A hysterectomy may be a major operation, but it is also a common and well-established procedure. Doctors recommend it to help treat conditions that cause ongoing pain, heavy bleeding or other symptoms that affect your daily life.
By learning about the different hysterectomy surgical options, you can better understand why a particular approach is recommended and feel more prepared as you take the next steps on your treatment journey.
Types of hysterectomy

Because every woman's body and medical needs are unique, there is no single approach to hysterectomy surgery. Your doctor will carefully consider your specific condition, your age, and your overall health before recommending the appropriate option for you.
A partial hysterectomy
A partial hysterectomy means your surgeon removes the upper part of your uterus while leaving your cervix in place. It is often recommended if you are dealing with a benign (non-cancerous) condition and want relief from ongoing symptoms.
Your doctor might suggest this option if you are experiencing issues such as:
Uterine fibroids that cause discomfort or heaviness
Because your cervix remains, you can still develop cervical cancer. As such, cervical screening is still important.
In most cases, you will need to continue routine screening until the age of 65, as long as you have no history of high-grade or cancerous cell changes.
A total hysterectomy
For a total hysterectomy, your surgeon removes your entire uterus, which includes your cervix. This is considered the most common type of hysterectomy surgery.
This option is often recommended if you are dealing with ongoing symptoms or certain medical conditions, such as:
Uterine fibroids, adenomyosis, and endometriosis
Chronic pelvic pain or abnormal uterine bleeding
Pelvic organ prolapse
Various gynaecological cancers, such as uterine cancer, cervical cancer or ovarian cancer
Because your cervix is removed, your risk of cervical cancer becomes very low. In most cases, you may not need routine screening afterwards unless you have previously had cervical cancer or precancerous cell changes.
Your care team will guide you on whether any future screening is needed based on your personal medical history, so you can feel reassured about your long-term care.
A hysterectomy with oophorectomy
Sometimes, your doctor may recommend removing your ovaries at the same time as your uterus to fully treat your condition. A hysterectomy removes your uterus and cervix. An oophorectomy means removing one or both ovaries.
When these procedures are done together, it is usually to treat conditions such as:
Severe endometriosis
Uterine fibroids
Specific gynaecological cancers
If both ovaries are removed, your body will go into surgical menopause straight away. This happens because your ovaries are your main source of oestrogen.
If this applies to you, your doctor may recommend hormone replacement therapy (HRT) to help ease symptoms and make the transition more manageable.
A hysterectomy with salpingo-oophorectomy
This is a more extensive type of surgery. “Salpingo” refers to the fallopian tubes. In this procedure, your surgeon removes your uterus, cervix, one or both fallopian tubes, and one or both ovaries.
It may be recommended if you are dealing with:
Severe cases of endometriosis or chronic pelvic pain
Fibroids and pelvic organ prolapse
Gynaecological cancers
Preventive treatment if you have a high risk of ovarian cancer
Your healthcare provider will work closely with you to manage any menopausal symptoms and explore options like HRT if it is suitable for your health profile.
A radical hysterectomy
A radical hysterectomy is the most extensive type of hysterectomy. It involves removing your uterus, cervix, the upper part of your vagina, much of the surrounding tissue, and sometimes nearby pelvic lymph nodes.
This surgery is usually recommended for:
Early-stage cervical cancer
Certain early-stage uterine cancers
Selected cases of other gynaecological cancers
The goal is to remove the cancer completely, along with a small margin of healthy tissue around it, to reduce the risk of any cancer cells being left behind. It is often performed through a cut in the lower abdomen, although in some cases a laparoscopic approach may be possible.
Depending on your results after surgery, you may need further treatment such as chemotherapy or radiotherapy, especially if there is a concern that the cancer has spread.
Your care team will guide you through each step, monitor your recovery closely, and explain clearly what to expect next so you feel supported and informed throughout your treatment.
Our O&G specialists
Loading...
What type of hysterectomy do you need?
The type of surgery you need depends on your specific diagnosis, symptoms and medical history. Each approach has its own benefits, and the right choice is the one that best supports your health now and in the long term.
Benefits of a partial hysterectomy
A partial hysterectomy keeps your cervix in place. For some women, this may offer certain functional benefits.
Potential advantages include:
Slightly shorter recovery time
Lower risk of injury to the bladder or bowel during surgery
Better natural pelvic support, which may reduce the risk of pelvic organ prolapse
This option can be helpful when treating benign conditions. However, because the cervix remains, you will still need regular cervical screening. Your doctor will help you balance these benefits with the need for ongoing monitoring.
Benefits of a total hysterectomy
A total hysterectomy removes the cervix completely.
