Many women face hysterectomy after years of heavy bleeding, pelvic pain, or fibroids. While the goal is to improve your health, questions about desire and physical intimacy are common.
For most women, quality of life improves once the original symptoms are gone. Understanding what changes to expect during recovery can help you feel more prepared and confident moving forward.
What is a hysterectomy?
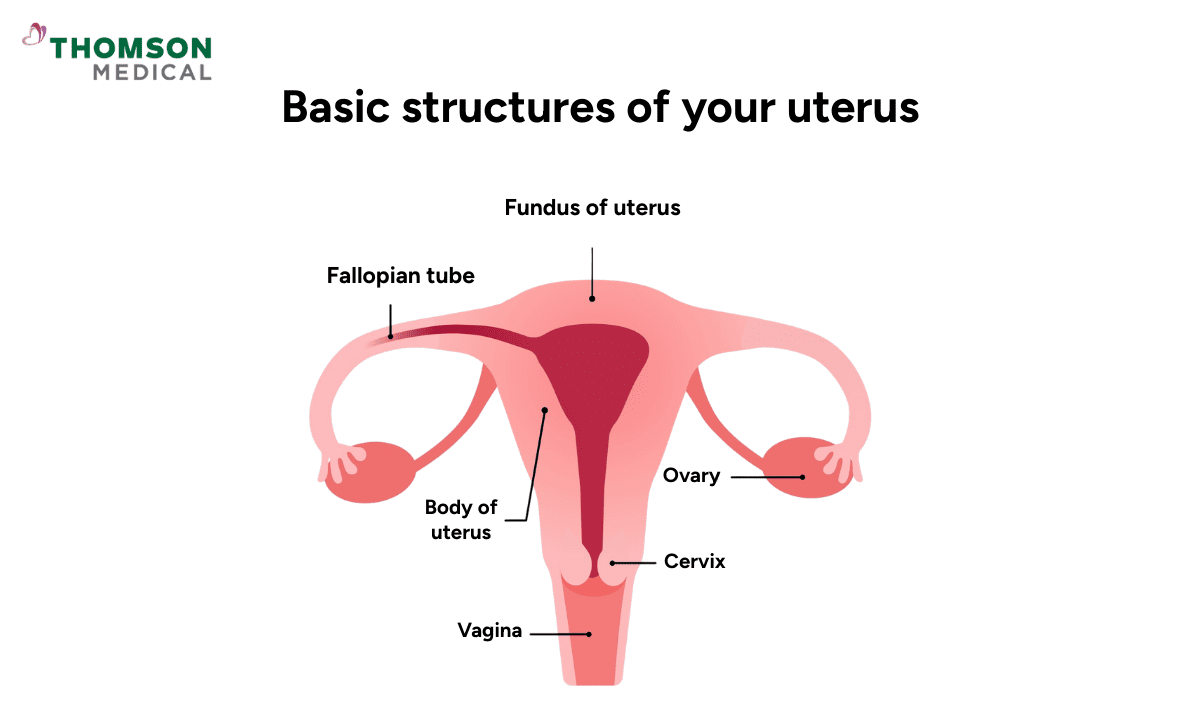
A hysterectomy is a surgical procedure to remove your uterus. Depending on your specific health needs, such as a diagnosis of cervical cancer or ovarian cancer, your surgeon may also need to remove other parts such as your ovaries to protect your long-term health.
The type of hysterectomy you have affects which parts are removed and how your body responds during recovery.
Common types of the procedure include:
Total hysterectomy:
Your surgeon removes the entire uterus and the cervix
Supracervical hysterectomy:
Also known as a partial hysterectomy, your surgeon removes the upper part of your uterus but leaves the cervix in place.
Hysterectomy with salpingo-oophorectomy:
This involves removing one or both ovaries and your fallopian tubes.
Radical hysterectomy:
Often performed for cancer, this involves removing the uterus, cervix, and surrounding tissues, which may include nearby lymph nodes.
The surgical approach your doctor uses also affects how quickly you heal. These can include an abdominal hysterectomy, which requires a larger incision, or more minimally invasive options like a vaginal hysterectomy or laparoscopic hysterectomy.
