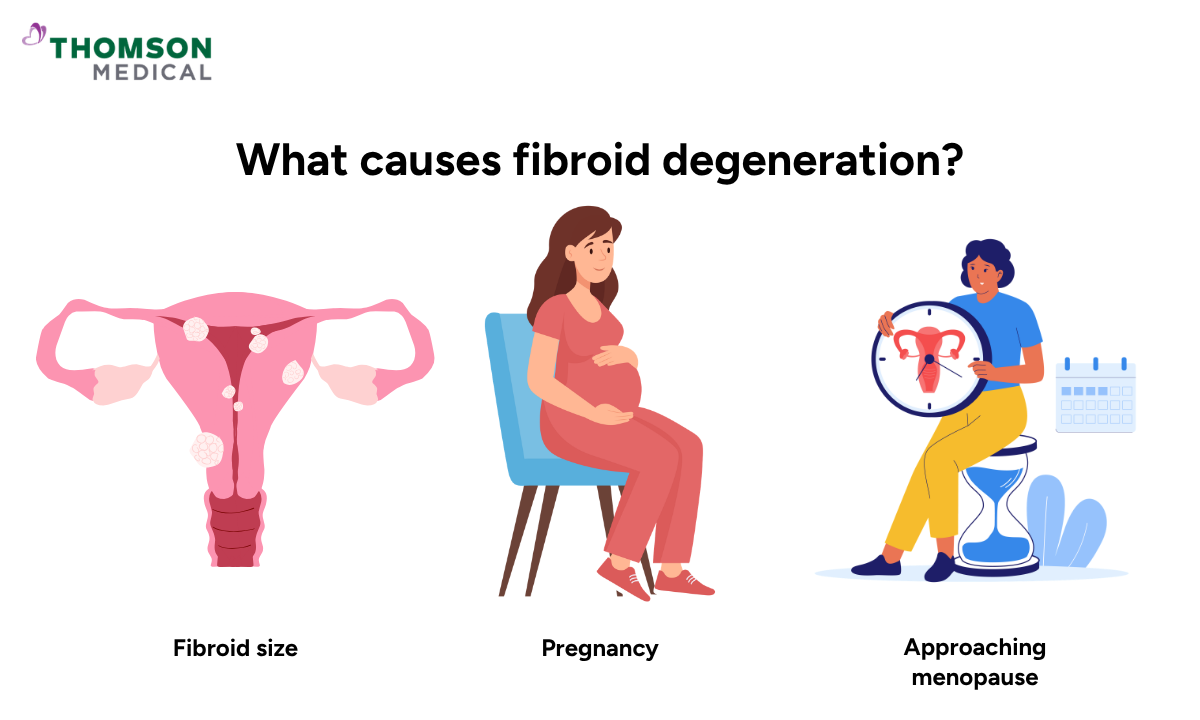
Fibroid degeneration becomes more likely when a fibroid grows to a size where its inner tissue can no longer receive enough oxygen and nutrients.
Several factors can make this more likely:
Fibroid size:
Larger fibroids carry a higher risk because their inner tissue sits furthest from the blood supply.
Pregnancy:
Rapid uterine growth and hormonal changes can alter circulation, making degeneration more common during this time.
Approaching menopause:
Natural hormonal changes may affect how blood flows to your fibroid tissue, causing some fibroids to shrink and develop calcification over time.
Changes in blood supply:
Any situation that reduces blood flow to the fibroid may increase the chance of degeneration.
Degeneration during pregnancy is often temporary and may settle with supportive care. However, abdominal pain during pregnancy should always be discussed with your doctor so they can check both you and your baby and rule out other causes.
Our gynaecologists
Loading...