This offers several benefits, including:
Significantly lower risk of developing cervical cancer
No longer needing routine cervical screening in most cases
Greater peace of mind, especially if you have had abnormal cell changes in the past
Your doctor will confirm whether you can safely stop routine screening after your recovery, based on your personal medical history.
Benefits of a hysterectomy with salpingo-oophorectomy
Removing the ovaries and fallopian tubes alongside the uterus offers benefits including:
A significantly reduced risk of ovarian cancer
A proactive option if you have a strong family history of ovarian cancer
An important risk-reducing step if you carry certain genetic mutations
For women identified as high risk, this approach can be a meaningful part of a long-term health plan, helping you feel more in control of your future wellbeing.
Benefits of a radical hysterectomy
Although it is a more extensive procedure, a radical hysterectomy offers important benefits, including:
A higher chance of completely removing the cancer
Improved survival rates in early-stage cervical cancer
Better control of certain early endometrial cancers
Greater reassurance that the surrounding affected tissue has been cleared
By removing not only the uterus but also nearby tissues and sometimes lymph nodes, this surgery reduces the risk of cancer remaining in the pelvis. In some cases, it may also reduce the need for additional treatments or allow them to be more precisely tailored. For many women, this creates a clearer treatment plan and a stronger starting point for recovery.
If you have been advised to consider a radical hysterectomy and would like to understand whether it is the right option for your condition, seeking specialist advice is essential. You may schedule a consultation with Thomson Medical to discuss your diagnosis, treatment options, and personalised care plan.
Surgical techniques for hysterectomy
Just as there are different types of hysterectomy, there are also different ways your surgeon can perform the operation. The technique chosen will depend on the size of your uterus, your overall health, and the reason for your surgery.
Open surgery hysterectomy
An open surgery, also called an abdominal hysterectomy, is performed under general anaesthesia. Your surgeon makes a horizontal or vertical cut in your lower abdomen to remove your uterus.
You can generally expect:
Surgery lasting about 1 to 4 hours
A hospital stay of around 1 to 3 days, depending on your condition
A recovery period of roughly 6 to 12 weeks
This traditional approach allows your surgeon to clearly see and access your pelvic organs. It is often recommended for complex cases, very large fibroids, or certain cancers where wider access is needed.
Minimally invasive hysterectomy
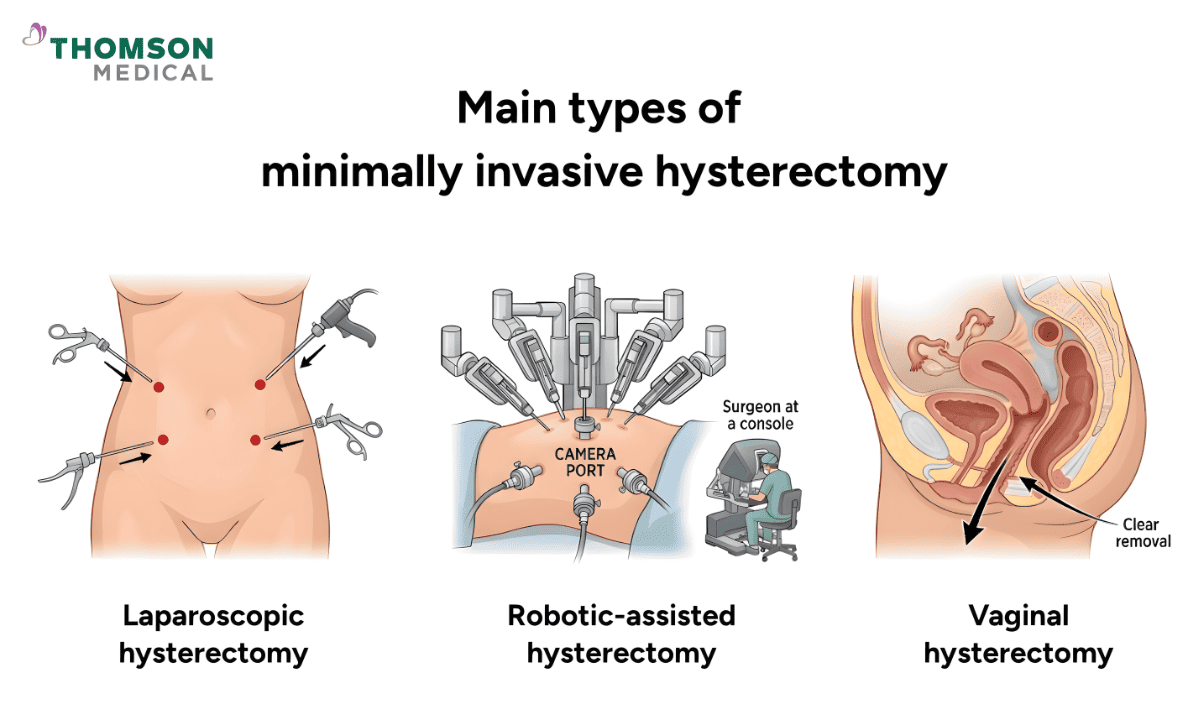
Minimally invasive procedures (MIP) aim to reduce the physical impact of surgery. They are performed under general or sometimes regional anaesthesia and usually take 1 to 3 hours.