Laparoscopic surgery typically allows for a shorter hospital stay and faster overall recovery, letting you return to your daily routines sooner.
How does surgery affect your sex life?

Your sexual life after surgery is influenced by both physical changes and how you feel emotionally about those changes. It is helpful to remember that every woman’s experience is unique, and your body may need time to adjust.
Physical changes to the vaginal canal
If you have a total hysterectomy, your surgeon removes your cervix and closes the top of your vaginal canal with stitches. This closure is called a vaginal cuff.
Because the cervix is no longer there, the overall length of your vaginal canal may become slightly shorter. The vagina is naturally very elastic and adaptable, so most people continue to have comfortable sexual activity after healing.
Most women find that once healed, intercourse feels normal. You might need to experiment with positions to find what's most comfortable, especially in the first few months.
These changes are usually subtle. Giving your body enough time to recover and following your doctor’s guidance about when to resume intercourse can help you feel more comfortable and confident as you heal.
Hormone levels and vaginal dryness
If your ovaries were removed during your surgery, your body will experience a sudden drop in oestrogen. Your body will experience surgical menopause, which often brings a few noticeable symptoms.
Some symptoms include:
Vaginal dryness:
Thinner, less lubricated vaginal tissues can make intercourse uncomfortable or sensitive.
Hot flushes:
Sudden waves of heat and sweating can affect your general comfort and sleep quality.
Changes in sexual desire (libido):
Lower hormone levels may lead to a temporary decrease in your libido.
These hormonal shifts can feel overwhelming at first, but they are manageable with the right support. Understanding that these are normal responses of your body can help you and your partner approach this topic with patience.
If you are experiencing vaginal dryness, hot flushes, or changes in libido after surgery, it is important to seek medical advice to explore supportive treatment options. You may arrange a consultation with Thomson Medical to discuss personalised care for managing surgical menopause symptoms.
Nerve and blood flow changes
Your pelvic area contains nerves and blood vessels that support arousal, lubrication, and orgasm. Surgeons aim to protect these during a hysterectomy, but it is still common to notice temporary changes while your body heals.
You might feel that:
It takes longer than usual to feel turned on
You need more direct or sustained touch to feel aroused
Certain spots inside the vagina feel less sensitive than before
The top of your vagina feels different during penetration
Orgasms may feel stronger, softer, or simply unfamiliar at first.
There is mild numbness or a “dull” sensation in the early weeks
These experiences are often linked to swelling and healing. As your body recovers, sensation commonly becomes more familiar again.
For many women, clitoral stimulation remains a dependable way to reach orgasm, since the nerves connected to your clitoris are usually not directly affected by hysterectomy.
When is it safe to have sex again?
After a hysterectomy, most doctors suggest waiting about six to eight weeks before having penetrative sex. This gives the top of your vagina, where it has been closed with stitches, time to heal properly and lowers your risk of infection or other complications such as blood clots.
In the early weeks, it is common to feel more tired than usual or to notice some mild pelvic discomfort. Your energy and comfort levels can vary from day to day, and that is a normal part of recovery.
If you are unsure about when it is safe to resume sexual activity or have concerns during your recovery, you may schedule a consultation with Thomson Medical to receive guidance tailored to your healing progress.
Managing sexual dysfunction and discomfort
Finding that sexual intercourse is painful or that your desire has changed can be stressful. However, there are many treatment options and strategies to help you feel like yourself again.
Addressing vaginal dryness
Using a high-quality, water-based lubricant can make a significant difference if you are experiencing dryness.
For more persistent symptoms, your doctor might suggest a few medical options:
Hormone replacement therapy (HRT):
This can help manage broad menopause symptoms like hot flashes and mood changes.
Vaginal oestrogen:
Creams, tablets, or rings applied directly to your vaginal canal can safely restore moisture and elasticity to the tissues.
Strengthening the pelvic floor
The pelvic floor muscles support your bladder and bowel, and they also play an important role in sexual function. After surgery, these muscles can feel weaker or less coordinated for a while.
