You've heard the term BRCA2 – maybe from a doctor, maybe after a relative's diagnosis – and now many questions start coming: “Am I at risk? Does this mean cancer? What am I supposed to do with this?”
The worry and uncertainty can feel overwhelming, especially if you weren't prepared.
BRCA2 is a gene everyone has, and it only becomes a concern when a change, or mutation, develops in it. Understanding what BRCA2 actually is and what a mutation does and doesn't mean for your health can take a lot of weight off your shoulders.
What is the BRCA2 gene?
The BRCA2 gene is one of the genes everyone naturally carries. Normally, it works quietly to repair damaged DNA and keep cell growth under control, protecting you against certain types of cancer.
However, in some cases, this gene can carry a mutation that stops it from working properly. When the protective function is weakened, cells can grow and divide unchecked, potentially increasing the risk of certain cancers developing.
What is the difference between BRCA1 and BRCA2?
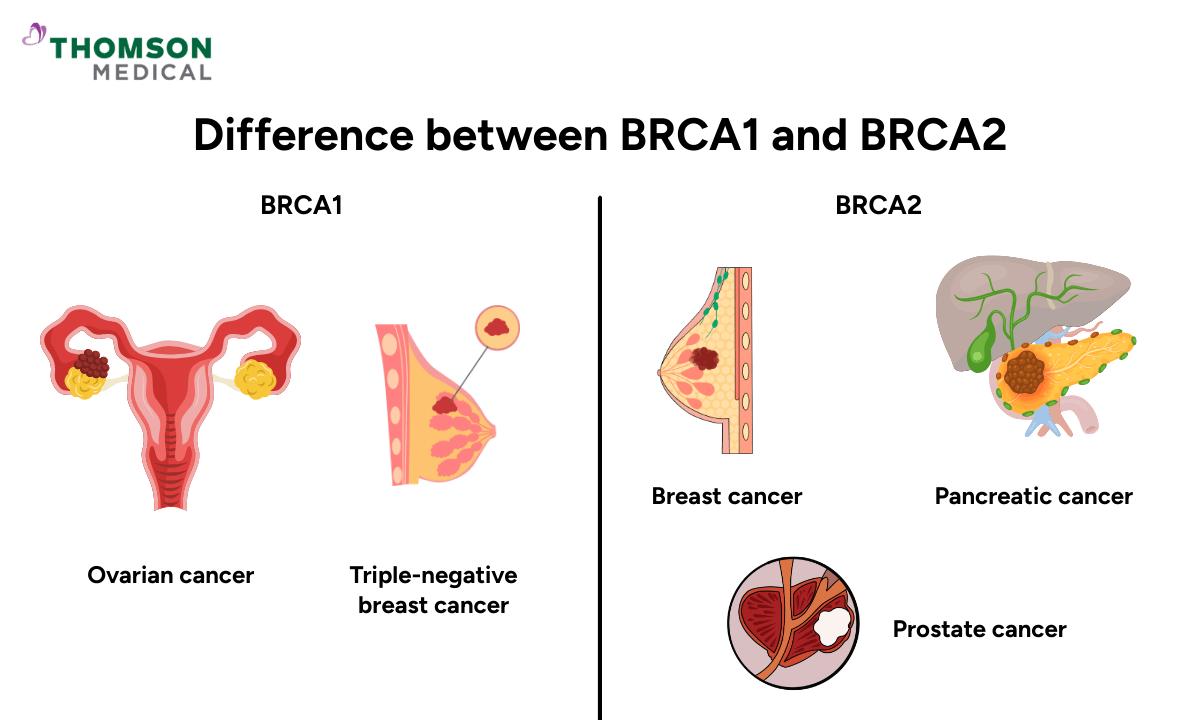
You may have heard of the BRCA genes (BRCA1 and BRCA2) mentioned together. Both genes help repair DNA, and mutations in each of these can raise the risk of breast and ovarian cancer. However, they’re not exactly the same.
Here’s how they differ:
BRCA1 mutations are more strongly linked to:
Triple-negative breast cancer, a type of breast cancer that does not respond to hormone-based treatments
BRCA2 mutations are more commonly linked to:
Pancreatic cancer
Prostate cancer (in men), often with a higher risk of developing the disease earlier
Neither mutation is better or worse than the other. They’re simply different, and knowing which one you carry can help your doctor tailor the approach for you specifically.
Who is more likely to carry a BRCA2 mutation?
It’s natural to wonder whether BRCA2 could affect you or someone you love. The truth is, while BRCA2 mutations can affect anyone, some people are more likely to carry one than others.
You may have a higher chance of carrying a BRCA2 mutation if:
Your close relative (parent, sibling, child) has been diagnosed with breast or ovarian cancer, especially at a younger age
Relatives on the same side of your family have had breast, ovarian, pancreatic, or prostate cancer
Your male relative has had breast cancer
Your family member has already tested positive for a BRCA2 mutation
Having one or more of these factors doesn’t guarantee you carry the mutation. That said, if any of them feel familiar, it’s worth discussing with your doctor.
