Learning that you need laparoscopic surgery can bring up a lot of feelings at once. At the same time, questions about the different types of laparoscopic surgery, recovery time, scarring, and what to expect are all completely natural.
Knowing what to expect, from the type of procedure involved to what recovery looks like, can help you feel more informed and prepared going into your operation.
What is laparoscopic surgery?
Laparoscopic surgery is a type of minimally invasive surgery. Instead of one large cut, your surgeon makes 2 to 5 small keyhole incisions, each usually 1 to 2 cm long.
A thin, flexible camera called a laparoscope is gently inserted through one of these small openings. It sends a magnified, real-time image to a video monitor, giving your surgeon a detailed view of your internal organs. This technique can be used across many areas of your body, including your abdomen, pelvis, and chest.
Why is laparoscopic surgery used?
While open surgery requires a large incision to give the surgeon direct access to the area being treated, laparoscopic surgery achieves the same goal through much smaller openings. This means less disruption to the surrounding tissue.
Your doctor chooses laparoscopic surgery when:
Your condition can be safely treated without wide surgical access
The area being treated is accessible through small incisions
Reducing surgical trauma and recovery time is a priority
You are in good enough health for the procedure
Your doctor will consider your overall health, your condition, and the nature of your surgery to determine whether the laparoscopic surgical approach is appropriate for you.
Our gynaecologists
Loading...
What are the types of laparoscopic surgery?
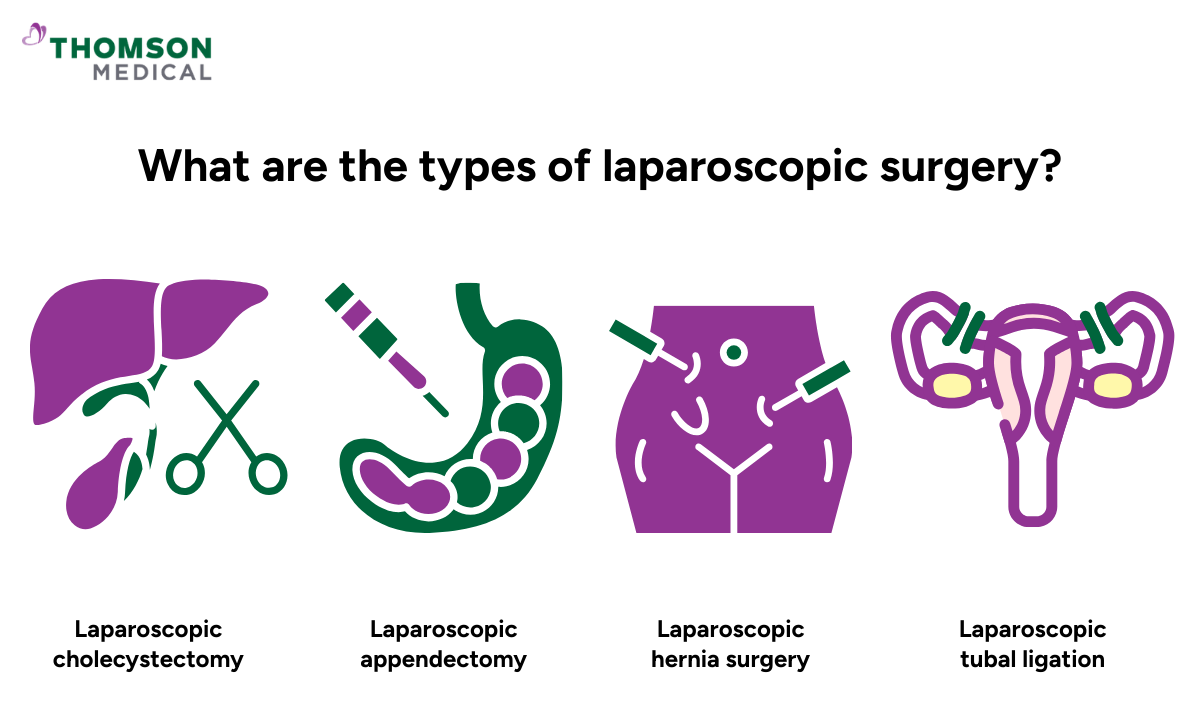
Laparoscopic surgery is very flexible. Your doctor uses the same basic method but adjusts it depending on the type of surgical procedure you need.
Laparoscopic cholecystectomy
Laparoscopic cholecystectomy is the surgical removal of the gallbladder and is one of the most frequently performed laparoscopic procedures. The gallbladder is a small organ that sits under your liver. It stores bile, a fluid that helps your body digest fat. If it becomes blocked or inflamed, removing it is often the recommended treatment.