There are three main types of MIP hysterectomy:
Laparoscopic hysterectomy:
Your surgeon makes a small cut near your belly button to insert a camera (laparoscope).
They then add another two small cuts lower down to insert specialised surgical instruments.
Your uterus is removed through one of these small cuts.
Robotic-assisted hysterectomy:
This technique is similar to laparoscopic surgery, but your surgeon uses robotic arms to guide the instruments.
This allows for more precise and controlled movements during the procedure.
Vaginal hysterectomy:
Your surgeon removes your uterus directly through the vagina.
This means there is no visible scar on your abdomen.
These advanced techniques often mean you may not need to stay in the hospital for long, and in some cases, you can go home the very next day.
Recovery is usually quicker as well, with many women able to resume their daily routines within about 2 to 4 weeks, depending on the type of surgery and your overall health.
Comparison of MIP and open surgery hysterectomy
When deciding between an MIP and open surgery, your doctor will discuss the pros and cons of each with you. Generally, minimally invasive techniques offer several notable physical advantages for your recovery.
Compared to open surgery, an MIP usually offers:
A faster overall recovery time
A shorter hospital stay
A lower risk of infection, post-operative bleeding, and pain
Smaller, less noticeable scars on the abdomen, or no abdominal scars at all
While MIP has many physical benefits, it is not suitable for every medical condition. Your surgeon will carefully evaluate your medical history to recommend the safest and most effective surgical route for your body.
If you are considering hysterectomy surgery and would like guidance on whether MIP or open surgery is more suitable for you, schedule a consultation with Thomson Medical to discuss your options and plan the suitable approach for your condition.
FAQ
What is the most common type of hysterectomy surgery?
A total hysterectomy is the most common. It removes the uterus and cervix and is used to treat both benign conditions and certain gynaecological cancers.
Which is the most painful hysterectomy?
An abdominal, or open, hysterectomy is usually the most painful because it involves a larger incision. Recovery typically takes 6 to 12 weeks, and pain management is part of your care plan.
What is better, a partial hysterectomy or a full hysterectomy?
It depends on your diagnosis. A total hysterectomy lowers the risk of cervical cancer. A partial hysterectomy keeps the cervix and may help maintain pelvic support. Your doctor will recommend what suits your condition best.
Which type has the shortest recovery time?
Minimally invasive options, such as a laparoscopic or vaginal hysterectomy, offer a much shorter recovery time. They usually take about 2 to 3 weeks to recover from, compared to an abdominal hysterectomy, which can take 6 to 8 weeks or more.
How long does the surgery take?
The duration of the surgery can vary depending on the technique and complexity. In general, it takes about 1 to 4 hours. However, some complex cases or procedures involving the removal of additional tissue may take up to 5 hours to complete safely.
Which type is considered the safest?
A vaginal hysterectomy is generally considered the safest and least invasive method. It tends to offer positive outcomes with fewer complications, less pain, and a quicker recovery time. It is frequently offered for benign conditions such as endometriosis, fibroids, pelvic organ prolapse, and abnormal uterine bleeding.
What fills the space after a partial hysterectomy?
It is very common to wonder what happens inside your body once an organ is removed. After the surgery, your small and large intestines will naturally shift downward to fill most of the space that your uterus previously occupied.
The information provided is intended for general guidance only and should not be considered medical advice. For personalised recommendations and tailored advice based on your unique situations, please consult a specialist at Thomson Medical. Request an appointment with Thomson Medical today.
For more information, contact us:
Thomson Specialists (Women's Health)
Thomson Women's Clinic (TWC)
- Novena:
6592 6686 (Call), 8611 8986 (WA) - Bukit Batok:
6569 0668 (Call), 8686 3525 (WA) - Choa Chu Kang:
6893 1227 (Call), 8282 1796 (WA) - Jurong:
6262 8588 (Call), 6262 8588 (WA) - Katong (female doctor):
6970 2272 (Call), 8611 9020 (WA) - Punggol:
6243 6843 (Call), 8811 0328 (WA) - Sembawang: 6753 5228
- Sengkang: 6388 8125
- Serangoon (female doctor): 6382 3313
- Tampines: 6857 6266
- Tiong Bahru: 6276 1525
Notice
The range of services may vary between TWC/TS locations. Please contact your preferred branch directly to enquire about the current availability.
Request an Appointment