Most people know that human papillomavirus (HPV) can lead to cancer, but few stop to ask, “What actually happens inside my body for that to occur?"
In reality, the process is far more complex than a simple infection.
Knowing how this virus operates in your body helps you protect your health early before the virus causes any lasting damage.
What is human papillomavirus?
Human papillomavirus (HPV) is not just a single virus. It is the name of a group of over 200 related viruses that infect your skin and mucosal cells (the moistlinings inside your body).
There are two main types of HPV:
Low-risk types:
These strains may cause genital warts or even common warts on your hands and feet.
They are generally considered mild and manageable.
High-risk types:
These strains may lead to cancer if they are not cleared naturally by your body.
HPV-16 and HPV-18 are the two most common causes of cervical cancers.
While a high-risk HPV type has the potential to develop cancer, it alone is not enough to cause cancer. Many women with HPV infection do not develop cancer, even with high-risk strains. This is why regular screening and preventive measures such as vaccination are so important, as they help detect changes early or prevent infections before they have a chance to develop.
If you have concerns about HPV infection or would like to learn more about prevention and screening, it is helpful to speak with a doctor. You may arrange a consultation with Thomson Medical for personalised medical advice.
How does HPV infect your body?
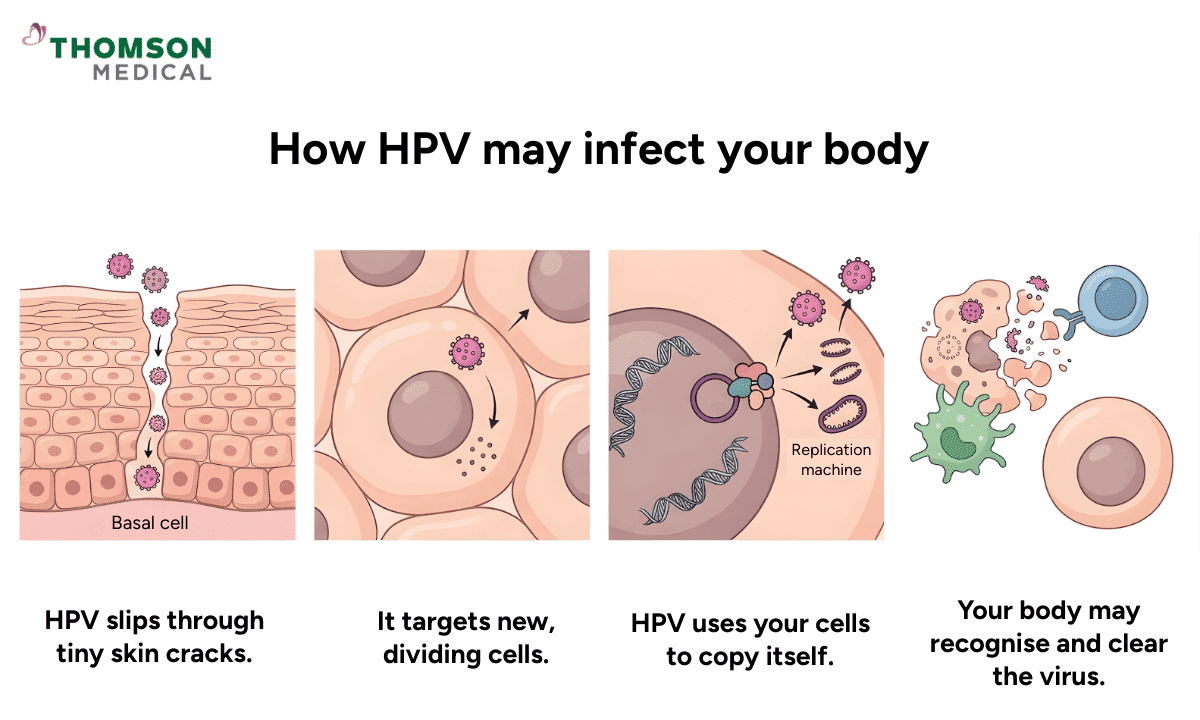
HPV enters the body through tiny breaks in the skin or mucosal surfaces during close contact. This means that intimate, skin-to-skin contact is the most common way HPV spreads from person to person.
