When your doctor first mentions a hysterectomy, it's natural to feel anxious about what it might mean for your body. The truth is, how a hysterectomy is performed makes a significant difference in your recovery and your comfort. The laparoscopic approach, which uses small incisions rather than one large cut, is minimally invasive. For many women, it means going home sooner and healing faster than they expected.
If you've been considering a laparoscopic hysterectomy in Singapore, knowing what to expect at every stage can help you make an informed decision about your care.
What is a laparoscopic hysterectomy?
A hysterectomy is a surgical procedure to remove the uterus. It’s most commonly recommended to treat gynaecological conditions such as fibroids, endometriosis, uterine prolapse, and gynaecological cancers.
If your doctor suggests a hysterectomy, they might recommend using a laparoscopic approach.
A normal open surgery involves making a large abdominal cut to give the surgeon direct access to the area being treated.
However, during a laparoscopic procedure, your surgeon makes just a few small incisions in your abdomen and uses a tiny camera (laparoscope) along with specialised instruments to carefully remove your uterus. Depending on your condition and the reason for surgery, your surgeon may also remove your cervix, fallopian tubes, or ovaries.
Compared to open (abdominal) hysterectomy, the laparoscopic approach means:
Less pain after surgery
A shorter hospital stay
Smaller scars
A faster return to daily life
For many women, that difference is exactly what makes the laparoscopic approach worth considering.
What types of laparoscopic hysterectomies are available in Singapore?
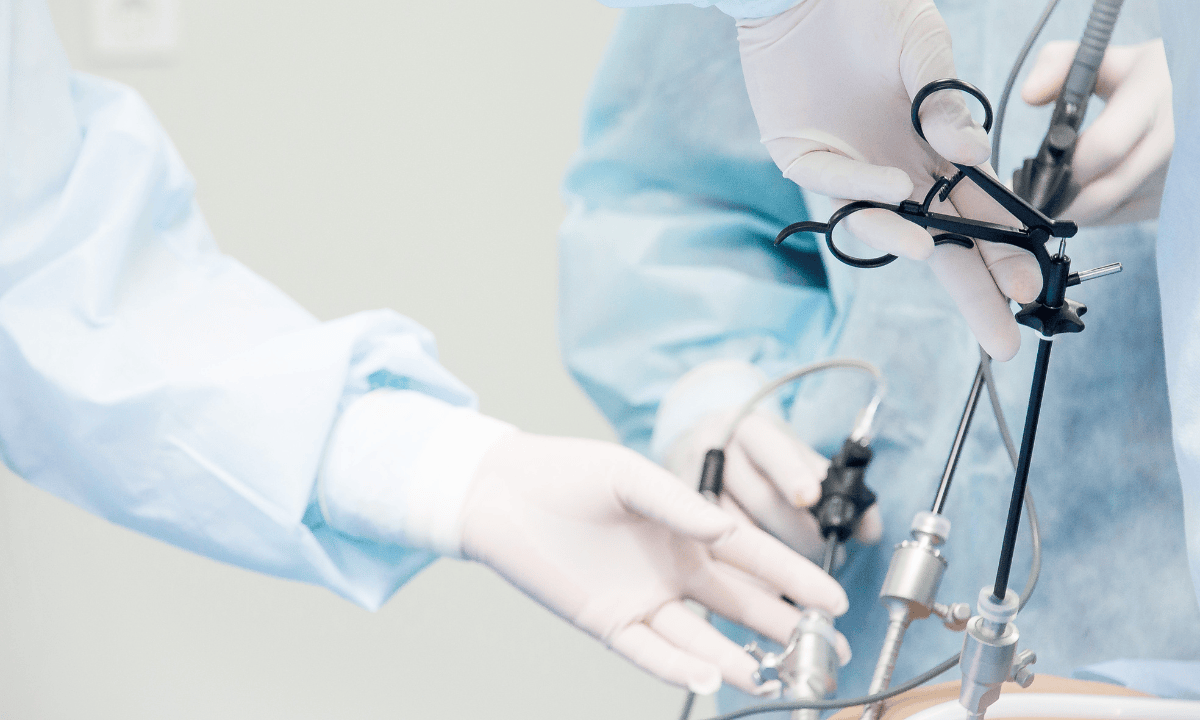
Not all laparoscopic hysterectomies are the same. Your surgeon will recommend a specific type based on your condition and what needs to be removed. In Singapore, there are three main approaches available.