Gentle pelvic floor exercises, often called Kegel exercises, may help you:
Increase blood flow to the pelvic region to aid in nerve healing
Improve muscle tone and control for better sensation during intimacy
Reduce the risk of urinary incontinence when laughing or sneezing
A physical therapy consultation can provide you with a tailored programme for these exercises. Working with a professional ensures you are isolating the right pelvic floor muscles and actively supporting your long-term recovery.
Rebuilding intimacy at your own pace
You do not have to jump straight back into penetrative intercourse. Take things slowly and focus on other forms of intimacy with your partner as you rebuild your confidence.
Communication:
Talk openly with your partner about your concerns, boundaries, or any physical discomfort you are feeling.
Explore non-penetrative sexual intercourse:
Sensual massage, kissing, and manual stimulation can help you reconnect without putting any pressure on the surgical site.
Try intimate toys:
Vibrators or other aids can help increase blood flow and sensitivity as you become comfortable with touch again.
Letting go of the pressure to perform can create space for curiosity and comfortable exploration. When you slow things down and focus on gentle touch, you give yourself the chance to rebuild intimacy at a pace that feels safe. You may find that this gradual approach leads to more satisfying sexual intercourse in the long run.
These adjustments often help you feel more in control of their recovery and more connected to your partners during a vulnerable time.
When to seek medical advice
While you may expect some physical changes, certain symptoms require a prompt check-up with your specialist.
Reach out to your doctor immediately if you experience:
Severe or worsening pelvic pain that does not improve with rest or prescribed medication
Unusual vaginal discharge or a noticeable foul smell
Bright red vaginal bleeding after the initial postoperative recovery period
Sudden leg swelling or chest pain, which could indicate a medical emergency
These symptoms do not always mean something serious, but they do need medical review. Getting clarity early can help address any underlying issue quickly and give you reassurance as you continue healing.
Our O&G specialists
Loading...
Protecting your long-term health
Resuming your sexual life is just one part of your journey after a hysterectomy. Maintaining healthy, consistent habits will support your overall wellbeing and sexual function for years to come.
A few habits that specifically support sexual recovery include:
Staying active to keep your circulation healthy, boost your mood, and maintain your energy levels.
Drinking plenty of water and eating nutrient-rich foods to support tissue healing and hormonal balance.
Attending your scheduled medical screenings and discussing any ongoing concerns with your care team, even after a hysterectomy.
These everyday choices may seem simple, but over time they help protect your body adapt to its new normal. Feeling physically well often lays the groundwork for feeling comfortable, confident, and at ease in your intimate life too.
FAQ
Is sexual intimacy still possible after a hysterectomy?
For many women, sexual pleasure is still possible. Some women even find intimacy more comfortable if surgery has relieved long-standing pain or heavy bleeding. You may notice temporary changes in sensation while your body heals, but these often improve with time.
Will my partner notice a difference?
In most cases, your partner is unlikely to notice significant physical changes. If you experience dryness or increased sensitivity, intimacy may feel different at first. Small adjustments and open communication can help you both feel more comfortable.
Can intimacy feel uncomfortable after surgery?
You might experience some discomfort in the early stages of healing. Ongoing discomfort can sometimes be linked to dryness, scar tissue, or hormonal changes. If symptoms persist or concern you, seeking medical advice is important to rule out underlying causes.
Does a hysterectomy affect sexual desire?
Your libido can be influenced by hormone levels, emotional wellbeing, and how your recovery progresses. If your ovaries were removed, you may experience hormonal shifts that affect desire. On the other hand, you may notice an improvement in sexual interest if previous symptoms have resolved.
Is hormone therapy necessary?
Hormone therapy is not necessary for everyone. If you are experiencing symptoms such as vaginal dryness or broader menopausal changes, you may wish to discuss possible treatment options with a qualified healthcare professional. The decision depends on your individual health history and needs.
When can you resume sexual activity?
Many women are advised to wait around six weeks before resuming vaginal intercourse to allow internal healing. Your recovery timeline may vary depending on the type of surgery you had and how your body heals.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Fertility Centre
- Paragon: 6252 7766
- Novena: 6399 3758, 8811 0358 (WA)
Thomson Specialists (Women's Health)
Thomson Women's Clinic
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