Here’s how HPV may infect your body:
The virus slips through very small cracks and reaches your basal layer, where new skin cells are constantly being made.
HPV infects the early-stage cells because they are still growing and dividing.
Once inside, HPV uses the cell’s replication mechanism to copy its viral DNA and produce more virus particles.
Your body may recognise the infection and eliminate the virus.
HPV does not go into the bloodstream. Instead, it stays on the surface tissues of your skin or mucous membranes, such as the cervix, where viral particles may continue to be produced in infected cells.
Most of the time, HPV infections go away on their own, and many people never realise they were infected.
How does HPV cause cancer at the cellular level?
If HPV stays in your body long enough without being cleared by your immune system, it can begin causing abnormal changes in the cells of the cervix. This condition is called “cervical dysplasia” and may lead to cervical cancer if left untreated.
It does this through an intricate process:
Process | What happens? |
Apoptosis | Healthy cells in your body naturally break down to prevent abnormal cells from growing uncontrollably. |
Production of viral proteins | The virus produces proteins, E6 and E7 proteins, that interfere with the cell’s natural function.
|
Unchecked multiplication of damaged cells | Because these protective signals become weak, infected cells may continue dividing even when damaged. |
Accumulation of mutations | As these abnormal cells keep dividing, DNA mutations gradually accumulate. |
This uncontrolled growth can lead to precancerous changes in cervical cells, which may develop into cancer over time. However, it is important to remember that only a persistent high-risk infection may cause this condition.
In other words, early prevention helps reduce the risk of cancers.
How long does it take for HPV to turn into cancer?
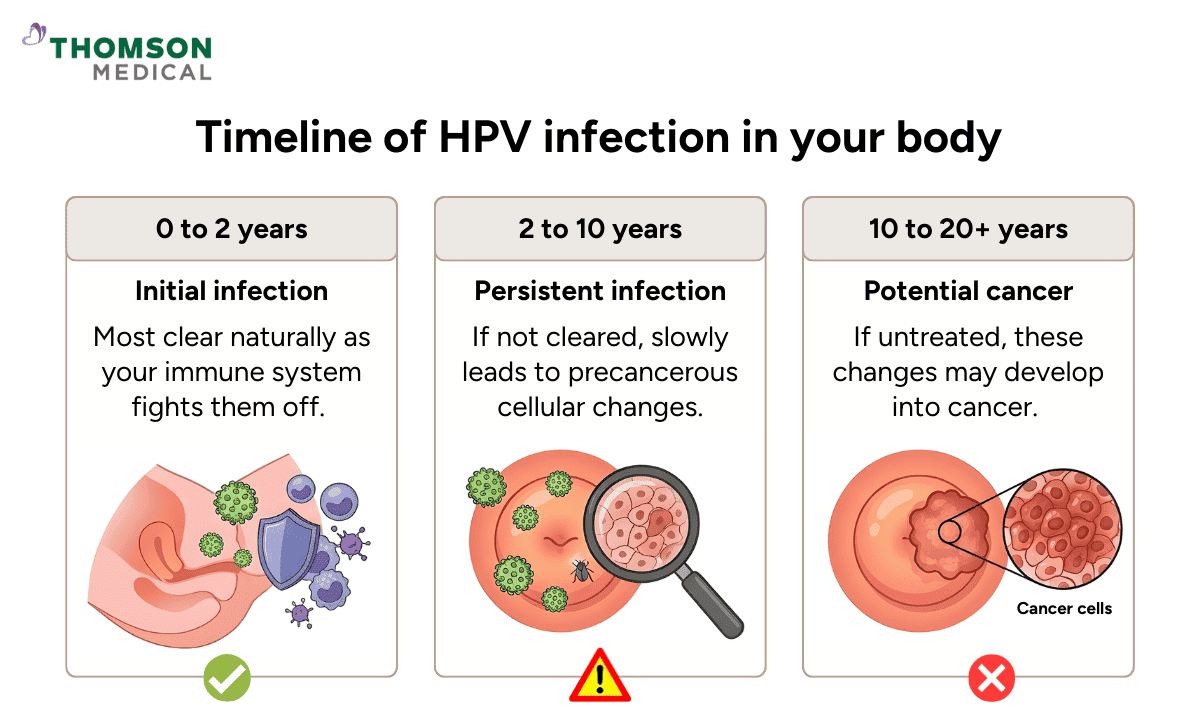
The good news is that this cellular change usually happens very slowly, often over many years.