Does having a BRCA2 mutation mean you will get cancer?
No. Carrying a BRCA2 mutation increases your lifetime risk of certain cancers, but it does not mean cancer is guaranteed. Many people with this mutation go through life without ever developing cancer. Your genes are just one factor, along with your lifestyle, environment, and how you care for your health.
Even if you have a BRCA2 mutation, early detection can improve outcomes. You and your doctor can:
Set up a personalised screening plan to monitor your health more closely
Explore preventative options that are right for your situation
Learning about your BRCA2 status may feel overwhelming at first. But it also gives you valuable information, so you can plan ahead, take action, and feel more in control of your health journey.
If you have a family history of breast or ovarian cancer and want to understand your risk, you may schedule an appointment with Thomson Medical. Our specialists can help walk you through your risks and what you can do about it.
Our specialists in Singapore
Loading...
How is BRCA2 inherited?

BRCA2 mutations are inherited. This means they can be passed down through families. You only need to inherit one affected copy from your mother or your father for the mutation to be present.
It’s also worth knowing that each child of a BRCA2 carrier has a 50% chance of inheriting the mutation, though it’s not a certainty.
The mutation can come from your father’s side just as much as your mother’s. So if there’s a history of breast or ovarian cancer (among the women) on your father’s side, that’s also worth mentioning to your doctor.
It can feel unsettling to think about a mutation passing through generations. However, understanding your family history can be helpful for managing your own health and may also provide valuable information for other family members.
What is BRCA2 genetic testing, and how does it work?
Deciding whether to get tested for the BRCA2 mutation isn’t always straightforward. It brings up a lot of questions and emotions. Once you know what to expect and why each step matters, it becomes much easier to approach with confidence.
Who should consider testing?
BRCA genetic testing is not recommended for everyone.
Your doctor may suggest it if:
Your parent, sibling, or child has tested positive for a BRCA2 mutation
Your personal or family history includes multiple cases of cancer, or cancers diagnosed at a young age
You've been diagnosed with breast or ovarian cancer yourself and want to understand whether a hereditary factor may be involved
If you’re unsure whether testing is right for you, your doctor can review your family history and help you decide.
What to expect during the process?
Before testing, you’ll usually have a session with a genetic counsellor.
They will help you understand:
What the test involves
What the results may mean
How to think through your options
The test itself is simple. Your doctor will collect a blood sample or saliva swab and then send it to a laboratory for analysis. Results are usually available within a few weeks.
What do your results mean?
There are a few possible outcomes from a BRCA2 test:
Negative:
No mutation is found
That said, other factors can still influence cancer risk, so routine health checks remain important
Positive:
A BRCA2 mutation is found, which means your cancer risk is higher than average
Your doctor will help you figure out the next steps, which may include more frequent screenings, medication, or other preventive options
Variant of uncertain significance (VUS):
A change in the gene is detected, but there isn’t yet enough scientific evidence to determine whether it’s harmful
- This is not the same as a positive result, and most people with a VUS follow standard screening guidelines, though your doctor may adjust this based on your personal or family history
Your doctor will explain in detail what it means for your situation
Whatever your result, you don't have to figure it out on your own. Your doctor will help you make sense of what it means for your health and your family, explore the options available to you, and put a plan in place that works for you specifically.
If you're considering BRCA2 genetic testing and want guidance on the next step, you may schedule an appointment with Thomson Medical. Our specialists will review your personal and family history and help you decide whether testing is right for you.
FAQ
Is BRCA2 only relevant to women?
No. Men have the BRCA2 gene too, and a mutation raises their risk of breast cancer, prostate cancer, and pancreatic cancer.
Does a BRCA2 mutation mean I will definitely develop cancer?
No. It raises your lifetime risk, but many people with a BRCA2 mutation never develop cancer. Having the mutation means closer monitoring and more proactive conversations with your doctor.
Can a negative BRCA2 test result guarantee I won't get cancer?
No. A negative result means no BRCA2 mutation was found, but cancer can develop for other reasons, including other gene variants or non-genetic factors.
Can men carry and pass on a BRCA2 mutation?
Yes. Fathers can pass the mutation to both sons and daughters. If your father carries a BRCA2 mutation, you have a 50% chance of inheriting it.
Can lifestyle changes reduce my risk if I have a BRCA2 mutation?
Lifestyle factors, such as maintaining a healthy weight, limiting alcohol, and staying physically active, support your overall health and may have some influence on cancer risk. However, they cannot override a BRCA2 mutation.
What is the next step after a positive BRCA2 result?
It’s best to speak with your doctor, gynaecological oncologist, or genetic counsellor. They'll help you develop a personalised care plan, discuss risk-reducing options, and answer questions specific to your situation.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, request an appointment with Thomson Medical today.
