A hysterectomy is a surgical procedure that removes the uterus and is usually recommended when certain conditions cause significant symptoms or when other treatments have not been effective.
Understanding the reasons a hysterectomy may be advised can help you feel more prepared when discussing your options with your doctor. Learning about the conditions that may lead to this surgery, as well as what it means for your health and recovery, can help you make a more informed decision about your care.
What are common reasons for a hysterectomy?
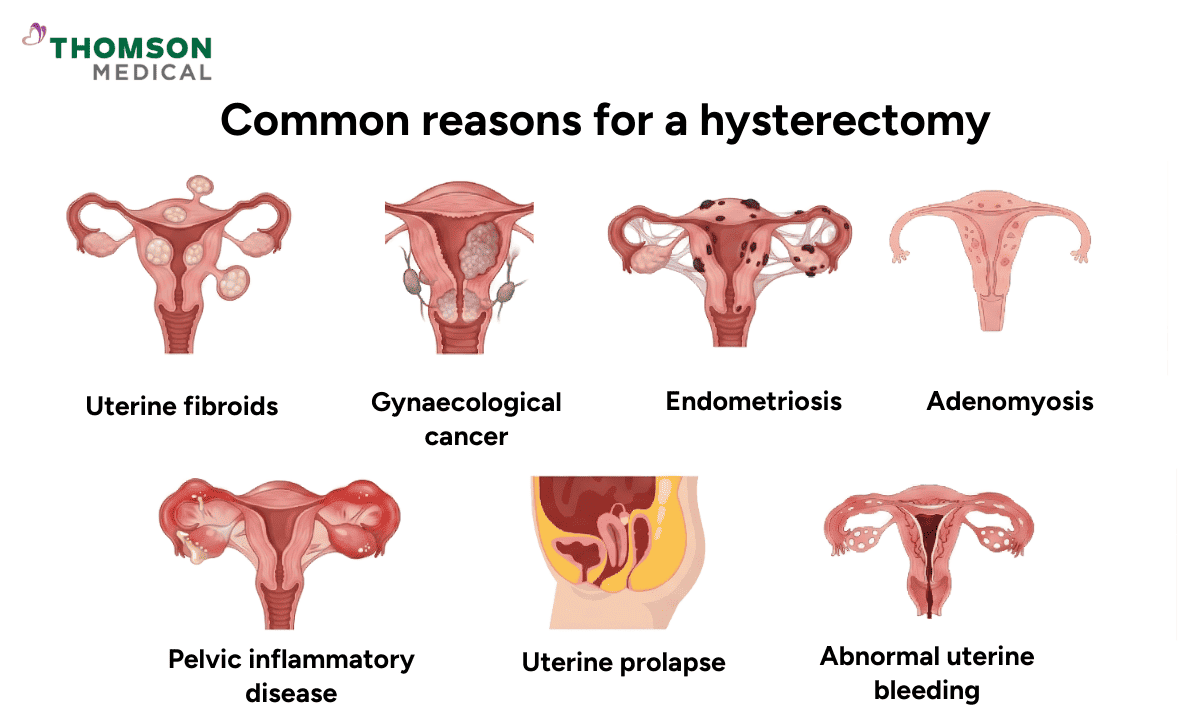
There are several medical conditions that can severely impact your quality of life and lead your healthcare team to recommend removing the uterus.
The most common reasons for a hysterectomy include:
Condition | What is it | Treatment approach |
Non-cancerous muscle growths in the uterus. This is the most common reason for this surgery. | Surgery is considered for large, multiple, or recurring growths. | |
Cancer of the uterus, cervix, ovaries, or endometrium (the lining of your uterus) | Surgery may be life-saving and is often combined with removing other surrounding structures. | |
Tissue similar to the uterine lining grows outside your uterus. | Surgery may help, but pain can persist if tissue remains outside. | |
Endometrial tissue grows directly into your uterine muscle, causing severe pain and very heavy periods. | A hysterectomy helps treat this condition once your childbearing is complete. | |
A chronic or severe pelvic infection. | Surgery is considered if complications are serious and persistent. | |
Uterine prolapse | Your uterus drops into the vagina due to weakened pelvic floor muscles, often after childbirth or menopause. | Surgery is often part of a larger reconstructive procedure. |
Heavy, prolonged, or unpredictable bleeding that disrupts your daily life. | Surgery is recommended only after other treatments have not responded well. |
Living with these conditions can be challenging, especially when symptoms such as pain or heavy bleeding affect your daily life. If you are experiencing severe symptoms, speaking with your doctor about whether a hysterectomy is appropriate for your condition is an important step in understanding your treatment options.
What are the different types of hysterectomy?
If you and your doctor decide that surgery is the suitable path forward, there are different ways the procedure can be performed. The type you receive will depend on your specific medical condition.