In many cases, HPV infects your body through this timeline:
0 to 2 years:
Most infections clear naturally as your immune system fights them off.
2 to 10 years:
If the infection is not cleared, it becomes a persistent infection.
This may slowly lead to precancerous changes to your cells.
10 to 20 years or more:
If those precancerous changes are left untreated, they may end up developing into cancer.
This gradual progression allows your healthcare provider to detect and remove these abnormal cells through regular screening tests long before they become dangerous.
Which cancers are caused by HPV?
While the virus is most famously linked to cervical cancer, high-risk strains can affect several other parts of your body.
High-risk HPV is responsible for causing:
In women:
Cervical cancer (accounting for about 99% of cervical cancer cases worldwide)
Vulvar cancer
In men:
Penile cancer
In both men and women:
Anal cancer
Certain head and neck cancers, especially oropharyngeal cancer, which affects the back of your throat, tonsils, and base of your tongue
Many throat cancers are linked to persistent oral HPV infections, especially HPV type 16. As these cancers can be difficult to detect in the early stages, it is important to seek medical advice if you notice lasting symptoms such as mouth sores or difficulty swallowing.
Our gynaecologists in Singapore
Loading...
How can you reduce the risk of HPV-related cancers?
To lower your risk of developing cancers from HPV, there are several strategies you can take to protect your health over time.
HPV vaccination
Getting the HPV vaccine is considered a highly effective way to prevent infection with cancer-causing types.
The vaccine may offer some benefits, including:
Protecting against cervical, anal, throat, and genital cancers
Remaining beneficial even after you have become sexually active
For this reason, HPV vaccination is recommended as part of routine protection against HPV-related diseases.
Regular screening
Routine medical appointments allow your doctor the opportunity to spot any issues at the earliest possible stage and prevent further complications from the virus.
Some common testing options include:
Pap smears detect precancerous cell changes early.
HPV DNA tests identify the presence of a high-risk infection.
Anal Pap tests check for abnormal cell changes in the anal canal that could develop into cancer, particularly in people at higher risk.
Your doctor can advise which screening tests are appropriate based on your age, medical history, and individual risk factors.
Immune system support
Your immune system is your first line of defence, and your daily habits play a key role in its function.
Some healthy habits include:
Quit smoking, as smoking may prevent your body from clearing the virus
Manage any existing chronic illnesses with your doctor
Ensure you get adequate sleep and a nutrient-rich diet
Maintaining these healthy habits can help support your immune system in managing HPV infections.
Safer sexual practices
As HPV is a common sexually transmitted infection (STI), being careful of how you approach intimacy may help reduce your chance of exposure to the virus.
Some common steps include:
Using condoms to reduce your risk of transmission, though they do not eliminate it entirely
Having fewer sexual partners to limit exposure
Being open with your partners about sexual health and STI testing
Reducing your risk of HPV-related cancers often involves the combination of these four approaches. While they don’t offer complete protection, taking these precautions early may help create a safer environment for both you and your partners.
What treatment options exist for HPV-related abnormalities?
While there is currently no medication that removes the virus itself, there are effective ways to manage HPV and treat any health changes it may cause.