It may be recommended for:
Gallstones
Gallbladder inflammation
A gallbladder that is not working properly
Most people are able to live normally without a gallbladder. After surgery, bile flows directly from your liver into your small intestine. Most people do not notice any major changes in digestion once they have fully recovered.
Laparoscopic appendectomy
This surgical procedure removes your appendix and is most often done to treat acute appendicitis. When your appendix becomes inflamed, it can cause sudden abdominal pain. Your doctor will act promptly to prevent the infection from spreading. With a laparoscopic approach, this can usually be done safely and with minimal disruption to your body.
Your surgeon can also see your entire abdomen clearly during the procedure, which allows them to check for other possible causes of your pain at the same time.
Once you have recovered, the absence of your appendix will not affect your longer-term health or digestion.
Laparoscopic hernia surgery
This surgery is used to repair weaknesses in the abdominal wall that allow internal tissue to push through. You might notice a soft lump, and it can feel uncomfortable when you lift, cough, or bend.
However, not all hernias need surgery right away. If your hernia causes ongoing discomfort, grows larger, or becomes trapped, your doctor may suggest a hernia repair to prevent further problems.
Laparoscopic surgery can fix different types of hernias, such as inguinal (groin), femoral (upper thigh), and ventral (abdominal wall). It may be especially useful if you have hernias on both sides or have had previous hernia surgery.
Laparoscopic hysterectomy
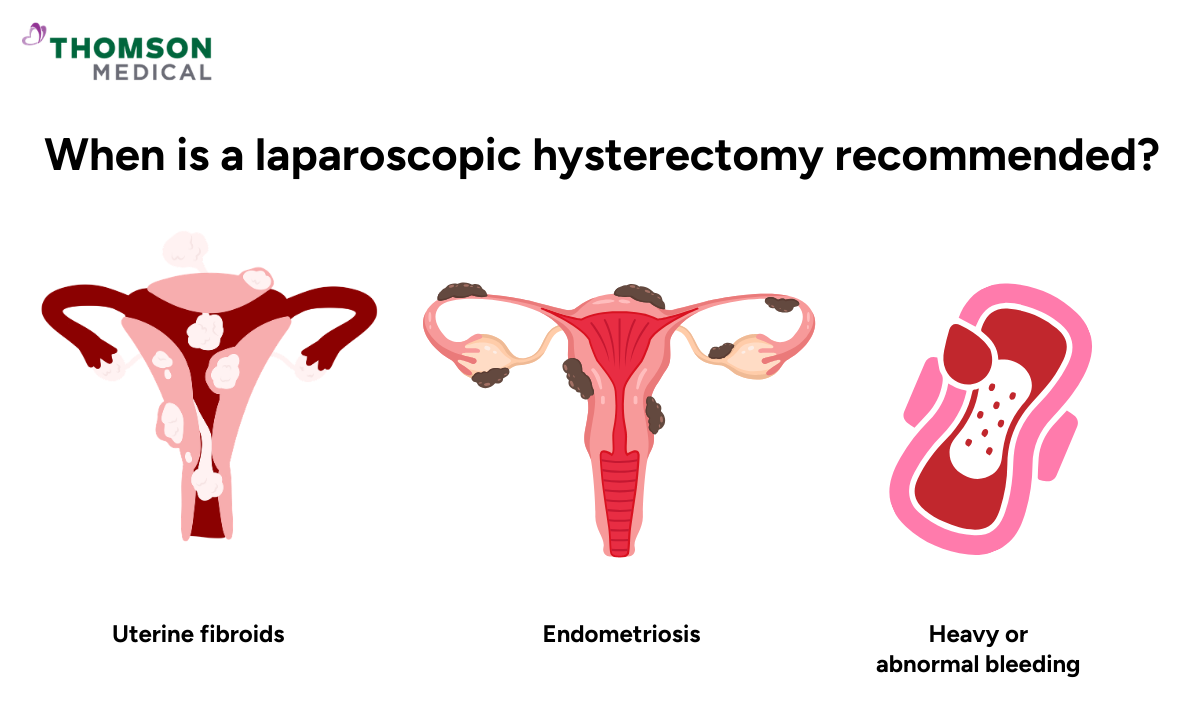
A hysterectomy is a gynaecological surgery to remove your uterus (womb). It is usually considered when your symptoms are affecting your daily life and other treatments have not provided sufficient relief.
It may be recommended if you have:
Endometriosis
Heavy or abnormal bleeding
Early-stage uterine cancer
There are two main approaches your doctor may discuss with you:
Total laparoscopic hysterectomy:
Your uterus is removed completely through small incisions in the abdomen.
Laparoscopic-assisted vaginal hysterectomy:
Your uterus is first freed using small abdominal incisions, then removed through the vagina.