Types of fibroid degeneration
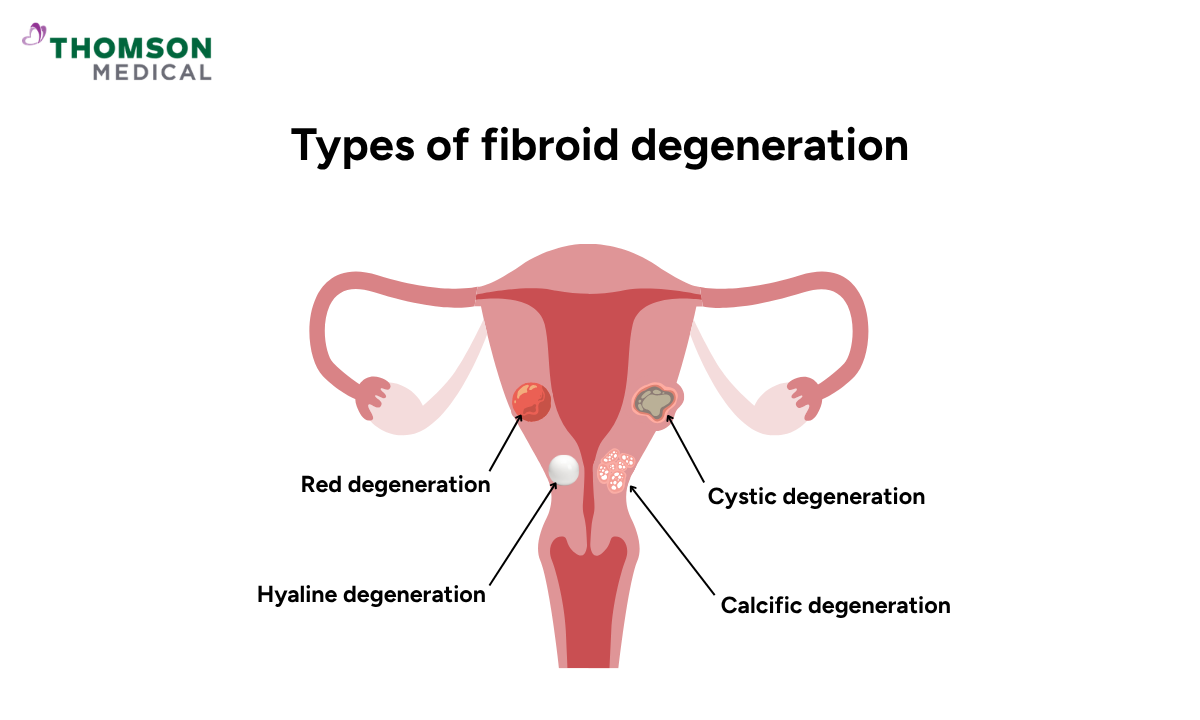
Not all fibroid degeneration is the same. The type depends on how blood flow is reduced, the size of the fibroid, and your life stage, such as pregnancy or menopause.
Hyaline degeneration
This is the most common type. Fibroid tissue is gradually replaced by a firm, smooth material, changing the internal structure of the fibroid. This is a slow change that takes place over time.
Red degeneration (carneous degeneration)
This type is more sudden and can be quite painful. It happens when blood flow is cut off suddenly, often with bleeding inside the fibroid. This type is most commonly seen during pregnancy. It tends to develop more abruptly than other types.
Cystic degeneration
This develops over time, as areas of tissue breakdown turn into spaces filled with fluid within the fibroid. This usually happens after earlier degeneration has taken place.
Calcific degeneration
This type tends to occur after menopause. As oestrogen levels fall, fibroids shrink and can develop calcium deposits that cause them to harden over time. This tends to happen later on.
Knowing the type of degeneration helps your doctor understand what to expect and plan the right approach for managing your symptoms.
If your symptoms have changed suddenly or feel unusual, request an appointment with Thomson Medical. Our specialist can assess whether fibroid degeneration may be the cause and guide appropriate management.
What are the symptoms to look out for?