For precancerous changes, your doctor may suggest:
Monitoring, or watchful waiting, on the cells to see if they heal on their own
Cryotherapy to freeze and destroy abnormal cells
LEEP or cone biopsy to carefully remove the abnormal tissue from your cervix
If the cells have progressed to cancer, there are still many effective treatments available:
Surgery to remove the cancerous tumour and surrounding tissue
Radiation to target and shrink the cancer cells
Chemotherapy to target cancer cells using specialised medications
Immunotherapy, depending on the stage, to help your immune system fight the cancer more effectively
Your medical team will discuss the available options with you and recommend a care plan suited to your situation, supporting you at every step of the process.
If you have been diagnosed with HPV-related cell changes or would like to understand your treatment options, schedule a consultation with Thomson Medical to discuss the most suitable next steps for your condition.
FAQ
How does HPV turn into cancer?
Only persistent high-risk HPV can cause cancer. It does this by disabling tumour-suppressor genes that normally control cell growth. Without these safeguards, damaged cells can multiply unchecked and eventually form a tumour.
How long can someone have HPV before it becomes cancerous?
In most cases, it takes 10 to 20 years or longer. Cancer caused by HPV develops slowly, which gives your doctor time to detect and treat precancerous changes during routine screenings.
Can HPV go away on its own?
Yes. Around 70 to 90 percent of infections clear naturally within one to two years. Younger people and those with strong immune systems often clear the virus faster.
Can oral HPV cause throat cancer?
Yes. If the infection persists in your mouth or throat, certain types, especially HPV 16, can lead to cancers of the tonsils, the base of the tongue, or the oropharynx.
What if HPV does not clear after 2 years?
This is called persistent HPV. It does not mean you have cancer, but it does increase your risk. Your doctor may recommend more frequent screening, biopsies, or treatment of precancerous cells to keep you safe.
Are all HPV infections high risk for cancer?
No. Most HPV types are low-risk and will never cause cancer. Only about 14 types are considered high risk and need closer monitoring.
Does vaccination still help if someone already has HPV?
Yes. The vaccine will not treat the infection you already have, but it can still protect you from other high-risk HPV types you have not been exposed to, helping reduce your future cancer risk.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
Reference
Bogani, G., Sopracordevole, F., Ciavattini, A., Vizza, E., Vercellini, P., Giannini, A., Ghezzi, F., Scambia, G., Raspagliesi, F., Di Donato, V., & Italian Society of Colposcopy and Cervico-Vaginal Pathology (SICPCV); The Investigators of the Italian HPV study group (iHPV study group) (2023). Duration of human papillomavirus persistence and its relationship with recurrent cervical dysplasia. European journal of cancer prevention : the official journal of the European Cancer Prevention Organisation (ECP), 32(6), 525–532. https://doi.org/10.1097/CEJ.0000000000000822
Centers for Disease Control and Prevention. (2024, April 23). Chapter 11: Human papillomavirus. In Epidemiology and prevention of vaccine-preventable diseases (The Pink Book). https://www.cdc.gov/pinkbook/hcp/table-of-contents/chapter-11-human-papillomavirus.html
Köse, F. M., & Naki, M. M. (2014). Cervical premalignant lesions and their management. Journal of the Turkish German Gynecological Association, 15(2), 109–121. https://doi.org/10.5152/jtgga.2014.29795
National Cancer Institute. (2025, May 9). HPV and cancer. U.S. Department of Health and Human Services. https://www.cancer.gov/about-cancer/causes-prevention/risk/infectious-agents/hpv-and-cancer
UK Health Security Agency. (2013, March 20). Human papillomavirus (HPV): The Green Book, chapter 18a. https://assets.publishing.service.gov.uk/media/5a7c5284ed915d3d0e87b997/dh_133346.pdf
World Health Organization. (2017, April 5). Human papillomavirus (HPV). https://www.who.int/europe/news-room/fact-sheets/item/human-papillomavirus-(hpv)
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) - Jurong:
6262 8588 (Call), 6262 8588 (WA) - Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
Notice
The range of services may vary between TWC/TS locations. Please contact your preferred branch directly to enquire about the current availability.
Request an Appointment