Your doctor will work with you to choose the approach that feels right for your situation, recognising that a hysterectomy can be a very personal decision. The recommendation will be based on the size and position of your uterus, any scar tissue from previous surgery or endometriosis, and whether your cervix needs to be removed.
Laparoscopic tubal ligation
This surgical procedure permanently prevents pregnancy by blocking or sealing your fallopian tubes. It is one option your doctor may discuss with you if you are certain that you do not want future pregnancies.
Tubal ligation is intended to be a permanent solution, so it is worth taking the time to feel fully confident before going ahead. Reversal is sometimes possible, but success is not guaranteed, and your doctor will talk this through with you carefully.
Laparoscopic endometriosis surgery
Endometriosis happens when tissue similar to the lining of your uterus grows outside your uterus, usually in your pelvis. It can lead to ongoing pelvic pain, heavy periods, and sometimes difficulty getting pregnant.
Laparoscopy is the standard approach for both diagnosing and treating endometriosis. During the procedure, your surgeon can remove or destroy the affected tissue directly.
Surgery will not cure endometriosis, but it may help reduce the symptoms you are experiencing. Your doctor will work with you on an ongoing plan, which may include medication, regular check-ins, or further surgery if your symptoms come back.
Laparoscopic colorectal surgery
Laparoscopic colorectal surgery treats conditions affecting your colon, rectum, or both. Traditionally, these operations required large incisions, but the laparoscopic approach allows your surgeon to perform colon resections with smaller cuts, causing less disruption to your body.
This type of surgery may be recommended if you have:
Colorectal cancer
Diverticular disease (a condition where small pouches form in the wall of the colon and become inflamed or infected)
Inflammatory bowel diseases such as Crohn's disease or ulcerative colitis
Recovery from colorectal surgery usually takes longer than some other laparoscopic procedures, often several weeks. Your care team will support you through this process and help you understand what to expect at each stage.
Laparoscopic bariatric surgery
Bariatric surgery may be an option for you if you are living with obesity and related health conditions, such as type 2 diabetes, high blood pressure, or sleep apnoea, that have not improved with lifestyle changes alone.
The surgery works by reducing the size or changing the function of your stomach and, in some cases, adjusting your digestive tract.
Common procedures include:
Laparoscopic sleeve gastrectomy:
A part of your stomach is removed to reduce its size
Laparoscopic gastric bypass:
Your digestive system is rerouted to limit food intake and absorption.
Many people experience meaningful weight loss after surgery, and some also see improvement in related conditions such as type 2 diabetes and high blood pressure.
Your doctor and dietitian will guide you on what to eat before and after surgery, and your follow-up appointments will help track your progress and support any nutritional needs along the way.
For personalised guidance on the type of laparoscopic surgery that may be suitable for your condition, request an appointment with Thomson Medical. Our specialists can assess your situation, explain the options, and help you understand what to expect before, during, and after your procedure.
What are the benefits of laparoscopic surgery?
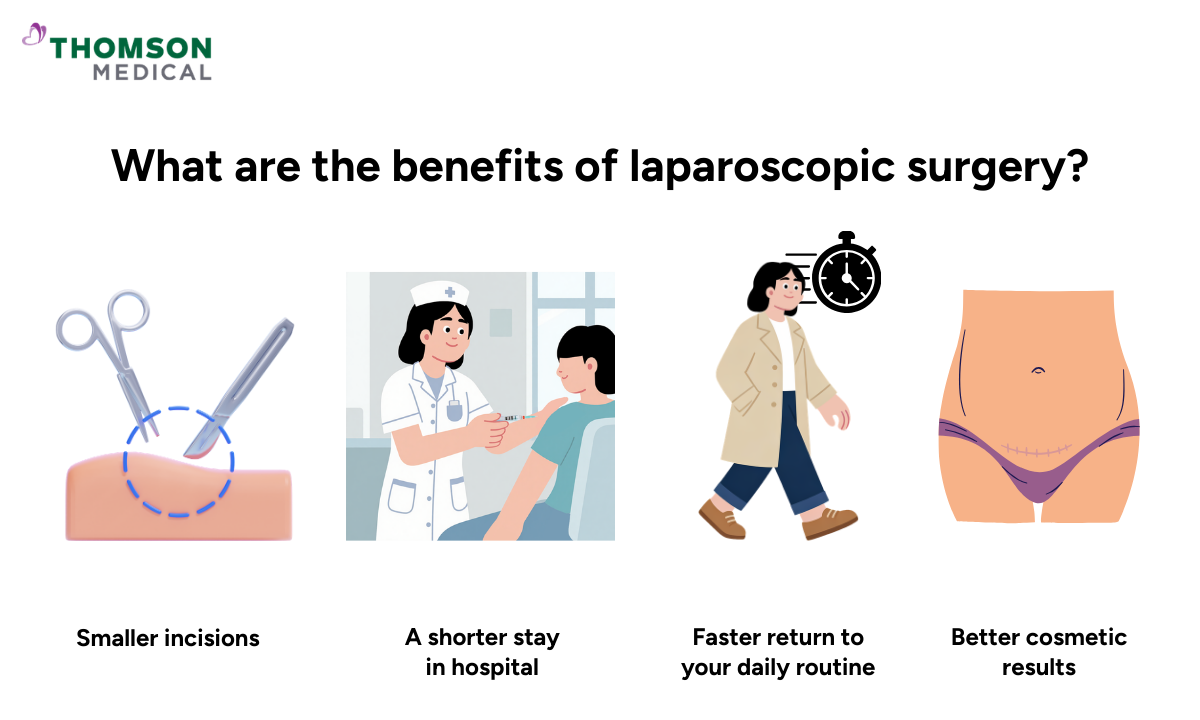
Laparoscopic surgery is widely used because it may offer a more comfortable recovery and a gentler experience overall.