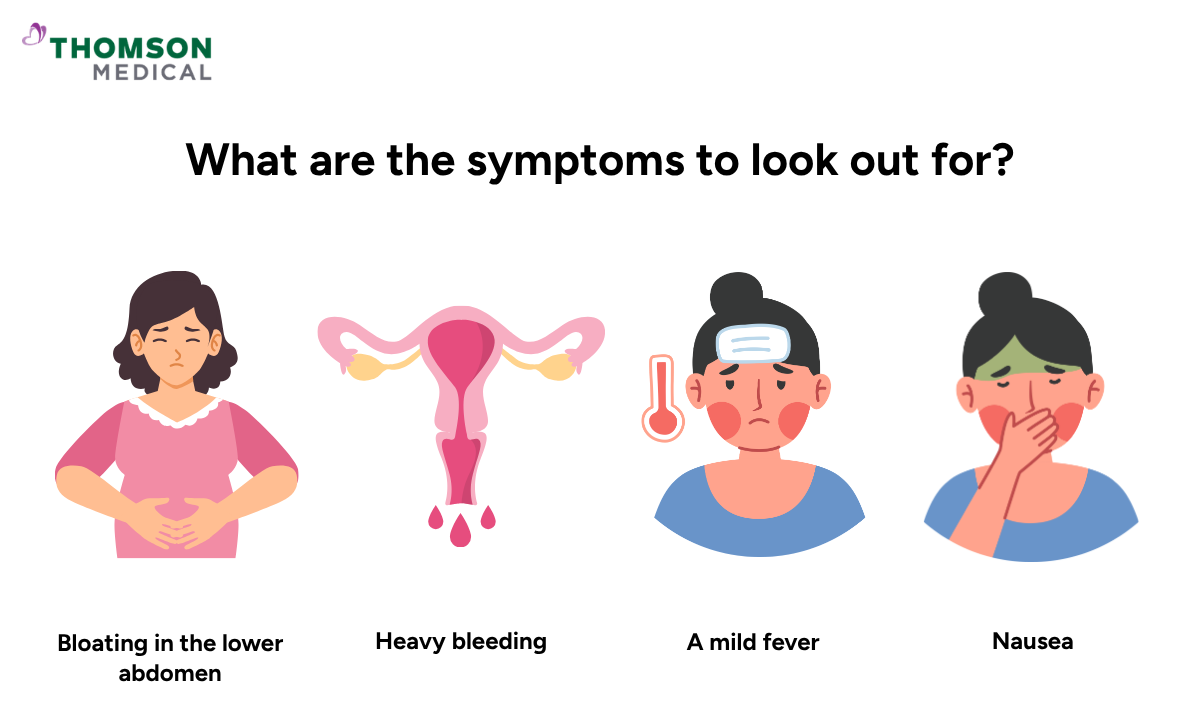
Fibroid degeneration can feel different from person to person. Some women have no symptoms, while others may notice more sudden or noticeable changes.
You might experience:
Pelvic pain that feels sharp, stabbing, or constant, and different from your usual period cramps
Tenderness when pressing on the abdomen
Mild swelling or bloating in the lower abdomen
Heavy bleeding or changes in your menstrual cycle if the fibroid affects the womb lining
A mild fever
Nausea or vomiting in more painful cases
The type of degeneration also makes a difference to what you experience. Hyaline and calcific degeneration often cause few or no symptoms, while red degeneration can be more uncomfortable, particularly during pregnancy.
If you develop sudden pelvic pain and you have fibroids, please speak with your doctor rather than waiting for it to settle.
How is fibroid degeneration diagnosed?
Your doctor will usually start with a pelvic exam to check for tenderness or changes in the size of your uterus. From there, imaging gives the clearest picture of what is happening inside.
These include:
Ultrasound scan:
Usually the first scan your doctor will arrange.
Can show changes in your fibroid's internal structure, such as irregular areas or fluid pockets.
Magnetic resonance imaging (MRI) scan:
Can identify bleeding, fluid changes, or calcium deposits within the fibroid.
MRI may help show bleeding, fluid changes or calcium deposits within a fibroid and may be used when ultrasound findings are unclear or when other causes of pain need to be considered.
Blood tests:
Your doctor may request these if there are signs of infection.
Degeneration itself does not usually cause noticeable changes in your blood results.
Because the symptoms can feel similar to other conditions such as appendicitis, ovarian cysts, or pelvic inflammatory disease, imaging helps rule these out and confirm the diagnosis.
Treatment options for fibroid degeneration
Treatment for fibroid degeneration depends on how severe your symptoms are and whether you are pregnant. In most cases, the aim is to manage discomfort while the fibroid settles on its own.