Total laparoscopic hysterectomy (TLH)
This is the most common form. The entire uterus, including the cervix, is removed through the small incisions on your abdomen. Your surgeon may also remove the fallopian tubes and/or ovaries if needed, depending on your diagnosis.
Laparoscopic supracervical hysterectomy (LSH)
This surgery only removes the upper portion of the uterus while leaving the cervix intact. You may also have your fallopian tubes and ovaries removed at the same time. This option may be suitable for you if you wish to retain your cervix and do not have cervical disease.
Laparoscopic-assisted vaginal hysterectomy (LAVH)
This approach combines laparoscopy with vaginal access. The laparoscope is used to detach the upper connections of the uterus, and the lower portion is removed through the vaginal canal. It’s a useful option when vaginal access is feasible and appropriate for your situation.
Your surgeon will carefully review your condition and walk you through which approach is right for your individual needs. It’s always worth asking questions until you feel clear and comfortable with the plan.
If you're unsure which type of laparoscopic hysterectomy is right for you, schedule an appointment with Thomson Medical for a personalised consultation.
Who is suitable for a laparoscopic hysterectomy?
Your surgeon may recommend a laparoscopic hysterectomy if you’re dealing with benign (non-cancerous) conditions, including:
Symptomatic uterine fibroids
Endometriosis
Adenomyosis
Uterine prolapse
Chronic pelvic pain that doesn’t improve with medication
Abnormal uterine bleeding that is not responding to medical treatment
It may also be a good option if:
You’ve been diagnosed with early-stage gynaecological cancers, such as endometrial or cervical cancer
You prefer a shorter recovery time
You’re in good overall health and have a general surgical history
That said, every situation is different. The most important step is to have an honest, open conversation with your surgeon. They will explain your options and discuss your concerns so that together, you can make a decision that feels right for you.
Gynaecologists at Thomson Medical
Loading...
A laparoscopic hysterectomy procedure: what to expect
Going into surgery always brings up questions and sometimes anxiety. Knowing what to expect at each stage can make the experience feel less uncertain and more at ease.
What happens before a laparoscopic hysterectomy?
Before your surgery, you’ll have a comprehensive preoperative consultation with your surgeon.
This is when they’ll review your medical history and perform a physical and pelvic examination. You can expect imaging tests such as ultrasound or MRI scans, along with blood tests, to help your surgeon plan the procedure.
If you’re taking supplements or medications, let your surgeon know, as some might affect the outcome of your surgery.
You’ll also meet your anaesthetist to discuss your anaesthesia options, including the risks, benefits, and possible alternatives. Your care team will give you specific instructions on fasting, medications, and hospital admission before the surgery.
If you have any concerns, don’t hesitate to bring them up. This is your chance to feel prepared.
What happens during a laparoscopic hysterectomy?