With this approach, you may experience:
Smaller incisions and less noticeable scars
Less pain after the procedure
Reduced blood loss during surgery
A shorter stay in hospital
Faster return to your daily routine
Lower risk of infection
These benefits mean you’ll usually recover more comfortably and get back to your normal activities sooner.
What are the risks of laparoscopic surgery to consider?
It is natural to have questions about surgical risks, and your doctor will go through these with you in detail before your operation. The risks involved will depend on the type of procedure and your overall health.
Possible risks include:
Bleeding during or after surgery
Infection
Accidental injury to nearby organs
Blood clots
Complications related to anaesthesia
The need to convert to open surgery if the laparoscopic approach is not safe to continue
Your surgical team will assess your personal risk and take steps to reduce complications, including careful anaesthetic planning and close postoperative care monitoring. You will have the chance to ask questions and share any concerns before you decide to proceed.
When laparoscopic surgery may not be suitable
Laparoscopic surgery is not suitable in every situation. There are specific clinical factors that may make open surgery a safer or more effective option for you.
Your doctor may recommend a different approach if:
You have significant scar tissue from previous abdominal surgery
You have certain heart or lung conditions that could be affected by the procedure's positioning or gas used
Your surgery requires a wider view or access than laparoscopy allows
Active bleeding needs to be brought under control first
Your condition, such as cancer, requires more extensive access
Sometimes, a procedure that starts laparoscopically may need to be converted to open surgery during the operation. This is a deliberate decision your surgeon makes to keep you safe and not a sign that something went wrong. Your team will explain this possibility before your surgery.
If you want to understand the potential risks and whether laparoscopic surgery is suitable for you, request an appointment with Thomson Medical. Our specialists can review your health, discuss possible complications, and guide you on the safest approach for your procedure.
FAQ
Is laparoscopic surgery always better than open surgery?
Not always. Laparoscopic surgery offers many advantages, but open surgery may be the safer choice in more complex cases or when your surgeon needs wider access to the affected area. Your doctor will recommend the approach that is most appropriate for your specific situation.
Are all abdominal surgeries suitable for laparoscopy?
Not all abdominal procedures can be performed laparoscopically. Some complex or emergency situations may require open surgery. Surgical techniques continue to develop, and your doctor will advise on the most appropriate approach for your condition.
How long does recovery usually take?
Recovery varies depending on the type of surgery and how your body heals. For many laparoscopic procedures, people return to their normal activities within one to three weeks, though recovery from more complex operations may take longer.
Is laparoscopic surgery safe for older people?
Yes, in many cases. Older people can benefit from the reduced pain and shorter recovery period that laparoscopic surgery offers. However, your doctor will carefully review your overall health and any existing medical conditions before making a recommendation.
Can laparoscopic surgery be converted to open surgery?
Yes, and this is not uncommon. If your surgeon encounters poor visibility, unexpected findings, or needs to manage bleeding more effectively, they may decide to convert to open surgery during the procedure. This decision is always made with your safety in mind.
Will laparoscopic surgery leave scars?
Yes, but the scars are generally small and tend to fade over time. Most people find them barely noticeable once fully healed.
How will I know which laparoscopic procedure I need?
Your doctor will discuss the suitable procedure with you based on your diagnosis, any imaging results, your medical history, and your overall health. If you have any concerns or questions after your consultation, do not hesitate to ask your doctor for further clarification.
The information is intended for general guidance only and should not be considered medical advice. For personalised recommendations and advice based on your unique situation, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) - Jurong:
6262 8588 (Call), 6262 8588 (WA) - Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
Notice
The range of services may vary between TWC/TS locations. Please contact your preferred branch directly to enquire about the current availability.
Request an Appointment