Here are common types of hysterectomy:
Total hysterectomy:
Your entire uterus and your cervix are completely removed.
Subtotal or partial hysterectomy:
Your surgeon removes the upper part of your uterus but leaves the cervix in place.
Radical hysterectomy:
Typically performed for cancer, this comprehensive procedure removes your uterus, cervix, the upper part of your vagina, and the surrounding tissues.
It is important to note that your ovaries may or may not be removed during any of these procedures. Whether you keep your ovaries makes a huge difference to your hormone balance, which your doctor will discuss with you beforehand.
If you are considering a hysterectomy and would like to understand which surgical option is better for your circumstances, you can arrange a consultation with Thomson Medical to discuss your condition and treatment options.
What happens to your body after a hysterectomy?
Your physical and emotional changes after surgery will largely depend on whether your ovaries are removed along with your uterus.
If your ovaries are kept
If your ovaries remain in place, the transition after surgery is usually more gradual because your body continues to produce hormones.
You may notice that:
You will no longer have periods.
Your hormone levels will remain mostly normal.
You will not experience sudden or immediate menopause.
Your sexual function is usually well preserved
Because the ovaries continue producing important hormones, menopause will usually occur at the natural age rather than immediately after surgery.
If your ovaries are removed
If your procedure includes removing both ovaries, the changes in your body may happen more quickly because your oestrogen levels drop suddenly.
You may experience:
You will enter immediate surgical menopause.
You may experience sudden hot flushes and night sweats.
You might notice increased vaginal dryness.
You will have an increased risk of bone loss and heart disease due to the drop in oestrogen.
Your doctor may recommend hormone replacement therapy (HRT) to help manage these symptoms. With the right medical support, many women are able to manage surgical menopause well.
Other general changes
Regardless of whether your ovaries are removed, you will experience some common changes after the surgery.
You may notice that:
Future pregnancy is no longer possible.
Your pelvic support may change slightly as your body heals.
Your emotional response to the surgery may vary.
It is normal to experience a range of emotions afterwards. Some women feel relief that their symptoms have improved, while others may need time to adjust to the change, especially if fertility is affected.
Allow yourself time to recover both physically and emotionally, and speak with your doctor or support network if you need additional guidance.
Our gynaecologists in Singapore
Loading...
What to consider before having a hysterectomy
Because a hysterectomy is an irreversible procedure, it can be helpful to discuss several important questions with your doctor.
Some questions you should consider include:
Is my condition life-threatening or significantly affecting my quality of life?
Have I explored all non-surgical treatment options?
Are there any uterus-sparing alternatives available?
Do I want to preserve my future fertility?
Will my ovaries be removed, and what are the reasons for this?
What is the expected recovery time and the possible long-term effects on my body?
Discussing these questions can help you better understand your treatment options and make a decision that aligns with your health needs and personal priorities. Seeking a second opinion is also a reasonable step if you would like additional reassurance about your treatment plan.
If you are considering a hysterectomy and would like guidance before making a decision, it is helpful to speak with a specialist about your options. You may schedule a consultation with Thomson Medical to discuss your concerns and receive personalised medical advice.
FAQ
What is the most common reason for a hysterectomy?
Uterine fibroids are the most common reason. When fibroids grow large enough, they can cause heavy bleeding, pelvic pressure, or severe pain that interferes with daily life.
What is the average age for a hysterectomy?
Hysterectomies are most commonly performed in women between 40 and 50 years old. However, the procedure may be done earlier in cases such as cancer or severe gynaecological disease.
Is a hysterectomy a major surgery?
Yes, a hysterectomy is considered a major surgery. It is performed under general anaesthesia and may require a hospital stay of one to three days, although minimally invasive procedures may allow same-day discharge.
Recovery takes 2-4 weeks for laparoscopic/vaginal surgery and 4-8 weeks for abdominal/open surgery. Minimally invasive options often allow same-day or next-day discharge.
How painful is a hysterectomy?
Most women experience moderate pain in the first few days after surgery, but it improves steadily as healing progresses. Pain is usually well-managed with medication, and minimally invasive procedures such as laparoscopic or vaginal surgery are often less painful than open abdominal surgery.
Does your body shape change after a hysterectomy?
No, removing the uterus does not directly change your body shape or cause hip widening. However, temporary bloating or weight gain from inactivity may occur. Hormonal changes may also affect weight distribution if your ovaries are removed.
Who should not get a hysterectomy?
A hysterectomy may not be suitable for people who wish to preserve future fertility, whose symptoms are manageable with other treatments, or who have effective less invasive options available. Your doctor will also consider whether the potential benefits outweigh the surgical risks.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) Jurong:
6262 8588 (Call), 6262 8588 (WA)- Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