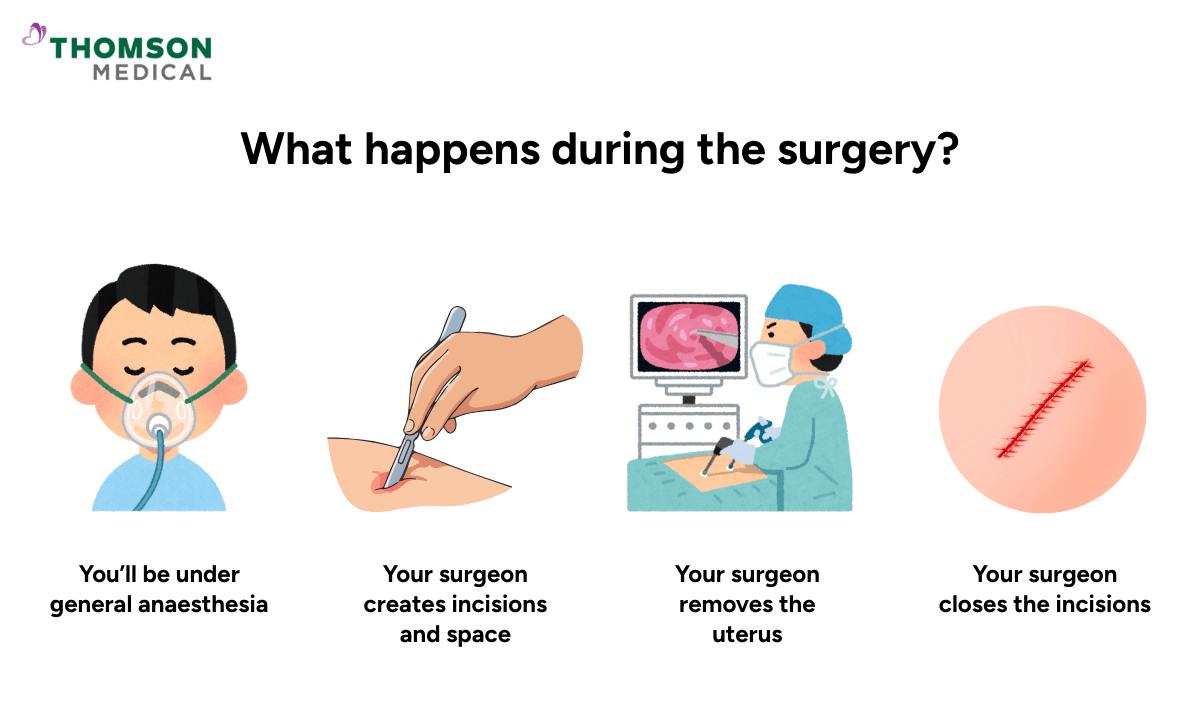
The surgery is performed under general anaesthesia, which means you’ll be asleep throughout and won’t feel anything.
Here is what your surgeon will do:
Your surgeon creates a small incision near your belly button to insert a camera, along with a few additional small cuts in your lower abdomen for surgical instruments.
Some carbon dioxide gas will be introduced into your belly to create space and give your surgeon a clear view inside your pelvic organs.
Your surgeon will remove the uterus either vaginally or through one of the cuts in your belly.
Once the procedure is complete, your surgeon will close the incisions with stitches or skin glue.
The surgery typically takes between one and three hours. Your hospital stay will depend on how your procedure goes and how your recovery progresses. Some women return home on the same day, while others may stay for one to three days.
What can I expect after a laparoscopic hysterectomy?
The first few days after surgery, it’s completely normal to feel more tired than usual. Your body has just been through surgery, so you are encouraged to rest more during this recovery time. Most women will feel more like themselves within a few weeks.
You should be able to resume normal activities around 3 to 4 weeks after the surgery.
In the meantime, your surgeon may advise you to avoid:
Sexual intercourse for at least 4 to 6 weeks
Heavy lifting for at least 6 weeks
Driving for 2 to 3 weeks
A few side effects that are normal and expected in recovery include:
Shoulder pain due to the gas used during surgery
Some pain and discomfort in your lower abdomen
Slight vaginal bleeding, similar to a light period
No bleeding at first, followed by a sudden gush of old blood or fluid after surgery
Everyone heals at a different pace, and if you need more time, that’s completely normal. If you feel unsure about what you’re experiencing during your recovery, don’t hesitate to check with your care team. They will help you understand what’s happening and address any concerns promptly.
What side effects or potential risks should I be aware of?
Laparoscopic hysterectomy is widely considered a safe and effective procedure, and most women recover without significant complications. However, like any surgical procedure, there are some side effects and risks you should be aware of.