Managing mild to moderate symptoms
For many women, management focuses on staying comfortable while the fibroid settles on its own. This may include rest, hydration, and pain relief such as paracetamol or anti-inflammatory medicines, if appropriate for you.
If you are pregnant, speak with your doctor before taking any medication, including anti-inflammatory medicines such as ibuprofen, as some may not be suitable during certain stages of pregnancy. Symptoms often improve gradually over a few days to weeks.
Treatment during pregnancy
If degeneration happens while you are pregnant, your doctor will take a gentle, measured approach. The priority is safe pain relief and careful monitoring of you and your baby. Red degeneration during pregnancy, while painful, usually resolves without needing further treatment.
When symptoms are more persistent or severe
.png?branch=production)
If pelvic pain keeps coming back or your fibroids are causing ongoing problems, further treatment options may be worth exploring with your doctor.
These treatment options include:
Uterine artery embolisation (UAE):
A procedure that reduces the blood supply to your fibroids, causing them to shrink over time.
UAE may not be suitable for everyone, especially if future pregnancy is a priority. Your doctor can discuss the benefits, risks and alternatives based on your fertility plans and fibroid characteristics.
Myomectomy:
Myomectomy is a surgery to remove fibroids while keeping your uterus intact. This is often considered for women who wish to preserve their fertility.
Hysterectomy:
Hysterectomy is a surgery to remove the uterus. This is usually only considered when other treatments have not provided enough relief.
Your doctor will consider both the degeneration and the overall state of your fibroids when discussing next steps. The aim is to ease your symptoms and lower the chance of them coming back.
Concerns about fibroid size or fibroid location are best discussed with a healthcare provider who can review your scans and symptoms together. Request an appointment with Thomson Medical to better understand your condition and explore suitable next steps for care.
FAQ
Can fibroid degeneration cause cancer?
No, fibroid degeneration does not cause cancer. Degeneration simply means that part of the fibroid has lost its blood supply and started to break down, which is a benign process. Uterine fibroids themselves are benign growths.
In very rare cases, a type of cancer called uterine leiomyosarcoma can occur, but it develops on its own and is not caused by fibroid degeneration. New or rapidly enlarging pelvic masses, especially after menopause, should be assessed by a doctor.
Is fibroid degeneration dangerous during pregnancy?
Fibroid degeneration can occur during pregnancy, most commonly as red (carneous) degeneration due to changes in blood flow. While it can be quite painful, it is usually not dangerous to you or your baby.
Treatment usually involves safe pain relief, rest, and hydration. Your doctor will also check to rule out other causes of abdominal pain. In some cases, hospital observation may be needed if symptoms are severe.
Can I prevent fibroid degeneration?
There is no certain way to prevent fibroid degeneration. It usually occurs when a fibroid outgrows its blood supply or when circulation changes, such as during pregnancy or near menopause. Seeing your doctor regularly and discussing treatment options early may help reduce complications, but degeneration itself cannot be reliably prevented.
Does fibroid degeneration affect fertility?
Fibroid degeneration itself does not directly affect fertility. However, the presence of uterine fibroids, especially submucosal fibroids that distort the uterine cavity, can affect implantation and pregnancy. Your fertility is more closely related to the size, number, and location of fibroids rather than degeneration itself.
What should I avoid during fibroid degeneration?
During fibroid degeneration, it is best to avoid strenuous physical activity or heavy lifting if it worsens pelvic pain. You should also avoid taking any medication without medical advice, especially during pregnancy.
If you experience severe pain, a high fever, heavy bleeding, or unexpected vaginal bleeding, see your doctor straight away. Otherwise, light daily activities can usually continue as long as you feel comfortable.
How long does fibroid degeneration last?
The duration varies depending on the type and severity. Sudden red degeneration usually causes pain lasting from a few days up to one to two weeks. Mild discomfort may persist slightly longer in some cases.
Other types of degeneration may cause few to no symptoms and are often detected only through imaging. Most cases improve with rest and pain relief, but persistent or worsening pain should be checked by your doctor.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