Side effects
Most side effects after a laparoscopic hysterectomy are common and temporary. They happen as part of the normal recovery process.
You may experience:
Pain from the surgery and the gas used during the procedure
Vaginal bleeding for up to 6 weeks after surgery
Fatigue
Bowel and bladder changes such as constipation and difficulty urinating
Nausea and vomiting from general anaesthesia
Menopausal symptoms if the ovaries are removed
If any symptoms feel severe or don’t improve with time, let your care team know.
Potential risks
Complications are uncommon, but your surgeon will discuss these with you:
Infection
Bleeding
Injury to nearby organs, such as the bladder or bowel
Blood clot formation
Conversion to open surgery if technical difficulties arise during laparoscopic surgery
Your surgeon will go through all of this with you before your operation. If anything feels off during your recovery, it’s always better to get checked.
If you have concerns about the risks involved or simply want to know what to expect, schedule an appointment with Thomson Medical. Our specialists will take the time to address your questions and help you feel confident going into surgery.
How much is a laparoscopic hysterectomy in Singapore?
The cost of a laparoscopic hysterectomy in Singapore varies depending on different factors, including:
The type of procedure
Hospital choice: public or private hospital
Your residency status: Singapore citizen, permanent resident or foreigner
Generally, the cost ranges from SGD 8,000 to SGD 20,000. Medisave and private insurance may cover a significant portion of these costs, depending on your policy and the medical necessity of the procedure. It is worth checking with your insurer to understand what your plan covers before your procedure.
For an accurate cost estimate specific to your situation, it’s best to check with your care team or hospital admissions team. They will walk you through the expected costs and available payment options so you can plan ahead with confidence.
Please note that these costs are based on 2026 rates and may vary over time.
FAQ
Who qualifies for a laparoscopic hysterectomy?
Laparoscopic hysterectomy is suitable for women with benign conditions such as symptomatic fibroids, adenomyosis, endometriosis, uterine prolapse, or abnormal vaginal bleeding that hasn’t responded to medical treatments.
It may also be suitable for early-stage gynaecological cancers.
How many days of rest are required after a laparoscopic hysterectomy?
Most women need about 2 to 3 weeks of rest before they start feeling better and can usually return to normal activities around three to four weeks after surgery.
What alternatives are there to a hysterectomy?
Depending on your condition, there are several alternatives to hysterectomy, including:
Medical treatments:
Non-steroidal anti-inflammatory drugs (NSAIDs) and hormonal treatments are used to treat heavy menstrual bleeding, endometriosis, fibroids, and chronic pelvic pain.
Myomectomy:
This is a surgical procedure that removes fibroids while preserving the uterus.
Uterine artery embolisation (UAE):
A non-invasive procedure in which your doctor injects small particles into the blood vessels that supply your uterine fibroid, while preserving your uterus.
Endometrial ablation:
This uses various methods, such as thermal balloon, cryoablation, or radiofrequency ablation, to remove the lining of your uterus to treat heavy menstrual bleeding.
What age is recommended for a hysterectomy?
There is no age limit for a hysterectomy. Most hysterectomies are performed in women between the ages of 30 and 50 for various reasons, such as fibroids, endometriosis, chronic pelvic pain, abnormal uterine bleeding, and gynaecological cancers.
Will I go into menopause after a hysterectomy?
No, you will not go into menopause after a hysterectomy. However, if the surgery involves the removal of the ovaries, you are likely to experience menopausal symptoms because the ovaries produce female reproductive hormones such as oestrogen and progesterone.
Is laparoscopy a high-risk surgery?
Laparoscopic hysterectomy is generally considered lower risk than open abdominal surgery, with fewer complications, less blood loss, and faster recovery.
Risks do exist, but serious complications are uncommon. Your surgical team will discuss your individual risk profile with you before the procedure.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and advice based on your unique situation, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) - Jurong:
6262 8588 (Call), 6262 8588 (WA) - Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
Notice
The range of services may vary between TWC/TS locations. Please contact your preferred branch directly to enquire about the current availability.
Request an Appointment